Peripheral Thrombolysis
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
AMBULATORY CARE:
What you need to know about peripheral thrombolysis:
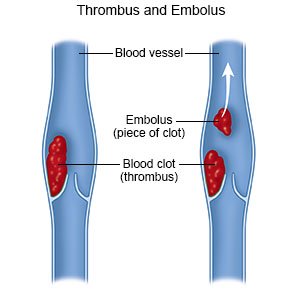
Peripheral thrombolysis is a procedure to break up or dissolve a blood clot in your arm or leg. The clot may be removed with a device during the procedure. You may need thrombolysis to remove a clot quickly so it does not break free. You may need the procedure to remove a blood clot from deep veins, called deep vein thrombosis (DVT). A DVT usually happens in a leg, but it can also happen in an arm. A DVT can also break free. A clot that breaks off in your arm or leg may travel to your lungs. This can be life-threatening.
 |
How to prepare for the procedure:
- Your healthcare provider will tell you how to prepare. Your provider may tell you not to eat or drink anything after midnight on the day of your procedure. Arrange to have someone drive you home when you are discharged.
- Tell your provider about all your current medicines. Your provider will tell you if you need to stop any medicine for the procedure, and when to stop. Your provider will tell you which medicines to take or not take on the day of your procedure.
- Tell your provider about any allergies you have, including to anesthesia, contrast liquid, or medicines. You may be given contrast liquid before or during the procedure to help your healthcare provider see the clot better. You may be given antibiotics to prevent an infection caused by bacteria.
What will happen during the procedure:
- You will be given local anesthesia to numb the procedure area. With local anesthesia, you may still feel pressure or pushing, but you should not feel any pain.
- Your healthcare provider will inject medicine into your IV that will help dissolve or break up the clot. It is most often given into a vein, but it may be given into an artery. A catheter is guided by x-ray so it is near the blood clot.
What to expect after the procedure:
Healthcare providers will apply pressure on the procedure area to stop any bleeding. You will be monitored closely for any problems. Do not get out of bed until your healthcare provider says it is okay. You will then be able to go home or be taken to your hospital room.
- The catheter may be left in place if the medicine needs to continue to break up the clot. You will need to stay in the hospital if the catheter is left in place. Your healthcare provider will need to do the thrombolysis again to remove the rest of the clot. You will be told not to move the leg or arm used for the procedure while the catheter is in place. You will need to lie still. Tell your healthcare provider if lying flat starts to cause back discomfort. If there is no bleeding, your provider may help you roll onto your side. A Foley catheter may be placed in your bladder. This catheter allows urine to drain from your bladder into a collection bag.
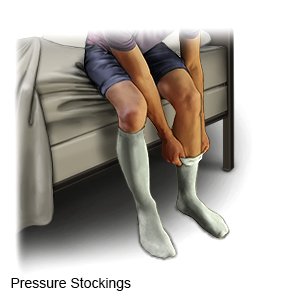
- You may need to wear a compression device if your procedure was for a leg clot. Examples include pressure stockings, intermittent pneumatic compression (IPC), and sequential compression devices (SCD). Compression helps keep blood from pooling in your leg veins. You may need to continue wearing a compression device after you leave the hospital. Your provider will tell you when to start wearing the device and how long to wear it.
- You will be helped to walk around the same day of your procedure, or the day after. Movement will help prevent blood clots. You may also be given exercises to do in bed. Do not get out of bed on your own until your healthcare provider says you can. Ask before you get up the first time. You may need help to stand up safely. When you are able to get up on your own, sit or lie down right away if you feel weak or dizzy. Then press the call button to let someone know you need help.
- Medicines:
- Anticoagulants are a type of blood thinner medicine that helps prevent clots. Anticoagulants may cause you to bleed or bruise more easily.
- Antiplatelets help prevent blood clots. This medicine makes it more likely for you to bleed or bruise.
Risks of peripheral thrombolysis:
Thrombolysis increases your risk for bleeding. You may have increased nosebleeds or bleeding from your gums. You may also have bleeding in your stomach or brain. Bleeding can become severe and life-threatening. You may have an allergic reaction to the contrast liquid or to the medicine used to break up the clot.
Call your local emergency number (911 in the US) or have someone call if:
- You feel lightheaded, short of breath, and have chest pain.
- You cough up blood.
Seek care immediately if:
- Your arm or leg feels warm, tender, and painful. It may look swollen and red.
- The procedure area does not stop bleeding even after you apply firm pressure for 10 minutes.
- The leg or arm used for your procedure is numb, painful, or changes color.
- The bruise at your catheter area gets bigger or becomes swollen.
- You have purple spots or blisters on your skin.
Related medications
Call your doctor or hematologist if:
- You have a fever.
- You have a new skin rash and itching.
- You feel weak, lightheaded, or faint.
- You have new swelling around your eyes.
- You have questions or concerns about your condition or care.
