Triumeq: Package Insert / Prescribing Info
Package insert / product label
Generic name: abacavir sulfate, dolutegravir sodium, lamivudine
Dosage form: tablet, film coated
Drug class: Antiviral combinations
Medically reviewed by Drugs.com. Last updated on Jul 12, 2024.
On This Page
- Indications and Usage
- Dosage and Administration
- Dosage Forms and Strengths
- Contraindications
- Warnings and Precautions
- Adverse Reactions/Side Effects
- Drug Interactions
- Use In Specific Populations
- Overdosage
- Description
- Clinical Pharmacology
- Nonclinical Toxicology
- Clinical Studies
- How Supplied/Storage and Handling
- Patient Counseling Information
- Medication Guide
Highlights of Prescribing Information
TRIUMEQ (abacavir, dolutegravir, and lamivudine) tablets, for oral use
TRIUMEQ PD (abacavir, dolutegravir, and lamivudine) tablets for oral suspension
Initial U.S. Approval: 2014
WARNING: HYPERSENSITIVITY REACTIONS, AND EXACERBATIONS OF HEPATITIS B
See full prescribing information for complete boxed warning.
Hypersensitivity Reactions
- •
- Serious and sometimes fatal hypersensitivity reactions have occurred with abacavir-containing products. (5.1)
- •
- Hypersensitivity to abacavir is a multi-organ clinical syndrome. (5.1)
- •
- Patients who carry the HLA‑B*5701 allele are at a higher risk of experiencing a hypersensitivity reaction to abacavir. (5.1)
- •
- TRIUMEQ and TRIUMEQ PD are contraindicated in patients with a prior hypersensitivity reaction to abacavir and in HLA-B*5701-positive patients. (4)
- •
- Discontinue TRIUMEQ or TRIUMEQ PD as soon as a hypersensitivity reaction is suspected. Regardless of HLA-B*5701 status, permanently discontinue TRIUMEQ or TRIUMEQ PD if hypersensitivity cannot be ruled out, even when other diagnoses are possible. (5.1)
- •
- Following a hypersensitivity reaction to TRIUMEQ or TRIUMEQ PD, NEVER restart TRIUMEQ, TRIUMEQ PD, or any other abacavir‑containing product. (5.1)
Exacerbations of Hepatitis B
- •
- All patients with HIV-1 should be tested for the presence of hepatitis B virus (HBV) prior to or when initiating TRIUMEQ or TRIUMEQ PD. Emergence of lamivudine-resistant HBV variants associated with lamivudine-containing antiretroviral regimens has been reported. If TRIUMEQ or TRIUMEQ PD is used in patients co-infected with HIV-1 and HBV, additional treatment should be considered for appropriate treatment of chronic HBV; otherwise, consider an alternative regimen.
- •
- Severe acute exacerbations of HBV have been reported in patients who are co-infected with HBV and HIV‑1 and have discontinued lamivudine, a component of TRIUMEQ and TRIUMEQ PD. Closely monitor hepatic function in these patients and, if appropriate, initiate anti-HBV treatment. (5.2)
Recent Major Changes
Indications and Usage for Triumeq
TRIUMEQ and TRIUMEQ PD are a combination of dolutegravir (integrase strand transfer inhibitor [INSTI]), abacavir, and lamivudine (both nucleoside analogue reverse transcriptase inhibitors) indicated for the treatment of HIV-1 infection in adults and in pediatric patients aged at least 3 months and weighing at least 6 kg. (1)
Limitations of Use:
TRIUMEQ and TRIUMEQ PD alone are not recommended in patients with resistance-associated integrase substitutions or clinically suspected INSTI resistance because the dose of dolutegravir in TRIUMEQ and TRIUMEQ PD is insufficient in these subpopulations. See the dolutegravir prescribing information. (1)
Triumeq Dosage and Administration
- •
- Before initiating TRIUMEQ or TRIUMEQ PD, screen for the HLA‑B*5701 allele because TRIUMEQ and TRIUMEQ PD contain abacavir. (2.1).
- •
- Prior to or when initiating TRIUMEQ or TRIUMEQ PD, test patients for HBV infection. (2.2)
- •
- TRIUMEQ and TRIUMEQ PD may be taken with or without food. (2.4, 2.5)
- •
- Adults: One tablet of TRIUMEQ daily. (2.4)
| ABC = abacavir, DTG = dolutegravir, 3TC = lamivudine. | ||
|
Pediatric Population Body Weight |
Number of Tablets (once daily) |
Recommended Daily Dose |
|
TRIUMEQ PD Tablets (6 kg to <25 kg) |
||
|
6 kg to <10 kg |
3 |
180 mg ABC, 15 mg DTG, and 90 mg 3TC |
|
10 kg to <14 kg |
4 |
240 mg ABC, 20 mg DTG, and 120 mg 3TC |
|
14 kg to <20 kg |
5 |
300 mg ABC, 25 mg DTG, and 150 mg 3TC |
|
20 kg to <25 kg |
6 |
360 mg ABC, 30 mg DTG, and 180 mg 3TC |
|
TRIUMEQ Tablets (≥25 kg) |
||
|
≥25 kg |
1 |
600 mg ABC, 50 mg DTG, and 300 mg 3TC |
- •
- Do not substitute TRIUMEQ and TRIUMEQ PD on a milligram-per-milligram basis. (2.3)
- •
- If dosing with certain UGT1A or CYP3A inducers, then the recommended dolutegravir dosage regimen should be adjusted. See Table 2 for complete dosing recommendations. (2.6)
- •
- Because TRIUMEQ and TRIUMEQ PD are fixed-dose tablets and cannot be dose adjusted, TRIUMEQ and TRIUMEQ PD are not recommended in patients with creatinine clearance <30 mL/min and pediatric patients with a similar degree of renal impairment based on age-appropriate assessment of renal function, or patients with hepatic impairment. (2.7, 4)
Dosage Forms and Strengths
Contraindications
Warnings and Precautions
- •
- Hepatotoxicity has been reported in patients receiving a dolutegravir-containing regimen. Monitoring for hepatotoxicity is recommended. (5.3)
- •
- Lactic acidosis and severe hepatomegaly with steatosis, including fatal cases, have been reported with the use of nucleoside analogues. (5.4)
- •
- Immune reconstitution syndrome has been reported in patients treated with combination antiretroviral therapy. (5.6)
- •
- TRIUMEQ tablets and TRIUMEQ PD tablets for oral suspension are not substitutable. (2.3, 5.7)
Adverse Reactions/Side Effects
The most commonly reported adverse reactions of at least moderate intensity and incidence at least 2% (in those receiving TRIUMEQ) were insomnia, headache, and fatigue. (6.1)
To report SUSPECTED ADVERSE REACTIONS, contact ViiV Healthcare at 1-877-844-8872 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
Drug Interactions
Use In Specific Populations
- •
- Pediatrics: Not recommended for patients aged <3 months or weighing <6 kg. (8.4)
- •
- TRIUMEQ and TRIUMEQ PD are not recommended in patients with creatinine clearance less than 30 mL/min and pediatric patients with a similar degree of renal impairment based on age-appropriate assessment of renal function. (8.6)
- •
- If a dose reduction of abacavir, a component of TRIUMEQ and TRIUMEQ PD, is required for patients with mild hepatic impairment, then the individual components should be used. (8.7)
See 17 for PATIENT COUNSELING INFORMATION and Medication Guide.
Revised: 7/2024
Full Prescribing Information
WARNING: HYPERSENSITIVITY REACTIONS, AND EXACERBATIONS OF HEPATITIS B
Hypersensitivity Reactions
Serious and sometimes fatal hypersensitivity reactions, with multiple organ involvement, have occurred with abacavir, a component of TRIUMEQ and TRIUMEQ PD (abacavir, dolutegravir, and lamivudine). Patients who carry the HLA‑B*5701 allele are at a higher risk of a hypersensitivity reaction to abacavir, although hypersensitivity reactions have occurred in patients who do not carry the HLA‑B*5701 allele [see Warnings and Precautions (5.1)].
TRIUMEQ and TRIUMEQ PD are contraindicated in patients with a prior hypersensitivity reaction to abacavir and in HLA‑B*5701-positive patients [see Contraindications (4), Warnings and Precautions (5.1)]. All patients should be screened for the HLA‑B*5701 allele prior to initiating therapy with TRIUMEQ or TRIUMEQ PD or reinitiation of therapy with TRIUMEQ or TRIUMEQ PD, unless patients have a previously documented HLA‑B*5701 allele assessment. Discontinue TRIUMEQ or TRIUMEQ PD immediately if a hypersensitivity reaction is suspected, regardless of HLA‑B*5701 status and even when other diagnoses are possible [see Contraindications (4), Warnings and Precautions (5.1)].
Following a hypersensitivity reaction to TRIUMEQ or TRIUMEQ PD, NEVER restart TRIUMEQ or TRIUMEQ PD or any other abacavir‑containing product because more severe symptoms, including death can occur within hours. Similar severe reactions have also occurred rarely following the reintroduction of abacavir-containing products in patients who have no history of abacavir hypersensitivity [see Warnings and Precautions (5.1)].
Exacerbations of Hepatitis B
All patients with HIV-1 should be tested for the presence of hepatitis B virus (HBV) prior to or when initiating TRIUMEQ or TRIUMEQ PD. Emergence of lamivudine-resistant HBV variants associated with lamivudine-containing antiretroviral regimens has been reported. If TRIUMEQ or TRIUMEQ PD is used in patients co-infected with HIV-1 and HBV, additional treatment should be considered for appropriate treatment of chronic HBV; otherwise, consider an alternative regimen.
Severe acute exacerbations of hepatitis B have been reported in patients who are co‑infected with HBV and HIV-1 and have discontinued lamivudine, a component of TRIUMEQ and TRIUMEQ PD. Closely monitor hepatic function in these patients and, if appropriate, initiate anti-HBV treatment [see Warnings and Precautions (5.2)].
1. Indications and Usage for Triumeq
TRIUMEQ and TRIUMEQ PD are indicated for the treatment of HIV-1 infection in adults and in pediatric patients aged at least 3 months and weighing at least 6 kg.
Limitations of Use:
TRIUMEQ and TRIUMEQ PD alone are not recommended in patients with resistance‑associated integrase substitutions or clinically suspected integrase strand transfer inhibitor (INSTI) resistance because the dose of dolutegravir in TRIUMEQ and TRIUMEQ PD is insufficient in these subpopulations. See full prescribing information for TIVICAY (dolutegravir).
2. Triumeq Dosage and Administration
2.1 Screening for HLA−B*5701 Allele prior to Initiating TRIUMEQ
Screen for the HLA‑B*5701 allele prior to initiating therapy with TRIUMEQ or TRIUMEQ PD [see Boxed Warning, Warnings and Precautions (5.1)].
2.2 Testing prior to or When Initiating Treatment with TRIUMEQ
Prior to or when initiating TRIUMEQ or TRIUMEQ PD, test patients for HBV infection [see Warnings and Precautions (5.2)].
2.3 Overview of TRIUMEQ Dosage Forms
TRIUMEQ is available in two dosage forms. Do not substitute TRIUMEQ tablets and TRIUMEQ PD tablets for oral suspension on a milligram-per-milligram basis due to differing pharmacokinetic profiles for the dolutegravir component [see Warnings and Precautions (5.7), Clinical Pharmacology (12.3)].
- •
- TRIUMEQ tablets: 600 mg of abacavir, 50 mg of dolutegravir, and 300 mg of lamivudine. TRIUMEQ is recommended in adults and pediatric patients weighing at least 25 kg [see Dosage and Administration (2.4, 2.5)].
- •
- TRIUMEQ PD tablets for oral suspension: 60 mg of abacavir, 5 mg of dolutegravir, and 30 mg of lamivudine. TRIUMEQ PD is recommended in pediatric patients weighing 6 kg to less than 25 kg [see Dosage and Administration (2.5)].
- •
- Because TRIUMEQ PD is a fixed-dose tablet and the dosage of individual components cannot be adjusted, it may lead to a suboptimal dosing for patients weighing ≥25 kg. TRIUMEQ PD is not recommended in patients weighing 25 kg or more [see Dosage and Administration (2.4, 2.5)].
