Cervical Cone Biopsy
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
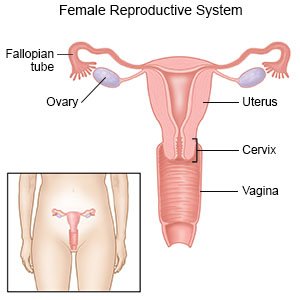
A cervical cone biopsy is surgery to take cells from your cervix. Surgery may be done so cells can be tested for cancer or can be removed before they become cancer.
 |
DISCHARGE INSTRUCTIONS:
Call your surgeon or gynecologist if:
- You have white or yellow vaginal discharge.
- You have more vaginal bleeding than you were told to expect.
- You have a fever.
- You have new or increased pain in your lower abdomen and pelvic area.
- You have vaginal bleeding, and it is not time for your monthly period.
- You feel pain when you urinate, or your urine looks cloudy.
- You have questions or concerns about your condition or care.
Related medications
Medicines:
You may need any of the following:
- Prescription pain medicine may be given. Ask your healthcare provider how to take this medicine safely. Some prescription pain medicines contain acetaminophen. Do not take other medicines that contain acetaminophen without talking to your healthcare provider. Too much acetaminophen may cause liver damage. Prescription pain medicine may cause constipation. Ask your healthcare provider how to prevent or treat constipation.
- Antibiotics prevent or fight an infection caused by bacteria.
- Take your medicine as directed. Contact your healthcare provider if you think your medicine is not helping or if you have side effects. Tell your provider if you are allergic to any medicine. Keep a list of the medicines, vitamins, and herbs you take. Include the amounts, and when and why you take them. Bring the list or the pill bottles to follow-up visits. Carry your medicine list with you in case of an emergency.
Self-care:
- Care for the surgery area as directed. Do not use tampons or have sex for 2 to 3 weeks after your surgery. Do not douche during this time.
- Ask about vaccines. Ask your healthcare provider or gynecologist for more information about the vaccine for human papillomavirus (HPV). The HPV vaccine may help decrease your risk for an HPV infection and abnormal cervical cells. A condom can help prevent the spread of HPV during sex. Ask your healthcare provider for more information on ways to prevent HPV infection.
- Talk to your providers about pregnancy. You may have trouble becoming pregnant after a cervical cone biopsy. If you do become pregnant, your baby may need to be delivered early. You may need more care during a future pregnancy to help prevent problems.
- Do not smoke. Smoking increases the risk of abnormal cells in your cervix. Ask for information if you need help quitting. Do not use E-cigarettes or smokeless tobacco in place of cigarettes or to help you quit. These still contain nicotine.
Follow up with your surgeon or gynecologist as directed:
You may need to return to make sure your cervix is healing. Write down your questions so you remember to ask them during your visits.
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
