Perineal Prostatectomy
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What do I need to know about perineal prostatectomy?
A perineal prostatectomy is surgery to remove your prostate gland.
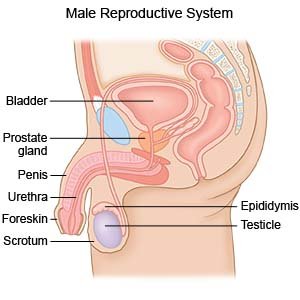 |
How do I prepare for surgery?
Your surgeon will talk to you about how to prepare for surgery. You will need to be on a clear liquid diet the day before your surgery. He or she may also tell you not to eat or drink anything after midnight on the day of your surgery. He or she will tell you what medicines to take or not take on the day of your surgery.
Related medications
What will happen during surgery?
Your surgeon will make an incision between your scrotum and anus. He or she will move layers of skin, tissue, and muscle to get to your prostate. Your surgeon will cut your prostate gland away from your urethra (tube that drains urine from your bladder). He or she will reattach your bladder to your urethra and place a Foley catheter to drain urine. Your surgeon may make another incision in your abdomen and remove lymph nodes. Your incisions will be closed with stitches and covered with a bandage. Your prostate gland will be sent to a lab for testing.
What are the risks of surgery?
Surgery may increase your risk for bleeding or an infection. Nerves, organs, or tissues near your prostate may be injured during surgery. After surgery, you may leak urine and bowel movements. Urine leakage may be short-term or permanent. You may have trouble having an erection or ejaculating. You may get a blood clot in your leg. This may become life-threatening.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