2.4 Recommended Dosage in Adults
TRIUMEQ is a fixed-dose combination product containing 600 mg of abacavir, 50 mg of dolutegravir, and 300 mg of lamivudine. The recommended dosage regimen of TRIUMEQ in adults is one tablet once daily orally with or without food. Do not use TRIUMEQ PD in adults.
2.5 Recommended Dosage and Administration Instructions for Pediatric Patients Weighing at Least 6 kg
The dosage and dosage form recommended for pediatric patients varies by weight as shown in Table 1 below.
| a TRIUMEQ is a fixed-dose combination product containing 600 mg of abacavir, 50 mg of dolutegravir, and 300 mg of lamivudine. | |||
| b TRIUMEQ PD is a fixed-dose combination product containing 60 mg of abacavir, 5 mg of dolutegravir, and 30 mg of lamivudine. | |||
|
Body Weight |
TRIUMEQ Tabletsa |
TRIUMEQ PDb Number of Tablets |
Total Daily Dose |
|
6 kg to <10 kg |
Not recommended |
3 tablets once daily |
180 mg abacavir, 15 mg dolutegravir, and 90 mg lamivudine once daily |
|
10 kg to <14 kg |
Not recommended |
4 tablets once daily |
240 mg abacavir, 20 mg dolutegravir, and 120 mg lamivudine once daily |
|
14 kg to <20 kg |
Not recommended |
5 tablets once daily |
300 mg abacavir, 25 mg dolutegravir, and 150 mg lamivudine once daily |
|
20 kg to <25 kg |
Not recommended |
6 tablets once daily |
360 mg abacavir, 30 mg dolutegravir, and 180 mg lamivudine once daily |
|
≥25 kg |
1 tablet once daily |
Not recommended |
600 mg of abacavir, 50 mg of dolutegravir, and 300 mg of lamivudine |
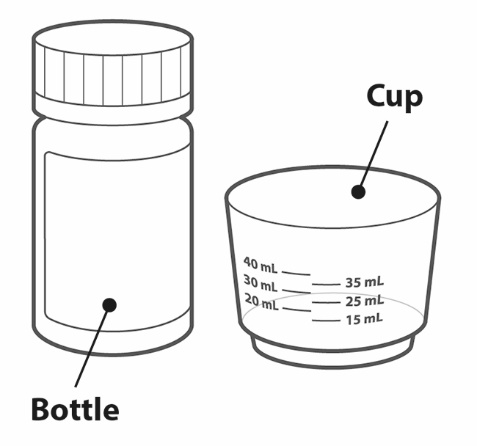
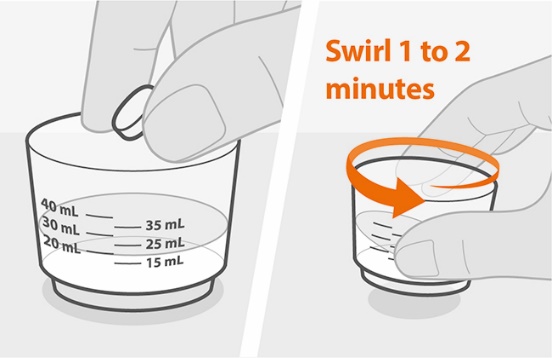
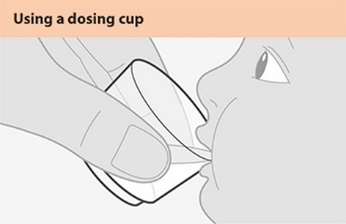
Administer TRIUMEQ PD tablets for oral suspension with or without food. Instruct patients (or instruct caregivers) to fully disperse the tablets for oral suspension in 20 mL of drinking water (if using 4, 5, or 6 tablets for oral suspension) or 15 mL (if using 3 tablets for oral suspension) in the supplied cup; swirl the suspension so that no lumps remain. After full dispersion, administer the oral suspension within 30 minutes of mixing [see Instructions for Use]. Do not swallow the tablets for oral suspension whole, and do not chew, cut, or crush the tablets.
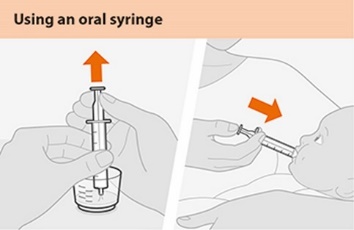
For children unable to use the supplied cup, an appropriate-sized syringe may be used to administer the oral suspension.
Administer TRIUMEQ tablet with or without food. Do not chew, cut, or crush the tablet.
2.6 Dosage Recommendation with Certain Concomitant Medications
The dolutegravir dose in TRIUMEQ (50 mg) and TRIUMEQ PD (5 mg) is insufficient when coadministered with medications listed in Table 2 that may decrease dolutegravir concentrations; the following dolutegravir dosage regimen is recommended.
|
Coadministered Drug |
Dosing Recommendation |
|
Efavirenz, fosamprenavir/ritonavir, tipranavir/ritonavir, carbamazepine, or rifampin |
In adults and in pediatric patients weighing at least 25 kg, the recommended dolutegravir dosage regimen is 50 mg twice daily. Thus, an additional TIVICAY 50-mg tablet, separated by 12 hours from TRIUMEQ, should be taken. In pediatric patients weighing 6 kg to <25 kg, an additional weight-based dose of dolutegravir should be given separated by 12 hours from TRIUMEQ PD.
|
2.7 Not Recommended Due to Lack of Dosage Adjustment
Because TRIUMEQ and TRIUMEQ PD are fixed-dose tablets and cannot be dose adjusted, TRIUMEQ and TRIUMEQ PD are not recommended in:
- •
- patients with creatinine clearance <30 mL/min and pediatric patients with a similar degree of renal impairment based on age-appropriate renal function assessment. There are no data available on the use of lamivudine, a component of TRIUMEQ and TRIUMEQ PD, in pediatric patients with renal impairment [see Use in Specific Populations (8.4, 8.6)].
- •
- patients with mild hepatic impairment. TRIUMEQ and TRIUMEQ PD are contraindicated in patients with moderate or severe hepatic impairment [see Contraindications (4), Use in Specific Populations (8.7)].
3. Dosage Forms and Strengths
TRIUMEQ tablets are purple, biconvex, oval, and debossed with “572 Trı” on one side. Each film-coated tablet contains 600 mg of abacavir (as abacavir sulfate), 50 mg of dolutegravir (as dolutegravir sodium), and 300 mg of lamivudine [see Description (11)].
TRIUMEQ PD tablets for oral suspension are yellow, capsule-shaped, strawberry cream flavored, biconvex, film-coated tablets debossed with “SV WTU” on one side. Each film-coated tablet contains 60 mg of abacavir (as abacavir sulfate), 5 mg of dolutegravir (as dolutegravir sodium), and 30 mg of lamivudine [see Description (11)].
4. Contraindications
TRIUMEQ and TRIUMEQ PD are contraindicated in patients:
- •
- who have the HLA-B*5701 allele [see Warnings and Precautions (5.1)].
- •
- with prior hypersensitivity reaction to abacavir, dolutegravir [see Warnings and Precautions (5.1)], or lamivudine.
- •
- receiving dofetilide due to the potential for increased dofetilide plasma concentrations and the risk for serious and/or life-threatening events with concomitant use of dolutegravir [see Drug Interactions (7)].
- •
- with moderate or severe hepatic impairment [see Use in Specific Populations (8.7)].
5. Warnings and Precautions
5.1 Hypersensitivity Reactions
Hypersensitivity reactions have been reported with the use of abacavir or dolutegravir, components of TRIUMEQ and TRIUMEQ PD.
Abacavir
Serious and sometimes fatal hypersensitivity reactions have occurred with abacavir-containing regimens. See full prescribing information for ZIAGEN (abacavir).
Abacavir hypersensitivity reactions have included multi-organ failure and anaphylaxis and typically occurred within the first 6 weeks of treatment with abacavir (median time to onset was 9 days); although abacavir hypersensitivity reactions have occurred any time during treatment [see Adverse Reactions (6.1)]. Patients who carry the HLA‑B*5701 allele are at a higher risk of abacavir hypersensitivity reactions; although, patients who do not carry the HLA‑B*5701 allele have developed hypersensitivity reactions. Hypersensitivity to abacavir was reported in approximately 206 (8%) of 2,670 patients in 9 clinical trials with abacavir-containing products where HLA‑B*5701 screening was not performed. The incidence of suspected abacavir hypersensitivity reactions in clinical trials was 1% when subjects carrying the HLA-B*5701 allele were excluded. In any patient treated with abacavir, the clinical diagnosis of hypersensitivity reaction must remain the basis of clinical decision making.
Due to the potential for severe, serious, and possibly fatal hypersensitivity reactions with abacavir:
- •
- All patients should be screened for the HLA‑B*5701 allele prior to initiating therapy with TRIUMEQ or TRIUMEQ PD or reinitiation of therapy with TRIUMEQ or TRIUMEQ PD, unless patients have a previously documented HLA‑B*5701 allele assessment.
- •
- TRIUMEQ and TRIUMEQ PD are contraindicated in patients with a prior hypersensitivity reaction to abacavir and in HLA‑B*5701‑positive patients.
- •
- Before starting TRIUMEQ or TRIUMEQ PD, review medical history for prior exposure to any abacavir-containing product. NEVER restart TRIUMEQ or TRIUMEQ PD or any other abacavir-containing product following a hypersensitivity reaction to abacavir, regardless of HLA‑B*5701 status.
- •
- To reduce the risk of a life‑threatening hypersensitivity reaction, regardless of HLA‑B*5701 status, discontinue TRIUMEQ or TRIUMEQ PD immediately if a hypersensitivity reaction is suspected, even when other diagnoses are possible (e.g., acute onset respiratory diseases such as pneumonia, bronchitis, pharyngitis, or influenza; gastroenteritis; or reactions to other medications). Clinical status, including liver chemistries, should be monitored and appropriate therapy initiated.
- •
- If a hypersensitivity reaction cannot be ruled out, do not restart TRIUMEQ or TRIUMEQ PD or any other abacavir-containing products because more severe symptoms, which may include life-threatening hypotension and death, can occur within hours.
- •
- Clinically, it is not possible to determine whether a hypersensitivity reaction with TRIUMEQ or TRIUMEQ PD would be caused by abacavir or dolutegravir. Therefore, never restart TRIUMEQ or TRIUMEQ PD or any other abacavir- or dolutegravir-containing product in patients who have stopped therapy with TRIUMEQ or TRIUMEQ PD due to a hypersensitivity reaction.
- •
- If a hypersensitivity reaction is ruled out, patients may restart TRIUMEQ or TRIUMEQ PD. Rarely, patients who have stopped abacavir for reasons other than symptoms of hypersensitivity have also experienced life-threatening reactions within hours of reinitiating abacavir therapy. Therefore, reintroduction of TRIUMEQ or TRIUMEQ PD, or any other abacavir-containing product, is recommended only if medical care can be readily accessed.
- •
- A Medication Guide and Warning Card that provide information about recognition of abacavir hypersensitivity reactions should be dispensed with each new prescription and refill.
Dolutegravir
Hypersensitivity reactions have been reported and were characterized by rash, constitutional findings, and sometimes organ dysfunction, including liver injury. The events were reported in <1% of subjects receiving TIVICAY in Phase 3 clinical trials. Discontinue TRIUMEQ or TRIUMEQ PD and other suspect agents immediately if signs or symptoms of hypersensitivity reactions develop (including, but not limited to, severe rash or rash accompanied by fever, general malaise, fatigue, muscle or joint aches, blisters or peeling of the skin, oral blisters or lesions, conjunctivitis, facial edema, hepatitis, eosinophilia, angioedema, difficulty breathing). Clinical status, including liver aminotransferases, should be monitored and appropriate therapy initiated. Delay in stopping treatment with TRIUMEQ or TRIUMEQ PD or other suspect agents after the onset of hypersensitivity may result in a life-threatening reaction.
Clinically, it is not possible to determine whether a hypersensitivity reaction with TRIUMEQ or TRIUMEQ PD would be caused by abacavir or dolutegravir. Therefore, never restart TRIUMEQ or TRIUMEQ PD or any other abacavir- or dolutegravir-containing product in patients who have stopped therapy with TRIUMEQ or TRIUMEQ PD due to a hypersensitivity reaction.
