Lower Gastrointestinal Endoscopic Ultrasonography
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
WHAT YOU NEED TO KNOW:
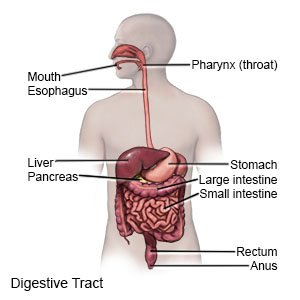
A lower gastrointestinal endoscopic ultrasound is used to help diagnose and treat diseases that affect the lower gastrointestinal (GI) tract. The lower GI tract includes some parts of the small intestine, the colon, and the rectum.
 |
HOW TO PREPARE:
The week before your procedure:
- Arrange to have someone drive you home after the procedure.
- Tell your provider about all medicines you currently take. He or she will tell you if you need to stop any medicine for the procedure, and when to stop. He or she will tell you which medicines to take or not take on the day of the procedure.
- Tell your provider if you had similar procedures and when they were done. These may include a colonoscopy, sigmoidoscopy, or upper or lower GI x-rays. Tell him or her if you had any surgeries of your GI tract.
- You may need to have blood tests, urine tests, or x-rays before your procedure.
The night before your procedure:
- You may be told not to eat or drink anything after midnight.
- You may need an enema the night before your procedure. This is liquid put into your rectum to help empty your bowel.
The day of your procedure:
- You or a close family member will be asked to sign a legal document called a consent form. It gives healthcare providers permission to do the procedure or surgery. It also explains the problems that may happen, and your choices. Make sure all your questions are answered before you sign this form.
- Take only the medicines your healthcare provider told you to take.
- Healthcare providers may insert an intravenous tube (IV) into your vein. A vein in the arm is usually chosen. You may be given liquids or medicine through the IV.
- An anesthesiologist will talk to you before your surgery. You may need medicine to keep you asleep or numb an area of your body during surgery. Tell healthcare providers if you or anyone in your family has had a problem with anesthesia in the past.
WHAT WILL HAPPEN:
What will happen:
- You will be asked to lie on your left side and raise one or both knees toward your chest. Your healthcare provider will examine your anus and use a finger to perform a digital rectal exam to check your rectum.
- The echoendoscope will be placed into your anus. It will then be passed through the rectum and into the large intestine. You may feel some pressure or discomfort. Your provider will slowly move the scope forward while he or she watches its movement on a screen. He or she will also take pictures. Tissue samples may be taken and sent to a lab for tests. Your provider may also treat any conditions you have.
After your procedure:
You will be taken to a room to rest until you are fully awake. You will be monitored closely for any problems. Do not get out of bed until your healthcare provider says it is okay. You may be given medicine to make it easier for you to have a bowel movement. You may need this medicine to treat or prevent constipation.
CONTACT YOUR HEALTHCARE PROVIDER IF:
- You have a fever.
- You get a cold or the flu.
- You have constipation, and the medicine is not helping to empty your bowel.
- You have questions or concerns about your procedure.
Seek Care Immediately if
- You are not able to eat or drink.
- You have blood in your bowel movement.
- Your abdomen becomes tender and hard.
- Your vomit has blood or bile in it.
Risks
You may have bleeding, an abnormal heartbeat, high blood pressure, or trouble breathing. Your small intestines, large intestines, or rectum may get injured because of increased pressure from the scope.
Related medications
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Learn more about Lower Gastrointestinal Endoscopic Ultrasonography
Care guides
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
