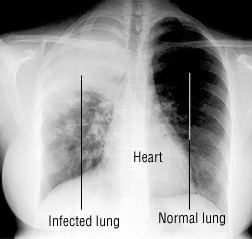
Pneumonia
Medically reviewed by Drugs.com. Last updated on Feb 23, 2024.
What is pneumonia?

Pneumonia is an infection of the lungs. Almost all cases of pneumonia are caused by viral or bacterial infections.
When pneumonia is first diagnosed, there often is no way to be sure if the infection is caused by a virus or bacteria. Therefore your doctor will need to treat it with antibiotics.
There are multiple antibiotics that treat pneumonia. The initial choice of drug(s) is made based on the category of pneumonia you most likely have. The two major categories are community acquired pneumonia (CAP) and health care associated pneumonia (HCAP).
Community acquired pneumonia refers to pneumonia in a person that has not recently stayed in the hospital or a nursing home. The most common bacterial cause of CAP is Streptococcus pneumoniae.
Health care associated pneumonia refers to pneumonia that develops in a person that is in the hospital now or has recently been in the hospital or a nursing home. These pneumonias tend to be more serious. The organisms found in a hospital often become resistant to many antibiotics. Also hospitalized patients are often weakened by other illnesses and are less able to fight off the infection.
A type of pneumonia called aspiration pneumonia develops when chemical irritants and bacteria from the mouth or stomach are inhaled into the lungs. It is more common in people who have had strokes or a neurological condition that results in difficulty controlling their swallowing reflexes. People who are unconscious as a result of alcohol or other drug overdose are also at high risk of aspiration pneumonia.
In people with compromised immune systems, the organisms that cause pneumonia are different than those seen in the other types of pneumonia.
Symptoms of pneumonia
Most types of pneumonia cause fever, cough with sputum (coughed-up mucus), shortness of breath and fatigue. In older patients, fatigue or confusion can be the only or most noticeable symptom. In viral pneumonia, a dry cough without sputum is more common.
Diagnosing pneumonia
Your doctor first will ask about your symptoms. During the physical exam, your doctor will check to see if you are breathing rapidly. He or she also will look for confusion and a purplish hue in your lips, fingernails or hands because these symptoms can indicate that you have low levels of oxygen in your blood. Using a stethoscope, a health care professional can listen through your back for abnormal sounds from the lungs. The diagnosis of pneumonia most often is confirmed by a chest X-ray.
|
|
Your doctor may order blood tests to look for an elevation of infection-fighting white blood cells and to make sure your electrolytes and kidney function are normal. A sample of your sputum or blood may be sent to a laboratory to help identify the specific cause of your pneumonia. Identifying the infectious organism can help your doctor to choose the best antibiotic to treat the infection. Even though most of the time no single germ is identified, the pneumonia still can be treated successfully with antibiotics.
Expected duration of pneumonia
How long pneumonia lasts can vary from a few days to a week or longer, depending on how early you start antibiotics and what other medical problems you may have. Antibiotic treatment for pneumonia usually lasts from 5 to 14 days. Many people find that it takes a few weeks to several weeks to regain the level of energy they had before the pneumonia.
Preventing pneumonia
Vaccination against the most common bacterial cause of pneumonia called S. pneumoniae helps protect adults age 65 and older and those younger people at increased risk of pneumonia from developing this infection. High risk people includes those with:
- lung disease including asthma
- heart disease
- liver disease
- kidney disease
- a cochlear implant
- a damaged spleen or no spleen
- certain types of cancer or undergoing cancer treatment
- a weakened immune system.
Children younger than age 5 should receive the full vaccination series. Although it is used mostly to reduce the risk of meningitis and ear infections in children, it also lowers the risk of pneumonia.
Everyone should stay current with their age appropriate vaccination schedule to prevent other infections, including influenza, respiratory syncytial virus (RSV), and COVID-19.
Drugs used to treat this and similar conditions
Treatment options
The following list of medications are related to or used in the treatment of this condition.
Treating pneumonia
The main treatment for pneumonia is one or more antibiotics. A younger or healthier person can be treated safely with antibiotics at home and can feel better in a few days. Some people are at higher risk of complications and may need to be hospitalized. They include people who are older than 60 or have other diseases such as heart failure, active cancer, chronic kidney disease or chronic obstructive pulmonary disease (COPD).
In addition to antibiotics, other treatments for pneumonia include rest, adequate fluid, and supplemental oxygen if needed to maintain a safe blood oxygen level.
When to call a professional
A simple cold or bronchitis caused by a virus can share many of the same symptoms as pneumonia. Pneumonia is possible when your cough produces sputum with a green or brown color, you are having shaking chills and/or high fever, or you are having trouble breathing. In these cases, you should promptly call your doctor.
Also, if you have been diagnosed with a cold or bronchitis and symptoms are getting worse or persist after a week, you should call your doctor's office for another evaluation.
Prognosis
Most pneumonia is treated successfully, especially if antibiotics are started early. Pneumonia can be fatal. The very old and frail, especially those with many other medical conditions, are most vulnerable.
Pneumonia usually does not cause permanent damage to the lungs. Rarely, pneumonia causes infected fluid to collect around the outside of the lung, called an empyema. The empyema may need to be drained with a special tube or surgery. With aspiration pneumonia, the affected lung may develop a lung abscess that needs many weeks of antibiotic therapy.
Additional info
American Lung Association
https://www.lungusa.org/
National Heart, Lung, and Blood Institute (NHLBI)
https://www.nhlbi.nih.gov/
Learn more about Pneumonia
Treatment options
Care guides
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.