5.2 Patients Co-infected with HIV-1 and HBV: Emergence of Lamivudine-Resistant HBV and the Risk of Posttreatment Exacerbations of HBV
All patients with HIV-1 should be tested for the presence of HBV prior to or when initiating TRIUMEQ or TRIUMEQ PD.
Emergence of Lamivudine Resistant HBV
Safety and efficacy of lamivudine have not been established for treatment of chronic HBV in subjects dually infected with HIV-1 and HBV. Emergence of HBV variants associated with resistance to lamivudine has been reported in HIV‑1−infected subjects who have received lamivudine‑containing antiretroviral regimens in the presence of concurrent infection with HBV. If a decision is made to administer TRIUMEQ or TRIUMEQ PD to patients co-infected with HIV-1 and HBV, additional treatment should be considered for appropriate treatment of chronic HBV; otherwise, consider an alternative regimen.
Severe Acute Exacerbations of HBV in Patients Co-infected with HIV-1 and HBV
Severe acute exacerbations of HBV have been reported in patients who are co-infected with HIV-1 and HBV and have discontinued products containing lamivudine, and may occur with discontinuation of TRIUMEQ or TRIUMEQ PD. Patients who are co-infected with HIV-1 and HBV who discontinue TRIUMEQ or TRIUMEQ PD should be closely monitored with both clinical and laboratory follow-up for at least several months after stopping treatment with TRIUMEQ or TRIUMEQ PD. If appropriate, initiation of anti-HBV therapy may be warranted, especially in patients with advanced liver disease or cirrhosis since posttreatment exacerbation of hepatitis may lead to hepatic decompensation and liver failure.
5.3 Hepatotoxicity
Hepatic adverse events have been reported in patients receiving a dolutegravir-containing regimen [see Adverse Reactions (6.1, 6.2)]. Patients with underlying hepatitis B or C may be at increased risk for worsening or development of transaminase elevations with use of TRIUMEQ or TRIUMEQ PD [see Adverse Reactions (6.1)]. In some cases, the elevations in transaminases were consistent with immune reconstitution syndrome or hepatitis B reactivation particularly in the setting where anti-hepatitis therapy was withdrawn. Cases of hepatic toxicity, including elevated serum liver biochemistries, hepatitis, and acute liver failure, have also been reported in patients, including pediatric patients receiving a dolutegravir-containing regimen who had no pre-existing hepatic disease or other identifiable risk factors. Drug-induced liver injury leading to liver transplant has been reported with TRIUMEQ. Monitoring for hepatotoxicity is recommended.
5.4 Lactic Acidosis and Severe Hepatomegaly with Steatosis
Lactic acidosis and severe hepatomegaly with steatosis, including fatal cases, have been reported with the use of nucleoside analogues, including abacavir and lamivudine (components of TRIUMEQ and TRIUMEQ PD). A majority of these cases have been in women. Female sex and obesity may be risk factors for the development of lactic acidosis and severe hepatomegaly with steatosis in patients treated with antiretroviral nucleoside analogues. See full prescribing information for ZIAGEN (abacavir) and EPIVIR (lamivudine). Treatment with TRIUMEQ or TRIUMEQ PD should be suspended in any patient who develops clinical or laboratory findings suggestive of lactic acidosis or pronounced hepatotoxicity, which may include hepatomegaly and steatosis even in the absence of marked transaminase elevations.
5.5 Risk of Adverse Reactions or Loss of Virologic Response Due to Drug Interactions
The concomitant use of TRIUMEQ or TRIUMEQ PD and other drugs may result in known or potentially significant drug interactions, some of which may lead to [see Contraindications (4), Drug Interactions (7.3)]:
- •
- Loss of therapeutic effect of TRIUMEQ or TRIUMEQ PD and possible development of resistance.
- •
- Possible clinically significant adverse reactions from greater exposures of concomitant drugs.
See Table 6 for steps to prevent or manage these possible and known significant drug interactions, including dosing recommendations. Consider the potential for drug interactions prior to and during therapy with TRIUMEQ or TRIUMEQ PD, review concomitant medications during therapy with TRIUMEQ or TRIUMEQ PD, and monitor for the adverse reactions associated with the concomitant drugs.
5.6 Immune Reconstitution Syndrome
Immune reconstitution syndrome has been reported in patients treated with combination antiretroviral therapy, including TRIUMEQ or TRIUMEQ PD. During the initial phase of combination antiretroviral treatment, patients whose immune systems respond may develop an inflammatory response to indolent or residual opportunistic infections (such as Mycobacterium avium infection, cytomegalovirus, Pneumocystis jirovecii pneumonia [PCP], or tuberculosis), which may necessitate further evaluation and treatment.
Autoimmune disorders (such as Graves’ disease, polymyositis, Guillain-Barré syndrome, autoimmune hepatitis) have also been reported to occur in the setting of immune reconstitution; however, the time to onset is more variable, and can occur many months after initiation of treatment.
5.7 Different Formulations Are Not Substitutable
TRIUMEQ and TRIUMEQ PD are not bioequivalent and are not substitutable on a milligram-per-milligram basis [see Clinical Pharmacology (12.3)]. If a pediatric patient switches from the tablets for oral suspension to the tablets, the dosage must be adjusted [see Dosage and Administration (2.3, 2.5)]. Incorrect dosing of a given formulation may result in underdosing and loss of therapeutic effect and possible development of resistance or possible clinically significant adverse reactions from greater exposure to the individual components.
5.8 Myocardial Infarction
Several prospective, observational, epidemiological studies have reported an association with the use of abacavir and the risk of myocardial infarction (MI). Meta-analyses of randomized, controlled clinical trials have observed no excess risk of MI in abacavir‑treated subjects as compared with control subjects. To date, there is no established biological mechanism to explain a potential increase in risk. In totality, the available data from the observational studies and from controlled clinical trials show inconsistency; therefore, evidence for a causal relationship between abacavir and the risk of MI is inconclusive.
As a precaution, the underlying risk of coronary heart disease should be considered when prescribing antiretroviral therapies, including abacavir, and action taken to minimize all modifiable risk factors (e.g., hypertension, hyperlipidemia, diabetes mellitus, smoking).
6. Adverse Reactions/Side Effects
The following adverse reactions are discussed in other sections of the labeling:
- •
- Serious and sometimes fatal hypersensitivity reaction [see Boxed Warning, Warnings and Precautions (5.1)].
- •
- Exacerbations of hepatitis B [see Boxed Warning, Warnings and Precautions (5.3)].
- •
- Hepatotoxicity [see Warnings and Precautions (5.3)].
- •
- Lactic acidosis and severe hepatomegaly with steatosis [see Warnings and Precautions (5.4)].
- •
- Immune reconstitution syndrome [see Warnings and Precautions (5.6)].
- •
- Myocardial infarction [see Warnings and Precautions (5.8)].
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared with rates in the clinical trials of another drug and may not reflect the rates observed in clinical practice.
Clinical Trials in Adults
Serious and Fatal Abacavir-Associated Hypersensitivity Reactions: In clinical trials, serious and sometimes fatal hypersensitivity reactions have occurred with abacavir, a component of TRIUMEQ and TRIUMEQ PD [see Boxed Warning, Warnings and Precautions (5.1)]. These reactions have been characterized by 2 or more of the following signs or symptoms: (1) fever; (2) rash; (3) gastrointestinal symptoms (including nausea, vomiting, diarrhea, or abdominal pain); (4) constitutional symptoms (including generalized malaise, fatigue, or achiness); (5) respiratory symptoms (including dyspnea, cough, or pharyngitis). Almost all abacavir hypersensitivity reactions include fever and/or rash as part of the syndrome.
Other signs and symptoms have included lethargy, headache, myalgia, edema, arthralgia, and paresthesia. Anaphylaxis, liver failure, renal failure, hypotension, adult respiratory distress syndrome, respiratory failure, myolysis, and death have occurred in association with these hypersensitivity reactions. Physical findings have included lymphadenopathy, mucous membrane lesions (conjunctivitis and mouth ulcerations), and maculopapular or urticarial rash (although some patients had other types of rashes and others did not have a rash). There were reports of erythema multiforme. Laboratory abnormalities included elevated liver chemistries, elevated creatine phosphokinase, elevated creatinine, and lymphopenia and abnormal chest x‑ray findings (predominantly infiltrates, which were localized).
Serious Dolutegravir Hypersensitivity Reactions: In clinical trials, hypersensitivity reactions have occurred with dolutegravir, a component of TRIUMEQ and TRIUMEQ PD [see Warnings and Precautions (5.1)]. These hypersensitivity reactions have been characterized by rash, constitutional findings, and sometimes organ dysfunction, including liver injury.
Additional Treatment-Emergent Adverse Drug Reactions (ADRs) with Use of TRIUMEQ: The safety assessment of TRIUMEQ is primarily based on the analyses of data from a randomized, international, multicenter, double-blind, active-controlled trial, SINGLE (ING114467) and supported by data in treatment-experienced, INSTI-naive subjects from SAILING (ING111762) and by data from other treatment-naive trials. See full prescribing information for TIVICAY.
Treatment-Naive Subjects: In SINGLE, 833 adult subjects were randomized and received at least one dose of either dolutegravir (TIVICAY) 50 mg with fixed-dose abacavir and lamivudine (EPZICOM) once daily (n = 414) or fixed-dose efavirenz/emtricitabine/tenofovir (ATRIPLA) once daily (n = 419) (study treatment was blinded through Week 96 and open-label from Week 96 through Week 144). Through 144 weeks, the rate of adverse events leading to discontinuation was 4% in subjects receiving TIVICAY + EPZICOM and 14% in subjects receiving ATRIPLA once daily.
Treatment‑emergent ADRs of moderate to severe intensity observed in at least 2% of subjects in either treatment arm of SINGLE are provided in Table 3.
| a Includes pooled terms: rash, rash generalized, rash macular, rash maculo-papular, rash pruritic, and drug eruption. | ||
|
Adverse Reaction |
TIVICAY + EPZICOM Once Daily (n = 414) |
ATRIPLA Once Daily (n = 419) |
|
Psychiatric | ||
|
Insomnia |
3% |
3% |
|
Depression |
1% |
2% |
|
Abnormal dreams |
<1% |
2% |
|
Nervous System | ||
|
Dizziness |
<1% |
5% |
|
Headache |
2% |
2% |
|
Gastrointestinal | ||
|
Nausea |
<1% |
3% |
|
Diarrhea |
<1% |
2% |
|
General Disorders | ||
|
Fatigue |
2% |
2% |
|
Skin and Subcutaneous Tissue | ||
|
Rasha |
<1% |
6% |
|
Ear and Labyrinth | ||
|
Vertigo |
0 |
2% |
Treatment-Experienced Subjects: SAILING is an international, double-blind trial in INSTI-naive, antiretroviral treatment-experienced adult subjects. Subjects were randomized and received either TIVICAY 50 mg once daily or raltegravir 400 mg twice daily with investigator-selected background regimen consisting of up to 2 agents, including at least one fully active agent. At 48 weeks, the rate of adverse events leading to discontinuation was consistent with that seen in the overall treatment-naive patient population. See full prescribing information for TIVICAY.
The ADRs observed in the subset of subjects who received TIVICAY + EPZICOM were generally consistent with those seen in the overall treatment-naive patient population.
Less Common Adverse Reactions Observed in Clinical Trials: The following adverse reactions occurred in <2% of treatment-naive or treatment-experienced subjects in any one trial. These events have been included because of their seriousness and/or assessment of potential causal relationship.
Gastrointestinal Disorders: Abdominal pain, abdominal distention, abdominal discomfort, dyspepsia, flatulence, gastroesophageal reflux disease, upper abdominal pain, vomiting.
General Disorders: Fever, lethargy.
Hepatobiliary Disorders: Hepatitis.
Metabolism and Nutrition Disorders: Anorexia, hypertriglyceridemia.
Musculoskeletal Disorders: Arthralgia, myositis.
Nervous System Disorders: Somnolence.
Psychiatric Disorders: Suicidal ideation, attempt, behavior, or completion. These events were observed primarily in subjects with a pre-existing history of depression or other psychiatric illness. Nightmare and sleep disorder.
