Zejula: Package Insert / Prescribing Info
Package insert / product label
Generic name: niraparib
Dosage form: capsule
Drug class: PARP inhibitors
Medically reviewed by Drugs.com. Last updated on Jul 2, 2025.
On This Page
- Indications and Usage
- Dosage and Administration
- Dosage Forms and Strengths
- Contraindications
- Warnings and Precautions
- Adverse Reactions/Side Effects
- Use In Specific Populations
- Description
- Clinical Pharmacology
- Nonclinical Toxicology
- Clinical Studies
- How Supplied/Storage and Handling
- Patient Counseling Information
Highlights of Prescribing Information
ZEJULA (niraparib) tablets, for oral use
Initial U.S. Approval: 2017
Recent Major Changes
|
6/2025 |
|
|
6/2025 |
|
|
6/2025 |
Indications and Usage for Zejula
ZEJULA is a poly (ADP-ribose) polymerase (PARP) inhibitor indicated:
- •
- for the maintenance treatment of adult patients with advanced epithelial ovarian, fallopian tube, or primary peritoneal cancer who are in a complete or partial response to first-line platinum-based chemotherapy and whose cancer is associated with homologous recombination deficiency (HRD)-positive status defined by either
- •
- for the maintenance treatment of adult patients with deleterious or suspected deleterious germline BRCA-mutated recurrent epithelial ovarian, fallopian tube, or primary peritoneal cancer who are in a complete or partial response to platinum-based chemotherapy. Select patients for therapy based on an FDA-approved companion diagnostic for ZEJULA. (1.2, 2.1)
Zejula Dosage and Administration
- •
- First-line maintenance treatment of HRD-positive advanced ovarian cancer:
- •
- Maintenance treatment of recurrent germline BRCA-mutated ovarian cancer: The recommended dosage is 300 mg taken orally once daily. (2.2)
- •
- Continue treatment until disease progression or unacceptable toxicity. (2.2)
- •
- ZEJULA may be taken with or without food. (2.2)
- •
- For adverse reactions, consider interruption of treatment, dose reduction, or dose discontinuation. (2.3)
- •
- For patients with moderate hepatic impairment, recommended dosage is 200 mg taken orally once daily. (2.4)
Dosage Forms and Strengths
Tablets: 100 mg, 200 mg, 300 mg. (3)
Contraindications
None. (4)
Warnings and Precautions
- •
- Myelodysplastic Syndrome/Acute Myeloid Leukemia (MDS/AML): MDS/AML occurred in patients exposed to ZEJULA, and some cases were fatal. Monitor patients for hematological toxicity and discontinue if MDS/AML is confirmed. (5.1)
- •
- Bone Marrow Suppression: Test complete blood counts weekly for the first month, monthly for the next 11 months, and periodically thereafter for clinically significant changes. (5.2)
- •
- Hypertension and Cardiovascular Effects: Monitor blood pressure and heart rate at least weekly for the first 2 months, then monthly for the first year and periodically thereafter during treatment with ZEJULA. Manage with antihypertensive medications and adjustment of the dose of ZEJULA, if necessary. (5.3)
- •
- Posterior Reversible Encephalopathy Syndrome (PRES): PRES has occurred in patients treated with ZEJULA. Discontinue ZEJULA if PRES is confirmed. (5.4)
- •
- Embryo-Fetal Toxicity: ZEJULA can cause fetal harm. Advise females of reproductive potential of the potential risk to a fetus and to use effective contraception. (5.5, 8.1, 8.3)
Adverse Reactions/Side Effects
Most common adverse reactions (incidence ≥10%) in patients who received ZEJULA were nausea, thrombocytopenia, anemia, fatigue, constipation, musculoskeletal pain, abdominal pain, vomiting, neutropenia, decreased appetite, leukopenia, insomnia, headache, dyspnea, rash, diarrhea, hypertension, cough, dizziness, acute kidney injury, urinary tract infection, and hypomagnesemia. (6.1)
To report SUSPECTED ADVERSE REACTIONS, contact GlaxoSmithKline at 1-888-825-5249 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
Use In Specific Populations
Lactation: Advise not to breastfeed. (8.2)
See 17 for PATIENT COUNSELING INFORMATION and FDA-approved patient labeling.
Revised: 6/2025
Full Prescribing Information
1. Indications and Usage for Zejula
1.1 First-Line Maintenance Treatment of HRD-Positive Advanced Ovarian Cancer
ZEJULA is indicated for the maintenance treatment of adult patients with advanced epithelial ovarian, fallopian tube, or primary peritoneal cancer who are in a complete or partial response to first-line platinum-based chemotherapy and whose cancer is associated with homologous recombination deficiency (HRD)-positive status defined by either:
- •
- a deleterious or suspected deleterious BRCA mutation, and/or
- •
- genomic instability.
1.2 Maintenance Treatment of Recurrent Germline BRCA-Mutated Ovarian Cancer
ZEJULA is indicated for the maintenance treatment of adult patients with deleterious or suspected deleterious germline BRCA-mutated (gBRCAmut) recurrent epithelial ovarian, fallopian tube, or primary peritoneal cancer who are in a complete or partial response to platinum-based chemotherapy.
Select patients for therapy based on an FDA-approved companion diagnostic for ZEJULA [see Dosage and Administration (2.1)].
2. Zejula Dosage and Administration
2.1 Patient Selection
First-Line Maintenance Treatment of HRD-Positive Advanced Ovarian Cancer
Select patients for first-line maintenance treatment of advanced ovarian cancer with ZEJULA based on the presence of HRD defined by either a deleterious or suspected deleterious BRCA mutation, and/or genomic instability [see Clinical Studies (14.1)].
An FDA-approved test for detection of HRD-positive status for selecting patients for treatment with ZEJULA is not currently available.
Maintenance Treatment of Recurrent Germline BRCA-Mutated Ovarian Cancer
Select patients for the maintenance treatment of recurrent ovarian cancer with ZEJULA based on the presence of deleterious or suspected deleterious germline BRCA mutations [see Clinical Studies (14.2)].
Information on FDA-approved tests for the detection of deleterious or suspected deleterious germline BRCA mutations for this indication is available at https://www.fda.gov/companiondiagnostics.
2.2 Recommended Dosage and Administration
Continue treatment with ZEJULA until disease progression or unacceptable toxicity.
Instruct patients to take their dose of ZEJULA at approximately the same time each day. Advise patients to swallow tablets whole and not to chew, crush, or split ZEJULA prior to swallowing. ZEJULA may be taken with or without food. Bedtime administration may be a potential method for managing nausea.
In the case of a missed dose of ZEJULA, instruct patients to take their next dose at its regularly scheduled time. If a patient vomits or misses a dose of ZEJULA, an additional dose should not be taken.
First-Line Maintenance Treatment of HRD-Positive Advanced Ovarian Cancer
- •
- For patients weighing <77 kg (<170 lbs) OR with a platelet count of <150,000/mcL, the recommended dosage is 200 mg taken orally once daily.
- •
- For patients weighing ≥77 kg (≥170 lbs) AND who have a platelet count ≥150,000/mcL, the recommended dosage is 300 mg taken orally once daily.
For the maintenance treatment of advanced ovarian cancer, start ZEJULA no later than 12 weeks after their most recent platinum-containing regimen.
Maintenance Treatment of Recurrent Germline BRCA-Mutated Ovarian Cancer
The recommended dosage of ZEJULA is 300 mg taken orally once daily.
For the maintenance treatment of recurrent ovarian cancer, start ZEJULA no later than 8 weeks after their most recent platinum-containing regimen.
