Stroke
Medically reviewed by Drugs.com. Last updated on Jan 23, 2025.
What is a Stroke?

A stroke is a brain injury that occurs because the brain's blood supply is interrupted.
The brain's blood supply can be disrupted for different reasons. Doctors generally classify strokes into three categories, depending on the cause:
-
Hemorrhagic stroke — Bleeding (hemorrhage) causes this type of stroke. Bleeding can occur within the brain or between the brain and the skull. When bleeding occurs, small blood vessels near the hemorrhage tighten in a spasm. As a result, some brain areas get too little blood flow.
A hemorrhagic stroke that occurs within the brain is called an intracerebral hemorrhage. It often is linked to high blood pressure, old age, heavy alcohol use, or the use of cocaine or methamphetamines. A stroke that occurs between the brain and the skull is called a subarachnoid hemorrhage.
Hemorrhagic strokes are much less common than strokes caused by clots.
-
Thrombotic stroke — A blood clot (thrombus) forms inside one of the brain's arteries. It blocks blood flow. This usually happens inside an artery that has been narrowed by atherosclerosis. Atherosclerosis is the buildup of fatty deposits along the walls of blood vessels.
Thrombotic strokes are the most common type of stroke. They account for almost half of all strokes. Thrombotic strokes can affect large or small arteries in the brain. When a thrombotic stroke occurs in a small artery deep within the brain, the stroke is called a lacunar stroke.
-
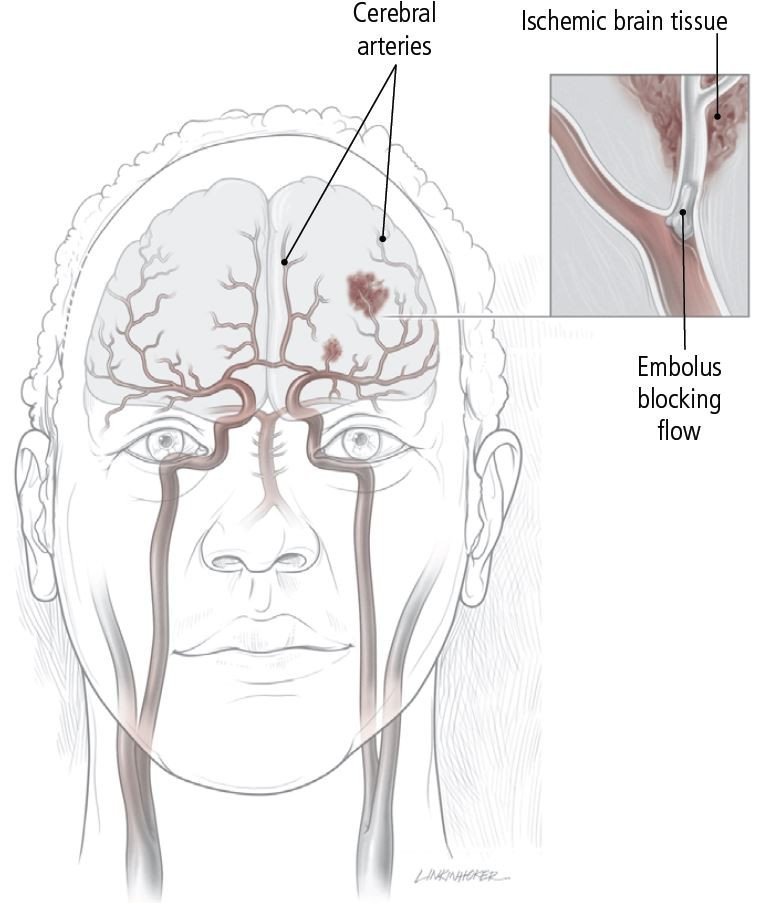
Embolic stroke — In an embolic stroke, a blood clot or other solid mass of debris travels to the brain, where it blocks a brain artery. In many cases a floating blood clot, called an embolus, originates inside the heart. In another type of embolic stroke, the floating debris is a clump of bacteria and inflammatory cells. This type of embolus can form if there is a bacterial infection on the valves of the heart.
|
|
In some cases, the type of stroke cannot be clearly determined.
