Laparoscopic Bowel Resection
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What do I need to know about laparoscopic bowel resection?
Laparoscopic bowel resection is surgery to remove all or parts of the small or large intestine (bowel). This is done to treat conditions such as intestinal bleeding, blockages, inflammation, or infections. It may also be done to remove large polyps (growths) or early signs of tumors in the intestines. The amount of intestine removed depends on the reason this surgery is needed. An ileostomy or colostomy may also be made. This is an opening in the abdomen to drain bowel movement into a bag.
 |
What health information do I need to give my surgeon?
- Tell your surgeon about all medicines you currently take. He or she will tell you if you need to stop any medicine for surgery, and when to stop. He or she will tell you which medicines to take or not take on the day of surgery.
- You may be given antibiotic medicine 30 minutes before your surgery to help prevent a bacterial infection. Tell your surgeon if you had an allergic reaction to an antibiotic.
- You may need to take medicine to thin your blood. Blood thinning medicine helps prevent blood clots from forming in your veins. Tell your surgeon if you have a bleeding disorder or a history of bleeding or blood clots.
- Tell your surgeon if you have other diseases, including diabetes, bleeding disorders, or heart or kidney problems.
- Tell your surgeon if you have had other abdominal surgeries.
- If you are female, tell your surgeon if you know or think you might be pregnant.
How do I prepare for surgery?
- Your surgeon will tell you how to prepare. Arrange to have someone drive you home from surgery.
- Directions for eating and drinking:
- A clear liquid diet or a diet that helps to clean out your bowel may be started 1 to 4 days before your surgery. Clear liquids may include plain gelatin, unsweetened fruit juices, clear soup, or broth.
- Do not eat foods with fiber or that are hard to digest. Some examples include fruits, vegetables, cereal, nuts, peas, beans, fried foods, and bread.
- Increase the amount of water you are drinking. Make sure you drink 8 to 10 (eight-ounce) cups of liquid, especially on the day before your surgery.
- You may need to have abdominal x-rays, a CT scan, ultrasound, or colonoscopy. Other tests may also be needed, such as chest x-ray, electrocardiogram (ECG), or blood or urine tests.
Related medications
What do I need to do the day before surgery?
- Drink 8 to 10 (eight-ounce) cups of liquid during the day.
- You will need to clean out your bowel to get ready for this surgery. An enema uses warm water that is put into your rectum to help empty your bowel. You may be given 8 to 12 (eight-ounce) cups of bowel prep medicine to drink.
- If you have diabetes, ask your surgeon for instructions about what you may eat and drink before your surgery. If you use medicine to treat diabetes, your surgeon may have instructions about using it before surgery. You may need to check your blood sugar more often before and after surgery.
What will happen during surgery?
- General anesthesia will be used to keep you asleep and free from pain during surgery. Your surgeon will make a small incision near your belly button. A laparoscope will be put into the incision. He or she will insert other tools through 2 to 5 small incisions on your abdomen.
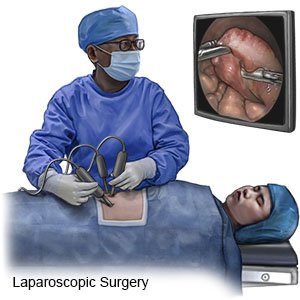
- Your abdomen will then be filled with a gas (carbon dioxide) to lift the abdominal wall away from the internal organs. The affected bowel will be separated from the healthy part. Blood vessels will be tied and cut. Your surgeon will then remove all or part of the small or large bowel. The remaining healthy parts of the bowel will then be attached or sewn together.
- Your surgeon may send samples of bowel tissues to a lab for tests. Lymph nodes may also be removed during surgery. Drains may be placed to remove fluid or pus from your abdomen. A colostomy or ileostomy may be made. The incisions will be closed by stitches or surgical tape and covered with bandages.
What should I expect after surgery?
- You will be taken to a recovery room until you are fully awake. Do not get out of bed until healthcare providers say it is okay. When providers see that you are okay, you will be taken back to your hospital room. The bandages used to cover your stitches keep the area clean and dry to prevent infection. A provider may remove the bandages soon after your surgery to check your wound, tubes, drains, or ostomy.
- The gas used during your surgery may cause shoulder or chest pain for 1 to 2 days after your surgery.
- You will be helped to walk around after surgery. Movement helps prevent blood clots.
- Medicines may be given to prevent or treat pain or nausea. Blood thinning medicine may be given to help prevent blood clots. You may also need medicine to make it easier to have a bowel movement. This medicine can also help prevent constipation.
- You may develop a condition called post-operative ileus. This condition means your bowel did not start working as expected after surgery. You may have nausea, vomit, or have no gas or bowel movements. You may also have abdominal pain and feel bloated. This condition may last for a few days. Healthcare providers may help you walk around to get your bowels moving. You may also need medicines and be on a liquid diet, or you may need a nasogastric (NG) tube. An NG tube is put into your nose, and passes down your throat until it reaches your stomach. Food and medicine may be given through an NG tube.
- You may be able to eat when bowel sounds are heard. Ice chips are usually given first. Liquids may be given within a few days. If you have a colostomy or ileostomy, you may not be able to eat solid food for several days.
What are the risks of laparoscopic bowel resection?
Problems may happen during your laparoscopic surgery that may lead to an open surgery. Your stomach, liver, intestines, blood vessels, or nerves may get injured during surgery. This may cause too much bleeding, or the bowel contents may leak. You could also have trouble breathing or an infection during or after surgery. You may also develop a life-threatening blood clot.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
