Retropubic Prostatectomy
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
WHAT YOU NEED TO KNOW:
A retropubic prostatectomy is surgery to remove your prostate gland.
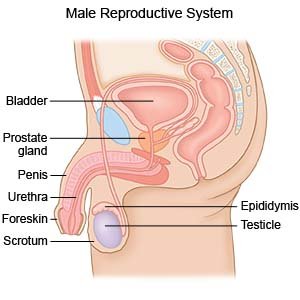 |
HOW TO PREPARE:
Before your surgery:
- Tell your surgeon about all medicines you currently take. He or she will tell you if you need to stop taking any medicine before surgery, and when to stop. He or she will tell you which medicines to take or not take on the day of surgery.
- You may need blood and urine tests and a transrectal ultrasound.
- You will need to be on a clear liquid diet the day before your surgery. You may drink clear liquids, including water, broth, apple juice, or lemon-lime soft drinks. You may also suck on ice chips or eat gelatin.
The night before your surgery:
You may be told not to eat or drink anything after midnight. You may need to drink a medicine that cleans out your bowel.
The day of your surgery:
- You or a close family member will be asked to sign a legal document called a consent form. It gives healthcare providers permission to do the procedure or surgery. It also explains the problems that may happen, and your choices. Make sure all your questions are answered before you sign this form.
- You may be given an enema (liquid medicine put in your rectum) to help clean out your bowel.
- You may need to take antibiotic medicine to help prevent an infection caused by bacteria. You may get antibiotic medicine before and after your surgery.
- An IV will be placed into a vein. You may be given medicine or liquid through the IV.
- Anesthesia is medicine to make you comfortable during the surgery. Healthcare providers will work with you to decide which anesthesia is best for you:
- General anesthesia will keep you asleep and free from pain during surgery. Anesthesia may be given through your IV. You may instead breathe it in through a mask or a tube placed down your throat. The tube may cause you to have a sore throat when you wake up.
- Spinal anesthesia is injected into the spine to numb you below the waist. You will remain awake during the surgery.
WHAT WILL HAPPEN:
What will happen:
- A catheter (long, thin tube) will be inserted in your urethra and into your bladder to drain your urine. An incision will be made in your abdomen below your belly button. Your surgery may be done with a laparoscope, through small cuts in your abdomen. A laparoscope is a long metal tube with a light and camera on the end. Your surgeon may use a robot-assist device if a laparoscope is used during surgery. Before your prostate gland is removed, lymph nodes may be removed and sent to a lab to test for cancer.
- Your surgeon will cut your urethra below the prostate gland and remove the catheter. Stitches will be put into your urethra to help stop bleeding. Your prostate gland will be cut away from your bladder neck and removed through the cut in your abdomen. The bladder neck is where the bottom of your bladder meets your urethra. Your bladder neck and urethra will be sewn back together, and a new catheter will be put in. Liquid will be flushed through the catheter to remove blood and blood clots from your bladder. A drain will be placed in your incision to remove blood and fluid. Your incision will be closed with stitches. The area will be covered with a bandage.
After your surgery:
You will be taken to a room to rest until you are awake. Healthcare providers will check your drain and catheter for urine and blood. You may be given medicine to decrease or take away your pain. Do not get out of bed until your healthcare provider says it is okay. Once healthcare providers see that you are not having any problems, you will be taken to your hospital room.
CONTACT YOUR HEALTHCARE PROVIDER IF:
- You have a fever.
Seek Care Immediately if
- You are urinating very little or not at all.
- You have new or increased abdominal or pelvic pain.
Risks
- During surgery, your nerves, bowel, rectum, and other organs and tissues may be damaged. Blood vessels may be damaged, causing you to bleed more than expected. You may need a blood transfusion if this happens. After surgery, blood may collect in your pelvic area (between your legs and hips) that needs draining. You may have pain, and you may get an infection in your wound or urinary tract. Your urethra or bladder neck may become narrow and block the flow of your urine. Urine may leak from your bladder and collect in nearby areas, such as your abdomen. You may get a hernia in your lower abdomen. A hernia occurs when part of your intestine pushes through weak muscle in your abdomen.
- After surgery, you may leak urine and bowel movements. Urine leakage may be short-term or permanent. You may have trouble having an erection. You may have pain or trouble ejaculating. You may get a blood clot in your arm or leg. The clot may travel to your heart or brain and cause life-threatening problems, such as a heart attack or stroke. Even with surgery, your cancer may not be completely removed, the cancer may spread, or it may come back.
Related medications
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
