What causes a rash that moves to different parts of the body?
Hives are raised red or skin-colored welts or rashes that typically flare up suddenly and have a habit of changing shape or moving from one area of the body to another. These welts can vary in size, and they are notorious for causing intense itching, often surrounded by a wheal. These wheals can sometimes merge, forming a map-like pattern or a large patch.
In 10% of people, there may also be swelling or edema which may affect the eyelids, lips, hands or elsewhere. While this swelling is usually short-lasting and not serious, it can become a cause for concern if it affects the throat, impeding breathing or causing hoarseness. In such cases, it's crucial to seek immediate medical attention by calling 911 or visiting the emergency room.
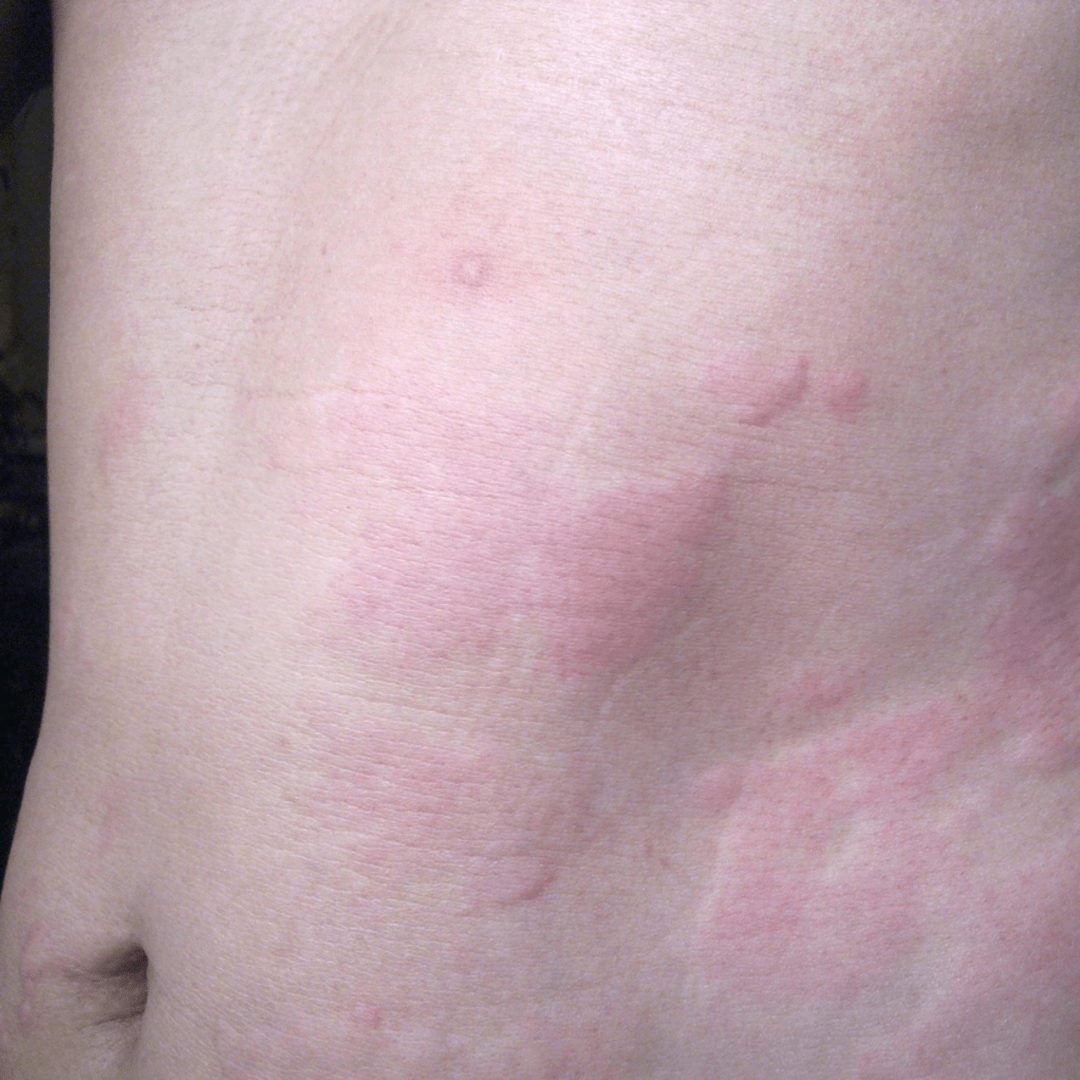
The Medical Term: Urticaria
Hives are medically referred to as urticaria, derived from the Latin words "urtica" meaning nettle and "urere" meaning to burn. Despite their commonality, hives can manifest differently from one person to another and may even vary within the same individual on different occasions.
