CABG (Coronary Artery Bypass Graft)
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What do I need to know about coronary artery bypass graft (CABG) surgery?
A CABG is open heart surgery to clear blocked arteries in your heart. CABG surgery improves blood flow to your heart by bypassing (sending blood around) the blocked part of an artery. This restores blood flow to your heart and helps prevent a heart attack.
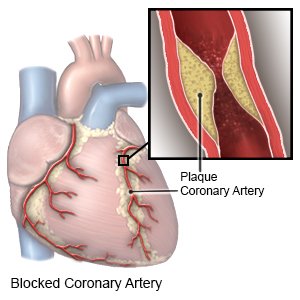 |
How do I prepare for CABG surgery?
- Your surgeon will talk to you about how to prepare for surgery. He or she may tell you not to eat or drink anything after midnight on the day of your surgery. Arrange to have someone drive you home after you are discharged.
- Tell your surgeon about all your current medicines. He or she will tell you if you need to stop any medicine for surgery, and when to stop. He or she will tell you which medicines to take or not take on the day of surgery.
- You may be able to donate your own blood before surgery. This is called autologous blood donation. You may also ask a family member or friend with the same blood type to donate blood for you. This is called directed blood donation.
- Tell your surgeon about any allergies you have, including to medicines or anesthesia.
What will happen during CABG surgery?
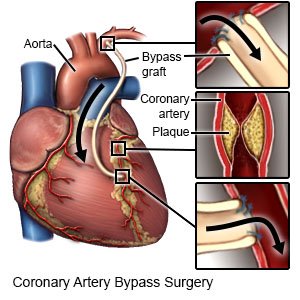 |
- You will be given general anesthesia to keep you asleep and free from pain during surgery. Your surgeon will make an incision in your chest. He or she will cut or spread your ribcage apart to reach your heart. He or she may safely slow your heartbeat to attach the graft. Your heart may be connected to a bypass machine. This machine pumps blood to your body and keeps blood out of your heart during surgery.
- Your surgeon will make a separate incision to remove the graft. The graft is a piece of healthy blood vessel taken from somewhere else in your body, such as your leg. He or she will sew the graft vessel to your artery above and below the block. This allows blood to flow around the blocked area to your heart muscle. After surgery, the blood will be allowed to flow through your heart. Your surgeon will close the incision where the graft came from with stitches and cover it with bandages. Your chest incision will be closed. A bandage will cover your incisions to keep the area clean and dry to prevent infection.
Related medications
What should I expect after CABG surgery?
- A chest tube is placed during surgery to drain air and extra fluid from around your lungs. This allows your lungs and heart to work properly. The chest tube is attached to a container. Call a healthcare provider right away if the tube comes apart from the container. Let the provider know if the tubing gets bent, twisted, or the tape comes loose. The chest tube may be removed 24 to 48 hours after surgery. Your provider will monitor how much fluid collects and decide when to remove it.
- A Foley catheter is a tube put into your bladder to drain urine into a bag. Keep the bag below your waist. This will prevent urine from flowing back into your bladder and causing an infection or other problems. Also, keep the tube free of kinks so the urine will drain properly. Do not pull on the catheter. This can cause pain and bleeding, and may cause the catheter to come out.
- Extra oxygen may be needed if your blood oxygen level is lower than it should be. You may get oxygen through a mask placed over your nose and mouth or through small tubes placed in your nostrils. Ask your healthcare provider before you take off the mask or oxygen tubing.
- You may need to wear pressure stockings or inflatable boots after surgery. The stockings are tight and put pressure on your legs. The boots have an air pump that tightens and loosens different areas of the boots. Both of these improve blood flow and help prevent clots.
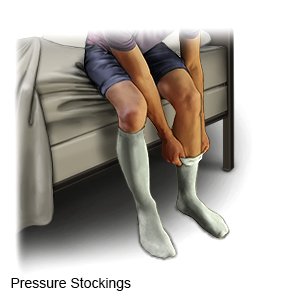
- You may not be able to do your normal activities for a few months. Your sternum (breastbone) will need time to heal. For 6 to 8 weeks after surgery, you will need to follow your healthcare provider's activity instructions.
What can I do to help recover from surgery?
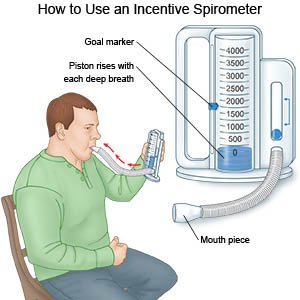
- Deep breathing and coughing will decrease your risk for a lung infection. Take a deep breath and hold it for as long as you can. Let the air out and then cough strongly. Deep breaths help open your airway. You may be given an incentive spirometer to help you take deep breaths. Put the plastic piece in your mouth and take a slow, deep breath. Then let the air out and cough. Repeat these steps 10 times every hour.
- You may need to walk around the same day of surgery , or the day after. Movement will help prevent blood clots. You may also be given exercises to do in bed. Do not get out of bed on your own until your healthcare provider says you can. Talk to healthcare providers before you get up the first time. They may need to help you stand up safely. When you are able to get up on your own, sit or lie down right away if you feel weak or dizzy. Then press the call light button to let healthcare providers know you need help.
- You will be able to drink liquids and eat certain foods when your stomach function returns after surgery. You may be given ice chips at first. Then you will get liquids such as water, broth, juice, and clear soft drinks. If your stomach does not become upset, you may then be given soft foods, such as ice cream and applesauce. When you can eat soft foods easily, you may slowly begin to eat solid foods.
What are the risks of CABG surgery?
- You may develop an infection. You may bleed more than expected and need a blood transfusion. You may have fast, irregular heartbeats. Your heart may not get enough oxygen and have trouble pumping blood through your body after surgery. Your signs and symptoms may come back. You may need another CABG.
- You may have fluid buildup around your heart. This fluid puts pressure on the heart and prevents it from working properly. You may also have fluid buildup around your lungs. This may make it hard for you to breathe after surgery. You may get a blood clot in your leg or arm. These problems can be life-threatening.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