2.3 Dosage Modifications for Adverse Reactions
To manage adverse reactions, consider interruption of treatment, dose reduction, or dose discontinuation. The recommended dosage modifications for adverse reactions are listed in Tables 1, 2, and 3.
| a If further dose reduction below 100 mg/day is required, discontinue ZEJULA. | ||
|
Starting Dose Level |
200 mg |
300 mg |
|
First dose reduction |
100 mg/daya |
200 mg/day |
|
Second dose reduction |
Discontinue ZEJULA. |
100 mg/daya |
| CTCAE = Common Terminology Criteria for Adverse Events. | |
|
Non-hematologic CTCAE ≥Grade 3 adverse reaction that persists despite medical management |
|
|
CTCAE ≥Grade 3 treatment-related adverse reaction lasting more than 28 days while patient is administered ZEJULA 100 mg/day |
Discontinue ZEJULA. |
| a If myelodysplastic syndrome or acute myeloid leukemia (MDS/AML) is confirmed, discontinue ZEJULA [see Warnings and Precautions (5.1, 5.2)]. | |
|
Monitor complete blood counts weekly for the first month, monthly for the next 11 months of treatment, and periodically after this time [see Warnings and Precautions (5.2)]. |
|
|
Platelet count <100,000/mcL |
First occurrence:
Second occurrence:
|
|
Neutrophil <1,000/mcL or hemoglobin <8 g/dL |
|
|
Hematologic adverse reaction requiring transfusion |
|
2.4 Dosage Modifications for Hepatic Impairment
For patients with moderate hepatic impairment (total bilirubin ≥1.5 to 3 x ULN and any AST level), the recommended dosage of ZEJULA is 200 mg once daily, regardless of body weight or platelet count [see Use in Specific Populations (8.6), Clinical Pharmacology (12.3)]. Monitor patients for hematologic toxicity and reduce the dose, if needed [see Dosage and Administration (2.3)].
3. Dosage Forms and Strengths
- •
- Tablets: 100-mg gray, oval-shaped, film-coated tablet debossed with “100” on one side and “Zejula” on the other side.
- •
- Tablets: 200-mg blue, oval-shaped, film-coated tablet debossed with “200” on one side and “Zejula” on the other side.
- •
- Tablets: 300-mg green, oval-shaped, film-coated tablet debossed with “300” on one side and “Zejula” on the other side.
5. Warnings and Precautions
5.1 Myelodysplastic Syndrome/Acute Myeloid Leukemia
Myelodysplastic syndrome/acute myeloid leukemia (MDS/AML), including cases with a fatal outcome, have been reported in patients who received ZEJULA.
In PRIMA, of patients within the HRD-positive population, MDS/AML occurred in 8 out of 245 (3.3%) patients treated with ZEJULA and in 3 out of 125 (2.4%) patients treated with placebo with a follow-up of 6.1 years [see Adverse Reactions (6.1)]. The duration of therapy with ZEJULA in patients who developed secondary MDS/cancer-therapy–related AML varied from 5.5 months to 5 years.
In NOVA, of patients within the gBRCAmut cohort, MDS/AML occurred in 10 out of 136 (7%) patients treated with ZEJULA and in 2 out of 65 (3%) patients treated with placebo [see Adverse Reactions (6.1)]. The duration of therapy with ZEJULA in patients who developed secondary MDS/cancer-therapy–related AML varied from 3.6 months to 5.9 years.
All patients who developed secondary MDS/cancer-therapy–related AML had received previous chemotherapy with platinum agents and/or other DNA-damaging agents, including radiotherapy.
For suspected MDS/AML or prolonged hematological toxicities, refer the patient to a hematologist for further evaluation. Discontinue ZEJULA if MDS/AML is confirmed.
5.2 Bone Marrow Suppression
Hematologic adverse reactions, including thrombocytopenia, anemia, neutropenia, and/or pancytopenia have been reported in patients treated with ZEJULA [see Adverse Reactions (6)].
In PRIMA, the overall incidences of ≥Grade 3 thrombocytopenia, anemia, and neutropenia were reported in 39%, 31%, and 21%, respectively, of patients receiving ZEJULA. Discontinuation due to thrombocytopenia, anemia, and neutropenia occurred in 4%, 2%, and 2%, respectively, of patients. In patients who were administered a starting dose of ZEJULA based on baseline weight or platelet count, ≥Grade 3 thrombocytopenia, anemia, and neutropenia were reported in 22%, 23%, and 15%, respectively, of patients receiving ZEJULA. Discontinuation due to thrombocytopenia, anemia, and neutropenia occurred in 3%, 3%, and 2%, respectively, of patients.
In NOVA, ≥Grade 3 thrombocytopenia, anemia, and neutropenia were reported in 29%, 25%, and 20%, respectively, of patients receiving ZEJULA. Discontinuation due to thrombocytopenia, anemia, and neutropenia occurred in 3%, 1%, and 2%, respectively, of patients.
Do not start ZEJULA until patients have recovered from hematological toxicity caused by previous chemotherapy (≤Grade 1). Monitor complete blood counts weekly for the first month, monthly for the next 11 months of treatment, and periodically after this time. If hematological toxicities do not resolve within 28 days following interruption, discontinue ZEJULA and refer the patient to a hematologist for further investigations, including bone marrow analysis and blood sample for cytogenetics [see Dosage and Administration (2.3)].
5.3 Hypertension and Cardiovascular Effects
Hypertension and hypertensive crisis have been reported in patients treated with ZEJULA [see Adverse Reactions (6)].
In PRIMA, Grade 3 to 4 hypertension occurred in 6% of patients treated with ZEJULA compared with 1% of placebo-treated patients with a median time from first dose to first onset of 43 days (range: 1 to 531 days) and with a median duration of 12 days (range: 1 to 61 days). There were no discontinuations due to hypertension.
In NOVA, Grade 3 to 4 hypertension occurred in 9% of patients treated with ZEJULA compared with 2% of placebo-treated patients with a median time from first dose to first onset of 77 days (range: 4 to 504 days) and with a median duration of 15 days (range: 1 to 86 days). Discontinuation due to hypertension occurred in <1% of patients.
Monitor blood pressure and heart rate at least weekly for the first 2 months, then monthly for the first year and periodically thereafter during treatment with ZEJULA. Closely monitor patients with cardiovascular disorders, especially coronary insufficiency, cardiac arrhythmias, and hypertension. Medically manage hypertension with antihypertensive medications and adjustment of the dose of ZEJULA, if necessary [see Dosage and Administration (2.3), Nonclinical Toxicology (13.2)].
5.4 Posterior Reversible Encephalopathy Syndrome
Posterior reversible encephalopathy syndrome (PRES) occurred in 0.1% of 2,165 patients treated with ZEJULA in clinical trials and has also been described in postmarketing reports [see Adverse Reactions (6.2)]. Signs and symptoms of PRES include seizure, headache, altered mental status, visual disturbance, or cortical blindness, with or without associated hypertension. A diagnosis of PRES requires confirmation by brain imaging, preferably magnetic resonance imaging.
Monitor all patients treated with ZEJULA for signs and symptoms of PRES. If PRES is suspected, promptly discontinue ZEJULA and administer appropriate treatment. The safety of reinitiating ZEJULA in patients previously experiencing PRES is not known.
5.5 Embryo-Fetal Toxicity
Based on its mechanism of action, ZEJULA can cause fetal harm when administered to a pregnant woman [see Clinical Pharmacology (12.1)]. ZEJULA has the potential to cause teratogenicity and/or embryo-fetal death since niraparib is genotoxic and targets actively dividing cells in animals and patients (e.g., bone marrow) [see Warnings and Precautions (5.2), Nonclinical Toxicology (13.1)]. Due to the potential risk to a fetus based on its mechanism of action, animal developmental and reproductive toxicology studies were not conducted with niraparib.
Apprise pregnant women of the potential risk to a fetus. Advise females of reproductive potential to use effective contraception during treatment and for 6 months after the last dose of ZEJULA [see Use in Specific Populations (8.1, 8.3)].