Although these welts are raised, they typically have a smooth surface (unlike dermatitis, which tends to be rough). Some individuals may have bright red welts, while others may experience paler, skin-colored welts. Some hives take on a circular appearance with a pale center and a distinctive red halo.
Other symptoms associated with hives may include a burning or stinging sensation. When pressed, the center of a red hive usually turns white; this phenomenon is known as "blanching." Hives can migrate across the skin, appearing on one part of the body for a short period, disappearing, and then reappearing in a different area.
Diagnosing Hives: What You Need to Know
Hives are known for their ever-changing nature. They typically don't stick around for more than 24 to 48 hours, and they can look different from day to day or episode to episode. You don't need to capture pictures; doctors can diagnose hives by listening to your description of symptoms.
However, if hives last for more than six weeks (which is considered chronic), dermatologists might run some tests. These could include allergy tests, blood work, or a skin biopsy. They may also ask about your family's hives history. But in most cases of chronic hives, the cause remains a mystery.
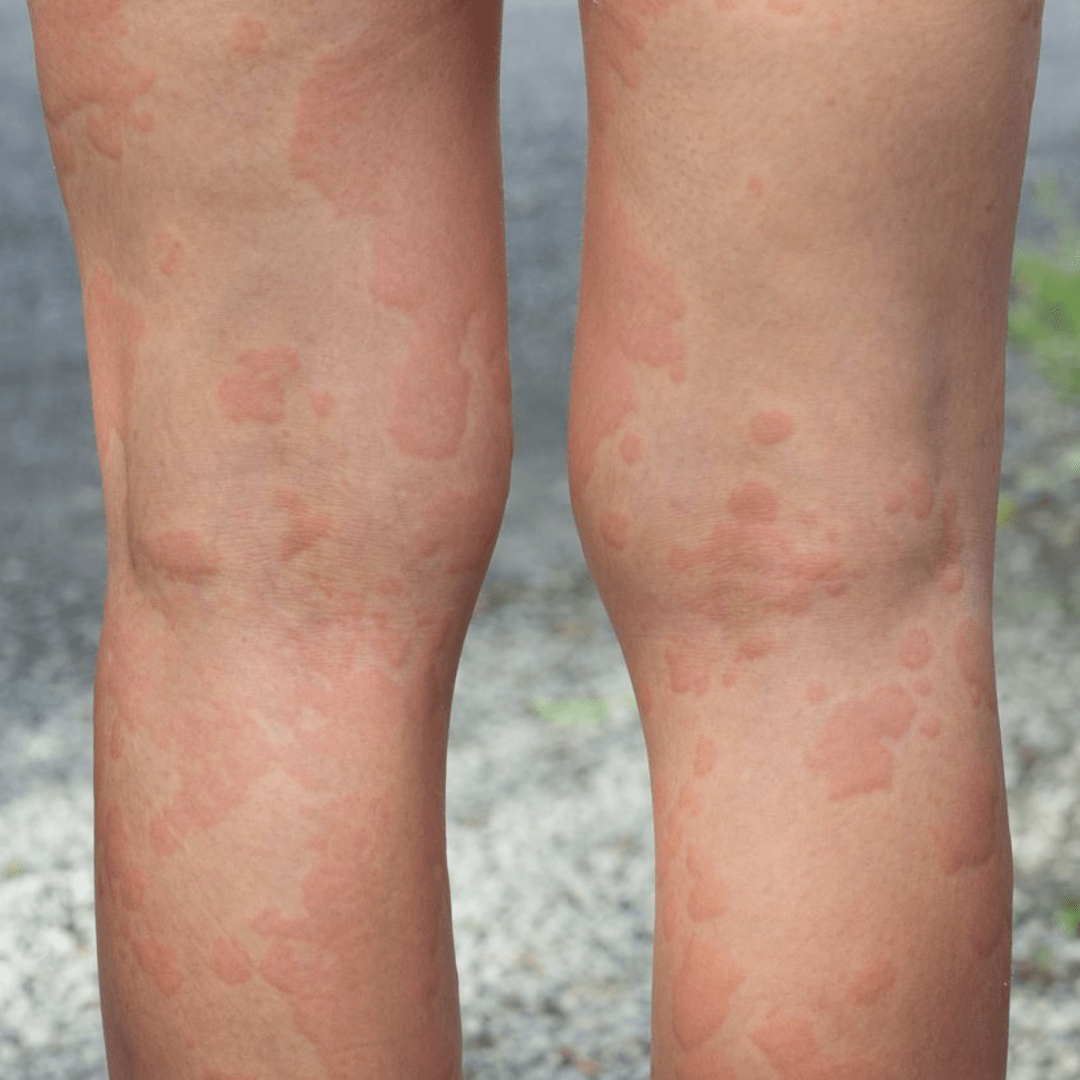
Causes of Hives
While many assume that hives are primarily caused by allergies, it's essential to note that over 75% of hives in adults are not related to allergies. However, in cases where allergies are a trigger, common culprits include:
- Blood transfusions
- Certain foods like berries, chocolate, eggs, fish, nuts, shellfish, soy, or wheat
- Food additives such as tartrazine or MSG
- Insect stings and bites, or jellyfish stings
- Latex
- Medications, including antibiotics, aspirin, and ibuprofen
- Pet dander
- Plants like poison oak, poison ivy, and sumac
- Pollen
Hives can also be triggered by environmental factors, bacteria, viruses, anxiety, or stress.
Types of Inducible Hives
Certain physical stimuli can induce hives in susceptible individuals. These include:
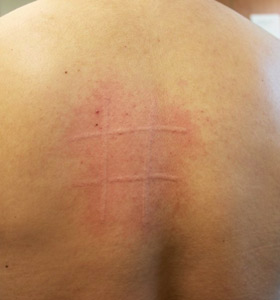
- Dermographism: Hives or raised skin areas appear where the skin has been stroked, scratched, or rubbed, or after contact with tight clothing or towel drying after a hot shower.
- Cold urticaria: Hives develop on skin exposed to cold air, cold water, ice blocks, or following cryotherapy.
