Decision Aid for Hip Osteoarthritis
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
AMBULATORY CARE:
What you need to know about decisions for hip osteoarthritis:
You can help make decisions about being screened for osteoarthritis. You can also help plan treatment if osteoarthritis is found with screening, or you develop it. Osteoarthritis screening is a test done to find osteoarthritis early. Screening is different from diagnosis because screening is used when you first start to have signs or symptoms. This means management or treatment can start early to help prevent joint damage. Treatments include medicine and surgery, but you can also manage osteoarthritis with lifestyle changes.
What you need to know about hip osteoarthritis:
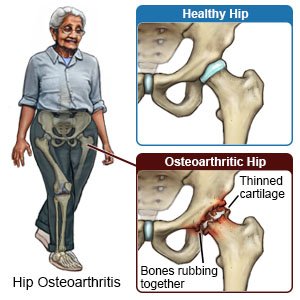
- Osteoarthritis is a condition that causes tissue between bones to wear away. This can happen slowly over time or quickly because of an injury. The bones rub together when you move. This causes pain and can limit mobility.
- Osteoarthritis is the most common form of arthritis. About 30 million people in the US have osteoarthritis.
- Osteoarthritis is more likely if you are female than if you are male.
- Talk to your healthcare provider if you think you have signs or symptoms of osteoarthritis. Examples include joint pain with movement, tender or stiff joint, or a grating feeling with movement. You may also feel hard lumps around the joint, called bone spurs.
 |
How to tell if you are a good candidate for osteoarthritis screening:
Screening may be helpful for you if any of the following is true:
- Age 50 years or older
- Overweight or obesity
- Work that involves putting repeated stress on your hip joint
- A family history of osteoarthritis
- A joint injury, even if it happened many years ago
- Being born with a joint or cartilage problem
- Mild signs or symptoms of osteoarthritis
- Symptoms affect your ability to do your daily activities
How osteoarthritis screening is done:
No test is used to diagnose osteoarthritis. Your healthcare provider will check the following:
- How much pain, tenderness, or inflammation you have in the joint
- Range of motion in the joint (how far it can move in every direction)
- Your ability to walk without pain, or how your symptoms changed the way you walk
- The strength of muscles around the joint
Benefits and risks of screening:
Talk with your healthcare provider about the risks and benefits of screening:
- Benefits include finding osteoarthritis early, when you can manage the condition. You may be able to slow the progress of joint damage by losing weight or exercising more. You can also help make a treatment plan that you can change over time as needed.
- Risks include a false belief that you will not develop osteoarthritis. Your screening test may find that you do not have osteoarthritis. This can be because signs and symptoms are mild. You can still develop more severe signs and symptoms over time. It is important to talk with your healthcare provider about how often to have screening.
Related medications
Questions to ask your healthcare provider to help you make decisions about screening:
- How high is my risk for osteoarthritis?
- How often do I need to have screening?
- Where is the screening done?
- Do I need to do anything to get ready to have screening?
What happens after you have osteoarthritis screening:
You will meet with your healthcare provider to go over the results of your screening. You, your family or caregiver, and your healthcare provider can talk about your treatment options. Together you can decide which treatment is right for you. You may need more tests to diagnose anything that showed up on the screening test. Common tests include an x-ray or CT scan to check the amount of tissue between bones or to find bone spurs.
How osteoarthritis is treated, and the benefits of treatment:
- Lifestyle changes include weight loss and exercise. Weight loss can help take pressure off the joint. Exercise can help build muscles around the joint. This helps build stability and strength. Your healthcare provider, a dietitian, or a physical therapist can help you make nutrition and exercise plans.
- Devices can help you stay active and relieve your symptoms. Shoe inserts support your joint and take pressure off the joint. This can help reduce pain that happens when you stand or walk. A cane can help take weight off your hip as you walk.
- Medicines include acetaminophen, NSAIDs, and certain antidepressants. Acetaminophen and NSAIDs, such as ibuprofen, help relieve pain. NSAIDs also help reduce inflammation. Both medicines are available without a prescription. Do not take these medicines without talking to your healthcare provider first. Stronger forms of these medicines are available with a prescription. Antidepressants are only available with a prescription.
- Therapy includes physical and occupational therapy. A physical therapist can help you strengthen muscles around the joint and increase your range of motion. An occupational therapist can help you find easier ways to do your daily activities. For example, you may be shown how to sit or stand in a way that takes pressure off your hip.
- Steroid medicine may be injected into the hip area if your symptoms become worse. This can reduce inflammation and relieve pain.
- Surgery may be done if other treatments do not work and your symptoms become severe. Surgery called arthroplasty is used to remove the damaged joint and replace it with an artificial joint.
Risks of osteoarthritis treatment:
- Lifestyle changes will not reverse the damage to the tissue between your joints. It will only prevent symptoms from getting worse. It may also be difficult to exercise if you have severe hip pain.
- Medicines must be taken in limited doses. Acetaminophen can cause liver damage, and NSAIDs can cause kidney damage. The pain may come back before you can take another dose. Antidepressants can cause certain side effects.
- Steroid injections are usually limited to about 4 each year. This is because the medicine can cause joint damage over time. Steroids can also increase your risk for other infections, cause changes in your mood, and increase blood sugar levels.
- Surgery increases your risk for an infection or blood clot. An artificial joint may wear out over time. It may also become loose. It will need to be replaced if it wears out or comes loose.
Questions to ask your healthcare provider to help you make decisions about treatment:
- How will I know if signs and symptoms are becoming severe enough to need treatment?
- Am I a good candidate for steroid injections?
- Am I a good candidate for hip replacement surgery?
- How long is recovery from hip replacement surgery?
- If the treatment does not work, what other treatment choices do I have?
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