6. Adverse Reactions/Side Effects
The following clinically significant adverse reactions are described elsewhere in the labeling:
- •
- MDS/AML [see Warnings and Precautions (5.1)]
- •
- Bone marrow suppression [see Warnings and Precautions (5.2)]
- •
- Hypertension and cardiovascular effects [see Warnings and Precautions (5.3)]
- •
- Posterior reversible encephalopathy syndrome [see Warnings and Precautions (5.4)]
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared with rates in the clinical trials of another drug and may not reflect the rates observed in practice.
In a pooled safety population of patients (n = 1,314) with advanced ovarian, fallopian tube, or primary peritoneal cancer treated with ZEJULA monotherapy including PRIMA (n = 484), NOVA (n = 367), and another clinical trial (n = 463), the most common adverse reactions >10% were nausea (65%), thrombocytopenia (60%), anemia (56%), fatigue (55%), constipation (39%), musculoskeletal pain (36%), abdominal pain (35%), vomiting (33%), neutropenia (31%), decreased appetite (24%), leukopenia (24%), insomnia (23%), headache (23%), dyspnea (22%), rash (21%), diarrhea (18%), hypertension (17%), cough (16%), dizziness (14%), acute kidney injury (13%), urinary tract infection (12%), and hypomagnesemia (11%).
First-Line Maintenance Treatment of HRD-Positive Advanced Ovarian Cancer
The safety of ZEJULA for the treatment of patients with advanced ovarian cancer following first-line treatment with platinum-based chemotherapy was studied in the PRIMA trial, a placebo-controlled, double-blind study in which 484 patients received ZEJULA. Among this population, 245 patients were HRD-positive and their median duration of treatment was 13 months (range: 3 days to 29 months).
HRD-Positive Patients Receiving ZEJULA in PRIMA: Serious adverse reactions occurred in 30% of patients receiving ZEJULA. Serious adverse reactions in >2% of patients were thrombocytopenia (11%) and anemia (5%). Fatal adverse reactions occurred in 1.6% of patients, including AML (0.4%), cardiac arrest (0.4%), intestinal perforation (0.4%), and sudden death (0.4%).
Permanent discontinuation due to adverse reactions occurred in 11% of patients who received ZEJULA. Adverse reactions resulting in permanent discontinuation in >1% of patients who received ZEJULA included thrombocytopenia (3.7%), nausea (1.6%), and anemia (1.2%).
Adverse reactions led to dose reduction or interruption in 79% of patients, most frequently (>10%) from thrombocytopenia (53%), anemia (32%), and neutropenia (19%).
Tables 4 and 5 summarize the common adverse reactions and abnormal laboratory findings observed in the PRIMA trial.
| AST/ALT = Aspartate aminotransferase/alanine aminotransferase. | ||||
| a All adverse reactions in the table consist of grouped preferred terms except for nausea, vomiting, decreased appetite, headache, and insomnia, which are single preferred terms. | ||||
| b Common Terminology Criteria for Adverse Events version 4.02. | ||||
| c Includes neutropenia, neutropenic infection, neutropenic sepsis, and febrile neutropenia. | ||||
| d Includes leukopenia, lymphocyte count decreased, lymphopenia, and white blood cell count decreased. | ||||
| e Includes blood creatinine increased, blood urea increased, acute kidney injury, and renal failure. | ||||
|
Adverse Reaction |
Grades 1-4b |
Grades 3-4b |
||
|
ZEJULA (n = 245) % |
Placebo (n = 125) % |
ZEJULA (n = 245) % |
Placebo (n = 125) % |
|
|
Blood and lymphatic system disorders | ||||
|
Thrombocytopenia |
66 |
4 |
38 |
0 |
|
Anemia |
65 |
16 |
31 |
2 |
|
Neutropeniac |
43 |
9 |
17 |
2 |
|
Leukopeniad |
29 |
10 |
6 |
0.8 |
|
Gastrointestinal disorders | ||||
|
Nausea |
62 |
34 |
1 |
0 |
|
Constipation |
40 |
26 |
1 |
0.8 |
|
Vomiting |
23 |
14 |
2 |
0.8 |
|
General disorders and administration site conditions | ||||
|
Fatigue |
52 |
44 |
2 |
2 |
|
Musculoskeletal and connective tissue disorders | ||||
|
Musculoskeletal pain |
46 |
38 |
0.8 |
0 |
|
Nervous system disorders | ||||
|
Headache |
27 |
15 |
0.8 |
0 |
|
Dizziness |
20 |
11 |
0 |
0 |
|
Psychiatric disorders | ||||
|
Insomnia |
25 |
16 |
0.4 |
0.8 |
|
Anxiety |
12 |
6 |
0 |
0 |
|
Respiratory, thoracic, and mediastinal disorders | ||||
|
Dyspnea |
21 |
15 |
0 |
0.8 |
|
Cough |
20 |
14 |
0 |
0.8 |
|
Metabolism and nutrition disorders | ||||
|
Decreased appetite |
20 |
6 |
0.4 |
0 |
|
Vascular disorders | ||||
|
Hypertension |
20 |
8 |
7 |
2 |
|
Investigations | ||||
|
AST/ALT elevation |
14 |
8 |
3 |
0 |
|
Renal and urinary disorders | ||||
|
Acute kidney injurye |
13 |
3 |
0 |
0 |
|
Abnormal Laboratory Finding |
Grades 1-4 |
Grades 3-4 |
||
|
ZEJULA (n = 245) % |
Placebo (n = 125) % |
ZEJULA (n = 245) % |
Placebo (n = 125) % |
|
|
Decreased hemoglobin |
85 |
65 |
28 |
2 |
|
Decreased leukocytes |
72 |
37 |
9 |
0 |
|
Decreased platelets |
71 |
11 |
36 |
0 |
|
Decreased neutrophils |
64 |
28 |
21 |
2 |
|
Increased glucose |
62 |
57 |
3 |
4 |
|
Decreased lymphocytes |
55 |
26 |
9 |
5 |
|
Increased alkaline phosphatase |
48 |
19 |
2 |
0.8 |
|
Increased creatinine |
40 |
24 |
0 |
0 |
|
Decreased magnesium |
39 |
35 |
0.4 |
0 |
|
Increased aspartate aminotransferase |
35 |
18 |
2 |
0.8 |
|
Increased alanine aminotransferase |
32 |
19 |
2 |
2 |
|
Increased calcium |
31 |
23 |
1 |
0 |
HRD-Positive Patients Receiving ZEJULA with Dose Based on Baseline Weight or Platelet Count in PRIMA: Among patients who received ZEJULA with the dose based on weight and platelet count (n = 86), the median duration of treatment was 12 months (range: 4 days to 16 months).
Serious adverse reactions occurred in 24% of patients receiving ZEJULA. Serious adverse reactions in >2% of patients were anemia (9%) and thrombocytopenia (2%).
Permanent discontinuation due to adverse reactions occurred in 11% of patients who received ZEJULA. Adverse reactions resulting in permanent discontinuation in >2% of patients who received ZEJULA included nausea (3.5%).
Adverse reactions led to dose reduction or interruption in 72% of patients, most frequently (>10%) from thrombocytopenia (35%), anemia (22%), and neutropenia (17%).
