Intestinal Metaplasia
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is intestinal metaplasia (IM)?
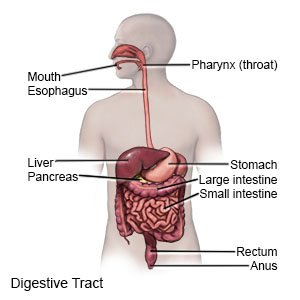
IM is a condition that changes the cells that line your stomach or esophagus. The cells are changed into or replaced by cells that line your intestines. When IM happens in the esophagus, it is called Barrett esophagus. IM is a precancer lesion. This means it is not cancer yet, but it may develop into cancer over time. IM can be a sign that you are at a very high risk for gastric (stomach) or esophageal cancer. The type of cancer depends on where you have IM.
 |
What causes or increases my risk for IM?
Bacteria called Helicobacter pylori (H. pylori) are thought to change food into chemicals that change the cells. An H. pylori infection does not always cause IM, but it increases the risk. The following are other factors that can increase your risk for IM:
- Chronic gastroesophageal reflux disease (GERD)
- Smoking cigarettes, or being around secondhand smoke
- A family history of stomach cancer
- Large amounts of sodium (salt) or alcohol
- Age older than 60 years, or being male
- Regularly eating smoked, salt-cured, or pickled foods such as bacon, ham, or corned beef
- Not eating many fruits or vegetables
What are the signs and symptoms of IM?
You may not have any signs or symptoms. You may develop certain signs or symptoms if you have H. pylori or GERD:
- Dull or burning pain in your stomach or throat
- Nausea, vomiting, bloating, or burping
- Loss of appetite or weight loss
- Pain at night or with an empty stomach
- Bitter or acid taste in your mouth
- Dry cough
- Trouble swallowing or pain with swallowing
- Hoarseness or sore throat
- Frequent burping or hiccups
- Feeling of fullness soon after you start eating
How is IM diagnosed?
Your healthcare provider may find IM during tests for another condition. Based on your age and risk factors, your provider may recommend IM screening. This means checking for IM before you have any signs or symptoms. Tests may be used to check for IM, or for an H. pylori infection. Tell your provider about if you have any symptoms of IM, and how long you have had them. Tell him or her about any medical conditions you have or medicines you take. You may also need any of the following:
- Endoscopy is a procedure that uses a scope to see the inside of your stomach. A scope is a soft, flexible tube with a light and tiny camera on the end. It is passed down your throat and into your stomach. Samples of your stomach tissue may be removed and sent to a lab to be tested.
- A urea breath test may be used to test for H. pylori infection. You will swallow pudding, liquid, or a capsule that contains a chemical. Then you will breathe into a container. Your breath sample will be tested for a reaction to the chemical that confirms H. pylori infection.
- A blood or bowel movement samples may be sent to a lab to test for H. pylori infection.
Related medications
How is IM treated?
Treatment may be given for the cause of your IM, or for any symptoms you are having. Your healthcare provider may recommend other treatment than the following if you have Barrett esophagus.
- Treatment for an H. pylori infection may be recommended. Treatment may slow or stop cells from changing into intestine cells. H. pylori treatment may include any of the following:
- Antibiotics help kill the bacteria. You may need to take this medicine for 10 to 14 days. Your healthcare provider will prescribe at least 2 antibiotics at the same time.
- Antiulcer medicines help decrease the amount of acid that is normally made by the stomach. These help relieve pain and heal or prevent ulcers.
- Bismuth is a liquid or tablet that may be used to decrease heartburn, upset stomach, or diarrhea. It may also decrease swelling in your stomach and help kill the infection if other medicines do not work. It also protects ulcers from stomach acid so they can heal.
- Medicines may be given to decrease stomach acid.
- Endoscopy may be used to remove certain IM lesions. Ask your healthcare provider for more information about endoscopy. He or she will tell you if endoscopy is right for you, if it is available. This may depend on your age, general health, and the size of any lesions you have.
What can I do to manage IM?
The following can help you prevent or manage symptoms. You may also help lower your risk for stomach or esophageal cancer with healthy lifestyle choices. Examples include eating healthy foods, exercising, and not smoking. Talk to your healthcare provider if you have questions about any of the following:
- Eat healthy foods. Healthy foods include fruit, vegetables, whole-grain breads, low-fat dairy products, beans, lean meats, and fish. Limit or do not eat foods such as salami, corned beef, ham, and bacon. Do not have foods or drinks that may increase heartburn if you have GERD. Examples include fried or fatty foods, spicy foods, onions, tomato-based foods, juice, and soft drinks.
- Do not eat large meals. When you eat a lot of food at one time, your stomach needs more acid to digest it. Eat 6 small meals each day instead of 3 large meals, and eat slowly. Do not eat meals 2 to 3 hours before bedtime.
- Drink liquids as directed. Liquids help your digestive system work correctly. Ask how much liquid to drink each day and which liquids are best for you.
- Exercise as directed. Exercise can help increase your energy level and appetite. Ask your healthcare provider how much exercise you need and which exercises are best for you.

- Elevate the head of your bed if you have GERD. Place 6-inch blocks under the head of your bed frame. You may also use more than one pillow under your head and shoulders while you sleep.
- Do not smoke. Nicotine can damage blood vessels and make it more difficult to manage IM. Smoking also increases your risk for new or returning cancer and delays healing after treatment. Do not use e-cigarettes or smokeless tobacco in place of cigarettes or to help you quit. They still contain nicotine. Ask your healthcare provider for information if you currently smoke and need help quitting.
- Do not drink alcohol. Alcohol can cause more stomach damage. Alcohol also increases the risk for stomach cancer.
When should I seek immediate care?
- You have bloody bowel movements, bloody vomit, or vomit that looks like coffee grounds.
- You have sudden, sharp stomach pain that does not go away or spreads to your back.
- You have trouble breathing after you vomit.
- You have trouble swallowing, or pain with swallowing.
When should I call my doctor?
- Your symptoms do not improve with treatment.
- You feel full after eating only a small amount of food.
- You lose weight without trying.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