Medicines:
- Antiplatelets , such as aspirin, help prevent blood clots. Take your antiplatelet medicine exactly as directed. These medicines make it more likely for you to bleed or bruise. If you are told to take aspirin, do not take acetaminophen or ibuprofen instead.
- Blood thinners help prevent blood clots. Clots can cause strokes, heart attacks, and death. Many types of blood thinners are available. Your healthcare provider will give you specific instructions for the type you are given. The following are general safety guidelines to follow while you are taking a blood thinner:
- Watch for bleeding and bruising. Watch for bleeding from your gums or nose. Watch for blood in your urine and bowel movements. Use a soft washcloth on your skin, and a soft toothbrush to brush your teeth. This can keep your skin and gums from bleeding. If you shave, use an electric shaver. Do not play contact sports.
- Tell your dentist and other healthcare providers that you take a blood thinner. Wear a bracelet or necklace that says you take this medicine.
- Do not start or stop any other medicines or supplements unless your healthcare provider tells you to. Many medicines and supplements cannot be used with blood thinners.
- Take your blood thinner exactly as prescribed by your healthcare provider. Do not skip a dose or take less than prescribed. Tell your provider right away if you forget to take your blood thinner, or if you take too much.
- Take your medicine as directed. Contact your healthcare provider if you think your medicine is not helping or if you have side effects. Tell your provider if you are allergic to any medicine. Keep a list of the medicines, vitamins, and herbs you take. Include the amounts, and when and why you take them. Bring the list or the pill bottles to follow-up visits. Carry your medicine list with you in case of an emergency.
Care for the procedure area as directed:
- Keep the procedure area clean and dry. Your healthcare provider will tell you when you can bathe. You will need to keep the bandage in place and dry for a day or two after your procedure. Cover the bandage with a plastic bag and tape the opening around your skin to keep water out.
- Wash the area with soap and water when it is okay to bathe without a bandage.
- Check the area each day for signs of infection. Examples include redness, swelling, and pus. Dry the area and put on new, clean bandages as directed. Change your bandage if it gets wet or dirty.
Watch for bleeding and bruising:
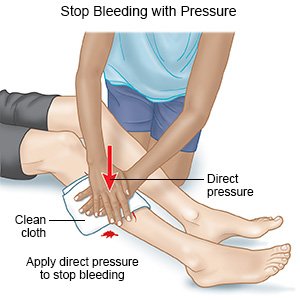
It is normal to have a bruise and soreness where the catheter went in. Contact your healthcare provider if your bruise gets larger. If the procedure area bleeds, use your hand to put pressure on the bandage. If you do not have a bandage, use a clean cloth to put pressure over and just above the area. Seek care immediately if the bleeding does not stop within 10 minutes.
 |
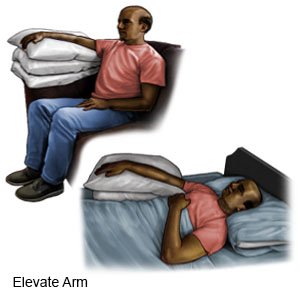
Keep your leg or arm elevated as directed:
Keep the leg or arm that had the blood clot above the level of your heart when you are sitting. Prop the arm or leg on pillows to keep it elevated comfortably. Ask how long to keep your leg elevated each day. You will need to balance elevation with movement to prevent blood clots.
 |
 |
Prevent another blood clot:
- Do not smoke. Nicotine and other chemicals in cigarettes and cigars can cause blood vessel and lung damage. Ask your healthcare provider for information if you currently smoke and need help to quit. E-cigarettes or smokeless tobacco still contain nicotine. Talk to your healthcare provider before you use these products.
- Limit alcohol. Do not drink alcohol for 24 hours after your procedure. Then limit alcohol to 1 drink a day if you are female or 2 drinks a day if you are male. A drink is 12 ounces of beer, 5 ounces of wine, or 1½ ounces of liquor.
- Stay active. Your healthcare provider will tell you when it is safe to drive and start doing your other normal daily activities. An active lifestyle can help prevent blood clots. Try to get at least 30 minutes of activity on most days of the week. If you sit most of the day for work, stand or walk around every half hour. After a future injury or illness, try to become active again as soon as possible. Activity can also help you manage your weight. Too much body weight can put pressure on your leg veins and cause blood to pool. This increases your risk for another blood clot.

- Manage other health conditions. Follow your healthcare provider's directions to manage health conditions that can cause a blood clot. Examples are high cholesterol and diabetes.
- Drink liquids as directed. Liquids will help flush out the contrast material used during your procedure. Liquid can also help prevent blood clots. Ask your healthcare provider how much liquid to drink each day and which liquids are best for you.
Follow up with your doctor or hematologist as directed:
You may need to be checked for blood clots for up to 3 years after treatment. Write down your questions so you remember to ask them during your visits.
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Learn more about Peripheral Thrombolysis
Care guides
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