- Cholinergic urticaria: Hives appear in response to sweat induced by exercise or emotional stress, or following a hot shower.
- Contact urticaria: Hives occur upon contact with an allergen, pseudoallergen, or irritating substance, such as cosmetics, hairy caterpillars, latex, meat, medicines, saliva, stinging nettle, textiles, or white flour.
- Delayed pressure urticaria: Hives appear (often after a few hours) where pressure has been exerted on a certain area of the skin, such as from a handbag, seatbelt, standing on a ladder rung, or sitting on a horse.
- Solar urticaria: Typically involves hives appearing on body areas not usually exposed to the sun, like the abdomen and top of the thighs, sparing the face, neck, and hands. It may be triggered by long-wavelength UV light or visible light.
- Heat urticaria: Hives develop on skin areas in contact with a hot water bottle or after ingesting a hot drink.
- Vibratory urticaria: Hives spontaneously occur after exposure to vibrations, such as using a jackhammer.
- Aquagenic urticaria: Hives develop upon exposure to fresh, chlorinated, or salty hot or cold water.

Related questions
- Can you have a vaginal yeast infection if you have no uterus?
- What are 7 Essential First Aid Kit Items?
- Prednisone: What are 12 Things You Should Know?
Hives Medications
Hives occur when certain chemicals in our body, like histamine, make your skin itchy, red, and swollen. To ease these symptoms, doctors often recommend antihistamines.
There are two types:
- Second-generation antihistamines: These include cetirizine, desloratadine, fexofenadine, or levocetirizine. They don't usually make you drowsy and work by blocking histamine, which causes the itch and redness. Just follow the recommended dosages and stop when the hives disappear. Taking a second antihistamine doesn't help much.
- Older (first-generation) antihistamines: These, like promethazine or chlorpheniramine, can make you feel sleepy and have side effects like a dry mouth, blurry vision, or constipation. They can also interact with other medications. They're considered for severe hives when stronger relief is needed.
Managing Hives: Avoiding Triggers and Supporting Recovery
If your hives are connected to allergies, a combination of avoiding the allergen and using antihistamines usually helps hives go away within 48 hours. Some types of hives triggered by specific factors tend to clear up quickly, but others might hang around even after you remove the trigger.