Renal and Urinary Disorders: Renal impairment.
Skin and Subcutaneous Tissue Disorders: Pruritus.
Laboratory Abnormalities: Treatment-Naive Subjects: Selected laboratory abnormalities (Grades 2 to 4) with a worsening grade from baseline and representing the worst-grade toxicity in at least 2% of subjects in SINGLE are presented in Table 4. The mean change from baseline observed for selected lipid values is presented in Table 5.
| ALT = Alanine aminotransferase, AST = Aspartate aminotransferase, ULN = upper limit of normal. | |||||
|
Laboratory Abnormality |
TIVICAY + EPZICOM Once Daily (n = 414) |
ATRIPLA Once Daily (n = 419) |
|||
|
ALT | |||||
|
Grade 2 (>2.5-5.0 x ULN) |
3% |
5% |
|||
|
Grade 3 to 4 (>5.0 x ULN) |
1% |
<1% |
|||
|
AST | |||||
|
Grade 2 (>2.5-5.0 x ULN) |
3% |
4% |
|||
|
Grade 3 to 4 (>5.0 x ULN) |
1% |
3% |
|||
|
Creatine kinase | |||||
|
Grade 2 (6.0-9.9 x ULN) |
5% |
3% |
|||
|
Grade 3 to 4 (≥10.0 x ULN) |
7% |
8% |
|||
|
Hyperglycemia | |||||
|
Grade 2 (126-250 mg/dL) |
9% |
6% |
|||
|
Grade 3 (>250 mg/dL) |
2% |
<1% |
|||
|
Lipase | |||||
|
Grade 2 (>1.5-3.0 x ULN) |
11% |
11% |
|||
|
Grade 3 to 4 (>3.0 ULN) |
5% |
4% |
|||
|
Total neutrophils | |||||
|
Grade 2 (0.75-0.99 x 109) |
4% |
5% |
|||
|
Grade 3 to 4 (<0.75 x 109) |
3% |
3% |
|||
| HDL = High-density lipoprotein, LDL = Low-density lipoprotein. | ||||||||
| a Subjects on lipid-lowering agents at baseline were excluded from these analyses (TIVICAY + EPZICOM: n = 30 and ATRIPLA: n = 27). Seventy-two subjects initiated a lipid-lowering agent post-baseline; their last fasted on-treatment values (prior to starting the agent) were used regardless of whether they discontinued the agent (TIVICAY + EPZICOM: n = 36 and ATRIPLA: n = 36). | ||||||||
|
Lipid |
TIVICAY + EPZICOM Once Daily (n = 414) |
ATRIPLA Once Daily (n = 419) |
||||||
|
Cholesterol (mg/dL) |
24.0 |
26.7 |
||||||
|
HDL cholesterol (mg/dL) |
5.4 |
7.2 |
||||||
|
LDL cholesterol (mg/dL) |
16.0 |
14.6 |
||||||
|
Triglycerides (mg/dL) |
13.6 |
31.9 |
||||||
Treatment-Experienced Subjects: Laboratory abnormalities observed in SAILING were generally similar compared with observations seen in the treatment-naive trials.
Hepatitis C Virus Co-infection: In SINGLE, the pivotal Phase 3 trial, subjects with hepatitis C virus co-infection were permitted to enroll provided that baseline liver chemistry tests did not exceed 5 times the upper limit of normal; subjects with hepatitis B co-infection were excluded. Overall, the safety profile in subjects with hepatitis C virus co-infection was similar to that observed in subjects without hepatitis C co-infection, although the rates of aspartate aminotransferase (AST) and alanine aminotransferase (ALT) abnormalities were higher in the subgroup with hepatitis C virus co-infection for both treatment groups. Grades 2 to 4 ALT abnormalities in hepatitis C co-infected compared with HIV mono-infected subjects receiving TRIUMEQ were observed in 15% and 2% (vs. 24% and 4% of subjects treated with ATRIPLA) (Week 96 analysis), respectively [see Warnings and Precautions (5.2)]. See also full prescribing information for TIVICAY.
Changes in Serum Creatinine: Dolutegravir has been shown to increase serum creatinine due to inhibition of tubular secretion of creatinine without affecting renal glomerular function [see Clinical Pharmacology (12.2)]. Increases in serum creatinine occurred within the first 4 weeks of treatment and remained stable through 144 weeks. In SINGLE, a mean change from baseline of 0.14 mg/dL (range: -0.25 mg/dL to 0.81 mg/dL) was observed after 144 weeks of treatment. Creatinine increases were similar in treatment-experienced subjects.
Abacavir and Lamivudine: Laboratory abnormalities observed in clinical trials of ZIAGEN (in combination with other antiretroviral treatment) were anemia, neutropenia, liver function test abnormalities, and elevations of creatine phosphokinase (CPK), blood glucose, and triglycerides. Additional laboratory abnormalities observed in clinical trials of EPIVIR (in combination with other antiretroviral treatment) were thrombocytopenia and elevated levels of bilirubin, amylase, and lipase.
Clinical Trials Experience in Pediatric Subjects
Abacavir, Dolutegravir and Lamivudine: The safety of TRIUMEQ PD and TRIUMEQ in pediatric subjects with HIV-1 infection weighing at least 6 kg was evaluated in the IMPAACT 2019 trial. This was a multicenter, open-label, non-comparative trial of pediatric subjects with HIV-1 infection, younger than 12 years of age. Fifty-seven subjects weighing at least 6 kg to less than 40 kg were enrolled in this trial [see Use in Specific Populations (8.4), Clinical Pharmacology (12.3), Clinical Studies (14.2)]. Overall, the safety data in this pediatric study was similar to that seen in adults.
The safety analysis through Week 48 included 57 subjects weighing at least 6 kg at enrollment who received the recommended dose (determined by weight) and formulation. This analysis showed that 26% of subjects experienced clinical adverse reactions. The most common adverse reactions were classified as laboratory abnormalities and included decreased glomerular filtration rate (n = 13, 23%), increased blood creatinine (n = 10, 18%), and increased ALT (n = 3, 5%). All other adverse reactions occurred at a rate of <2% of participants. Two subjects reported Grade 3 or 4 adverse reactions. One subject, an 8-year-old female who weighed 22 kg at baseline, experienced Grade 3 increased blood creatinine and Grade 3 decreased glomerular filtration rate. By Week 48, the glomerular filtration rate was improving, and the events did not lead to drug discontinuation. Another subject, a 7-year-old male who weighed 20 kg at baseline, experienced drug-induced liver injury with Grade 4 increased ALT and AST following 36 weeks of treatment with TRIUMEQ PD. Clinical signs or symptoms of hepatitis were not reported, and ALT and AST values normalized after TRIUMEQ PD was discontinued.
Abacavir and Lamivudine: The safety of once-daily compared with twice-daily dosing of abacavir and lamivudine, administered as either single products or as EPZICOM, was assessed in the ARROW trial (n = 336). Primary safety assessment in the ARROW (COL105677) trial was based on Grade 3 and Grade 4 adverse events. One event of Grade 4 hepatitis in the once-daily cohort was considered as uncertain causality by the investigator and all other Grade 3 or 4 adverse events were considered not related by the investigator. No additional safety issues were identified in pediatric subjects compared with historical data in adults.
Dolutegravir: The safety of dolutegravir in pediatric subjects with HIV-1 infection weighing at least 6 kg was evaluated in the IMPAACT P1093 trial [see Use in Specific Populations (8.4), Clinical Pharmacology (12.3)]. Overall, the safety data in this pediatric study was similar to that seen in adults.
IMPAACT P1093 is an ongoing multicenter, open-label, non-comparative trial of pediatric subjects with HIV-1 infection, aged <18 years. One hundred and forty-two subjects weighing at least 6 kg were enrolled in this trial [see Use in Specific Populations (8.4), Clinical Pharmacology (12.3), Clinical Studies (14.2)].
The safety analysis through Week 24 included 60 subjects weighing at least 6 kg at enrollment who received the recommended dose (determined by weight and age) and formulation. This analysis showed that 13% of subjects experienced adverse reactions. Grade 1 to 2 adverse reactions reported by more than one subject was immune reconstitution inflammatory syndrome (n = 2). There were no Grade 3 or 4 adverse reactions reported. No adverse reactions led to discontinuation.
The Grade 3 or 4 laboratory abnormalities reported in more than one subject weighing at least 6 kg at enrollment were decreased neutrophil count (n = 5), decreased blood bicarbonate (n = 3), increased lipase (n = 2), and increased blood potassium (n = 2). These laboratory events were not considered to be drug related. Changes in median serum creatinine were similar to those observed in adults.
6.2 Postmarketing Experience
In addition to adverse reactions reported from clinical trials, the following adverse reactions have been identified during postmarketing use with one or more of the components of TRIUMEQ and TRIUMEQ PD. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Blood and Lymphatic Systems
Aplastic anemia, anemia (including pure red cell aplasia and severe anemias progressing on therapy), lymphadenopathy, splenomegaly.
Digestive
Stomatitis.
Gastrointestinal
Pancreatitis.
General
Weakness.
Hepatobiliary Disorders
Acute liver failure, liver transplant [see Warnings and Precautions (5.3)].
Hypersensitivity
Sensitization reactions (including anaphylaxis), urticaria [see Warnings and Precautions (5.1), Adverse Reactions (6.1)].
Investigations
Weight increased.
Metabolism and Nutrition Disorders
Hyperlactemia.
Musculoskeletal
CPK elevation, muscle weakness, myalgia, rhabdomyolysis.
Nervous
Paresthesia, peripheral neuropathy, seizures.
Psychiatric
Anxiety.
Respiratory
Abnormal breath sounds/wheezing.
Skin
Alopecia, erythema multiforme. Suspected Stevens‑Johnson syndrome (SJS) and toxic epidermal necrolysis (TEN) have been reported in patients receiving abacavir primarily in combination with medications known to be associated with SJS and TEN, respectively. Because of the overlap of clinical signs and symptoms between hypersensitivity to abacavir and SJS and TEN, and the possibility of multiple drug sensitivities in some patients, abacavir should be discontinued and not restarted in such cases [see Adverse Reactions (6.1)].
Related/similar drugs
7. Drug Interactions
7.1 Effect of Dolutegravir on the Pharmacokinetics of Other Agents
In vitro, dolutegravir inhibited the renal organic cation transporters (OCT)2 (IC50 = 1.93 microM) and multidrug and toxin extrusion transporter (MATE)1 (IC50 = 6.34 microM). In vivo, dolutegravir inhibits tubular secretion of creatinine by inhibiting OCT2 and potentially MATE1. Dolutegravir may increase plasma concentrations of drugs eliminated via OCT2 or MATE1 (dofetilide, dalfampridine, and metformin) [see Contraindications (4), Drug Interactions (7.3)].
In vitro, dolutegravir inhibited the basolateral renal transporters, organic anion transporter (OAT) 1 (IC50 = 2.12 microM) and OAT3 (IC50 = 1.97 microM). However, in vivo, dolutegravir did not alter the plasma concentrations of tenofovir or para-amino hippurate, substrates of OAT1 and OAT3.
In vitro, dolutegravir did not inhibit (IC50 >50 microM) the following: cytochrome P450 (CYP)1A2, CYP2A6, CYP2B6, CYP2C8, CYP2C9, CYP2C19, CYP2D6, CYP3A, uridine diphosphate (UDP)-glucuronosyl transferase (UGT)1A1, UGT2B7, P-glycoprotein (P-gp), breast cancer resistance protein (BCRP), bile salt export pump (BSEP), organic anion transporter polypeptide (OATP)1B1, OATP1B3, OCT1, or multidrug resistance protein (MRP)2, or MRP4. In vitro, dolutegravir did not induce CYP1A2, CYP2B6, CYP3A4. Based on these data and the results of drug interaction trials, dolutegravir is not expected to affect the pharmacokinetics of drugs that are substrates of these enzymes or transporters.
In drug interaction trials, dolutegravir did not have a clinically relevant effect on the pharmacokinetics of the following drugs: tenofovir, methadone, midazolam, rilpivirine, and oral contraceptives containing norgestimate and ethinyl estradiol. Using cross-study comparisons to historical pharmacokinetic data for each interacting drug, dolutegravir did not appear to affect the pharmacokinetics of the following drugs: atazanavir, darunavir, efavirenz, etravirine, fosamprenavir, lopinavir, ritonavir, and boceprevir.
