Laparoscopic Colostomy Reversal
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What do I need to know about laparoscopic colostomy reversal?
Laparoscopic colostomy reversal is surgery to remove your stoma and reconnect your colon. It is also called a colostomy takedown.
What will happen before my surgery?
- You may need tests to help your surgeon find any problems with your intestines. The tests may include a barium enema.
- Your surgeon may tell you to only eat and drink clear liquids for 2 days before your surgery. This helps to begin cleaning out your intestines for surgery.
- You may need to be admitted to the hospital the night before your surgery. Healthcare providers may give you medicine or an enema to make sure your intestines are empty.
- If you are not admitted, you will be told not to eat or drink anything after midnight the night before your surgery. Tell your surgeon about all your current medicines. He or she will tell you if you need to stop any medicine for surgery, and when to stop. He or she will tell you which medicines to take or not take the day of your surgery.
Related medications
What will happen during my surgery?
- You will be given general anesthesia to keep you asleep and pain-free during your surgery. You will be given antibiotics before your surgery to prevent an infection. You may also be given antibiotics during and after your surgery.
- Your surgeon will make several small incisions to place the scope and small tools through to complete the surgery. Your surgeon will cut your stoma away from your abdomen. He or she may need to use a gas to move other organs out of the way. Your surgeon will sew or staple the ends of your colon together, then check for leaks.
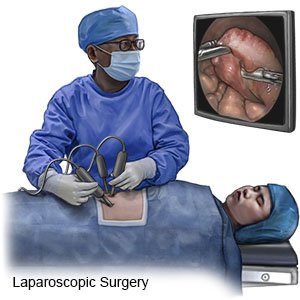
- The openings in your abdomen will be sewn or stapled shut. Your surgeon may need to leave part of the area open to allow it to heal from the inside out. A bandage will be placed over the area. Steristrips will be placed over the incisions.
What should I expect after my surgery?
- You will be monitored until you are fully awake, then taken to your hospital room.
- You will not be able to eat or drink until you pass gas or have a bowel movement.
- You may need a tube placed in your nose and guided to your stomach if you vomit and have nausea. The tube will remove anything in your stomach. It is removed after your bowels start working.
- Healthcare providers will help you get up and walk after surgery. When you walk, it helps prevent blood clots and also helps your bowels to start working.
What are the risks of a laparoscopic colostomy reversal?
You may bleed more than expected during or after your surgery. You may have problems that require open surgery. Your surgeon may not be able to reconnect your colon. If this happens, you will need to keep your colostomy. Your colon may leak or pull apart around the area where it was put back together. This can cause a serious infection that can become life-threatening. You may develop a blood clot in your leg or arm. The blood clot can break loose and travel to your brain or lungs. This can be life-threatening.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
