Transurethral Prostatectomy
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
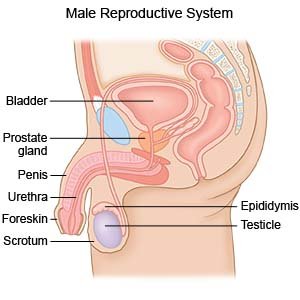
A TURP is surgery to remove part or all of your prostate gland. This surgery is also called transurethral resection of the prostate. After surgery, you may have feelings of urgency and difficulty controlling your urine. You may have pain when you urinate and also a small amount of blood in your urine. You may also have a problem getting an erection and keeping one.
 |
DISCHARGE INSTRUCTIONS:
Seek care immediately if:
- You have severe abdominal or back pain.
- You are dizzy or confused.
- You have abdominal pain, nausea, and vomiting.
- Your heartbeat is slower than usual.
Call your doctor or urologist if:
- You urinate little or not at all.
- You have a fever.
- You have new or more blood in your urine.
- You have trouble starting to urinate, or have a weak stream of urine when you urinate.
- You feel like you have a full bladder, even after you urinate.
- You often wake up during the night to urinate.
- You feel pain or pressure in your lower abdomen.
- Your urine looks cloudy, and smells bad.
- You have questions or concerns about your condition or care.
Medicines:
You may need any of the following:
- Prescription pain medicine may be given. Ask your healthcare provider how to take this medicine safely. Some prescription pain medicines contain acetaminophen. Do not take other medicines that contain acetaminophen without talking to your healthcare provider. Too much acetaminophen may cause liver damage. Prescription pain medicine may cause constipation. Ask your healthcare provider how to prevent or treat constipation.
- Antibiotics prevent or fight an infection caused by bacteria.
- Take your medicine as directed. Contact your healthcare provider if you think your medicine is not helping or if you have side effects. Tell your provider if you are allergic to any medicine. Keep a list of the medicines, vitamins, and herbs you take. Include the amounts, and when and why you take them. Bring the list or the pill bottles to follow-up visits. Carry your medicine list with you in case of an emergency.
Related medications
Treatment options
The following list of medications are related to or used in the treatment of this condition.
Foley catheter care:
Keep the bag below your waist. If the bag is too high, urine will flow back into your bladder. This can cause an infection. Do not pull on the catheter. This may cause pain and bleeding, and the catheter may come out. Do not let the catheter tubing kink or twist. A kink or twist will block the flow of urine. Your healthcare provider will tell you how to clean around the catheter if you go home with one You will need to clean the area 2 times a day to prevent infection.
Bladder control:
After surgery, you may leak urine and have trouble controlling when you urinate. The following can help decrease or manage urine leakage:
- Drink fluids as directed. Fluids may help your kidneys and bladder work properly. Fluids can also decrease your chance for infections. Ask your healthcare provider which fluids are best for you and how much you should drink.
- Do not have caffeine. Caffeine can cause problems with bladder control and increase your need to urinate.
- Wear a pad or adult diapers, if needed. These may help to absorb leaking urine and decrease odor.
- Do pelvic floor muscle exercises. Pelvic floor muscle exercises, also called Kegels, may help improve your bladder control. These exercises are done by tightening and relaxing your pelvic muscles. Ask how to do pelvic floor muscle exercises, and how often to do them.
Activity guidelines:
Ask when it is okay for you to return to work and activities, or to have sex.
Follow up with your surgeon or urologist as directed:
You may need to return to make sure you do not have an infection, or to have your Foley catheter removed. Write down your questions so you remember to ask them during your visits.
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Learn more about Transurethral Prostatectomy
Treatment options
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