7.2 Effect of Other Agents on the Pharmacokinetics of Dolutegravir
Dolutegravir is metabolized by UGT1A1 with some contribution from CYP3A. Dolutegravir is also a substrate of UGT1A3, UGT1A9, BCRP, and P-gp in vitro. Drugs that induce those enzymes and transporters may decrease dolutegravir plasma concentrations and reduce the therapeutic effect of dolutegravir.
Coadministration of dolutegravir and other drugs that inhibit these enzymes may increase dolutegravir plasma concentrations.
Etravirine significantly reduced plasma concentrations of dolutegravir, but the effect of etravirine was mitigated by coadministration of lopinavir/ritonavir or darunavir/ritonavir and is expected to be mitigated by atazanavir/ritonavir (Table 6) [see Drug Interactions (7.3), Clinical Pharmacology (12.3)].
In vitro, dolutegravir was not a substrate of OATP1B1 or OATP1B3.
Darunavir/ritonavir, lopinavir/ritonavir, rilpivirine, tenofovir, boceprevir, prednisone, rifabutin, and omeprazole had no clinically significant effect on the pharmacokinetics of dolutegravir.
7.3 Established and Other Potentially Significant Drug Interactions
There were no drug-drug interaction trials conducted with the abacavir, dolutegravir, and lamivudine fixed-dose combination tablets.
Information regarding potential drug interactions with the individual components of TRIUMEQ and TRIUMEQ PD are provided below. These recommendations are based on either drug interaction trials or predicted interactions due to the expected magnitude of interaction and potential for serious adverse events or loss of efficacy. [See Contraindications (4), Clinical Pharmacology (12.3).]
| a See Clinical Pharmacology (12.3) Table 8 or Table 10 for magnitude of interaction. | ||
|
Concomitant Drug Class:
|
Effect on Concentration |
Clinical Comment |
|
HIV-1 Antiviral Agents |
||
|
Non-nucleoside reverse transcriptase inhibitor: Etravirinea |
↓Dolutegravir |
Use of TRIUMEQ or TRIUMEQ PD with etravirine without coadministration of atazanavir/ritonavir, darunavir/ritonavir, or lopinavir/ritonavir is not recommended. |
|
Non-nucleoside reverse transcriptase inhibitor: Efavirenza |
↓Dolutegravir |
In adults and in pediatric patients weighing at least 25 kg, adjust dolutegravir dose to 50 mg twice daily. An additional 50-mg dose of TIVICAY should be taken, separated by 12 hours from TRIUMEQ. In pediatric patients weighing 6 to <25 kg, an additional weight-based dose of dolutegravir should be given separated by 12 hours from TRIUMEQ PD.
|
|
Non-nucleoside reverse transcriptase inhibitor: Nevirapine |
↓Dolutegravir |
Avoid coadministration with TRIUMEQ or TRIUMEQ PD because there are insufficient data to make dosing recommendations. |
|
Protease inhibitor: Fosamprenavir/ritonavira
|
↓Dolutegravir |
In adults and in pediatric patients weighing at least 25 kg, adjust dolutegravir dose to 50 mg twice daily. An additional TIVICAY 50-mg dose should be taken, separated by 12 hours from TRIUMEQ. In pediatric patients weighing 10 to <25 kg, an additional weight-based dose of dolutegravir should be given separated by 12 hours from TRIUMEQ PD.
|
|
Other Agents |
||
|
Antiarrhythmic: Dofetilide |
↑Dofetilide |
Coadministration is contraindicated with TRIUMEQ and TRIUMEQ PD [see Contraindications (4)]. |
|
Potassium channel blocker: Dalfampridine |
↑Dalfampridine |
Elevated levels of dalfampridine increase the risk of seizures. The potential benefits of taking dalfampridine concurrently with TRIUMEQ or TRIUMEQ PD should be considered against the risk of seizures in these patients. |
|
Carbamazepinea |
↓Dolutegravir |
In adults and in pediatric patients weighing at least 25 kg, adjust dolutegravir dose to 50 mg twice daily. An additional TIVICAY 50-mg dose should be taken, separated by 12 hours from TRIUMEQ. In pediatric patients weighing 6 to < 25 kg, an additional weight-based dose of dolutegravir should be given separated by 12 hours from TRIUMEQ PD.
|
|
Oxcarbazepine |
↓Dolutegravir |
Avoid coadministration with TRIUMEQ or TRIUMEQ PD because there are insufficient data to make dosing recommendations. |
|
Medications containing polyvalent cations
Cation-containing antacidsa or laxatives Sucralfate Buffered medications |
↓Dolutegravir |
Administer TRIUMEQ or TRIUMEQ PD 2 hours before or 6 hours after taking medications containing polyvalent cations. |
|
Oral calcium and iron supplements, including multivitamins containing calcium or irona |
↓Dolutegravir |
When taken with food, TRIUMEQ or TRIUMEQ PD and supplements or multivitamins containing calcium or iron can be taken at the same time. Under fasting conditions, TRIUMEQ or TRIUMEQ PD should be taken 2 hours before or 6 hours after taking supplements containing calcium or iron. |
|
Metformina |
↑Metformin |
Refer to the prescribing information for metformin for assessing the benefit and risk of concomitant use of TRIUMEQ or TRIUMEQ PD and metformin. |
|
Rifampina |
↓Dolutegravir |
In adults and in pediatric patients weighing at least 25 kg, adjust dolutegravir dose to 50 mg twice daily. An additional 50-mg dose of TIVICAY should be taken, separated by 12 hours from TRIUMEQ. In pediatric patients weighing 6 to <25 kg, an additional weight-based dose of dolutegravir should be given separated by 12 hours from TRIUMEQ PD.
|
Methadone
Abacavir: In a trial of 11 HIV-1–infected subjects receiving methadone-maintenance therapy with 600 mg of abacavir twice daily (twice the currently recommended dose), oral methadone clearance increased [see Clinical Pharmacology (12.3)]. This alteration will not result in a methadone dose modification in the majority of patients; however, an increased methadone dose may be required in a small number of patients.
Sorbitol
Lamivudine: Coadministration of single doses of lamivudine and sorbitol resulted in a sorbitol dose-dependent reduction in lamivudine exposures. When possible, avoid use of sorbitol-containing medicines with lamivudine-containing medicines [see Clinical Pharmacology (12.3)].
Riociguat
Abacavir: Coadministration with TRIUMEQ resulted in increased riociguat exposure, which may increase the risk of riociguat adverse reactions [see Clinical Pharmacology (12.3)]. The riociguat dose may need to be reduced. See full prescribing information for ADEMPAS (riociguat).
8. Use In Specific Populations
8.1 Pregnancy
Pregnancy Exposure Registry
There is a pregnancy exposure registry that monitors pregnancy outcomes in individuals exposed to TRIUMEQ during pregnancy. Healthcare providers are encouraged to register patients by calling the Antiretroviral Pregnancy Registry (APR) at 1‑800‑258‑4263.
Risk Summary
Data from two, ongoing birth outcome surveillance studies in Botswana and Eswatini which together include over 14,000 individuals evaluated during pregnancy show similar prevalence of neural tube defects among infants born to individuals taking dolutegravir at the time of conception compared to those born to individuals taking non-dolutegravir-containing regimens at conception or infants born to HIV-negative individuals (see Data).
There are insufficient human data on the use of TRIUMEQ during pregnancy to definitively assess a drug-associated risk for birth defects and miscarriage. However, available human data from the APR with the individual components of TRIUMEQ do not indicate an increased risk of birth defects (see Data). The background risk for major birth defects for the indicated population is unknown. In the U.S. general population, the estimated background rate for major birth defects and miscarriage in clinically recognized pregnancies is 2% to 4% and 15% to 20%, respectively.
In animal reproduction studies, no evidence of adverse developmental outcomes (including neural tube defects) was observed with dolutegravir at systemic exposures (AUC) less than (rabbits) and approximately 50 times (rats) the exposure in humans at the recommended human dose (RHD) (see Data). Oral administration of abacavir to pregnant rats during organogenesis resulted in fetal malformations and other embryonic and fetal toxicities at exposures 35 times the human exposure (AUC) at the RHD. No adverse developmental effects were observed following oral administration of abacavir to pregnant rabbits during organogenesis at exposures approximately 9 times the human exposure (AUC) at the RHD. Oral administration of lamivudine to pregnant rabbits during organogenesis resulted in embryolethality at a human exposure (AUC) similar to the RHD; however, no adverse development effects were observed with oral administration of lamivudine to pregnant rats during organogenesis at plasma concentrations (Cmax) 35 times the RHD (see Data).
Data
Human Data:
Dolutegravir:
Observational studies: The first interim analysis from an ongoing birth outcome surveillance study in Botswana identified an association between dolutegravir and an increased risk of neural tube defects when dolutegravir was administered at the time of conception and in early pregnancy. A subsequent analysis was conducted based on a larger cohort from the birth outcome surveillance study in Botswana and included over 9,460 individuals exposed to dolutegravir at conception, 23,664 individuals exposed to non-dolutegravir-containing regimens, and 170,723 HIV-negative pregnant individuals. The prevalence of neural tube defects in infants delivered to individuals taking dolutegravir at conception was 0.11% (95% CI: 0.05-0.19%). The observed prevalence rate did not differ significantly from that of infants delivered to individuals taking non-dolutegravir-containing regimens (0.11%, 95% CI: 0.07-0.16%), or to HIV-negative individuals (0.06%, 95% CI: 0.05-0.08%).
The Eswatini birth outcome surveillance study includes 9,743 individuals exposed to dolutegravir at conception, 1,838 individuals exposed to non-dolutegravir-containing regimens, and 32,259 HIV-negative pregnant individuals. The prevalence of neural tube defects in infants delivered to individuals taking dolutegravir at conception was 0.08% (95% CI: 0.04-0.16%). The observed prevalence rate did not differ significantly from that of infants delivered to individuals taking non-dolutegravir-containing regimens (0.22%, 95% CI: 0.06-0.56%) or to HIV-negative individuals (0.08%, 95% CI: 0.06-0.12%). The observed prevalence of neural tube defects in infants delivered to individuals taking non-dolutegravir-containing regimens had a wide confidence interval due to low sample size.
Limitations of these birth outcome surveillance studies include insufficient data to determine if baseline characteristics were balanced between the study groups or to assess other factors such as the use of folic acid during the preconception or first trimester periods.
Antiretroviral Pregnancy Registry: Based on prospective reports to the APR, of over 1,300 exposures to dolutegravir during pregnancy resulting in live births (including 874 exposed in the first trimester), the prevalence of defects in live births was 3.3% (95% CI: 2.2% to 4.7%) following first-trimester exposure to dolutegravir-containing regimens and 5.0% (95% CI: 3.2% to 7.3%) following second-/third-trimester exposure to dolutegravir-containing regimens. In the U.S. reference population of the Metropolitan Atlanta Congenital Defects Program (MACDP), the background birth defect rate was 2.7%.
Dolutegravir has been shown to cross the placenta. In a clinical trial in Uganda and South Africa in women during the last trimester of pregnancy receiving dolutegravir 50 mg once daily, the ratio of median dolutegravir concentration in fetal umbilical cord to that in maternal peripheral plasma was 1.21 (range 0.51-2.11) (n = 15).
Abacavir: Based on prospective reports to the APR of over 2,800 exposures to abacavir during pregnancy resulting in live births (including 1,455 exposed in the first trimester), there was no difference between the overall risk of birth defects for abacavir compared with the background birth defect rate of 2.7% in the U.S. reference population of the MACDP. The prevalence of defects in live births was 3.2% (95% CI: 2.4% to 4.3%) following first trimester exposure to abacavir-containing regimens and 3.0% (95% CI: 2.2% to 4.1%) following second/third trimester exposure to abacavir-containing regimens.
Abacavir has been shown to cross the placenta and concentrations in neonatal plasma at birth were essentially equal to those in maternal plasma at delivery [see Clinical Pharmacology (12.3)].
