Trigeminal Neuralgia
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is trigeminal neuralgia (TN)?
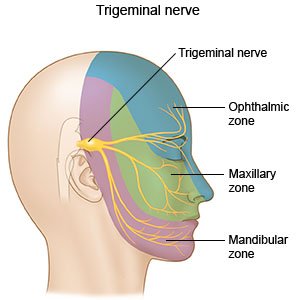
TN is a nerve disorder that causes sudden attacks of severe facial pain. You have a trigeminal nerve on each side of your face. The nerves allow you to feel pain, touch, and temperature changes in different areas of your face.
 |
What causes TN?
The exact cause of your TN may not be known. The following may increase your risk:
- Pressure from blood vessels in the head
- Pressure from a tumor or cyst
- Injury to the nerve from head trauma, surgery, or a stroke
- Damage from other diseases, such as multiple sclerosis (MS)
What can trigger a pain attack?
Most attacks are brought on by touching a trigger area on your face, such as from any of the following:
- Eating or drinking
- Smiling, yawning, or talking
- Shaving or washing your face
- Putting on makeup or combing your hair
- Wind or temperature changes
- Noise or lights
What are the signs and symptoms of TN?
TN causes sudden, sharp, or burning pain. It normally occurs on one side of your face but can occur on both sides. You can go days to years without any TN attacks. You may have any of the following:
- Pain attacks that last from 1 second up to 2 minutes and repeat every few minutes to hours
- Pain attacks that get worse over time
- Pain that is so severe you cannot eat, drink, or speak
- Spasms in your facial muscles during your pain attack
How is TN diagnosed?
Your healthcare provider will ask about your symptoms and when they started. Tell him or her if you have a family history of TN. Your provider will look at your head, neck, mouth, jaws, and teeth. A CT scan, MRI, or MRA pictures may be used to check bones, muscles, or blood vessels. You may be given contrast liquid to help the bones, muscles, or blood vessels show up better in the pictures. Tell the healthcare provider if you have ever had an allergic reaction to contrast liquid. Do not enter the MRI room with anything metal. Metal can cause serious injury. Tell the healthcare provider if you have any metal in or on your body.
Related medications
How is TN treated?
TN may go away on its own without treatment. If your TN is caused by another condition, your healthcare provider will also treat that condition.
- Medicines may be given to relieve or prevent your symptoms.
- A procedure may be used to destroy an area deep in your skull where nerve branches come together. A needle and tube are put through the base of your skull to reach this area. The nerve impulses that cause your pain attacks may be blocked. The nerve may be destroyed with medicine injections or may be frozen. Part of the nerve may also be removed. Medicine may be injected to make you lose feeling in the painful area.
- Surgery may be needed if other treatment does not help. Surgery may be used to separate the trigeminal nerve from the blood vessel pressing on it. The blood vessel may also be removed.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
How can I help manage TN?
- Keep your medicines nearby. Even if you have not had TN symptoms for a long time, keep your medicine nearby. If your symptoms return, contact your healthcare provider before you start taking your medicines again.
- Take your medicines as directed. Do not stop taking your medicines without talking with your healthcare provider first. You may have a bad reaction if you stop suddenly.
Where can I find more information?
- Trigeminal Neuralgia Association
2801 SW Archer Road
Gainesville , FL 32608
Phone: 1- 800 - 923-3608
Web Address: www.tna-support.org
Call your local emergency number (911 in the US) if:
- You are feeling so depressed you want to harm yourself.
- You are confused and cannot think clearly.
- You have sudden dizziness, or problems with movement, weakness, or numbness in your face.
When should I seek immediate care?
- You have a fever, stiff neck, or develop a rash or peeling skin.
- You are not eating or drinking, and you are losing weight.
- You have eye pain, eye numbness, or sudden vision or hearing changes.
When should I call my doctor?
- The medicines you are taking are not decreasing your symptoms.
- You feel worried or depressed and find it hard to do your daily activities.
- You have headaches, mouth sores, an upset stomach, or diarrhea.
- Your TN pain feels worse, different, or moves to another area of your face.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Trigeminal Neuralgia
Treatment options
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
