Transurethral Prostatectomy
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What do I need to know about a transurethral prostatectomy (TURP)?
A TURP is surgery to remove part or all of your prostate gland. This surgery is also called transurethral resection of the prostate.
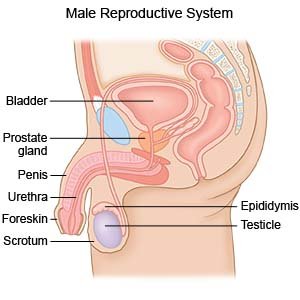 |
How do I prepare for a TURP?
- You may be given medicine to empty your bowels the day before surgery. Your healthcare provider will give you instructions.
- You may be told not to eat or drink anything after midnight on the day of surgery. Arrange to have someone drive you home after surgery.
- Tell your surgeon about all the medicines you currently take. He or she will tell you if you need to stop any medicine before surgery, and when to stop. He or she will tell you which medicines to take or not take on the day of surgery.
- Tell your surgeon if you have heart disease or blood clotting problems.
- You may be given medicine to shrink the size of your prostate. You may also be given antibiotics to help prevent or treat a bacterial infection. Tell your surgeon if you had an allergic reaction to antibiotics, anesthesia, or other medicine.
- You may need blood and urine tests. You may also need a rectal exam to check the size of your prostate.
Related medications
Treatment options
The following list of medications are related to or used in the treatment of this condition.
What will happen during a TURP?
- You may be given anesthesia to make you lose feeling from the waist down, or to keep you asleep during surgery. Your surgeon will insert a resectoscope through your urethra. A resectoscope is a tube with a small monitor on the end. The monitor shows your prostate on a screen during surgery. Your bladder may be filled with fluid during surgery.
- Heat that is produced by the resectoscope will be used to remove part, or all, of your prostate. Heat will also be used to stop bleeding in the surgery area. Fluid is used to wash away extra tissue and blood. The resectoscope will be removed from your urethra. A catheter (soft tube) will be put through your urethra and into your bladder. The catheter will be left in place to drain urine out of your body and into a bag.
What should I expect after a TURP?
A Foley catheter is inserted to drain urine into a bag. Your healthcare provider will tell you how to clean around the catheter if you go home with one. You will need to clean the area 2 times a day to prevent infection. You may have feelings of urgency and difficulty controlling your urine. You may have pain when you urinate and also a small amount of blood in your urine. You may also have a problem getting an erection and keeping one.
What are the risks of a TURP?
- Your prostate, bladder, or urethra may be damaged. Your urethra or part of your bladder may grow narrow. This can make it difficult or painful to urinate. You may feel like you need to urinate often, or have trouble controlling when you urinate. You may get blood clots in your urine that can block your urethra.
- You may develop a urinary tract infection, or an infection in the surgery area. You may have trouble getting an erection or ejaculating. You may develop TURP syndrome, which can cause dizziness, fatigue, stomach pain, and vomiting. If you had a partial resection of the prostate, the part of your prostate that was not removed may grow too large. This can cause your signs and symptoms to return, and you may need to have surgery again.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Transurethral Prostatectomy
Treatment options
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
