Biceps Tenodesis
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
AMBULATORY CARE:
What you need to know about a biceps tenodesis:
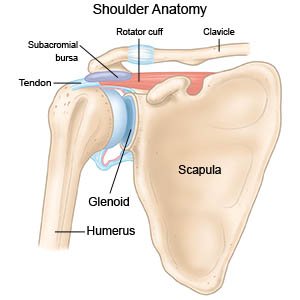
Biceps tenodesis is surgery to repair a biceps tendon tear or to help make the tendon more stable. The biceps tendon will be detached from your shoulder socket. The damaged part of the tendon will be removed. Then the tendon will be attached to your upper arm bone (called the humerus). This helps relieve pain in your shoulder and make it more stable.
 |
How to prepare for surgery:
- This surgery may be done as an open surgery or arthroscopically. During an open procedure one large and several small incisions are made. During an arthroscopic procedure, several small incisions are made. An arthroscope is used to look inside your joint. Your surgeon will insert tools and the arthroscope into the incisions to work on the tendon. Your surgeon will talk to you about which kind of surgery is right for you.
- You may be given medicine to use to clean your skin. You will need to use it at home a few days before surgery and on the day of surgery. The medicine will come as a soap to shower with or cloths to wipe the area. Your healthcare provider will give you specific instructions if you need to use this medicine.
- Your surgeon will tell you how to prepare for surgery. You will be told not to eat or drink anything after midnight on the day of surgery. Your surgeon will tell you which medicines to take or not take on the day of surgery. Arrange for someone to drive you home after surgery and stay with you for at least 24 hours.
What will happen during surgery:
- You will be given medicine to keep you asleep and pain-free during surgery.
- The 2 main kinds of biceps tenodesis surgery are soft tissue and hardware fixation:
- For a soft tissue surgery, the tendon is moved into a groove made in the humerus. Your surgeon will detach the tendon, roll the end into a ball, and stitch it together. Then it is put into the groove made in the humerus and moved so it will stay in place.
- For a hardware fixation surgery, the tendon is moved into a hole your surgeon will make. A screw or other device will be used to fix the tendon to the bone.
What will happen after surgery:
Your arm will be put into a sling for up to 6 weeks to keep it from moving while you heal. Your healthcare providers will tell you if you need to sleep in the sling and when to wear it during the day. You may have a stiff or painful shoulder after surgery. This is normal and should get better with time and physical therapy. Your providers will tell you when to start having shoulder rehabilitation. These are exercises that will help increase your range of motion.
Risks of a biceps tenodesis:
You may develop an infection or bleed more than expected during surgery. You may also develop a hematoma (collection of blood) or a seroma (collection of fluid) under your skin. Nerves or veins may be injured or the humerus may be broken. You may have an allergic reaction to the fixation device. Any device used to fix the tendon to bone may fail. You may have chronic shoulder pain or stiffness, even after physical therapy.
Seek care immediately if:
- Blood soaks through your bandage.
- You cannot feel or move your fingers or arm.
Related medications
Contact your healthcare provider if:
- You have signs of infection in the surgery wound, such as swelling, pus, or red streaks.
- You have a fever or chills.
- You have severe pain that is not helped with pain medicine.
- You have questions or concerns about your condition or care.
Medicines:
- Prescription pain medicine may be given. Ask your healthcare provider how to take this medicine safely. Some prescription pain medicines contain acetaminophen. Do not take other medicines that contain acetaminophen without talking to your healthcare provider. Too much acetaminophen may cause liver damage. Prescription pain medicine may cause constipation. Ask your healthcare provider how to prevent or treat constipation.
- Take your medicine as directed. Contact your healthcare provider if you think your medicine is not helping or if you have side effects. Tell your provider if you are allergic to any medicine. Keep a list of the medicines, vitamins, and herbs you take. Include the amounts, and when and why you take them. Bring the list or the pill bottles to follow-up visits. Carry your medicine list with you in case of an emergency.
Apply ice to your shoulder:
Ice helps decrease swelling and pain and may help prevent tissue damage. Use an ice pack or put crushed ice in a plastic bag. Cover the bag with a towel before you apply it to your skin. Apply the pack or bag to your shoulder for 15 to 20 minutes every hour, or as directed. Your healthcare provider will tell you how often to do this and for how many days after surgery.
Care for your incision wound as directed:
- Keep your wound dry. When your healthcare provider says it is okay to bathe, cover the incision wound with a plastic bag. Tape the ends of the bag to your skin so water does not get in. Take showers instead of baths until your healthcare provider says it is okay to take a bath. Do not swim or soak in a hot tub.
- Clean your wound as directed. Your healthcare provider will tell you when it is okay to remove the bandage and care for your wound. He or she will tell you how often to clean the wound and what to use to clean it. Check for signs of infection each time you care for the wound. Signs include pus, swelling, a fever, chills, and red streaks coming from the wound.
Activity:
- Your healthcare provider and physical therapist will give you specific instructions to follow. It is very important to follow the instructions carefully so you do not injure your shoulder while it is healing.
- Your healthcare provider will tell you when you can start driving and doing your normal activities again. Tell your provider what kind of work you do. You may need specific instructions if you do work that requires lifting objects or moving your arm overhead.
- Do not lift anything until your healthcare provider says it is okay.
- Do not play any sports that need throwing or overhead motion (such as baseball or tennis) until at least 16 weeks after surgery. Talk to your healthcare provider or physical therapist to make sure you are ready for this activity.
Go to physical therapy as directed:
Physical therapy will happen in 4 phases:
- The protective phase is the first 6 weeks after surgery. You will need to protect your shoulder by wearing a sling. Your healthcare providers will tell you how long to wear the sling each day and if you need to sleep in it. During this time, you will mainly do passive range-of-motion exercises. This means your physical therapist will gently move your shoulder in different directions to keep it flexible.
- The moderate protection phase is from week 7 to week 12. You will start wearing the sling less often. Physical therapy will focus on strengthening your rotator cuff. You will use bands or weights to help with this. You will begin to strengthen your biceps at about week 10. Your physical therapist will help you do this safely. You may also need to do stretching exercises at week 10 to improve your range of motion.
- The minimum protection phase is from week 13 to week 20. You will be doing active and passive range-of-motion exercises at this stage. You will also do exercises to increase strength.
- The advanced strengthening phase is from week 21 to week 26. At this stage, you will be doing advanced exercises to increase strength.
Follow up with your doctor as directed:
Write down your questions so you remember to ask them during your visits.
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