Lamivudine: Based on prospective reports to the APR of over 13,000 exposures to lamivudine during pregnancy resulting in live births (including 5,613 exposed in the first trimester), there was no difference between the overall risk of birth defects for lamivudine compared with the background birth defect rate of 2.7% in the U.S. reference population of the MACDP. The prevalence of birth defects in live births was 3.1% (95% CI: 2.6% to 3.6%) following first trimester exposure to lamivudine-containing regimens and 2.9% (95% CI: 2.5%, 3.3%) following second/third trimester exposure to lamivudine-containing regimens.
Lamivudine pharmacokinetics were studied in pregnant women during 2 clinical trials conducted in South Africa. The trials assessed pharmacokinetics in 16 women at 36 weeks’ gestation using 150 mg lamivudine twice daily with zidovudine, 10 women at 38 weeks’ gestation using 150 mg lamivudine twice daily with zidovudine, and 10 women at 38 weeks’ gestation using lamivudine 300 mg twice daily without other antiretrovirals. These trials were not designed or powered to provide efficacy information. Lamivudine concentrations were generally similar in maternal, neonatal, and umbilical cord serum samples. In a subset of subjects, amniotic fluid specimens were collected following natural rupture of membranes and confirmed that lamivudine crosses the placenta in humans. Based on limited data at delivery, median (range) amniotic fluid concentrations of lamivudine were 3.9-fold (1.2- to 12.8-fold) greater compared with paired maternal serum concentration (n = 8).
Animal Data:
Dolutegravir: Dolutegravir was administered orally to pregnant rats and rabbits (up to 1,000 mg/kg/day) on Gestation Days 6 to 17 and 6 to 18, respectively, and to rats on Gestation Day 6 to lactation/post-partum Day 20. No adverse effects on embryo-fetal (rats and rabbits) or pre/post-natal (rats) development were observed up to the highest dose tested. During organogenesis, systemic exposures (AUC) to dolutegravir in rabbits were less than the exposure in humans at the RHD and in rats were approximately 50 times the exposure in humans at the RHD. In the rat pre/post-natal development study, decreased body weight of the developing offspring was observed during lactation at a maternally toxic dose (approximately 50 times human exposure at the RHD).
Abacavir: Abacavir was administered orally to pregnant rats (at 100, 300, and 1,000 mg/kg/day) and rabbits (at 125, 350, or 700 mg/kg/day) during organogenesis (on Gestation Days 6 through 17 and 6 through 20, respectively). Fetal malformations (increased incidences of fetal anasarca and skeletal malformations) or developmental toxicity (decreased fetal body weight and crown‑rump length) were observed in rats at doses up to 1,000 mg/kg/day, resulting in exposures approximately 35 times the human exposure (AUC) at the RHD. No developmental effects were observed in rats at 100 mg/kg/day, resulting in exposures (AUC) 3.5 times the human exposure at the recommended daily dose. In a fertility and early embryo-fetal development study conducted in rats (at 60, 160, or 500 mg/kg/day), embryonic and fetal toxicities (increased resorptions, decreased fetal body weights) or toxicities to the offspring (increased incidence of stillbirth and lower body weights) occurred at doses up to 500 mg/kg/day. No developmental effects were observed in rats at 60 mg/kg/day, resulting in exposures (AUC) approximately 4 times the human exposure at the RHD. Studies in pregnant rats showed that abacavir is transferred to the fetus through the placenta. In pregnant rabbits, no developmental toxicities and no increases in fetal malformations occurred at up to the highest dose evaluated, resulting in exposures (AUC) approximately 9 times the human exposure at the RHD.
Lamivudine: Lamivudine was administered orally to pregnant rats (at 90, 600, and 4,000 mg/kg/day) and rabbits (at 90, 300 and 1,000 mg/kg/day and at 15, 40, and 90 mg/kg/day) during organogenesis (on Gestation Days 7 through 16 [rat] and 8 through 20 [rabbit]). No evidence of fetal malformations due to lamivudine was observed in rats and rabbits at doses producing plasma concentrations (Cmax) approximately 35 times higher than human exposure at the recommended daily dose. Evidence of early embryolethality was seen in the rabbit at systemic exposures (AUC) similar to those observed in humans, but there was no indication of this effect in the rat at plasma concentrations (Cmax) 35 times higher than human exposure at the recommended daily dose. Studies in pregnant rats showed that lamivudine is transferred to the fetus through the placenta. In the fertility/pre- and postnatal development study in rats, lamivudine was administered orally at doses of 180, 900, and 4,000 mg/kg/day (from prior to mating through postnatal Day 20). In the study, development of the offspring, including fertility and reproductive performance, were not affected by the maternal administration of lamivudine.
8.2 Lactation
Risk Summary
Abacavir, dolutegravir and lamivudine are present in human milk. There is no information on the effects of TRIUMEQ or its components on the breastfed infant or the effects of the drug on milk production.
Potential risks of breastfeeding include: (1) HIV‑1 transmission (in HIV-1–negative infants), (2) developing viral resistance (in HIV-1–positive infants), and (3) adverse reactions in a breastfed infant similar to those seen in adults.
8.4 Pediatric Use
The clinical data supporting use of TRIUMEQ and TRIUMEQ PD in pediatric patients with HIV-1 infection aged at least 3 months old weighing at least 6 kg is derived from the following previously conducted pediatric trials using TRIUMEQ and TRIUMEQ PD or the individual components:
- •
- The safety, pharmacokinetics, and antiviral activity (efficacy) of TRIUMEQ and TRIUMEQ PD were established through an open-label, multicenter clinical trial (IMPAACT 2019), in which HIV-1–infected, treatment-naïve, or treatment-experienced, pediatric subjects younger than 12 years and weighing at least 6 kg to less than 40 kg were treated with TRIUMEQ or TRIUMEQ PD [see Adverse Reactions (6.1), Clinical Pharmacology (12.3), Clinical Studies (14.2)].
- •
- The safety and efficacy of once-daily abacavir and lamivudine were established with a randomized, multicenter trial (ARROW [COL105677]) in HIV-1–infected, treatment-naive subjects aged 3 months to 17 years with a first-line regimen containing abacavir and lamivudine, using either the combination of EPIVIR and ZIAGEN or EPZICOM [see Adverse Reactions (6.1), Clinical Studies (14.2)].
- •
- The safety, pharmacokinetics, and antiviral activity (efficacy) of TIVICAY and TIVICAY PD were established through an ongoing, open-label, multicenter, dose-finding clinical trial (IMPAACT P1093), in which HIV-1–infected, treatment-naive or treatment-experienced, INSTI-naive, pediatric and adolescent subjects aged 4 weeks to <18 years and weighing at least 3 kg were treated with TIVICAY or TIVICAY PD plus optimized background therapy [see Adverse Reactions (6.1), Clinical Pharmacology (12.3), Clinical Studies (14.2)].
- •
- Additional pharmacokinetics data were evaluated in 2 pharmacokinetic substudies in ODYSSEY, an ongoing open-label, randomized, non-inferiority trial to evaluate the safety, efficacy, and pharmacokinetic parameters of TIVICAY or TIVICAY PD plus two nucleoside reverse transcriptase inhibitors (NRTIs) (mainly abacavir and lamivudine) compared with standard of care in HIV-1–infected pediatric subjects younger than 18 years [see Clinical Pharmacology (12.3)].
Overall, the safety, and efficacy profile of TRIUMEQ and TRIUMEQ PD in pediatric patients is comparable to that observed in adults. There are no data available on the use of lamivudine in pediatric patients with renal impairment [see Dosage and Administration (2.7), Warnings and Precautions (5.3), Adverse Reactions (6.1), Use in Specific Populations (8.6), Clinical Pharmacology (12.3), Clinical Studies (14.2)].
The safety and effectiveness of TRIUMEQ PD have not been established in pediatric patients aged less than 3 months or weighing less than 6 kg.
8.5 Geriatric Use
Clinical trials of abacavir, dolutegravir, or lamivudine did not include sufficient numbers of subjects aged 65 and over to determine whether they respond differently from younger subjects. In general, caution should be exercised in the administration of TRIUMEQ in elderly patients reflecting the greater frequency of decreased hepatic, renal, or cardiac function, and of concomitant disease or other drug therapy [see Clinical Pharmacology (12.3)].
8.6 Patients with Impaired Renal Function
TRIUMEQ and TRIUMEQ PD are not recommended for patients with creatinine clearance <30 mL/min and pediatric patients with a similar degree of renal impairment based on age-appropriate assessment of renal function because TRIUMEQ and TRIUMEQ PD are fixed-dose combinations, and the dosage of the individual components cannot be adjusted. If a dose reduction of lamivudine, a component of TRIUMEQ and TRIUMEQ PD, is required for patients with creatinine clearance <30 mL/min and in pediatric patients with a similar degree of renal impairment based on age-appropriate assessment of renal function, then the individual components should be used [see Clinical Pharmacology (12.3)].
Patients with a creatinine clearance between 30 and 49 mL/min receiving TRIUMEQ may experience a 1.6- to 3.3-fold higher lamivudine exposure (AUC) than patients with a creatinine clearance ≥50 mL/min. There are no safety data from randomized, controlled trials comparing TRIUMEQ to the individual components in patients with a creatinine clearance between 30 and 49 mL/min who received dose-adjusted lamivudine. Additionally, there are no data available on the use of lamivudine in pediatric patients with renal impairment. In the original lamivudine registrational trials in combination with zidovudine, higher lamivudine exposures were associated with higher rates of hematologic toxicities (neutropenia and anemia), although discontinuations due to neutropenia or anemia each occurred in <1% of subjects.
Patients with a sustained creatinine clearance between 30 and 49 mL/min or pediatric patients with a similar degree of renal impairment based on an age-appropriate assessment of renal function who receive TRIUMEQ or TRIUMEQ PD should be monitored for hematologic toxicities. If new or worsening neutropenia or anemia develop, dose adjustment of lamivudine, per lamivudine prescribing information, is recommended. If lamivudine dose adjustment is indicated, TRIUMEQ or TRIUMEQ PD should be discontinued, and the individual components should be used to construct the treatment regimen.
8.7 Patients with Impaired Hepatic Function
TRIUMEQ and TRIUMEQ PD are fixed-dose combinations, and the dosage of the individual components cannot be adjusted. If a dose reduction of abacavir, a component of TRIUMEQ and TRIUMEQ PD, is required for patients with mild hepatic impairment (Child-Pugh Score A), then the individual components should be used [see Clinical Pharmacology (12.3)].
The safety, efficacy, and pharmacokinetic properties of abacavir have not been established in patients with moderate (Child-Pugh Score B) or severe (Child-Pugh Score C) hepatic impairment; therefore, TRIUMEQ and TRIUMEQ PD are contraindicated in these patients [see Contraindications (4)].
10. Overdosage
There is no known specific treatment for overdose with TRIUMEQ or TRIUMEQ PD. If overdose occurs, the patient should be monitored, and standard supportive treatment applied as required.
Dolutegravir
As dolutegravir is highly bound to plasma proteins, it is unlikely that it will be significantly removed by dialysis.
Abacavir
It is not known whether abacavir can be removed by peritoneal dialysis or hemodialysis.
Lamivudine
Because a negligible amount of lamivudine was removed via (4-hour) hemodialysis, continuous ambulatory peritoneal dialysis, and automated peritoneal dialysis, it is not known if continuous hemodialysis would provide clinical benefit in a lamivudine overdose event.
11. Triumeq Description
TRIUMEQ and TRIUMEQ PD
TRIUMEQ and TRIUMEQ PD contain an INSTI (dolutegravir) and 2 nucleoside analogues (abacavir and lamivudine) with inhibitory activity against HIV.
Each film-coated tablet of TRIUMEQ, for oral use, contains 600 mg of abacavir (present as 702 mg of abacavir sulfate), 50 mg of dolutegravir (present as 52.6 mg of dolutegravir sodium), and 300 mg of lamivudine. The inactive ingredients of TRIUMEQ tablets include D-mannitol, magnesium stearate, microcrystalline cellulose, povidone, and sodium starch glycolate. The tablet film‑coating contains the inactive ingredients iron oxide black, iron oxide red, macrogol/PEG, polyvinyl alcohol–part hydrolyzed, talc, and titanium oxide.