To improve your chances of relief:
Address Underlying Infections: In some cases, chronic hives might be linked to infections like Helicobacter pylori or intestinal parasites. Treating these infections can help with chronic hives.
Lifestyle Adjustments: While some factors don't directly cause hives, they can make the situation worse. To ease discomfort, consider these steps:
- Stay cool and minimize heat exposure.
- Opt for pain relief alternatives like acetaminophen instead of drugs like aspirin, NSAIDs, or opioids.
- Reduce your intake of potential food triggers for at least three weeks.
- Apply cooling methods, like using a fan, an ice pack, or a cold cloth on the affected area.
- If you have specific types of hives, like solar urticaria, wearing sun-protective clothing can be helpful.
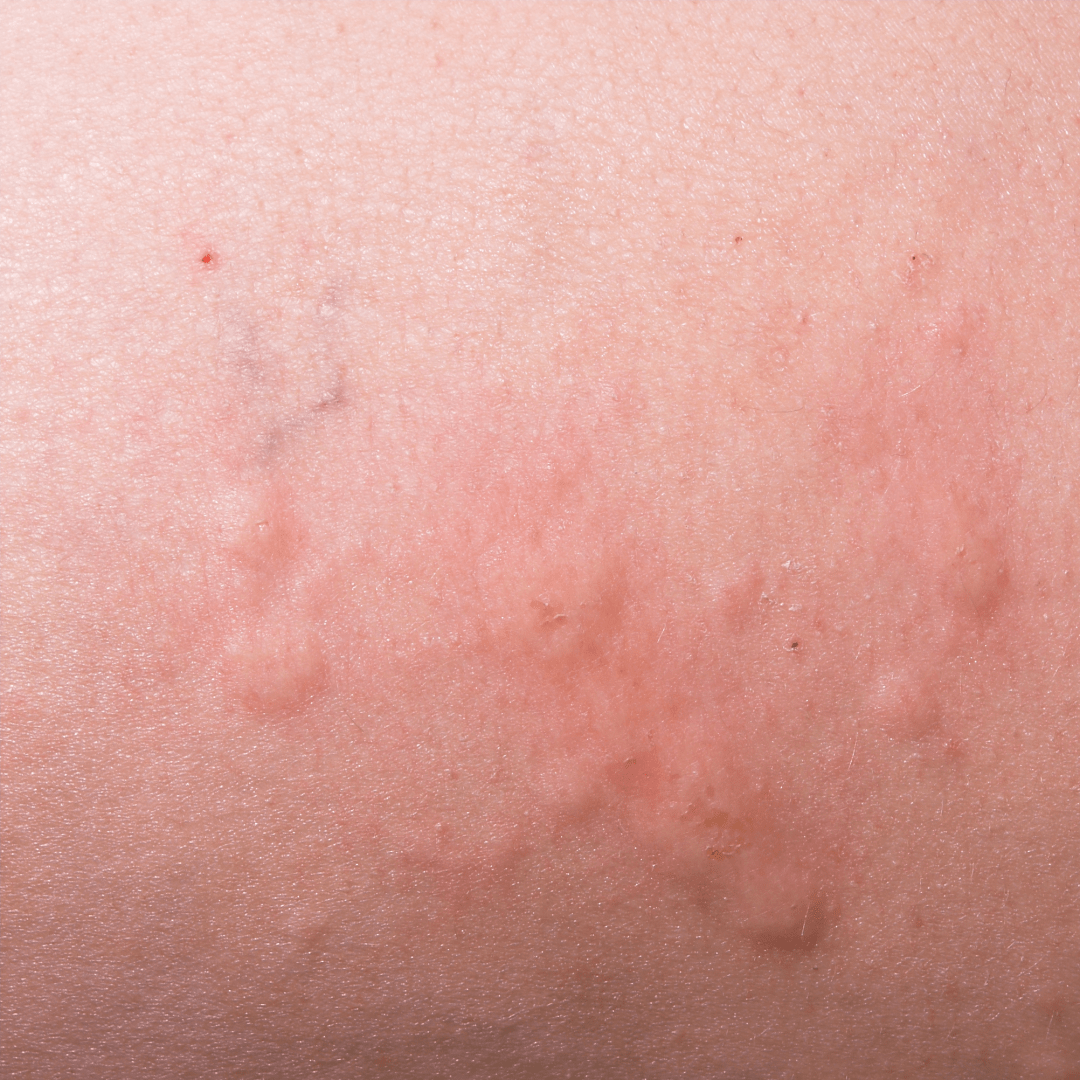
More pictures of Hives
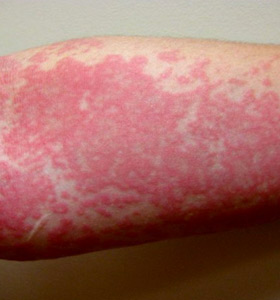
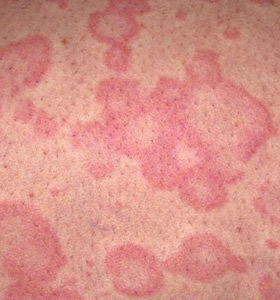
References
- Hives: Diagnosis and Treatment. American Academy of Dermatology Association. 2023. https://www.aad.org/public/diseases/a-z/hives-treatment
- Hives and angioedema. Mayo Clinic. 2023. https://www.mayoclinic.org/diseases-conditions/hives-and-angioedema/symptoms-causes/syc-20354908
- Benedetti J. Urticaria MSD Manual Professional Version. Updated Sept 2022. https://www.msdmanuals.com/professional/dermatologic-disorders/approach-to-the-dermatologic-patient/urticaria
- Fine LM, Bernstein JA. Guideline of Chronic Urticaria Beyond. Allergy Asthma Immunol Res. 2016;8(5):396-403. doi:10.4168/aair.2016.8.5.396
Read next
Amoxicillin rash: When should I be concerned?
From 5% to 10% of children will develop a rash from amoxicillin after taking it, which in most cases, is considered a side effect of amoxicillin and not an allergic rash. But in a small number of cases, the rash will be a sign of an allergic reaction which means the amoxicillin will need to be stopped right away. Continue reading
Hives vs Rash - What's the difference between them?
The main difference between hives and a rash is that hives are a particular type of rash, characterized by swollen, pale-red or skin-colored bumps on the skin that appear and disappear quickly, and tend to “blanch” (which means turn white) when pressed. Hives are also known as urticaria. Continue reading
