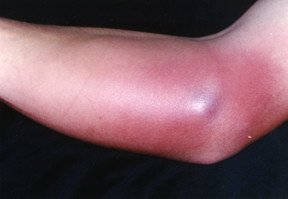
Cellulitis
Medically reviewed by Drugs.com. Last updated on May 21, 2024.
What is cellulitis?

Cellulitis is a serious bacterial infection of the skin. Bacteria break through the skin's protective outer layer, typically at the site of an injury, such as a cut, puncture, sore, burn or bite. Cellulitis can occur at the site of surgery, or where there is a catheter. Once beneath the skin surface, bacteria multiply and make chemicals that cause inflammation in the skin.
Cellulitis that is not caused by a wound or catheter most often occurs on the legs and feet. However, it can develop on any part of the body, including the trunk, arms and face. It often develops where there is edema (swelling), poor blood flow, or a skin rash that creates breaks in the skin, such as a fungus infection between the toes (athlete's foot).
Many types of bacteria can cause cellulitis. Most cases are caused by Streptococcus pyogenes (strep) or Staphylococcus aureus (staph). A strain of staph known as community-acquired methicillin-resistant staphylococcal aureus, or "community-acquired MRSA" can lead to blistering of the skin and a deeper, more serious infection.
Less common bacteria varieties can cause infection after animal bites, puncture wounds through wet shoes, or wounds exposed to freshwater lakes, aquariums, or swimming pools. When cellulitis is located around an eye socket, it is named periorbital cellulites. Because infection around the eye can spread to the brain if it is not quickly treated with antibiotics, periorbital cellulitis requires prompt medical attention.
Medical conditions that are closely related to cellulitis include:
- Erysipelas, a skin infection that causes raised, firm, bright red patches of skin — Usually, it is caused by Streptococcus bacteria. Erysipelas occurs most often on an arm or leg that has been damaged by previous surgery or is chronically swollen due to poor lymph flow (lymphedema). Erysipelas also can develop on the face, typically across the bridge of the nose and upper cheeks.
- Necrotizing fasciitis, also known as "flesh-eating strep" — This is an infection of the tissues below the skin, rather than the skin itself. Often, the skin in the area is discolored and extremely painful. Fasciitis is a life-threatening infection that requires prompt medical attention.
Symptoms of cellulitis
In cellulitis, the affected skin feels warm and is usually red, swollen and painful. The redness can be slight or can stand out compared to surrounding skin. The area of warmth can be felt with the back of the hand, especially when compared to surrounding skin. There may be a spreading network of red streaks in the skin, caused by infection in the vessels that carry lymph (tissue fluid), as well as enlarged lymph nodes (swollen glands) near the area of infection.
|
|
Fever and a general sick feeling (malaise) often accompany cellulitis. Severe infections can cause low blood pressure if bacteria get into the bloodstream. Bloodstream infections (blood poisoning) from cellulitis are particularly dangerous in the very young and very old, as well as in those with weakened immune systems or abnormal heart valves.
Diagnosing cellulitis
Many people who develop cellulitis have no other medical problems and no obvious injury or skin damage that allowed the infection to occur.
Your doctor can usually diagnose cellulitis based on your recent medical history, your symptoms and a physical examination. Your doctor may recommend tests to look for other conditions that may mimic cellulitis. For example, an ultrasound of the veins in your leg can help detect a blood clot. X-rays can help to determine whether the skin infection has spread to the bone.
In most cases, your doctor is not able to specifically tell you what bacteria type has caused your infection. Studies have shown that culture of the skin is not useful. An antibiotic can be chosen that kills most bacteria types that are causes of cellulitis. Your treatment can be adjusted if you are not improving.
Expected duration of cellulitis
How long cellulitis lasts depends on the extent of the cellulitis, the bacteria that caused the infection and your general health. Without proper antibiotic treatment, some forms of cellulitis can cause serious complications within a few days, even in otherwise healthy people.
Preventing cellulitis
To help prevent cellulitis:
- Prevent skin injury — Wear protective gloves while gardening and working outdoors. Wear long sleeves and trousers while hiking. Avoid going barefoot outdoors. Wear protective padding on elbows and knees while skating.
- Treat minor skin wounds promptly — Gently wipe away dirt, wash with antibiotic soap, apply antibiotic ointment and cover with a clean bandage.
- Seek medical attention — Medical attention is needed for all deep puncture wounds and animal bites and for all deep wounds involving a joint, hand or foot.
Drugs used to treat this and similar conditions
Treatment options
The following list of medications are related to or used in the treatment of this condition.
Treating cellulitis
Cellulitis is treated with antibiotics. Your doctor will choose a specific antibiotic depending on the site of your cellulitis and the likely cause of your infection. Most cases of cellulitis improve quickly once you start taking antibiotics.
If you have mild cellulitis, you can usually treat it at home with antibiotics taken by mouth. However, keep in touch with your doctor to be sure that the infection is improving as expected. At home, warm compresses, such as a warm, moist washcloth, and elevating the infected area can help.
If you have severe cellulitis, you may need to be treated in the hospital with antibiotics given intravenously (into a vein).
Community-acquired MRSA infections may worsen despite antibiotic treatment, because the antibiotics that are most commonly selected to treat cellulitis do not reliably kill this bacteria. If within the first two or three days of treatment you don't have obvious improvement in your skin pain, redness, and swelling, or if you develop blisters or pus on the surface of your skin rash, contact your doctor immediately. These can be signs of community-acquired MRSA infection.
When to call a professional
Call your doctor whenever a skin injury becomes red, warm, swollen or tender. Call your doctor promptly if you get a deep puncture wound, especially on a hand or foot, or if you are bitten by an animal or human.
Prognosis
In most cases, symptoms of cellulitis begin to improve within 24 to 48 hours after starting treatment with appropriate antibiotics. Always take all the antibiotics prescribed by your doctor, even if you think your infection has been cured. The prognosis is generally good, but the condition can return, especially in people with poor circulation, chronic (long-term) swelling in the legs or skin that is in poor condition.
Additional Info
Centers for Disease Control and Prevention
https://www.cdc.gov/
Learn more about Cellulitis
- Can You Drink Alcohol with Antibiotics?
- Common Side Effects from Antibiotics, and Allergies and Reactions
Treatment options
Care guides
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.