Each film-coated tablet of TRIUMEQ PD for oral suspension contains 60 mg of abacavir (present as 70.2 mg of abacavir sulfate), 5 mg of dolutegravir (present as 5.26 mg of dolutegravir sodium), and 30 mg of lamivudine. The inactive ingredients of TRIUMEQ PD tablets include acesulfame potassium, crospovidone, mannitol, microcrystalline cellulose, povidone K29/32, silicified microcrystalline cellulose, sodium starch glycolate, sodium stearyl fumarate, strawberry cream flavor and sucralose. The tablet film-coating contains the inactive ingredients: ferric oxide yellow, macrogol/PEG, polyvinyl alcohol-part hydrolyzed, talc and titanium dioxide.
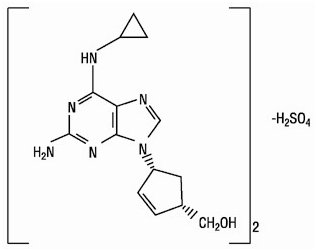
Abacavir Sulfate
The chemical name of abacavir sulfate is (1S,cis)-4-[2-amino-6-(cyclopropylamino)-9H-purin-9-yl]-2-cyclopentene-1-methanol sulfate (salt) (2:1). It has a molecular formula of (C14H18N6O)2•H2SO4 and a molecular weight of 670.76 g/mol. It has the following structural formula:
Abacavir sulfate is a white to off-white solid and is soluble in water.
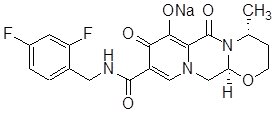
Dolutegravir Sodium
The chemical name of dolutegravir sodium is sodium (4R,12aS)-9-{[(2,4-difluorophenyl)methyl]carbamoyl}-4-methyl-6,8-dioxo-3,4,6,8,12,12a-hexahydro-2H-pyrido[1',2':4,5]pyrazino[2,1-b][1,3]oxazin-7-olate. The empirical formula is C20H18F2N3NaO5 and the molecular weight is 441.36 g/mol. It has the following structural formula:
Dolutegravir sodium is a white to light yellow powder and is slightly soluble in water.
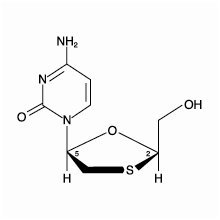
Lamivudine
The chemical name of lamivudine is (2R,cis)-4-amino-1-(2-hydroxymethyl-1,3-oxathiolan-5-yl)-(1H)-pyrimidin-2-one. Lamivudine is the (‑)enantiomer of a dideoxy analogue of cytidine. Lamivudine has also been referred to as (‑)2′,3′-dideoxy, 3′-thiacytidine. It has a molecular formula of C8H11N3O3S and a molecular weight of 229.3 g/mol. It has the following structural formula:
Lamivudine is a white to off-white crystalline solid and is soluble in water.
12. Triumeq - Clinical Pharmacology
12.1 Mechanism of Action
TRIUMEQ and TRIUMEQ PD are a fixed-dose combination of the HIV‑1 antiretroviral agents abacavir, dolutegravir, and lamivudine [see Microbiology (12.4)].
12.2 Pharmacodynamics
Effects on Electrocardiogram
A thorough QT trial has been conducted for dolutegravir. Neither the effects of abacavir nor lamivudine as single entities or the combination of abacavir, dolutegravir, and lamivudine on the QT interval have been evaluated.
In a randomized, placebo-controlled, cross-over trial, 42 healthy subjects received single-dose oral administrations of placebo, dolutegravir 250‑mg suspension (exposures approximately 3–fold of the 50-mg once-daily dose at steady state), and moxifloxacin 400 mg (active control) in random sequence. After baseline and placebo adjustment, the maximum mean QTc change based on Fridericia correction method (QTcF) for dolutegravir was 2.4 msec (1-sided 95% upper CI: 4.9 msec). Dolutegravir did not prolong the QTc interval over 24 hours postdose.
Effects on Renal Function
The effect of dolutegravir on renal function was evaluated in an open-label, randomized, 3-arm, parallel, placebo-controlled trial in healthy subjects (n = 37) who received dolutegravir 50 mg once daily (n = 12), dolutegravir 50 mg twice daily (n = 13), or placebo once daily (n = 12) for 14 days. A decrease in creatinine clearance, as determined by 24-hour urine collection, was observed with both doses of dolutegravir after 14 days of treatment in subjects who received 50 mg once daily (9% decrease) and 50 mg twice daily (13% decrease). Neither dose of dolutegravir had a significant effect on the actual glomerular filtration rate (determined by the clearance of probe drug, iohexol) or effective renal plasma flow (determined by the clearance of probe drug, para-amino hippurate) compared with the placebo.
12.3 Pharmacokinetics
Pharmacokinetics in Adults
One TRIUMEQ tablet was bioequivalent to one dolutegravir (TIVICAY) tablet (50 mg) plus one abacavir and lamivudine fixed-dose combination tablet (EPZICOM) under fasted conditions in healthy subjects (n = 62).
TRIUMEQ tablets and TRIUMEQ PD tablets for oral suspension are bioequivalent for the abacavir and lamivudine components, but not for the dolutegravir component. The relative dolutegravir bioavailability of TRIUMEQ PD is approximately 1.7-fold higher than TRIUMEQ; therefore, the 2 dosage forms are not substitutable on a milligram-per-milligram basis [see Dosage and Administration (2.3), Warnings and Precautions (5.7)]. The relative dolutegravir bioavailability is expected to be similar between TRIUMEQ PD and TIVICAY PD.
Abacavir: Following oral administration, abacavir is rapidly absorbed and extensively distributed. After oral administration of a single dose of 600 mg of abacavir in 20 subjects, Cmax was 4.26 ± 1.19 mcg/mL (mean ± SD) and AUC∞ was 11.95 ± 2.51 mcg•hour/mL. Binding of abacavir to human plasma proteins is approximately 50% and was independent of concentration. Total blood and plasma drug‑related radioactivity concentrations are identical, demonstrating that abacavir readily distributes into erythrocytes. The primary routes of elimination of abacavir are metabolism by alcohol dehydrogenase to form the 5′‑carboxylic acid and glucuronyl transferase to form the 5′‑glucuronide. In single-dose trials, the observed elimination half-life (t½) was 1.54 ± 0.63 hours. After intravenous administration, total clearance was 0.80 ± 0.24 L/h/kg (mean ± SD).
Dolutegravir: Following oral administration of dolutegravir, peak plasma concentrations were observed 2 to 3 hours postdose. With once-daily dosing, pharmacokinetic steady state is achieved within approximately 5 days with average accumulation ratios for AUC, Cmax, and C24 h ranging from 1.2 to 1.5. Dolutegravir is a P-gp substrate in vitro. The absolute bioavailability of dolutegravir has not been established. Dolutegravir is highly bound (≥98.9%) to human plasma proteins based on in vivo data and binding is independent of plasma concentration of dolutegravir. The apparent volume of distribution (Vd/F) following 50-mg once-daily administration is estimated at 17.4 L based on a population pharmacokinetic analysis.
Dolutegravir is primarily metabolized via UGT1A1 with some contribution from CYP3A. After a single oral dose of [14C] dolutegravir, 53% of the total oral dose is excreted unchanged in the feces. Thirty-one percent of the total oral dose is excreted in the urine, represented by an ether glucuronide of dolutegravir (18.9% of total dose), a metabolite formed by oxidation at the benzylic carbon (3.0% of total dose), and its hydrolytic N-dealkylation product (3.6% of total dose). Renal elimination of unchanged drug was <1% of the dose. Dolutegravir has a terminal half-life of approximately 14 hours and an apparent clearance (CL/F) of 1.0 L/h based on population pharmacokinetic analyses.
The pharmacokinetic properties of dolutegravir have been evaluated in healthy adult subjects and HIV‑1–infected adult subjects. Exposure to dolutegravir was generally similar between healthy subjects and HIV‑1–infected subjects.
|
Parameter |
50 mg Once Daily
|
|
AUC(0-24) (mcg•h/mL) |
53.6 (27) |
|
Cmax (mcg/mL) |
3.67 (20) |
|
Cmin (mcg/mL) |
1.11 (46) |
Cerebrospinal Fluid (CSF): In 11 treatment-naive subjects on dolutegravir 50 mg daily plus abacavir/lamivudine, the median dolutegravir concentration in CSF was 18 ng/mL (range: 4 ng/mL to 23.2 ng/mL) 2 to 6 hours postdose after 2 weeks of treatment. The clinical relevance of this finding has not been established.
Lamivudine: Following oral administration, lamivudine is rapidly absorbed and extensively distributed. After multiple‑dose oral administration of lamivudine 300 mg once daily for 7 days to 60 healthy subjects, steady-state Cmax (Cmax,ss) was 2.04 ± 0.54 mcg/mL (mean ± SD) and the 24‑hour steady‑state AUC (AUC24,ss) was 8.87 ± 1.83 mcg•hour/mL. Binding to plasma protein is low. Approximately 70% of an intravenous dose of lamivudine is recovered as unchanged drug in the urine. Metabolism of lamivudine is a minor route of elimination. In humans, the only known metabolite is the trans‑sulfoxide metabolite (approximately 5% of an oral dose after 12 hours). In most single-dose trials with plasma sampling up to 48 or 72 hours after dosing, the observed mean elimination half-life (t½) ranged from 13 to 19 hours. In HIV-1–infected subjects, total clearance was 398.5 ± 69.1 mL/min (mean ± SD).
Effect of Food on Oral Absorption
TRIUMEQ or TRIUMEQ PD may be taken with or without food. Overall, when compared with fasted conditions, administration of TRIUMEQ to healthy adult subjects with a high-fat meal (53% fat, 869 calories) resulted in decreased Cmax for abacavir and increased Cmax and AUC for dolutegravir. Lamivudine exposures were not affected by food. With a high-fat meal, the Cmax of abacavir decreased 23% and the Cmax and AUC of dolutegravir increased 37% and 48%, respectively. When compared with fasted conditions, administration of TRIUMEQ PD to healthy adult subjects with a high-fat meal (50% fat, 917 calories) resulted in decreased Cmax for abacavir (55%), dolutegravir (29%) and lamivudine (36%). AUCs for all 3 components were not affected by food.
Specific Populations
Patients with Renal Impairment: The pharmacokinetics for the individual components of TRIUMEQ and TRIUMEQ PD have been evaluated in patients with renal impairment (see the U.S. prescribing information for the individual abacavir, dolutegravir, and lamivudine components).
Patients with Hepatic Impairment: The pharmacokinetics for the individual components of TRIUMEQ and TRIUMEQ PD have been evaluated in patients with varying degrees of hepatic impairment (see the U.S. prescribing information for the individual abacavir, dolutegravir, and lamivudine components).
Pregnant women: Abacavir: Abacavir pharmacokinetics were studied in 25 pregnant women during the last trimester of pregnancy receiving abacavir 300 mg twice daily. Abacavir exposure (AUC) during pregnancy was similar to those in postpartum and in HIV-infected non-pregnant historical controls. Consistent with passive diffusion of abacavir across the placenta, abacavir concentrations in neonatal plasma cord samples at birth were essentially equal to those in maternal plasma at delivery.
Lamivudine: Lamivudine pharmacokinetics were studied in 36 pregnant women during 2 clinical trials conducted in South Africa. Lamivudine pharmacokinetics in pregnant women were similar to those seen in non-pregnant adults and in postpartum women. Lamivudine concentrations were generally similar in maternal, neonatal, and umbilical cord serum samples.
Pediatric Patients: The pharmacokinetics of TRIUMEQ, TRIUMEQ PD (abacavir, dolutegravir, and lamivudine) and their individual components have been evaluated in pediatric subjects.
Abacavir, Dolutegravir and Lamivudine: The pharmacokinetics of TRIUMEQ and TRIUMEQ PD were evaluated in the IMPAACT 2019 trial. Steady-state plasma exposure at doses by weight band are summarized in Table 8 [see Use in Specific Populations (8.4), Clinical Studies (14.2)].