Tables 6 and 7 summarize adverse reactions and abnormal laboratory findings observed in this group.
| a All adverse reactions in the table consist of grouped preferred terms except for nausea, vomiting, decreased appetite, headache, and insomnia, which are single preferred terms. | ||||
| b Common Terminology Criteria for Adverse Events version 4.02. | ||||
| c Includes neutropenia, neutropenic infection, neutropenic sepsis, and febrile neutropenia. | ||||
| d Includes leukopenia, lymphocyte count decreased, lymphopenia, and white blood cell count decreased. | ||||
| e Includes blood creatinine increased, blood urea increased, acute kidney injury, and renal failure. | ||||
|
Adverse Reaction |
Grades 1-4b |
Grades 3-4b |
||
|
ZEJULA (n = 86) % |
Placebo (n = 42) % |
ZEJULA (n = 86) % |
Placebo (n = 42) % |
|
|
Blood and lymphatic system disorders | ||||
|
Thrombocytopenia |
51 |
2 |
16 |
0 |
|
Anemia |
49 |
21 |
22 |
0 |
|
Neutropeniac |
35 |
7 |
13 |
0 |
|
Leukopeniad |
26 |
7 |
6 |
0 |
|
Gastrointestinal disorders | ||||
|
Nausea |
55 |
21 |
0 |
0 |
|
Constipation |
26 |
29 |
1 |
2 |
|
Vomiting |
16 |
17 |
0 |
2.4 |
|
General disorders and administration site conditions | ||||
|
Fatigue |
47 |
41 |
0 |
0 |
|
Nervous system disorders | ||||
|
Headache |
24 |
19 |
1 |
0 |
|
Dizziness |
15 |
7 |
0 |
0 |
|
Psychiatric disorders | ||||
|
Insomnia |
21 |
19 |
0 |
0 |
|
Metabolism and nutrition disorders | ||||
|
Decreased appetite |
19 |
7 |
1 |
0 |
|
Respiratory, thoracic, and mediastinal disorders | ||||
|
Dyspnea |
20 |
12 |
0 |
2 |
|
Vascular disorders | ||||
|
Hypertension |
16 |
12 |
4 |
5 |
|
Renal and urinary disorders | ||||
|
Acute kidney injurye |
14 |
2 |
0 |
0 |
|
Abnormal Laboratory Finding |
Grades 1-4 |
Grades 3-4 |
||
|
ZEJULA (n = 86) % |
Placebo (n = 42) % |
ZEJULA (n = 86) % |
Placebo (n = 42) % |
|
|
Decreased hemoglobin |
74 |
67 |
21 |
0 |
|
Decreased leukocytes |
70 |
36 |
6 |
0 |
|
Decreased platelets |
58 |
17 |
14 |
0 |
|
Increased glucose |
57 |
62 |
4 |
2 |
|
Decreased neutrophils |
57 |
31 |
13 |
0 |
|
Decreased lymphocytes |
55 |
24 |
6 |
5 |
|
Decreased magnesium |
51 |
41 |
0 |
0 |
|
Increased alkaline phosphatase |
42 |
12 |
2 |
0 |
|
Increased creatinine |
42 |
24 |
0 |
0 |
|
Increased aspartate aminotransferase |
31 |
21 |
2 |
0 |
|
Increased alanine aminotransferase |
30 |
17 |
2 |
2 |
|
Increased calcium |
29 |
36 |
0 |
0 |
Maintenance Treatment of Recurrent Germline BRCA-mutated Ovarian Cancer
The safety of monotherapy with ZEJULA 300 mg once daily has been studied in 136 patients with platinum-sensitive recurrent gBRCAmut ovarian, fallopian tube, and primary peritoneal cancer in the NOVA trial. The percentages of patients who experienced adverse reactions in NOVA that led to dose reduction and dose interruption were 79% and 68%, respectively, most frequently from thrombocytopenia (41% and 35%, respectively) and anemia (23% and 20%, respectively). The permanent discontinuation rate due to adverse reactions in NOVA was 13%. The median exposure to ZEJULA in these patients was 367 days.
Table 8 and Table 9 summarize the common adverse reactions and abnormal laboratory findings, respectively, observed in patients treated with ZEJULA in the gBRCAmut cohort in NOVA.
| gBRCAmut = Germline BRCA-mutated. | ||||
| a Common Terminology Criteria for Adverse Events version 4.02. | ||||
| b Includes platelet count decreased. | ||||
| c Includes hemoglobin decreased. | ||||
| d Includes neutrophil count decreased. | ||||
| e Includes asthenia, malaise, and lethargy. | ||||
|
Adverse Reaction |
Grades 1-4a |
Grades 3-4a |
||
|
ZEJULA (n = 136) % |
Placebo (n = 65) % |
ZEJULA (n = 136) % |
Placebo (n = 65) % |
|
|
Gastrointestinal disorders | ||||
|
Nausea |
77 |
34 |
5 |
3 |
|
Vomiting |
40 |
15 |
4 |
0 |
|
Constipation |
38 |
18 |
0.7 |
2 |
|
Dyspepsia |
17 |
12 |
0 |
0 |
|
Dry mouth |
13 |
3 |
0.7 |
0 |
|
Blood and lymphatic system disorders | ||||
|
Thrombocytopeniab |
71 |
5 |
38 |
2 |
|
Anemiac |
52 |
8 |
33 |
0 |
|
Neutropeniad |
31 |
9 |
21 |
3 |
|
General disorders and administration site conditions | ||||
|
Fatiguee |
61 |
35 |
8 |
2 |
|
Nervous system disorders | ||||
|
Headache |
35 |
8 |
0.7 |
0 |
|
Dizziness |
18 |
9 |
0 |
0 |
|
Dysgeusia |
13 |
2 |
0 |
0 |
|
Metabolism and nutrition disorders | ||||
|
Decreased appetite |
22 |
14 |
0 |
0 |
|
Vascular disorders | ||||
|
Hypertension |
21 |
8 |
8 |
5 |
|
Psychiatric disorders | ||||
|
Insomnia |
18 |
6 |
0.7 |
0 |
|
Anxiety |
10 |
11 |
0.7 |
0 |
|
Respiratory, thoracic, and mediastinal disorders | ||||
|
Dyspnea |
17 |
5 |
2 |
0 |
|
Cough |
16 |
2 |
0 |
0 |
|
Nasopharyngitis |
13 |
5 |
0 |
0 |
|
Musculoskeletal and connective tissue disorders | ||||
|
Back pain |
16 |
11 |
0.7 |
0 |
|
Infections and infestations | ||||
|
Urinary tract infection |
11 |
9 |
0 |
2 |
|
Skin and subcutaneous tissue disorders | ||||
|
Rash |
10 |
2 |
0 |
0 |
The following adverse reactions have been identified in ≥1 to <10% of the 136 patients receiving ZEJULA in the gBRCAmut cohort of the NOVA trial and not included in the table: palpitations (9%), mucositis/stomatitis (9%), MDS/AML (7%), tachycardia (7%), and bronchitis (4%).
| gBRCAmut = Germline BRCA-mutated. | ||||
|
Abnormal Laboratory Finding |
Grades 1-4 |
Grades 3-4 |
||
|
ZEJULA (n = 136) % |
Placebo (n = 65) % |
ZEJULA (n = 136) % |
Placebo (n = 65) % |
|
|
Decrease in hemoglobin |
85 |
62 |
32 |
0 |
|
Decrease in platelet count |
81 |
25 |
38 |
2 |
|
Decrease in white blood cell count |
71 |
37 |
9 |
2 |
|
Decrease in absolute neutrophil count |
56 |
34 |
23 |
3 |
|
Increase in aspartate aminotransferase |
35 |
25 |
0.7 |
0 |
|
Increase in alanine aminotransferase |
25 |
15 |
0.7 |
2 |
6.2 Postmarketing Experience
The following adverse reactions have been identified during postapproval use of ZEJULA. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Blood and Lymphatic System Disorders
Pancytopenia.
Immune System Disorders
Hypersensitivity (including anaphylaxis).
Nervous System Disorders
Posterior reversible encephalopathy syndrome (PRES).
Psychiatric Disorders
Confusional state/disorientation, hallucination, cognitive impairment (e.g., memory impairment, concentration impairment).
Respiratory, Thoracic, and Mediastinal Disorders
Non-infectious pneumonitis.
Skin and Subcutaneous Tissue Disorders
Photosensitivity.
Vascular Disorders
Hypertensive crisis.
