Cystic Fibrosis in Children
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
Cystic fibrosis (CF) is a lifelong condition that affects your child's lungs, digestive system, and other organs. Mucus, tears, sweat, and saliva become so thick and sticky that they clog the lungs and digestive system. CF typically causes problems with breathing and with breaking down and absorbing food.
WHILE YOU ARE HERE:
Informed consent
is a legal document that explains the tests, treatments, or procedures that your child may need. Informed consent means you understand what will be done and can make decisions about what you want. You give your permission when you sign the consent form. You can have someone sign this form for you if you are not able to sign it. You have the right to understand your child's medical care in words you know. Before you sign the consent form, understand the risks and benefits of what will be done to your child. Make sure all of your questions are answered.
Stay with your child for comfort and support
as often as possible while he or she is in the hospital. Ask another family member or someone close to the family to stay with your child when you cannot be there. Bring items from home that will comfort your child, such as a favorite blanket or toy.
Nutrition:
Your child may need to eat foods that have extra calories, fat, vitamins, or calcium. A dietitian will help you choose the best foods to give your child energy and strength.
Oxygen:
Your child may need extra oxygen if his or her blood oxygen level is lower than it should be. Your child may get oxygen through a mask placed over the nose and mouth or through small tubes placed in the nostrils. Ask your child's healthcare provider before you take off the mask or oxygen tubing.
Related medications
Medicines:
- Antibiotics help fight or prevent an infection caused by bacteria.
- Steroids help decrease inflammation in your child's lungs and help him or her breathe more easily.
- Mucus-thinning medicine is breathed in to help thin lung mucus so your child can cough it up more easily.
- Bronchodilators help open the air passages in your child's lungs, and help him or her breathe more easily.
- Pancreatic enzymes help your child's digestive system break down food and absorb nutrients properly.
Tests:
- Blood tests may show be used to find signs of infection and to check kidney function.
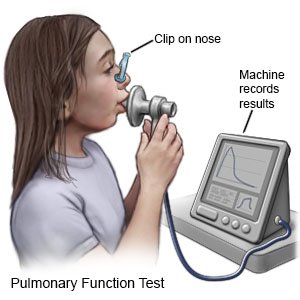
- Pulmonary function tests will show how much oxygen your child's body is getting. He or she breathes into a mouthpiece connected to a machine. The machine measures how much air he or she breathes in and out over a certain amount of time.
- A sputum sample is tested to find common sources of infection that can happen along with CF. Mucus from your child's lungs is collected in a cup when he or she coughs. He or she may need to give 3 samples of sputum, usually first thing in the morning.
- A fecal fat test is used to check the amount of fat in your child's bowel movements. His or her body may not be able to absorb fat from the foods he or she eats. You will be told how to get a sample of each bowel movement your child has over a 72 hour period.
- CT scan pictures of your child's sinuses may show growths, swelling, or mucus buildup. Your child may be given contrast liquid to help providers see problems better in the pictures. Tell the provider if your child has ever had an allergic reaction to contrast liquid.
Treatment:
- Airway clearance techniques are exercises to help remove mucus so your child can breathe more easily. Your child's healthcare provider will show him or her how to do the exercises. These exercises may be used along with machines or special devices to help decrease your child's symptoms and risk for infection.
- Surgery may be needed if your child has severe damage to organs, such as his or her liver or lungs. Ask your child's healthcare provider for more information about surgery.
- A ventilator is a machine that gives your child oxygen and breathes for him or her when needed. An endotracheal (ET) tube is put into your child's mouth or nose and attached to the ventilator. He or she may need a trach if an ET tube cannot be placed. A trach is a tube put through an incision and into his or her windpipe.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
RISKS:
Your child's symptoms may not go away, or may come back after treatment. His or her lungs, liver, or pancreas may be damaged. Your child may not get enough nutrients. He or she may not grow and gain weight properly. He or she may become weak and have an increased risk for broken bones. Your child can develop pancreatitis or diabetes. He or she may be at higher risk for lung infections. Your child's liver can develop cirrhosis (scarring) and not work normally. He or she may have severe breathing or bleeding problems, or a collapsed lung. These problems can be life-threatening.
CARE AGREEMENT:
You have the right to help plan your child's care. Learn about your child's health condition and how it may be treated. Discuss treatment options with your child's healthcare providers to decide what care you want for your child.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Learn more about Cystic Fibrosis
Treatment options
Care guides
Symptoms and treatments
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
