Trabeculectomy
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
WHAT YOU NEED TO KNOW:
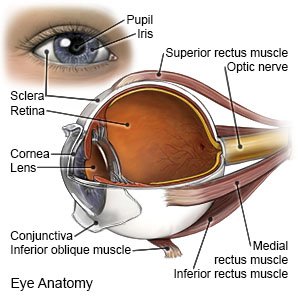
A trabeculectomy is surgery to treat open angle glaucoma. The trabecular meshwork is the drainage system for your eye. A trabeculectomy will help repair the drainage system and decrease your eye pressure.
 |
HOW TO PREPARE:
The week before your surgery:
- Arrange for someone to drive you home and stay with you for at least 24 hours after surgery.
- Do not drink alcohol for 48 hours before surgery. Alcohol can dehydrate you and make your eyes too dry for surgery.
- Tell your provider about all medicines you currently take. He or she will tell you if you need to stop any medicine, and when to stop. He or she will tell you which medicines to take or not take on the day of the procedure.
- Your doctor may give you eyedrops to use 3 or 4 days before surgery to help prevent infection.
- You may need blood tests before your procedure. Talk to your provider about these or other tests you may need. Write down the date, time, and location for each test.
- Get sunglasses with UVB protection to wear after surgery.
The night before your surgery:
Ask about directions for eating and drinking.
The day of your surgery:
- Use your eyedrops and other medicines as directed. Bring your medicines with you to your surgery.
- Do not wear contact lenses, earrings, or hearing aids.
- Do not wear makeup or lotion on your face.
- You or a close family member will be asked to sign a legal document called a consent form. It gives healthcare providers permission to do the procedure or surgery. It also explains the problems that may happen, and your choices. Make sure all your questions are answered before you sign this form.
- Healthcare providers may insert an intravenous tube (IV) into your vein. A vein in the arm is usually chosen. You may be given liquids or medicine through the IV.
- An anesthesiologist will talk to you before your surgery. You may need medicine to keep you asleep or numb an area of your body during surgery. Tell healthcare providers if you or anyone in your family has had a problem with anesthesia in the past.
WHAT WILL HAPPEN:
What will happen:
- You will be given eyedrops to numb your eye. You may also be given medicine to help keep you relaxed during surgery. Your provider will use an eyelid holder to keep your eye wide open during surgery. He or she will make a tiny hole in the top of your sclera. A small piece of the sclera will be removed.
- A piece of the conjunctiva (clear layer that covers your eye) will be stitched over the hole in the sclera. When eye fluid flows out of the hole, it forms a pocket on the surface of the sclera. The hole allows enough eye fluid to flow out to keep your eye pressure at a healthy level.
- Stitches will be used to close the incisions. The stitches in your eye will dissolve on their own. Eyedrops or ointment will be put in your eye after surgery. A bandage will be taped over your eye. This keeps the area clean and dry to prevent infection. A metal or plastic shield may be placed over the bandage to prevent you from accidentally bumping your eye.
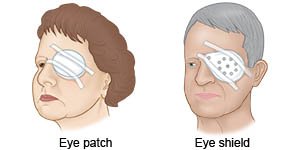
After your surgery:
You will be taken to a room where you can rest after your surgery. Your eye doctor will check your eye pressure. You will be able to go home when your eye doctor says it is okay.
CONTACT YOUR HEALTHCARE PROVIDER IF:
- You cannot make it to your surgery.
- You have a fever.
- You get a cold or the flu.
- You have questions or concerns about your surgery.
Seek Care Immediately if
- You have severe eye pain.
- You have a sudden change in your vision.
Risks
You may get an infection or your eye may bleed. Your eye pressure may not get better and could become worse. Your vision may be worse than before the surgery. You may develop cataracts (cloudy, dark vision) after laser surgery. You could lose your vision. You may develop a scar that causes the hole to close. This could make your eye pressure increase again.
Related medications
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
