Orchiectomy
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
Orchiectomy, also called orchidectomy, is surgery to remove one or both of your testicles.
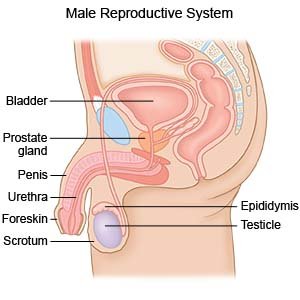 |
DISCHARGE INSTRUCTIONS:
Call your local emergency number (911 in the US) if:
- You feel lightheaded and short of breath.
- You have chest pain when you take a deep breath or cough.
- You cough up blood.
Seek care immediately if:
- You have severe pain or swelling in your legs.
- You have lower abdominal or back pain that does not go away, even after you take pain medicine.
- You have trouble urinating or having a bowel movement.
- Your incision is swollen, red, bleeding, or has pus coming from it.
- Your stitches come apart.
- Your leg feels warm, tender, and painful. It may look swollen and red.
Related medications
Call your doctor or surgeon if:
- You have nausea or are vomiting.
- You have a cough or feel weak and achy.
- You have a fever or chills.
- You have questions or concerns about your condition or care.
Medicines:
You may need any of the following:
- Antibiotics help prevent or treat a bacterial infection.
- Antihormone medicine may be given if your testosterone level does not decrease enough after your surgery.
- Bone strengthening medicines help decrease bone loss and reduce your risk of broken bones. These may include bisphosphonates, calcium, and vitamin D supplements.
- Prescription pain medicine may be given. Ask your healthcare provider how to take this medicine safely. Some prescription pain medicines contain acetaminophen. Do not take other medicines that contain acetaminophen without talking to your healthcare provider. Too much acetaminophen may cause liver damage. Prescription pain medicine may cause constipation. Ask your healthcare provider how to prevent or treat constipation.
- Take your medicine as directed. Contact your healthcare provider if you think your medicine is not helping or if you have side effects. Tell your provider if you are allergic to any medicine. Keep a list of the medicines, vitamins, and herbs you take. Include the amounts, and when and why you take them. Bring the list or the pill bottles to follow-up visits. Carry your medicine list with you in case of an emergency.
Care for the surgery area:
- You will have a bandage over your surgery site. Do not take the bandage off until your healthcare provider says it is okay.
- You may need to wear a jock strap for support and comfort. Ask for more information about caring for your wound and using your jock strap.
- Apply ice to your surgery area. Ice helps decrease swelling and pain. Ice may also help prevent tissue damage. Use an ice pack or put crushed ice in a plastic bag. Cover it with a towel, and place it on your incision for 15 to 20 minutes every hour as directed.
Follow up with your doctor or surgeon as directed:
You may need x-ray scans and blood tests after your surgery. Write down your questions so you remember to ask them during your visits.
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
