Peripheral Vascular Disease
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is peripheral vascular disease (PVD)?
PVD is a condition that causes decreased blood flow to your limbs because of blocked blood vessels. The blockage is usually caused by material such as cholesterol or a blood clot that sticks to the blood vessels and makes them narrow.
What increases my risk for PVD?
- Older age
- Smoking cigarettes
- Obesity or a lack of activity or exercise
- A medical condition, such as high blood pressure, high cholesterol, or diabetes
- History of a blood clot, kidney disease, or heart failure
- A family history of peripheral artery disease, heart disease, or stroke
What are the signs and symptoms of PVD?
- Painful cramps in your hip, thigh, or calf muscles, especially after you walk or climb stairs
- Burning pain in your hands, fingers, feet, or toes
- Shiny, tight, cold skin, and uneven hair growth on your skin
- A change in your skin color
- Sores on your skin that do not heal
- Weakness or numbness in your hands or feet
How is PVD diagnosed?
Your healthcare provider will ask about your symptoms and examine you. You may need any of the following tests:
- Blood or urine tests may be used to get information about how your body is working.
- An ankle brachial index compares the blood pressure in your arms to the blood pressure in your legs. A lower blood pressure in your legs may mean you have blocked blood vessels.
- Doppler ultrasound pictures may show narrow or blocked blood vessels.
- Angiography, CT, or MRI pictures may show blood flow and blockage. You may be given contrast liquid to help any problems show up better in the pictures. Tell the healthcare provider if you have ever had an allergic reaction to contrast liquid. Do not enter the MRI room with anything metal. Metal can cause serious injury. Tell the provider if you have any metal in or on your body.
How is PVD treated?
- Medicines may be given to help decrease your cholesterol level, open blood vessels, or prevent blood clots.
- Procedures may be used to open blocked blood vessels. Metal or plastic stents (tubes) may be put in where the artery was blocked to keep it open. Surgery may be used to place a new blood vessel near the blocked vessel. Surgery may be used to replace the area of the blood vessel.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
How can I manage PVD?
- Do not smoke. Nicotine and other chemicals in cigarettes and cigars can damage your blood vessels. Ask your healthcare provider for information if you currently smoke and need help to quit. E-cigarettes or smokeless tobacco still contain nicotine. Talk to your healthcare provider before you use these products.
- Exercise as directed. Your healthcare provider can help you create a safe exercise plan. He or she may recommend walking. Walking is a low-impact way to exercise and increase your blood flow. Stop and rest if you have pain in your legs.

- Care for your feet. Look closely at your feet every day. Check for cracks or sores. Wash your feet daily with mild soap and dry them well. Do not walk barefoot in case you step on a hard or sharp object.
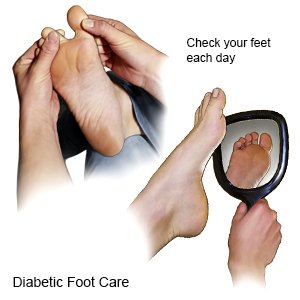
- Change your sleep position. You may have pain in your legs or feet when you sleep. Raise the head of your bed 4 inches, or use pillows to prop your upper body higher than your legs. This may help more blood go to your feet, decreasing pain.
- Protect and cushion your feet and hands. If you have ulcers on your feet, you may need to wear bandages with heel pads. You may also wear foam rubber booties. Hand or foot warmers may decrease pain in your hands or feet.
How can I prevent PVD?
- Eat a variety of healthy foods. Healthy foods include fruits, vegetables, whole-grain breads, low-fat dairy products, beans, lean meats, and fish. Ask if you need to be on a special diet.
- Maintain a healthy weight. Ask your healthcare provider what a healthy weight is for you. Ask him or her to help you create a weight loss plan if you are overweight.
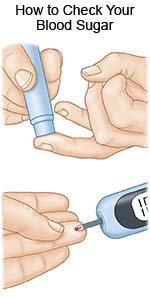
- Manage diabetes. Keep your blood sugar level in the range recommended by your healthcare provider. Check your blood sugar level as often as directed. Ask your provider if you should make nutrition, exercise, or medicine changes.
Related medications
Call your local emergency number (911 in the US) for any of the following:
- You have any of the following signs of a heart attack:
- Squeezing, pressure, or pain in your chest
- You may also have any of the following:
- Discomfort or pain in your back, neck, jaw, stomach, or arm
- Shortness of breath
- Nausea or vomiting
- Lightheadedness or a sudden cold sweat
- You have any of the following signs of a stroke:
- Numbness or drooping on one side of your face
- Weakness in an arm or leg
- Confusion or difficulty speaking
- Dizziness, a severe headache, or vision loss
When should I seek immediate care?
- Your arm or leg feels warm, tender, and painful. It may look swollen and red.
- You have leg pain that does not go away with rest.
- You have dark areas on the skin of your legs.
- You cannot see out of one or both eyes.
When should I call my doctor?
- Your signs and symptoms get worse or do not get better, even after treatment.
- You have a sore or ulcer that is not healing or gets worse.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Peripheral Vascular Disease
Treatment options
- Medications for Peripheral Arterial Disease
- Medications for Renal Artery Atherosclerosis
- Medications for Thromboangiitis Obliterans
Care guides
Symptoms and treatments
Medicine.com guides (external)
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
