Cardiac Resynchronization Therapy
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
WHAT YOU NEED TO KNOW:
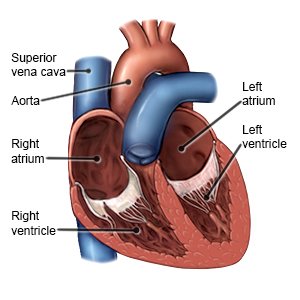
Cardiac resynchronization therapy (CRT) is a procedure used to treat problems with how your heart beats. CRT is also called biventricular pacing. The 2 upper chambers of the heart are called atria. The 2 lower chambers are called ventricles. Your heartbeat is synchronized when all areas of your heart beat together properly. When the areas of your heart do not beat as they should, your heart cannot pump enough blood and oxygen to your body. You may have trouble breathing, tire easily, and have swelling in your legs and feet.
 |
HOW TO PREPARE:
Before your procedure:
- Tell your healthcare provider about all medicines you currently take. Include prescription and non-prescription medicines, vitamins, and supplements. Your provider will tell you if you need to stop taking any medicine before your procedure, and when to stop.
- Tell your provider about any allergies you have. An anesthesiologist will talk to you about anesthesia to keep you asleep during the procedure. Tell him or her if you or anyone in your family has had a problem with anesthesia.
- You may need blood tests before your procedure. You may need tests to check your heart function. A vein x-ray may also be done to help your healthcare provider plan your procedure.
- Your provider will tell you how to prepare for your procedure. He or she will tell you which medicines to take or not take on the day of your procedure.
The night before your procedure:
You may be told not to eat or drink anything after midnight.
The day of your procedure:
- You or a close family member will be asked to sign a legal document called a consent form. It gives healthcare providers permission to do the procedure or surgery. It also explains the problems that may happen, and your choices. Make sure all your questions are answered before you sign this form.
- Take only the medicines your healthcare provider told you to take.
- Healthcare providers may put an IV into your vein. You may be given liquids or medicine through the IV.
WHAT WILL HAPPEN:
What will happen:
- A small incision will be made over a vein near your neck. An x-ray may be used to help guide your healthcare provider during the procedure. An electrode catheter holding 3 leads will be inserted through the incision. The catheter and leads are guided into your heart. The catheter records the activity of your heart to help your provider decide where to place the leads.
- If any of the leads cannot be placed through your vein, they may be placed through your chest. Your provider will make 3 or 4 small cuts on your left side, between your ribs. The leads will be placed directly on your heart. After the leads are placed, a pacemaker will be secured under the skin on your chest. The pacemaker will help your heart beat correctly. Your incisions will be closed with stitches or medical glue.
After your procedure:
You will be taken to a room to rest until you are fully awake. Healthcare providers will monitor you closely for any problems. Do not get out of bed until your healthcare provider says it is okay. You will then be taken to your hospital room.
CONTACT YOUR HEALTHCARE PROVIDER IF:
- You have a fever.
- You get a cold or the flu.
- You have questions or concerns about your procedure.
Risks
- You may need a large chest incision if the leads cannot be placed through your vein or small cuts. The activity of the pacemaker may make it hard for you to breathe at times. Your heart, blood vessels, and the area around them may be damaged. You may have abnormal heartbeats, and your heart may stop beating. Blood may collect around your heart, making it hard for your heart to beat. This can be life-threatening.
- You may get an infection around the pacemaker implant. The leads in your heart may move out of place. The leads may not be in the right position to synchronize your heartbeats. The pacemaker may not work properly.
Related medications
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
