Lyme disease
Medically reviewed by Drugs.com. Last updated on Jun 10, 2025.
What is Lyme disease?

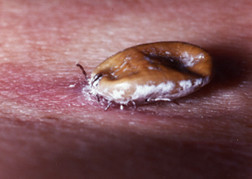
Lyme disease is an infection caused by bacteria called Borrelia burgdorferi. These bacteria are transmitted through the bites of ticks, primarily the deer tick. Not everyone who develops symptoms of Lyme disease remembers getting bitten by a tick because the deer tick is very small and its bite can go unnoticed.
|
|
Lyme disease is most common in the Northeastern, mid-Atlantic, and upper Midwestern United States. About 90% of US cases have been reported in 14 states: Connecticut, Maine, Maryland, Massachusetts, Minnesota, New Hampshire, New Jersey, New York, Pennsylvania, Rhode Island, Vermont, Virginia, West Virginia, and Wisconsin. Even within states, there are regions of high risk and others with very low rates of disease. This variation relates to where ticks that carry the bacteria live, breed, and come into contact with humans.
Late spring and early summer are the peak times of the year for Lyme disease to be diagnosed. However, the condition is not always diagnosed right away. So, cases still are identified all year long.
Deer ticks can carry other germs, such as Anaplasma, Babesia, and Borrelia miyamotoi. It's not uncommon for people to have one of these infections in addition to Lyme disease.
Symptoms of Lyme disease
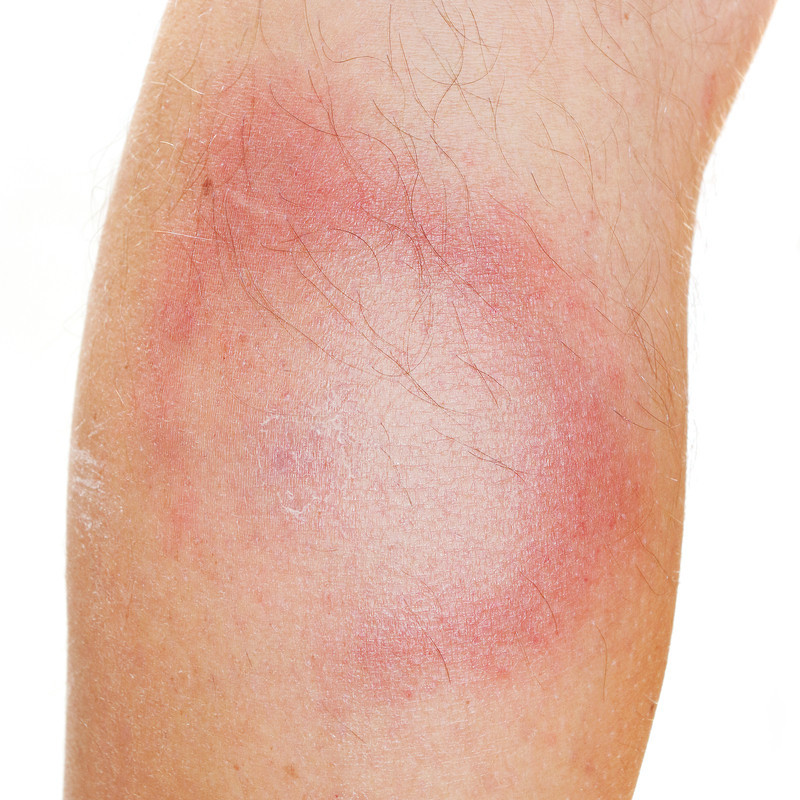
The most common initial symptom is a rash called erythema migrans (EM), which is typically a flat, reddish rash that spreads from the site of the tick bite. The rash is often larger than two inches wide and can grow even larger with a central clear area known as a bull's eye. The rash usually doesn't itch or hurt. In many cases, the rash is less classic (for example, without the central clearing) and in about a third of cases a person with Lyme disease recalls no rash at all.
Other symptoms at this stage can include fever, muscle and joint aches, fatigue, headache, and a stiff neck. In some cases, there are two or more of these well-defined rashes.
|
|
Over several days to weeks after the tick bite, Lyme disease can cause other problems. It can affect the nervous system. For example, it can cause Bell's palsy, a condition in which the nerve that controls most of the facial muscles becomes inflamed and the muscles get weak. The infection can get into the fluid that surrounds the brain and spinal cord, causing a type of meningitis.
Lyme disease also can affect the heart. The most common problem is a very slow heartbeat that leads to fatigue, dizziness, and fainting. The heart muscle can also be inflamed, called myocarditis.
In later stages of Lyme disease, pain and swelling of joints may develop. The arthritis commonly affects one knee, or causes episodes of swelling in several joints, called migratory arthritis. The symptoms can become persistent. Neurologic disease, causing problems with memory and concentration, can also develop as a late manifestation of Lyme disease.
