Diverticulosis
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is diverticulosis?
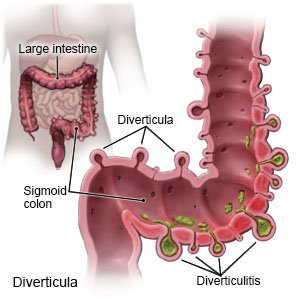
Diverticulosis is a condition that causes small pockets called diverticula to form in your intestine. These pockets make it difficult for bowel movements to pass through your digestive system.
 |
What causes diverticulosis?
Diverticula form when muscles have to work hard to move bowel movements through the intestine. The force causes bulges to form at weak areas in the intestine. This may happen if you eat foods that are low in fiber. Fiber helps give your bowel movements more bulk so they are larger and easier to move through your colon. The following may increase your risk of diverticulosis:
- A history of constipation
- Age 40 or older
- Obesity
- Lack of exercise
What are the signs and symptoms of diverticulosis?
Diverticulosis usually does not cause any signs or symptoms. It may cause any of the following in some people:
- Pain or discomfort in your lower abdomen
- Abdominal bloating
- Constipation or diarrhea
How is diverticulosis diagnosed?
Your healthcare provider will examine you and ask about your bowel movements, diet, and symptoms. He or she will also ask about any medical conditions you have or medicines you take. You may need any of the following:
- Blood tests may be done to check for signs of inflammation.
- A barium enema is an x-ray of your colon that may show diverticula. A tube is put into your anus, and a liquid called barium is put through the tube. Barium is used so that healthcare providers can see your colon more clearly.
- Flexible sigmoidoscopy is a test to look for any changes in your lower intestines and rectum. It may also show the cause of any bleeding or pain. A soft, bendable tube with a light on the end will be put into your anus. It will then be moved forward into your intestine.
- A colonoscopy is used to look at your whole colon. A scope (long bendable tube with a light on the end) is used to take pictures. This test may show diverticula.
- A CT scan , or CAT scan, may show diverticula. You may be given contrast liquid before the scan. Tell the healthcare provider if you have ever had an allergic reaction to contrast liquid.
Related medications
Treatment options
The following list of medications are related to or used in the treatment of this condition.
How is diverticulosis managed?
The goal of treatment is to manage any symptoms you have and prevent other problems such as diverticulitis. Diverticulitis is swelling or infection of the diverticula. Your healthcare provider may recommend any of the following:
- Eat a variety of high-fiber foods. High-fiber foods help you have regular bowel movements. High-fiber foods include cooked beans, fruits, vegetables, and some cereals. Most adults need 25 to 35 grams of fiber each day. Your healthcare provider may recommend that you have more. Ask your healthcare provider how much fiber you need. Increase fiber slowly. You may have abdominal discomfort, bloating, and gas if you add fiber to your diet too quickly. You may need to take a fiber supplement if you are not getting enough fiber from food.

- Medicines to soften your bowel movements may be given. You may also need medicines to treat symptoms such as bloating and pain.
- Drink liquids as directed. You may need to drink 2 to 3 liters (8 to 12 cups) of liquids every day. Ask your healthcare provider how much liquid to drink each day and which liquids are best for you.
- Apply heat on your abdomen for 20 to 30 minutes every 2 hours for as many days as directed. Heat helps decrease pain and muscle spasms.
How can I help prevent diverticulitis or other symptoms?
The following may help decrease your risk for diverticulitis or symptoms, such as bleeding. Talk to your provider about these or other things you can do to prevent problems that may occur with diverticulosis.
- Exercise regularly. Ask your healthcare provider about the best exercise plan for you. Exercise can help you have regular bowel movements. Get 30 minutes of exercise on most days of the week.

- Maintain a healthy weight. Ask your healthcare provider what a healthy weight is for you. Ask him or her to help you create a weight loss plan if you are overweight.
- Do not smoke. Nicotine and other chemicals in cigarettes increase your risk for diverticulitis. Ask your healthcare provider for information if you currently smoke and need help to quit. E-cigarettes or smokeless tobacco still contain nicotine. Talk to your healthcare provider before you use these products.
- Ask your healthcare provider if it is safe to take NSAIDs. NSAIDs may increase your risk of diverticulitis.
When should I seek immediate care?
- You have severe pain on the left side of your lower abdomen.
- Your bowel movements are bright or dark red.
When should I call my doctor?
- You have a fever and chills.
- You feel dizzy or lightheaded.
- You have nausea, or you are vomiting.
- You have a change in your bowel movements.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Diverticulosis
Treatment options
- Medications for Diverticulitis
- Medications for Diverticulitis with Hemorrhage
- Medications for Gastrointestinal Diverticula
- Medications for Gastrointestinal Diverticula with Hemorrhage
Care guides
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