Related/similar drugs
8. Use In Specific Populations
8.1 Pregnancy
Risk Summary
Based on its mechanism of action, ZEJULA can cause fetal harm when administered to pregnant women [see Clinical Pharmacology (12.1)]. There are no data regarding the use of ZEJULA in pregnant women to inform the drug-associated risk. ZEJULA has the potential to cause teratogenicity and/or embryo-fetal death since niraparib is genotoxic and targets actively dividing cells in animals and patients (e.g., bone marrow) [see Warnings and Precautions (5.2), Nonclinical Toxicology (13.1)]. Due to the potential risk to a fetus based on its mechanism of action, animal developmental and reproductive toxicology studies were not conducted with niraparib. Apprise pregnant women of the potential risk to a fetus.
The background risk of major birth defects and miscarriage for the indicated population is unknown. In the U.S. general population, the estimated background risk of major birth defects and miscarriage in clinically recognized pregnancies is 2% to 4% and 15% to 20%, respectively.
8.2 Lactation
Risk Summary
No data are available regarding the presence of niraparib or its metabolites in human milk, or on its effects on the breastfed child or milk production. Because of the potential for serious adverse reactions in a breastfed child, advise a lactating woman not to breastfeed during treatment with ZEJULA and for 1 month after receiving the last dose.
8.3 Females and Males of Reproductive Potential
ZEJULA can cause fetal harm when administered to a pregnant woman [see Use in Specific Populations (8.1)].
Pregnancy Testing
Verify the pregnancy status of females of reproductive potential prior to initiating treatment with ZEJULA.
Contraception
Females: Advise females of reproductive potential to use effective contraception during treatment with ZEJULA and for 6 months following the last dose.
Infertility
Males: Based on animal studies, ZEJULA may impair fertility in males of reproductive potential [see Nonclinical Toxicology (13.1)].
8.4 Pediatric Use
The safety and effectiveness of ZEJULA have not been established in pediatric patients.
8.5 Geriatric Use
In PRIMA, 39% of patients were aged 65 years or older and 10% were aged 75 years or older. In NOVA, 35% of patients were aged 65 years or older and 8% were aged 75 years or older. No overall differences in safety and effectiveness of ZEJULA were observed between these patients and younger patients but greater sensitivity of some older individuals cannot be ruled out.
8.6 Hepatic Impairment
For patients with moderate hepatic impairment, the recommended dosage of ZEJULA is 200 mg once daily, regardless of body weight or platelet count. Monitor patients for hematologic toxicity and reduce the dose, if needed [see Dosage and Administration (2.3, 2.4)]. Niraparib exposure increased in patients with moderate hepatic impairment (total bilirubin ≥1.5 to 3 x ULN and any AST level).
For patients with mild hepatic impairment (total bilirubin <1.5 x ULN and any AST level or bilirubin ≤ULN and AST >ULN), no dosage modification is recommended.
The effect of severe hepatic impairment (total bilirubin >3 x ULN and any AST level) on niraparib pharmacokinetics is unknown.
11. Zejula Description
Niraparib is an orally available poly (ADP-ribose) polymerase (PARP) inhibitor.
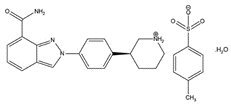
The chemical name for niraparib tosylate monohydrate is 2-{4-[(3S)-piperidin-3-yl]phenyl}-2H-indazole 7-carboxamide 4-methylbenzenesulfonate hydrate (1:1:1). The molecular formula is C26H30N4O5S and it has a molecular weight of 510.61 amu. The molecular structure is shown below:
Niraparib tosylate monohydrate is a white to off-white, non-hygroscopic crystalline solid. Niraparib solubility is pH independent below the pKa of 9.95, with an aqueous free base solubility of 0.7 mg/mL to 1.1 mg/mL across the physiological pH range.
Each ZEJULA tablet contains 159.3 mg, 318.7 mg, or 478.0 mg of niraparib tosylate monohydrate equivalent to 100 mg, 200 mg, or 300 mg, respectively, of niraparib free base as the active ingredient. The inactive ingredients in the core tablet are crospovidone, lactose monohydrate, magnesium stearate, microcrystalline cellulose, povidone, and silicon dioxide. The film-coating consists of Opadry II Gray (100 mg), Opadry II Blue (200 mg), or Opadry II Green (300 mg).
12. Zejula - Clinical Pharmacology
12.1 Mechanism of Action
Niraparib is an inhibitor of PARP enzymes, including PARP-1 and PARP-2, that play a role in DNA repair. In vitro studies have shown that niraparib-induced cytotoxicity may involve inhibition of PARP enzymatic activity and increased formation of PARP-DNA complexes resulting in DNA damage, apoptosis, and cell death. Increased niraparib‑induced cytotoxicity was observed in tumor cell lines with or without deficiencies in BRCA1/2. Niraparib decreased tumor growth in mouse xenograft models of human cancer cell lines with deficiencies in BRCA1/2 and in human patient-derived xenograft tumor models with homologous recombination deficiency (HRD) that had either mutated or wild-type BRCA1/2.
12.2 Pharmacodynamics
The pharmacodynamic response of niraparib has not been characterized.
Hypertension and Cardiovascular Effects
Niraparib has the potential to cause effects on pulse rate and blood pressure in patients receiving the recommended dose, which may be related to pharmacological inhibition of the dopamine transporter, norepinephrine transporter, and serotonin transporter [see Nonclinical Toxicology (13.2)].
In PRIMA, mean pulse rate and blood pressure increased over baseline in the niraparib arm relative to the placebo arm at most on-study assessments. Mean greatest increases from baseline in pulse rate on treatment were 22.4 and 14.0 beats/min in the niraparib and placebo arms, respectively. Mean greatest increases from baseline in systolic blood pressure on treatment were 24.4 and 19.6 mmHg in the niraparib and placebo arms, respectively. Mean greatest increases from baseline in diastolic blood pressure on treatment were 15.9 and 13.9 mmHg in the niraparib and placebo arms, respectively.
In NOVA, mean pulse rate and blood pressure increased over baseline in the niraparib arm relative to the placebo arm at all on-study assessments. Mean greatest increases from baseline in pulse rate on treatment were 24.1 and 15.8 beats/min in the niraparib and placebo arms, respectively. Mean greatest increases from baseline in systolic blood pressure on treatment were 24.5 and 18.3 mmHg in the niraparib and placebo arms, respectively. Mean greatest increases from baseline in diastolic blood pressure on treatment were 16.5 and 11.6 mmHg in the niraparib and placebo arms, respectively.
Cardiac Electrophysiology
At the approved maximum recommended dose, a mean increase in the QTc interval >20 ms was not observed.
12.3 Pharmacokinetics
Niraparib mean (±SD) maximum plasma concentration (Cmax) is 603 (±343) ng/mL at the approved maximum recommended dose of 300 mg. Niraparib steady-state Cmax and AUC increased in a dose-proportional manner with daily doses ranging from 30 mg (0.15 times the approved minimum recommended dose) to 400 mg (1.3 times the approved maximum recommended dose). The accumulation of niraparib exposure is approximately 2-fold at the approved recommended doses.
Absorption
The absolute bioavailability of niraparib is approximately 73%. Time to maximum plasma concentration (Tmax) is reached within 5 hours.
Food Effect: Niraparib Cmax increased by 11% and AUC by 28%, following administration with a high-fat meal (800 to 1,000 calories, 50% fat).
Distribution
Niraparib is 83% bound to human plasma proteins. Niraparib mean (±SD) apparent (oral) volume of distribution (Vd/F) is 1,220 (±1,114) L.
Elimination
Niraparib apparent (oral) total clearance (CL/F) is 15.9 (±3.8) L/h and mean half-life (t1/2) is 50 (±15) hours.
