Diabetes and your Skin
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What do I need to know about diabetes and my skin?
Diabetes can affect every part of your body, including your skin. Diabetes that is not well controlled can damage blood vessels and nerves. Damage to blood vessels can make it hard for blood to flow to tissues and organs. A lack of blood flow to your skin can cause sores that are hard to heal. People with diabetes also have a higher risk for bacterial skin infections. Skin sores and infections can be hard to heal, or become life- or limb-threatening, if not treated early.
What are common skin changes that I may see?
- Dry, flaky skin
- Skin tags on your eyelids, neck, or underarms
- Yellow color of your palms, soles of your feet, and nails
- Dark patches on your shins
- A constant redness of your face and neck
- Thick skin on the back of your hands and the top of your feet
- A smooth, dark thickness in the skin on your neck, groin, face, and underarms
How can I prevent skin sores?
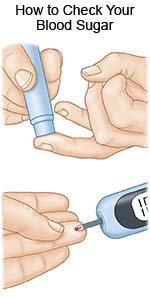
- Keep your blood sugar within the target range. Your diabetes care team provider will tell you what your blood sugar levels should be. High blood sugar levels increase your risk for skin infections and poor wound healing.
- Keep your skin from getting too dry. Do not take hot baths or showers. Use moisturizing soap. Apply moisturizing lotion after baths or showers, especially in cold, dry weather. When you scratch dry, itchy skin, you can cause your skin to be open to infection. Use a humidifier to keep air in your home from being dry.
- Apply lotion or a moisturizer on your dry feet. Ask your care team provider what lotions are best to use. Do not put lotion or moisturizer between your toes. Moisture between your toes could lead to skin breakdown.
- Keep areas where skin touches skin dry. Use talcum powder in areas such as armpits, groin, or under your breasts. Moisture in these areas can cause a fungal infection.
- Treat cuts immediately. Clean minor cuts with soap and water. Cover them with sterile gauze.
Related medications
Treatment options
The following list of medications are related to or used in the treatment of this condition.
When should I call my doctor or diabetes care team provider?
- You get a severe burn or cut.
- You have a sore that is painful, warm to the touch, or has redness around it.
- Your sore does not get better or seems to get worse.
- You have a fever.
- Your blood sugar levels continue to be higher than they should be.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Diabetes and your Skin
- Diabetes Medications and Alcohol Interactions
- FDA-Approved Weight Loss Drugs: Can They Help You?
- OneTouch Blood Glucose Meters
- Side Effects of Weight Loss Drugs
- Top 10 Diabetes Treatments You May Have Missed
- Which Drugs Cause Weight Gain?
Treatment options
Care guides
- Diabetic Hyperglycemia
- How to Draw Up Insulin
- Type 1 Diabetes in Adults: New Diagnosis
- Type 1 Diabetes in Children
- Type 2 Diabetes in Adults: New Diagnosis
- Type 2 Diabetes in Children
Symptoms and treatments
Medicine.com guides (external)
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