Diagnosing Lyme disease
Your doctor will ask about your symptoms and perform a complete physical and neurological examination. If you have had a recent tick bite and have saved the tick, your doctor may want to inspect the insect and send it to a laboratory to identify the species. Some laboratories can analyze the tick to see if it's carrying Lyme bacteria.
Your doctor will diagnose Lyme disease based on your symptoms, physical examination, and, in many cases, blood tests. However, blood tests are often negative in the first few weeks of Lyme disease. The basic Lyme test is called an ELISA (enzyme-linked immunosorbent assay). It is far from perfect: besides being negative in early disease, it may be positive in someone who doesn't have the illness (a false-positive result). Therefore, every positive or uncertain Lyme ELISA result needs to be confirmed with a test called a Western blot, which looks for more specific evidence of Lyme disease infection.
A positive Lyme blood test, even including a Western blot, doesn't mean that the disease is active and needs to be treated. This is because blood tests can remain positive for years, even after Lyme disease has been treated or has become inactive. To help diagnose Lyme disease and to check for other causes of symptoms, a sample of fluid may be withdrawn from an affected joint using a sterile needle. Cerebrospinal fluid also may be taken from around the spinal cord through a spinal tap (lumbar puncture), to test for Lyme disease antibodies and inflammation and check for other diseases.
Expected duration of Lyme disease
People often recover within two to six weeks without antibiotics. Even Lyme arthritis can improve on its own as the body's immune system attacks the infection, although it's common for the joint symptoms to return. Antibiotic therapy is highly effective at curing the illness. Significant improvement typically occurs within two to six weeks after beginning therapy.
Preventing Lyme disease
If you are in a region where Lyme disease is more common, you can:
- avoid woods, high brush, and grasses where ticks hide
- wear long pants and long sleeves; white clothing makes it easier to spot ticks
- examine your skin for ticks soon after returning from wooded areas or areas with high grass or brush
- apply tick repellents (especially those that contain DEET) to the skin and clothing.
Antibiotics are not prescribed for every tick bite because the risk of getting Lyme disease is quite low, ranging from less than 0.1% in most areas to 5% in some areas of the Northeast and Midwest. In addition, risk is lower if the tick has been attached for less than 36 hours. If a tick is engorged, it’s more likely to have been attached long enough to transmit Lyme disease.
A single dose of doxycycline can usually prevent disease if taken within three days of a tick bite. So for those at highest risk, early antibiotic treatment may be appropriate. A Lyme disease vaccine is not currently available for humans.
Drugs used to treat this and similar conditions
Treatment options
The following list of medications are related to or used in the treatment of this condition.
Treating Lyme disease
For the early Lyme EM rash, doctors usually prescribe oral antibiotics for 10 to 14 days. Doxycycline is the preferred treatment. Alternative antibiotics include amoxicillin, azithromycin, and cefuroxime (Ceftin, others). Similar treatment is usually recommended for people who have developed neurologic disease (such as Bell's palsy), arthritis, or carditis, although sometimes antibiotic treatment will be extended to three weeks.
Some people with heart or neurological problems will be treated with antibiotics such as ceftriaxone (Rocephin) given intravenously (into a vein) for two to four weeks. Intravenous treatment also may be recommended if a person with Lyme arthritis does not respond to oral antibiotics. Doxycycline should be avoided in children under 8 years old and for women who are pregnant or nursing. Azithromycin or clarithromycin may be less effective, but are often prescribed for people with Lyme disease who are allergic to doxycycline or can't tolerate the other options mentioned above.
Some people with heart inflammation due to Lyme disease require a temporary pacemaker; however, because antibiotic treatment is usually effective, a permanent pacemaker is rarely needed.
When to call a professional
Call your doctor if you develop a rash or flulike illness after you have been bitten by a tick, or if you could have been exposed to ticks. You should also call your doctor if you have facial paralysis, arthritis, or persistent dizziness or heart palpitations.
If you are taking oral antibiotics for Lyme disease and your symptoms do not improve within two to three weeks, call your doctor.
Prognosis
People with the Lyme disease rash rarely have problems after they are treated with antibiotics. In some cases, people become extremely tired after being treated for Lyme disease, but this problem doesn't tend to improve with additional antibiotics. The medical reason for this fatigue is uncertain. Many (and perhaps most) people with persistent symptoms have no clear evidence of active infection. Intensive antibiotic treatment (for example, intravenous treatment for prolonged periods) usually doesn't help.
Up to 10% of people with Lyme arthritis appear to have chronic (long-lasting) joint swelling despite taking antibiotics. This may be due to an autoimmune effect, in which Lyme infection triggers the immune system to attack the body's own cells. This problem seems to follow Lyme disease primarily in people of certain genetic types. These people may respond to medications that suppress the immune system (similar to those used in rheumatoid arthritis) rather than to continued antibiotics.
Additional info
Infectious Diseases Society of America
https://www.idsociety.org/
Centers for Disease Control and Prevention (CDC)
https://www.cdc.gov/
Learn more about Lyme disease
Treatment options
Care guides
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.