Metabolism: Niraparib is metabolized by carboxylesterases to form a major inactive metabolite M1, which subsequently undergoes glucuronidation.
Excretion: Following administration of a single oral dose of radio-labeled niraparib 300 mg, 48% of the dose was recovered in urine (11% unchanged) and 39% in feces (19% unchanged).
Specific Populations
No clinically significant differences in the pharmacokinetics of niraparib were observed based on age (18 to 65 years), race/ethnicity, and mild to moderate renal impairment (CLcr 30 to 90 mL/min).
The effect of severe renal impairment (CLcr <30 mL/min) or end-stage renal disease undergoing hemodialysis on the pharmacokinetics of niraparib is unknown.
Hepatic Impairment: Mild hepatic impairment (total bilirubin <1.5 x ULN and any AST level or bilirubin ≤ULN and AST >ULN) had no clinically significant effect on the pharmacokinetics of niraparib.
Niraparib AUC increased 1.6-fold in patients with moderate hepatic impairment (total bilirubin ≥1.5 to 3 x ULN and any AST level) with no effect on niraparib Cmax or protein binding.
The effect of severe hepatic impairment (total bilirubin >3 x ULN and any AST level) on the pharmacokinetics of niraparib is unknown.
Drug Interaction Studies
In Vitro Studies:
Cytochrome P450 (CYP) Enzymes: Niraparib and M1 did not inhibit CYP1A, CYP2B6, CYP2C8, CYP2C9, CYP2C19, CYP2D6, and CYP3A.
Niraparib and M1 do not induce CYP3A.
- Uridine 5'-Diphospho-Glucuronosyltransferases (UGTs): Niraparib did not inhibit UGT1A1, UGT1A4, UGT1A9, and UGT2B7.
Transporters: Niraparib inhibits BCRP, MATE1, and MATE2K, but does not inhibit P-glycoprotein (P-gp), BSEP, or MRP2.
M1 did not inhibit P-gp, BCRP, BSEP, MRP2, MATE1 or MATE2K. Niraparib and M1 did not inhibit OATP1B1, OATP1B3, OCT1, OAT1, OAT3, or OCT2.
Niraparib is a substrate of P-gp and BCRP, but not of BSEP, MRP2, MATE1, MATE2K, OATP1B1, OATP1B3, OCT1, OAT1, OAT3, or OCT2.
M1 is a substrate of MATE1 and MATE2K, but not of P-gp, BCRP, BSEP, MRP2, OATP1B1, OATP1B3, OCT1, OAT1, OAT3, or OCT2.
13. Nonclinical Toxicology
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Carcinogenicity studies have not been conducted with niraparib.
Niraparib was clastogenic in an in vitro mammalian chromosomal aberration assay and in an in vivo rat bone marrow micronucleus assay. This clastogenicity is consistent with genomic instability resulting from the primary pharmacology of niraparib and indicates potential for genotoxicity in humans. Niraparib was not mutagenic in a bacterial reverse mutation assay (Ames) test.
Fertility studies in animals have not been conducted with niraparib. In repeat-dose oral toxicity studies, niraparib was administered daily for up to 3 months’ duration in rats and dogs. Reduced sperm, spermatids, and germ cells in epididymides and testes were observed at doses ≥10 mg/kg and ≥1.5 mg/kg in rats and dogs, respectively. These dose levels resulted in systemic exposures approximately 0.3 and 0.012 times, respectively, the human exposure (AUC0-24h) at the recommended dose of 300 mg daily. There was a trend toward reversibility of these findings 4 weeks after dosing was stopped.
13.2 Animal Toxicology and/or Pharmacology
In vitro, niraparib bound to DAT, NET, and SERT and inhibited uptake of norepinephrine and dopamine in cells with IC50 values that were lower than the Cmin at steady-state in patients receiving the recommended dose. Niraparib has the potential to cause effects in patients related to inhibition of these transporters (e.g., cardiovascular, central nervous system).
Intravenous administration of niraparib to vagotomized dogs over 30 minutes at 1, 3, and 10 mg/kg resulted in an increased range of arterial pressures of 13% to 20%, 18% to 27%, and 19% to 25%, respectively, and increased range of heart rates of 2% to 11%, 4% to 17%, and 12% to 21%, respectively, above pre-dose levels. The unbound plasma concentrations of niraparib in dogs at these dose levels were approximately 0.5, 1.5, and 5.8 times the unbound Cmax at steady‑state in patients receiving the recommended dose.
In addition, niraparib crossed the blood-brain barrier in rats and monkeys following oral administration. The cerebrospinal fluid:plasma Cmax ratios of niraparib administered at 10 mg/kg orally to 2 rhesus monkeys were 0.10 and 0.52.
14. Clinical Studies
14.1 First-Line Maintenance Treatment of HRD-Positive Advanced Ovarian Cancer
PRIMA (NCT02655016) was a double-blind, placebo-controlled trial in which patients (N = 733) in complete or partial response to first-line platinum-based chemotherapy were randomized 2:1 to ZEJULA or matched placebo. Initially, the patients received a starting dosage of 300 mg once daily regardless of body weight or platelet count. The study was amended to include a starting dose of 200 mg for patients weighing <77 kg (<170 lbs) OR with a platelet count of <150,000/mcL or 300 mg for patients weighing ≥77 kg (≥170 lbs) AND who had a platelet count ≥150,000/mcL.
Patients were randomized post-completion of first-line platinum-based chemotherapy plus surgery. Randomization was stratified by best response during the front-line platinum regimen (complete response vs. partial response), neoadjuvant chemotherapy (NACT) (yes vs. no), and HRD status (positive vs. negative or not determined). HRD status was determined using an investigational HRD assay. HRD-positive status included either tumor BRCA mutant (tBRCAm) or a genomic instability score (GIS) ≥42.
The major efficacy outcome measure, progression-free survival (PFS), was determined by blinded independent central review (BICR) per Response Evaluation Criteria in Solid Tumors (RECIST) version 1.1. In some cases, criteria other than RECIST, such as clinical signs and symptoms and increasing CA-125, were also applied. Overall survival (OS) was an additional efficacy outcome measure.
Efficacy was evaluated in 373 patients in the HRD-positive population. The median age was 58 years (range 32 to 83 years). Eighty-seven percent of patients were White, 4.8% were Asian, 1.6% were Black or African American, 0.3% were Native Hawaiian or Other Pacific Islander, and 0.3% were American Indian or Alaska Native. Six percent of patients were Hispanic or Latino. Seventy-five percent of patients had an Eastern Cooperative Oncology Group Performance Status (ECOG PS) of 0 at trial baseline. Approximately 47% of patients were enrolled in the U.S. or Canada. Sixty-four percent of patients had Stage III disease and 36% had Stage IV disease. Sixty-three percent of the patients received NACT. Seventy-five percent of the patients had a complete response to the first-line platinum-based chemotherapy. Approximately 35% (n = 130) of patients received a starting dose of 200 or 300 mg depending on baseline body weight and platelet count.
PRIMA demonstrated a statistically significant improvement in PFS for patients randomized to ZEJULA as compared with placebo in the HRD-positive population (Table 10 and Figure 1).
| HRD = Homologous Recombination Deficient; NE = Not Estimable. | ||
| a Efficacy analysis was based on blinded independent central review. | ||
| b Based on a stratified Cox proportional hazards model. | ||
| c Based on a stratified log-rank test. | ||
|
ZEJULA (n = 247) |
Placebo (n = 126) |
|
|
PFS events, n (%) |
81 (33) |
73 (58) |
|
PFS median in months (95% CI) |
21.9 (19.3, NE) |
10.4 (8.1, 12.1) |
|
Hazard ratiob (95% CI) |
0.43 (0.31, 0.59) |
|
|
P valuec |
<0.0001 |
|
In an exploratory subgroup analysis of patients in the HRD-positive population who were administered a starting dose of ZEJULA or matched placebo based on baseline weight or platelet count (n = 130), the hazard ratio (HR) for PFS was 0.39 (95% CI: 0.22, 0.72).
