Pancreatic Cancer
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is pancreatic cancer?
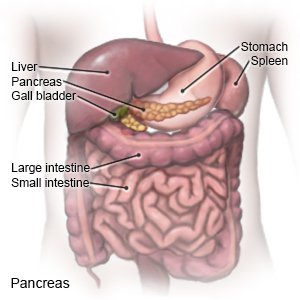
Pancreatic cancer starts in the pancreas. The pancreas is located just behind the stomach. It helps digest food by making enzymes. The pancreas also makes hormones, such as insulin, to help balance blood sugar levels.
 |
What increases my risk for pancreatic cancer?
- Cigarette smoking
- Diabetes
- Long-term pancreatitis (inflammation of the pancreas)
- Heavy alcohol use
- Obesity or a high-fat diet
- A family history of long-term pancreatitis or pancreatic cancer
What are the signs and symptoms of pancreatic cancer?
- Abdominal or low back pain
- Weight loss without trying
- Loss of appetite, nausea, or vomiting
- Fatigue and weakness
- Dark urine or light-colored bowel movements
- Jaundice (yellowing of the skin and the whites of the eyes)
How is pancreatic cancer diagnosed?
Your healthcare provider will examine you and ask about your symptoms. He or she may ask if you have a family history of pancreatic cancer. You may need any of the following:
- Ultrasound, CT, or MRI pictures will show the location and size of the cancer. Pictures may also show if cancer has spread to other places in your body. You may be given contrast liquid to help the cancer show up better in pictures. Tell the healthcare provider if you have ever had an allergic reaction to contrast liquid. Do not enter the MRI room with anything metal. Metal can cause serious injury. Tell the healthcare provider if you have any metal in or on your body.
- An endoscopy is a procedure used to check for a tumor. An endoscopic ultrasound uses sound waves to show your pancreas on a monitor. An endoscopic retrograde cholangiopancreatography (ERCP) may also be used to help open a narrow or blocked bile duct.
- A biopsy is a procedure to remove a small piece of tissue from your pancreas. A biopsy may be done during an endoscopic ultrasound or ERCP, or with a needle. The tissue sample will be sent to a lab to be tested for cancer.
- Genomic sequencing tests may show which cells are causing cancer. This can help your provider choose which medicine to give you.
How is pancreatic cancer treated?
- Medicines may be given to decrease pain or other symptoms. You may need pancreatic enzyme medicine to help your body digest protein, carbohydrates, and fats in your food. You may also need insulin to control your blood sugar level.
- Radiation therapy uses x-rays or gamma rays to treat cancer. Radiation kills cancer cells and may stop the cancer from spreading. It is also used to reduce symptoms, such as pain.
- Chemotherapy is medicine that kills cancer cells. Chemotherapy may also be used to shrink the tumor before surgery.
- Targeted therapy is medicine given to kill cancer cells without harming healthy tissue.
- Surgery is done to remove part or all of your pancreas and lymph nodes near your pancreas. It is most often done for tumors that have not spread to other parts of the body. The kind of surgery you need will depend on the size and location of the tumor.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
Related medications
What can I do to care for myself?
- Do not smoke. Nicotine and other chemicals in cigarettes and cigars can cause lung damage. Ask your healthcare provider for information if you currently smoke and need help to quit. E-cigarettes or smokeless tobacco still contain nicotine. Talk to your healthcare provider before you use these products.
- Eat small meals throughout the day. You may not feel hungry, but it is important that you eat. Proper nutrition can give you more energy, maintain your weight, and help you feel better. A dietitian can help you find ways to get enough protein, calories, vitamins, and minerals. Ask if you need to take a pancreatic enzyme supplement with meals to help with digestion.

- Drink liquids as directed. Ask how much liquid to drink each day and which liquids are best for you. You may need to drink more liquids than usual to prevent dehydration. This is especially true if you are vomiting or have diarrhea from cancer treatments.
- Limit or do not drink alcohol. Alcohol can make it difficult to manage your symptoms or side effects of treatment. Ask your oncologist before you drink alcohol. Also ask how much is okay for you to drink in 1 day or 1 week.
- Exercise as directed. Exercise may increase your energy level and appetite. Ask your healthcare provider how much exercise you need and which exercises are best for you.

Where can I find more information and support?
It may be difficult for you and your family to go through cancer and cancer treatments. Join a support group or talk with others who have gone through treatment.
- American Cancer Society
250 Williams Street
Atlanta , GA 30303
Phone: 1- 800 - 227-2345
Web Address: http://www.cancer.org
- National Cancer Institute
6116 Executive Boulevard, Suite 300
Bethesda , MD 20892-8322
Phone: 1- 800 - 422-6237
Web Address: http://www.cancer.gov
Call your local emergency number (911 in the US) for any of the following:
- You suddenly feel lightheaded and short of breath.
- You cough up blood.
When should I seek immediate care?
- Your arm or leg feels warm, tender, and painful. It may look swollen and red.
- Your pain does not get better, even after you take pain medicine.
- Your abdomen is larger than usual.
When should I call my doctor?
- You have new or worsening nausea or are vomiting.
- You have diarrhea, light-colored or oily, foul-smelling bowel movements.
- You have new or worsening weight loss, jaundice, or back pain.
- You feel depressed, anxious, or unable to cope with your condition.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Pancreatic Cancer
Treatment options
Symptoms and treatments
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