Symptoms
Different areas of the brain are responsible for different functions. These include sensation, movement, sight, speech, balance, and coordination.
The symptoms of stroke vary depending on which area of the brain is damaged. Symptoms can include
- headache, with or without vomiting
- dizziness or confusion
- weakness or paralysis on one side of the body
- sudden, severe numbness in any part of the body
- visual disturbance, including sudden loss of vision
- difficulty walking, including staggering or veering
- coordination problems in the arms and hands
- slurred speech or inability to speak
- sudden deviation of the eyes toward one direction
- seizures
- irregular breathing
- stupor
- coma.
The sudden appearance of one or more of these symptoms is a warning sign that a stroke may be in progress.
In some cases, strokes are preceded by one or more transient ischemic attacks (TIAs). TIAs are brief episodes of stroke-like symptoms. Most often the symptoms last for only five to 20 minutes, with no permanent brain damage.
Diagnosis
Your doctor will review your medical history and your risk factors for stroke. Risk factors for stroke include
- high blood pressure
- smoking
- diabetes
- certain types of heart disease
- family history of stroke.
Your doctor will examine you. He or she will pay specific attention to your blood pressure and your heart. The doctor will do a neurological examination to check for changes in your brain function.
To diagnose and classify your stroke, your doctor will need an imaging test of the brain. Tests can include:
- Computed tomography (CT) scan. Creates cross-sectional images of the head and brain.
- Magnetic resonance imaging (MRI). Uses magnetic fields to detect changes in brain tissue. MRI can provide an earlier and more accurate diagnosis of stroke than CT scan. But it is not as widely available as CT.
Depending on the type of stroke suspected, your doctor may do a lumbar puncture (also called a spinal tap). This checks your cerebrospinal fluid for blood. Other imaging tests, such as Doppler ultrasonography or MRI angiography, may be used to evaluate blood flow to your brain.
If it is clear that you are having a stroke, your evaluation will include tests to check for a cause. You may have a chest x-ray and an electrocardiogram (EKG). Blood tests will evaluate your blood cell counts and the ability of your blood to clot. You may undergo ultrasound testing of the arteries in the neck (carotid Doppler) or of the heart (echocardiogram).
Expected duration
If circulation to the brain is restored quickly, symptoms can improve within a few days. If the blood supply is interrupted for longer periods, brain injury can be more severe. Symptoms can last for many months. You may need physical rehabilitation.
Permanent brain damage can cause permanent disability. Some people, especially those who have a large hemorrhagic stroke, can die.
Prevention
You can help to prevent stroke by controlling risk factors. Risk factors for stroke include
- high blood pressure
- smoking
- abnormal heart rhythm (atrial fibrillation)
- high cholesterol
- atherosclerosis
- diabetes.
A healthy lifestyle and taking a daily aspirin can also help to prevent stroke.
Several medicines to treat high blood pressure are especially beneficial in preventing stroke. These include ACE inhibitors and thiazide diuretics.
If you have or have had atrial fibrillation, blood-thinning medication can greatly reduce your risk of stroke. Approved drugs for this use include warfarin (Coumadin), apixaban (Eliquis), dabigatran (Pradaxa), and rivaroxaban (Xarelto). They prevent clots from forming inside the heart. These are clots that might later dislodge and cause a stroke.
High cholesterol also should be treated aggressively. Cholesterol-lowering medications called statins can help to prevent strokes.
To help prevent stroke, you should exercise regularly and eat a healthy diet. A healthy diet
- is rich in fruits and vegetables
- is low in saturated fats, trans fats, and cholesterol
- includes two to four servings of fish per week
- avoids excessive alcohol.
In addition, never take cocaine or amphetamines (unless amphetamines are prescribed by your doctor): they can cause strokes.