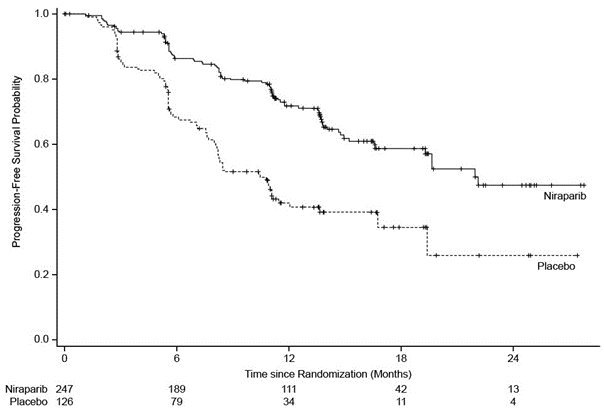
Figure 1. PRIMA Progression-Free Survival – HRD-Positive Population
HRD = Homologous Recombination Deficient.
A final OS analysis was conducted in the HRD-positive population after 185 events were observed; the HR was 0.95 (95% CI: 0.71, 1.29) with a median OS of 71.9 months (95% CI: 55.5, NE) for patients treated with ZEJULA and 69.8 months (95% CI: 51.6, NE) for patients on placebo.
14.2 Maintenance Treatment of Recurrent Germline BRCA-Mutated Ovarian Cancer
NOVA (NCT01847274) was a double-blind, placebo-controlled trial in which patients (N = 553) with platinum-sensitive recurrent epithelial ovarian, fallopian tube, or primary peritoneal cancer were randomized 2:1 to ZEJULA 300 mg orally daily or matched placebo within 8 weeks of the last therapy. Treatment was continued until disease progression or unacceptable toxicity. All patients had received at least 2 prior platinum-containing regimens and were in response (complete or partial) to their most recent platinum-based regimen.
Randomization was stratified by time to progression after the penultimate platinum therapy (6 to <12 months and ≥12 months), use of bevacizumab in conjunction with the penultimate or last platinum regimen (yes/no), and best response during the most recent platinum regimen (complete response and partial response). Eligible patients were assigned to 1 of 2 cohorts based on the results of germline BRCA testing with Myriad BRACAnalysis CDx. Patients with deleterious or suspected deleterious germline BRCA mutations (gBRCAmut) were assigned to the germline BRCA-mutated (gBRCAmut) cohort (n = 203), and those without germline BRCA mutations were assigned to the non-gBRCAmut cohort (n = 350). The efficacy results are based on the gBRCAmut cohort only.
The major efficacy outcome measure, PFS, was determined primarily by central independent assessment per RECIST version 1.1. In some cases, criteria other than RECIST, such as clinical signs and symptoms and increasing CA-125, were also applied. Overall survival (OS) was an additional outcome measure.
For the gBRCAmut cohort, the median age of patients was 57 years among patients treated with ZEJULA and 58 years among patients treated with placebo. Eighty-eight percent of all patients were White. Sixty-six percent of patients receiving ZEJULA and 74% of patients receiving placebo had an ECOG PS of 0 at study baseline. Approximately 40% of patients were enrolled in the U.S. or Canada, and 51% of all patients were in complete response to most recent platinum‑based regimen, with 39% on both arms with an interval of 6 to 12 months since the penultimate platinum regimen. Twenty-four percent of those treated with ZEJULA and 26% treated with placebo had received prior bevacizumab therapy. Approximately 50% of patients had 3 or more lines of treatment.
The trial demonstrated a statistically significant improvement in PFS for patients randomized to ZEJULA as compared with placebo in the gBRCAmut cohort (Table 11 and Figure 2).
| gBRCAmut = germline BRCA-mutated; IRC = Independent Review Committee; NR = Not Reached. | ||
| a Efficacy analysis was based on blinded central independent radiologic and clinical oncology review committee. | ||
| b Based on a stratified Cox proportional hazards model. | ||
| c Based on a stratified log-rank test. | ||
|
ZEJULA (n = 138) |
Placebo (n = 65) |
|
|
Progression-free survival median in months (95% CI) |
21.0 (12.9, NR) |
5.5 (3.8, 7.2) |
|
Hazard ratiob (95% CI) |
0.26 (0.17, 0.41) |
|
|
P valuec |
<0.0001 |
|
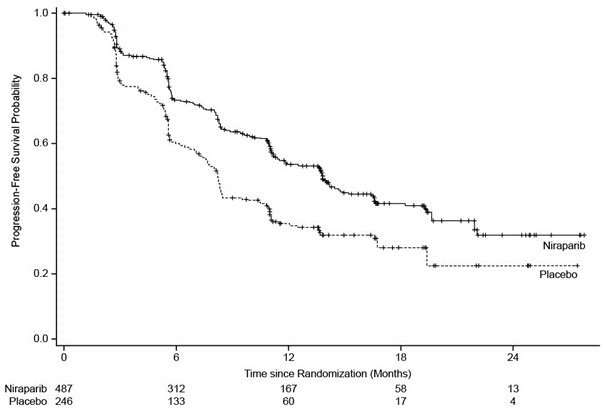
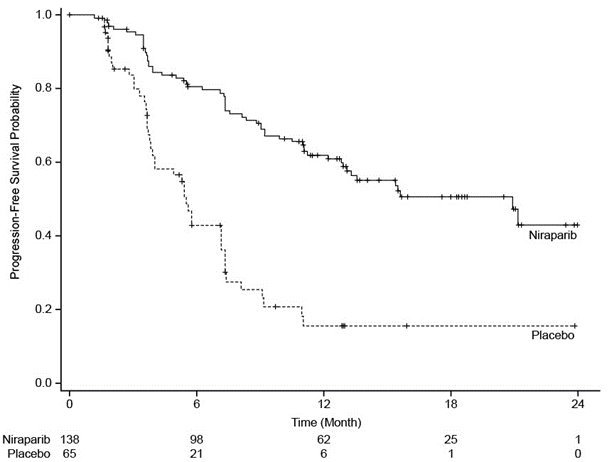
Figure 2. Progression-Free Survival – NOVA gBRCAmut Cohort Based on IRC Assessment (N = 203)
gBRCAmut = germline BRCA-mutated; IRC = Independent Review Committee.
A final OS analysis was conducted after 154 events were observed. Exploratory OS results showed a HR of 0.85 (95% CI: 0.61, 1.20) in the gBRCAmut cohort with a median OS of 40.9 months (95% CI: 34.9, 52.9) for patients treated with ZEJULA and 38.1 months (95% CI: 27.6, 47.3) for patients on placebo.
16. How is Zejula supplied
ZEJULA is available as oval-shaped, film-coated tablets containing 100 mg, 200 mg, or 300 mg of niraparib free base.
ZEJULA 100-mg tablets are gray, debossed with “100” on one side and “Zejula” on the other side. Bottle of 30 tablets (NDC 0173-0909-13).
ZEJULA 200-mg tablets are blue, debossed with “200” on one side and “Zejula” on the other side. Bottle of 30 tablets (NDC 0173-0912-13).
ZEJULA 300-mg tablets are green, debossed with “300” on one side and “Zejula” on the other side. Bottle of 30 tablets (NDC 0173-0915-13).
Store and dispense in the original bottle. Store at 20°C to 25°C (68°F to 77°F); excursions are permitted between 15°C to 30°C (59°F to 86°F) [see USP Controlled Room Temperature].
17. Patient Counseling Information
Advise the patient to read the FDA-approved patient labeling (Patient Information).
