Macular degeneration
Medically reviewed by Drugs.com. Last updated on Nov 20, 2024.
What is macular degeneration?

Macular degeneration is a common cause of vision problems among older people. Macular degeneration is also called age-related macular degeneration, or AMD.
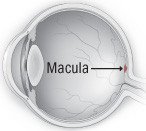
AMD damages the macula. The macula is a part of the eye that is responsible for seeing sharp details directly in the center of the field of vision. Damage caused by AMD can interfere with:
- the ability to see straight ahead: this is necessary for driving and viewing distances, such as when recognizing faces or watching television
- fine, detailed vision: this is necessary for reading newsprint, sewing, working with crafts, and making repairs.
|
|
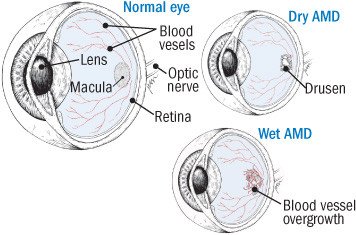
Most people with AMD have fluffy, yellow-white spots on the macula. These spots are called drusen. Not everyone who gets AMD has these spots.
There are two forms of AMD:
- Dry AMD: The vast majority of people who lose significant vision from AMD have dry AMD. In dry AMD, the cells of the macula slowly break down. This produces blurring, then blank spots in the eye's central vision. The symptoms are subtle at first, then become more noticeable over time. A small percentage of people with dry AMD can develop geographic atrophy, which is more likely to result in worsening vision loss.
- Wet AMD: In wet AMD, delicate new blood vessels begin to grow beneath the retina. They leak blood and fluid into the macula, causing scarring. Wet AMD can cause rapid loss of vision over days to weeks and continued loss of vision over time. Wet AMD is much less common than the dry form. But it generally progresses much more rapidly and is therefore more serious.
|
|
Age is the most important risk factor for AMD. Cigarette smoking and cardiovascular risk factors, such as high cholesterol levels, may also increase risk.
Symptoms of macular degeneration
Dry AMD sometimes does not cause any symptoms. Or, it can make central vision a little less clear. In a small number of cases, it gradually causes more significant blurring or loss of vision in the center of the visual field. In these more advanced cases, faces and printed words become hard to recognize.
As a first symptom of wet AMD, straight lines or edges appear crooked. Images become blurred. In some cases this is followed by a central blind spot, as in dry AMD. However, unlike in dry AMD, this vision loss usually develops rapidly.
AMD generally does not affect side vision, even in advanced cases. Most patients can continue to function independently.
People who have AMD may appear as though they see normally. But they may actually have difficulty recognizing friends. This can lead to social difficulties.
Some people with vision loss from AMD experience visual hallucinations — that is, they see things, such as people and patterns, that are not there.
Diagnosing macular degeneration
Your doctor will ask questions about your health history and about any risk factors you may have for AMD. He or she then will test your visual acuity. An eye specialist called an ophthalmologist will dilate your pupils to thoroughly examine your eyes, looking for drusen and other abnormal changes in your retina. The eye doctor may perform additional specialized imaging to confirm the diagnosis.
Expected duration of macular degeneration
AMD is a lifelong illness. However, few people with early AMD develop advanced AMD with vision loss.
Preventing macular degeneration
There is no proven way to prevent AMD.
However, smokers are more likely to develop AMD. Quitting can help prevent the condition. Those who stopped smoking more than 20 years before do not appear to have a higher risk of AMD. Some people with a family history of AMD have an increased risk of developing it and definitely should avoid smoking.
More recent evidence suggests that a diet rich in green leafy vegetables, fruits, fish, and nuts may reduce the risk of AMD.
Drugs used to treat this and similar conditions
Treatment options
The following list of medications are related to or used in the treatment of this condition.
Treating macular degeneration
Treatments can help slow or stop the disease from getting worse. Your treatment options depend on the type of AMD you have.
Dry AMD
For people with intermediate dry AMD, a specific combination of vitamins may slow the disease's progression. They may even prevent it from worsening to advanced AMD. For people with advanced AMD in only one eye, these vitamins may help prevent the other eye from being affected.
The original National Eye Institute's Age-Related Eye Disease Study (AREDS) suggested that the following vitamin formula could reduce the progression of dry AMD:
- 500 milligrams (mg) of vitamin C
- 400 International Units of vitamin E
- 15 mg of beta-carotene (often labeled as equivalent to 25,000 International Units of vitamin A); because beta-carotene has been linked to an increased risk of lung cancer in smokers, lutein (10 mg) and zeaxanthin (2 mg) should be taken instead of beta-carotene in those who smoke
- 80 mg of zinc as zinc oxide
- 2 mg of copper as cupric oxide.
However, concerns about the high level of vitamin A in the formula led to products with alternative ingredients that are safer. Talk with your doctor before starting any kind of AMD-related vitamin regimen. Be sure to mention if you take any other vitamins, including a multivitamin. Even the modified AREDS formulas can contain high doses of certain vitamins to avoid not getting too much of any particular one.
Wet AMD
The most common treatment for wet AMD is anti-VEGF therapy. When injected into the eye, these drugs may stop the growth of new abnormal blood vessels. They also decrease leakage from those vessels. Anti-VEGF therapy may even restore lost vision.
Patients need to get injections regularly for several months to a year, and maybe longer. Possible side effects include:
- eye pain
- irritation
- discharge
- seeing spots or floaters.
Most people don't develop these side effects.
Anti-VEGF treatments are generally painless. The doctor numbs the eye before administering the injection.
Other treatments that can slow or stop the progression of wet AMD include thermal laser surgery and photodynamic therapy. These are used much less frequently than anti-VEGF therapy.
Laser surgery burns the leaky blood vessels to seal them. Unfortunately, the laser treatment can also destroy some surrounding healthy tissue, thereby harming vision.
Both laser surgery and photodynamic therapy can temporarily slow the worsening of wet AMD, but they don't stop or reverse the damage. Both procedures may need to be repeated from time to time. In photodynamic therapy, a light-activated drug called verteporfin (Visudyne) is injected into a vein in your arm. The drug moves through your body and to your eyes. The doctor shines a light into your eyes to activate the drug. The activated drug kills abnormal blood vessels.
For active or sight-threatening disease, other options include injections of bevacizumab, aflibercept, or ranibizumab into the eye with or without laser surgery.
For people with wet AMD, your doctor may recommend a Mediterranean-style diet, although there is no evidence that diet actually helps in prevention or slowing the progression of vision loss.
The treatment of wet AMD is changing quickly. Make sure to seek treatment from a retinal specialist who has kept up to date on this rapidly evolving field.
Low vision aids
Patients who have lost vision because of AMD may be able to use low-vision aids to read or do other tasks.
Low-vision aids include:
- optical devices:
- magnifying spectacles
- handheld magnifiers
- stand magnifiers
- computer monitors with large type
- non-optical devices:
- books and newspapers with large print
- talking computers
- high-contrast watch dials
- enhanced lighting.
When to call a professional
Call your doctor immediately if you notice any change in your vision. This is especially true if the change happens suddenly and interferes with your ability to read newsprint or to recognize people's faces.
If you are at high risk of vision loss from AMD, you may keep a copy of the Amsler grid at home. Check your own vision periodically.
Prognosis
Dry AMD develops slowly. Most people who have it continue to lead relatively normal lives, especially if only one eye is affected.
If you have wet AMD, consult with a skilled retina specialist to see what form of therapy is best for you.
Additional info
National Eye Institute
https://www.nei.nih.gov/
Learn more about Macular degeneration
Treatment options
Care guides
Medicine.com guides (external)
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.