Is triamcinolone good for poison ivy?
Steroid prescription creams or ointments like high-potency triamcinolone 0.5% may be helpful during the first few days of a poison ivy rash on a small area, but have little effect once the fluid-filled blisters have appeared. Over-the-counter (OTC) products like hydrocortisone cream 1% are not usually strong enough for poison ivy. Your doctor may prescribe oral prednisone pills for a more severe rash. Continue reading
See also:
Related medical questions
- Prednisone vs Prednisolone - What's the difference?
- What is the best treatment for a poison ivy rash?
- What to do if I develop a rash while taking lamotrigine?
- I'm having a reaction after taking fluconazole, is this normal?
- What are Hives (Urticaria)?
- Should I stop using Xulane if I get a rash?
- I think I have an allergy to my antibiotic! What can I do to treat my infection?
- Can triamcinolone acetonide B be used to treat severe diaper rash on a little girl?
- What Vaccines do I need if I'm over 50?
- Jock Itch
- Poison Ivy
- How do I keep from getting Mpox (monkeypox)?
- Ticks: Why you should Avoid Bites
- I have Mpox: What should I do?
- Do I have Mpox (monkeypox)?
- Should I be Concerned about a Mpox Outbreak?
- Do I have Mpox?
- How do I get Mpox?
- Getting to the "Bottom" of Diaper Rash
- What is the Benadryl hat man?
- What are the most common skin conditions? (with photos)
- Zyrtec vs Claritin: Which is more effective for allergies?
- Allegra vs Claritin: Which is more effective for allergies?
- How Fast Does Benadryl Work? Onset Time and Duration
- Does Benadryl make you sleepy?
- Does Benadryl help with or cause anxiety?
- How fast does Dupixent work?
- Does Zyrtec cause weight gain?
- Diphenhydramine Hydrochloride vs Citrate: What's the difference?
- How does Dupixent work and what is its mechanism of action?
Related support groups
- Skin Rash (142 questions, 446 members)
- Hives (86 questions, 213 members)
- Urticaria (40 questions, 72 members)
- Dermatological Disorders (36 questions, 54 members)
- Dermatographism (1 questions, 7 members)
