Paracentesis
Medically reviewed by Drugs.com. Last updated on Jun 30, 2025.
What is paracentesis?
Paracentesis is a procedure to remove abnormal fluid buildup in your abdomen. Fluid may build up because of liver problems, such as swelling and scarring. Heart failure, kidney disease, a mass, or problems with your pancreas may also cause fluid buildup.
How do I prepare for paracentesis?
Your healthcare provider will tell you how to prepare. Tell your provider about all the medicines you take, including over-the-counter medicines. Your provider will tell you what medicines to take or not take on the day of your procedure. Tell your provider if you take any blood thinning medicines, including aspirin, an NSAID, or a prescription blood thinner. If you are a woman, tell your provider if you are or think you may be pregnant. Tell your provider if you have ever had an allergic reaction to any numbing medicine. Also tell your provider about any health conditions you have.
Related medications
Creon
Creon (pancrelipase) contains digestive enzymes and is used to improve food digestion in people who ...
Prednisone
Prednisone is used to treat allergic disorders, ulcerative colitis, psoriasis and arthritis. Learn ...
Botox
Botox is used cosmetically to reduce facial lines and wrinkles and for medical purposes for ...
Bumetanide
Bumetanide is used for ascites, autism, edema, pulmonary edema
Spironolactone
Spironolactone is a potassium-sparing diuretic that is primarily used to treat heart failure, high ...
Carvedilol
Carvedilol (Coreg) is used to treat heart failure and hypertension (high blood pressure). Includes ...
Montelukast
Montelukast is a daily oral medication used to prevent asthma attacks, exercise-induced ...
Pancreatin
Pancreatin is used for chronic pancreatitis, cystic fibrosis, pancreatic cancer, pancreatitis
Furosemide
Furosemide is a loop diuretic used to treat fluid retention and high blood pressure by increasing ...
What happens during paracentesis?
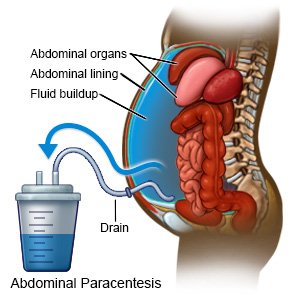
- Your healthcare provider will tap on and feel your abdomen to decide where to insert the needle. Your provider may also use an ultrasound to help decide where to insert the needle. Numbing medicine will be put on your skin where the procedure will be done. This medicine will help prevent pain. A needle will be inserted into your abdominal cavity. A syringe will be attached to the needle to remove a small amount of fluid.
- To remove a larger amount of fluid, a needle will be inserted into your abdominal cavity. A catheter (small, thin tube) is attached to the needle and the needle is removed. The catheter tubing will be attached to a suction device to help remove the fluid. The fluid will drain into a container attached to the tubing. The removal of large amounts of fluid may take up to 6 hours. When your healthcare provider has pulled enough fluid from your abdomen, the catheter will be removed. Your wound (procedure site) will be covered with a bandage. The fluid may be sent to a lab for tests.
 |
What should I expect after paracentesis?
You may need to lie on the side without the wound for up to 2 hours. This may prevent fluid leakage from your wound. If the wound leaks and will not stop, your healthcare provider may stitch the area closed. You may need fluids or volume expanders given through your IV after your procedure. These fluids include albumin or saline. Albumin is a protein found in your blood. The IV fluids help prevent a drop in your blood pressure.
What are the risks of paracentesis?
During paracentesis, the needle may damage your abdominal organs or blood vessels. After paracentesis, you may bleed, or remaining fluid may leak out from your wound. You may get an infection in your wound, or in the lining of your abdomen. If a large amount of fluid is removed during your procedure, your blood pressure may become very low. This may decrease blood flow in your body and make you dizzy or short of breath. You may get a blood clot in your abdomen or lungs. A blood clot in your lungs can cause chest pain and trouble breathing, and can be life-threatening. Even with paracentesis, your kidney or liver function may not improve. Fluid may build up again, and you may need another paracentesis.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