Myelodysplastic Syndrome/Acute Myeloid Leukemia
Advise patients to contact their healthcare provider if they experience weakness, feeling tired, fever, weight loss, frequent infections, bruising, bleeding easily, breathlessness, blood in urine or stool, and/or laboratory findings of low blood cell counts or a need for blood transfusions. This may be a sign of hematological toxicity or MDS or AML, which has been reported in patients treated with ZEJULA [see Warnings and Precautions (5.1)].
Bone Marrow Suppression
Advise patients that periodic monitoring of their blood counts is required. Advise patients to contact their healthcare provider for new onset of bleeding, fever, or symptoms of infection [see Warnings and Precautions (5.2)].
Hypertension and Cardiovascular Effects
Advise patients to undergo blood pressure and heart rate monitoring at least weekly for the first 2 months, then monthly for the first year of treatment and periodically thereafter. Advise patients to contact their healthcare provider if blood pressure is elevated [see Warnings and Precautions (5.3)].
Posterior Reversible Encephalopathy Syndrome
Inform patients that they are at risk of developing posterior reversible encephalopathy syndrome (PRES) that can present with signs and symptoms including seizure, headaches, altered mental status, or vision changes. Advise patients to contact their healthcare provider if they develop any of these signs or symptoms [see Warnings and Precautions (5.4)].
Dosing Instructions
Inform patients on how to take ZEJULA [see Dosage and Administration (2.2)]. ZEJULA should be taken once daily. Instruct patients that if they miss a dose of ZEJULA not to take an extra dose to make up for the one that they missed. They should take their next dose at the regularly scheduled time. Each tablet should be swallowed whole. ZEJULA may be taken with or without food. Bedtime administration may be a potential method for managing nausea.
Embryo-Fetal Toxicity
Advise females to inform their healthcare provider if they are pregnant or become pregnant. Inform female patients of the risk to a fetus and potential loss of the pregnancy [see Warnings and Precautions (5.5), Use in Specific Populations (8.1)].
Contraception
Advise females of reproductive potential to use effective contraception during treatment with ZEJULA and for 6 months after receiving the last dose [see Use in Specific Populations (8.3)].
Lactation
Advise patients not to breastfeed while taking ZEJULA and for 1 month after the last dose [see Use in Specific Populations (8.2)].
Trademarks are owned by or licensed to the GSK group of companies. Opadry is a trademark owned by or licensed to its respective owner and is not owned by or licensed to the GSK group of companies. The maker of Opadry is not affiliated with and does not endorse the GSK group of companies or its products.
Manufactured for
GlaxoSmithKline
Durham, NC 27701
©2025 GSK group of companies or its licensor.
ZJT:4PI
|
PATIENT INFORMATION ZEJULA (zuh-JOO-luh) (niraparib) tablets |
||
|
What is the most important information I should know about ZEJULA? ZEJULA may cause serious side effects including:
|
||
|
|
|
See “What are the possible side effects of ZEJULA?” for more information about side effects. |
||
|
What is ZEJULA? ZEJULA is a prescription medicine used to treat adults for:
It is not known if ZEJULA is safe and effective in children. |
||
|
Before taking ZEJULA, tell your healthcare provider about all of your medical conditions, including if you:
Tell your healthcare provider about all the medicines you take, including prescription and over-the-counter medicines, vitamins, and herbal supplements. |
||
|
How should I take ZEJULA?
|
||
|
What are the possible side effects of ZEJULA? ZEJULA may cause serious side effects, including:
The most common side effects of ZEJULA include: |
||
|
|
|
|
Your healthcare provider may change your dose, temporarily stop treatment, or permanently stop treatment with ZEJULA if you have certain side effects. These are not all the possible side effects of ZEJULA. Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088. |
||
|
How should I store ZEJULA?
Keep ZEJULA and all medicines out of the reach of children. |
||
|
General information about the safe and effective use of ZEJULA. Medicines are sometimes prescribed for purposes other than those listed in a Patient Information leaflet. Do not use ZEJULA for a condition for which it was not prescribed. Do not give ZEJULA to other people, even if they have the same symptoms that you have. It may harm them. You can ask your healthcare provider or pharmacist for information about ZEJULA that is written for health professionals. |
||
|
What are the ingredients in ZEJULA? Active ingredient: niraparib. Inactive ingredients: Core tablet: crospovidone, lactose monohydrate, magnesium stearate, microcrystalline cellulose, povidone, and silicon dioxide. Film-coating: Opadry II Gray (100 mg), Opadry II Blue (200 mg), or Opadry II Green (300 mg). For more information about ZEJULA, call 1-888-825-5249. Trademarks are owned by or licensed to the GSK group of companies. Opadry is a trademark owned by or licensed to its respective owner and is not owned by or licensed to the GSK group of companies. The maker of Opadry is not affiliated with and does not endorse the GSK group of companies or its products. Manufactured for: GlaxoSmithKline, Durham, NC 27701 ©2025 GSK group of companies or its licensor. ZJT:2PIL |
||
This Patient Information has been approved by the U.S. Food and Drug Administration Revised: June/2025
PRINCIPAL DISPLAY PANEL
NDC 0173-0909-13
Zejula
(niraparib)
tablets
100 mg
GSK
Rx only
30 tablets
Each 100-mg tablet is equivalent to 159.3 mg of niraparib tosylate monohydrate.
Store at 20°C to 25°C (68°F to 77°F); excursions are permitted between 15°C to 30°C (59°F to 86°F).[See USP Controlled Room Temperature]. Store and dispense in the original bottle.
Do not accept if membrane seal under cap is missing or broken. See prescribing information for dosage information. Keep out of reach of children.
Trademarks owned or licensed by GSK.
Mfd for GSK, Durham, NC 27701
©20243 GSK or licensor.
Rev. 9/24
MCK-150667-01
PRINCIPAL DISPLAY PANEL
NDC 0173-0912-13
Zejula
(niraparib)
tablets
200 mg
GSK
Rx only
30 tablets
Each 200-mg tablet is equivalent to 318.7 mg of niraparib tosylate monohydrate.
Store at 20°C to 25°C (68°F to 77°F); excursions are permitted between 15°C to 30°C (59°F to 86°F).[See USP Controlled Room Temperature]. Store and dispense in the original bottle.
Do not accept if membrane seal under cap is missing or broken. See prescribing information for dosage information. Keep out of reach of children.
Trademarks owned or licensed by GSK.
Mfd for GSK, Durham, NC 27701
©2024 GSK or licensor.
Rev. 9/24
MCK-150668-01
PRINCIPAL DISPLAY PANEL
NDC 0173-0915-13
Zejula
(niraparib)
tablets
300 mg
GSK
Rx only
30 tablets
Each 300-mg tablet is equivalent to 478.0 mg of niraparib tosylate monohydrate.
Store at 20°C to 25°C (68°F to 77°F); excursions are permitted between 15°C to 30°C (59°F to 86°F).[See USP Controlled Room Temperature]. Store and dispense in the original bottle.
Do not accept if membrane seal under cap is missing or broken. See prescribing information for dosage information. Keep out of reach of children.
Trademarks owned or licensed by GSK.
Mfd for GSK, Durham, NC 27701
©2024 GSK or licensor.
Rev. 9/24
MCK-150670-01
| ZEJULA
niraparib tablet, film coated |
||||||||||||||||||
|
||||||||||||||||||
|
||||||||||||||||||
|
||||||||||||||||||
|
||||||||||||||||||
|
||||||||||||||||||
|
||||||||||||||||||
| ZEJULA
niraparib tablet, film coated |
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
| ZEJULA
niraparib tablet, film coated |
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
| Labeler - GlaxoSmithKline LLC (167380711) |
Frequently asked questions
More about Zejula (niraparib)
- Check interactions
- Compare alternatives
- Pricing & coupons
- Reviews (58)
- Drug images
- Side effects
- Dosage information
- During pregnancy
- FDA approval history
- Drug class: PARP inhibitors
- Breastfeeding
- En español