Talk to your doctor about the potential benefits of taking an aspirin daily. Aspirin, in doses as low as 80 milligrams per day, can reduce the risk of stroke. Be aware, however, that daily aspirin slightly increases the risk of hemorrhagic stroke. Other medications can also help to prevent clots. Aspirin and other clot-preventing medicines are not safe for everyone.
Drugs used to treat this and similar conditions
Treatment
It is important to be aware of stroke symptoms. Seek immediate emergency care if you experience stroke symptoms.
The doctor will first try to determine whether your stroke is caused by a clot or bleeding. Based on this information, he or she will begin the appropriate treatment.
Thrombotic and embolic strokes
The most effective treatment for strokes caused by a clot is either a procedure to remove the clot or using a powerful clot-dissolving medication called tissue plasminogen activator (t-PA). Both may restore blood flow and oxygen to brain tissue affected by a stroke. But action must be taken as soon as possible — ideally within three hours of when stroke symptoms begin. That's why it is so important to get immediate medical care at the first sign of what might be a stroke. People who receive one of these therapies have less long-term disability following a stroke.
In treating thrombotic stroke, clot-prevention medications, such as heparin, may be used in later hours after a stroke. These medicines prevent existing blood clots from getting bigger. They also prevent new clots from forming.
After a stroke has stabilized, aspirin or another agent is usually prescribed daily to prevent another stroke.
People with an embolic stroke secondary to blood clots that originally formed in the heart should receive a blood-thinning medication to reduce the chance of another stroke. Warfarin (Coumadin) is the standard drug prescribed most frequently. For atrial fibrillation not related to a heart valve abnormality, alternatives to warfarin, such as apixaban (Eliquis), dabigatran (Pradaxa), and rivaroxaban (Xarelto), may be prescribed.
Hemorrhagic strokes
T-PA is not helpful to treat hemorrhagic stroke. In fact, it can cause more bleeding.
Sometimes, the hemorrhaged blood may have to be removed through surgery to relieve pressure on the brain. Occasionally, testing reveals that an abnormality of a blood vessel has caused the hemorrhage. This may require treatment with surgery in order to prevent another stroke.
Follow-up care
A person who has experienced a significant stroke of any type usually is hospitalized for observation in case the symptoms worsen. A severe stroke can affect breathing. Some people may need a breathing machine to help them breathe.
People who have had a stroke may need help with self-care or feeding. Early intervention by an occupational therapist and physical therapist is helpful. These therapists can help a person work around a new disability and regain strength after brain injury.
Hospitalization is often followed by a period of residence at a rehabilitation center. There, additional therapy may be provided intensively. The goal of rehabilitation is to maximize recovery.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
When to call a professional
If you or someone you are with develops any of the symptoms of stroke, call a doctor right away. Or call an ambulance or go to an emergency room.
It is important to be evaluated even if your symptoms last only a few minutes, and then go away. Symptoms of a stroke that go away are called a transient ischemic attack (TIA). A TIA can be a warning sign of a coming stroke. About 1 of 10 people who experience a TIA has a stroke during the next three months.
People who see a doctor immediately after having a TIA can receive treatment. This might include treatment for high blood pressure and high cholesterol, or an aspirin plan. If these risks are addressed quickly, you can significantly lower your risk for having a stroke over the next three months.
Prognosis
If the brain's blood supply is restored quickly and completely, the person may recover with little or no disability. In people with thrombotic strokes, early treatment with the clot-dissolving drug t-PA may reduce disability significantly.
Additional info
National Institute of Neurological Disorders and Stroke
https://www.ninds.nih.gov/
National Stroke Association
https://www.stroke.org/
American Heart Association (AHA)
https://www.heart.org/
Learn more about Stroke
- Atorvastatin (Lipitor): Top 12 Drug Facts You Need to Know
- Should you mix muscle relaxants with alcohol?
Treatment options
Care guides
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.