Overall, exposures of abacavir, dolutegravir and lamivudine at the recommended doses for TRIUMEQ PD and TRIUMEQ are within the observed exposure ranges at the recommended doses of individual products in adults and pediatrics. Refer to the prescribing information for EPIVIR, TIVICAY, and ZIAGEN for pharmacokinetic information on lamivudine, dolutegravir, and abacavir, respectively, in pediatric patients.
| %CV, coefficient of variation expressed as a percentage. | ||||||||
| a The relative dolutegravir bioavailability of TRIUMEQ PD tablets for oral suspension is ~1.7-fold that of TRIUMEQ tablets. | ||||||||
|
Drug |
Weight Band |
Dosea of single entities in TRIUMEQ or TRIUMEQ PD |
n |
Pharmacokinetic Parameter Geometric Mean (%CV) |
||||
|
Cmax (mcg/mL) |
AUC0-24h (mcg∙h/mL) |
C24h (ng/mL) |
||||||
|
Abacavir |
6 to <10 kg |
180 mg once daily TRIUMEQ PD |
7 |
7.30 (20) |
17.7 (34) |
3 (128) |
||
|
10 to <14 kg |
240 mg once daily TRIUMEQ PD |
7 |
8.36 (44) |
19.8 (51) |
5 (127) |
|||
|
14 to <20 kg |
300 mg once daily TRIUMEQ PD |
7 |
6.26 (31) |
15.1 (40) |
3 (108) |
|||
|
20 to <25 kg |
360 mg once daily TRIUMEQ PD |
7 |
6.65 (28) |
17.4 (19) |
4 (85) |
|||
|
25 to <40 kg |
600 mg once daily TRIUMEQ |
7 |
9.04 (22) |
25.7 (15) |
11 (229) |
|||
|
Dolutegravir |
6 to <10 kg |
15 mg once daily TRIUMEQ PD |
7 |
7.40 (28) |
75.9 (34) |
910 (68) |
||
|
10 to <14 kg |
20 mg once daily TRIUMEQ PD |
7 |
8.85 (21) |
91.0 (36) |
1220 (77) |
|||
|
14 to <20 kg |
25 mg once daily TRIUMEQ PD |
7 |
7.04 (17) |
71.4 (23) |
790 (44) |
|||
|
20 to <25 kg |
30 mg once daily TRIUMEQ PD |
7 |
7.29 (17) |
84.4 (26) |
1350 (95) |
|||
|
25 to <40 kg |
50 mg once daily TRIUMEQ |
7 |
6.25 (21) |
71.8 (14) |
980 (28) |
|||
|
Lamivudine |
6 to <10 kg |
90 mg once daily TRIUMEQ PD |
7 |
2.29 (40) |
10.7 (46) |
55 (39) |
||
|
10 to <14 kg |
120 mg once daily TRIUMEQ PD |
7 |
3.55 (19) |
14.2 (24) |
46 (48) |
|||
|
14 to <20 kg |
150 mg once daily TRIUMEQ PD |
7 |
2.92 (23) |
13.0 (16) |
58 (37) |
|||
|
20 to <25 kg |
180 mg once daily TRIUMEQ PD |
7 |
2.99 (32) |
14.5 (17) |
60 (18) |
|||
|
25 to <40 kg |
300 mg once daily TRIUMEQ |
7 |
4.15 (29) |
21.7 (26) |
84 (35) |
|||
Geriatric Patients: Population analyses using pooled pharmacokinetic data from adult trials indicated age had no clinically relevant effect on the pharmacokinetics of dolutegravir. The pharmacokinetics of abacavir or lamivudine have not been studied in subjects older than 65 years.
Male and Female Patients: There are no significant or clinically relevant gender differences in the pharmacokinetics of the individual components (dolutegravir, abacavir, or lamivudine) based on the available information that was analyzed for each of the individual components.
Racial Groups: There are no significant or clinically relevant racial differences in pharmacokinetics of the individual components (dolutegravir, abacavir, or lamivudine) based on the available information that was analyzed for each of the individual components.
Drug Interaction Studies
The drug interaction trials described were conducted with dolutegravir, abacavir, and/or lamivudine as single entities; no drug interaction trials have been conducted using the combination of abacavir, dolutegravir, and lamivudine. No clinically significant drug interactions are expected between dolutegravir, abacavir, and lamivudine.
Dosing recommendations as a result of established and other potentially significant drug-drug interactions with the individual components of TRIUMEQ and TRIUMEQ PD are provided in Section 7.3 [see Drug Interactions (7)].
| a The number of subjects represents the maximum number of subjects that were evaluated. | ||||||||||||||
|
Coadministered Drug(s) and Dose(s) |
Dose of Dolutegravir |
n |
Geometric Mean Ratio (90% CI) of Pharmacokinetic Parameters of Coadministered Drug with/without Dolutegravir
|
|||||||||||
|
Cmax |
AUC |
Cτ or C24 |
||||||||||||
|
Ethinyl estradiol |
50 mg |
15 |
0.99 |
1.03 |
1.02 |
|||||||||
|
Metformin |
50 mg |
15a |
1.66 |
1.79 |
— |
|||||||||
|
Metformin |
50 mg |
15a |
2.11 |
2.45 |
— |
|||||||||
|
Methadone |
50 mg |
11 |
1.00 |
0.98 |
0.99 |
|||||||||
|
Midazolam |
25 mg |
10 |
— |
0.95 |
— |
|||||||||
|
Norelgestromin |
50 mg |
15 |
0.89 |
0.98 |
0.93 |
|||||||||
|
Rilpivirine |
50 mg |
16 |
1.10 |
1.06 |
1.21 |
|||||||||
|
Tenofovir disoproxil fumarate |
50 mg |
15 |
1.09 |
1.12 |
1.19 |
|||||||||
| a Comparison is rifampin taken with dolutegravir 50 mg twice daily compared with dolutegravir 50 mg twice daily. b Comparison is rifampin taken with dolutegravir 50 mg twice daily compared with dolutegravir 50 mg once daily. c The number of subjects represents the maximum number of subjects that were evaluated. |
||||||||||||||||||||
|
Coadministered Drug(s) and Dose(s) |
Dose of Dolutegravir |
n |
Geometric Mean Ratio (90% CI) of Dolutegravir Pharmacokinetic Parameters with/without Coadministered Drugs
|
|||||||||||||||||
|
Cmax |
AUC |
Cτ or C24 |
||||||||||||||||||
|
Atazanavir 400 mg once daily |
30 mg |
12 |
1.50 |
1.91 |
2.80 |
|||||||||||||||
|
Atazanavir/ritonavir 300/100 mg once daily |
30 mg |
12 |
1.34 |
1.62 |
2.21 |
|||||||||||||||
|
Darunavir/ritonavir 600/100 mg twice daily |
30 mg |
15 |
0.89 |
0.78 |
0.62 |
|||||||||||||||
|
Efavirenz 600 mg once daily |
50 mg |
12 |
0.61 |
0.43 |
0.25 |
|||||||||||||||
|
Etravirine 200 mg twice daily |
50 mg |
16 |
0.48 |
0.29 |
0.12 |
|||||||||||||||
|
Etravirine + darunavir/ritonavir 200 mg + 600/100 mg twice daily |
50 mg |
9 |
0.88 |
0.75 |
0.63 |
|||||||||||||||
|
Etravirine + lopinavir/ritonavir 200 mg + 400/100 mg twice daily |
50 mg |
8 |
1.07 |
1.11 |
1.28 |
|||||||||||||||
|
Fosamprenavir/ritonavir 700 mg/100 mg twice daily |
50 mg |
12 |
0.76 |
0.65 |
0.51 |
|||||||||||||||
|
Lopinavir/ritonavir 400/100 mg twice daily |
30 mg |
15 |
1.00 |
0.97 |
0.94 |
|||||||||||||||
|
Rilpivirine 25 mg once daily |
50 mg |
16 |
1.13 |
1.12 |
1.22 |
|||||||||||||||
|
Tenofovir 300 mg once daily |
50 mg |
15 |
0.97 |
1.01 |
0.92 (0.82 to 1.04) |
|||||||||||||||
|
Tipranavir/ritonavir 500/200 mg twice daily |
50 mg |
14 |
0.54 |
0.41 |
0.24 |
|||||||||||||||
|
Antacid (MAALOX) simultaneous administration |
50 mg |
16 |
0.28 |
0.26 |
0.26 |
|||||||||||||||
|
Antacid (MAALOX) 2 h after dolutegravir |
50 mg |
16 |
0.82 |
0.74 |
0.70 |
|||||||||||||||
|
Boceprevir 800 mg every 8 h |
50 mg |
13 |
1.05 |
1.07 |
1.08 |
|||||||||||||||
|
Calcium carbonate 1,200 mg simultaneous administration (fasted) |
50 mg |
12 |
0.63 |
0.61 |
0.61 |
|||||||||||||||
|
Calcium carbonate 1,200 mg simultaneous administration (fed) |
50 mg |
11 |
1.07 |
1.09 |
1.08 |
|||||||||||||||
|
Calcium carbonate 1,200 mg 2 h after dolutegravir |
50 mg |
11 |
1.00 |
0.94 |
0.90 |
|||||||||||||||
|
Carbamazepine 300 mg twice daily |
50 mg |
16c |
0.67 |
0.51 |
0.27 |
|||||||||||||||
|
Ferrous fumarate 324 mg simultaneous administration (fasted) |
50 mg |
11 |
0.43 |
0.46 |
0.44 |
|||||||||||||||
|
Ferrous fumarate 324 mg simultaneous administration (fed) |
50 mg |
11 |
1.03 |
0.98 |
1.00 |
|||||||||||||||
|
Ferrous fumarate 324 mg 2 h after dolutegravir |
50 mg |
10 |
0.99 |
0.95 |
0.92 |
|||||||||||||||
|
Multivitamin (One-A-Day) simultaneous administration |
50 mg |
16 |
0.65 |
0.67 |
0.68 |
|||||||||||||||
|
Omeprazole 40 mg once daily |
50 mg |
12 |
0.92 |
0.97 |
0.95 |
|||||||||||||||
|
Prednisone 60 mg once daily with taper |
50 mg |
12 |
1.06 |
1.11 |
1.17 |
|||||||||||||||
|
Rifampina 600 mg once daily |
50 mg |
11 |
0.57 |
0.46 |
0.28 |
|||||||||||||||
|
Rifampinb 600 mg once daily |
50 mg |
11 |
1.18 |
1.33 |
1.22 |
|||||||||||||||
|
Rifabutin 300 mg once daily |
50 mg |
9 |
1.16 |
0.95 |
0.70 |
|||||||||||||||
Abacavir or Lamivudine: The drug interactions described are based on trials conducted with abacavir or lamivudine as single entities.
Effect of Abacavir and Lamivudine on the Pharmacokinetics of Other Agents: In vitro studies have shown that abacavir has potential to inhibit CYP1A1 and limited potential to inhibit metabolism mediated by CYP3A4. Lamivudine does not inhibit or induce CYP3A4. Abacavir and lamivudine do not inhibit or induce other CYP enzymes (such as CYP2C9 or CYP2D6). Based on in vitro study results, abacavir and lamivudine at therapeutic drug exposures are not expected to affect the pharmacokinetics of drugs that are substrates of the following transporters: OATP1B1/3, BCRP or P-gp, OCT1, OCT2, OCT3 (lamivudine only), or MATE1 and MATE2‑K.
Abacavir, Dolutegravir, and Lamivudine: Coadministration of a single dose of riociguat (0.5 mg) to HIV-1–infected subjects receiving TRIUMEQ is reported to increase riociguat AUC(∞) compared with riociguat AUC(∞) reported in healthy subjects due to CYP1A1 inhibition by abacavir. The exact magnitude of increase in riociguat exposure has not been fully characterized based on findings from two studies [see Drug Interactions (7.3)].
Effect of Other Agents on the Pharmacokinetics of Abacavir or Lamivudine: In vitro, abacavir is not a substrate of OATP1B1, OATP1B3, OCT1, OCT2, OAT1, MATE1, MATE2-K, MRP2 or MRP4; therefore, drugs that modulate these transporters are not expected to affect abacavir plasma concentrations. Abacavir is a substrate of BCRP and P-gp in vitro; however, considering its absolute bioavailability (83%), modulators of these transporters are unlikely to result in a clinically relevant impact on abacavir concentrations.
Lamivudine is a substrate of MATE1, MATE2-K, and OCT2 in vitro. Trimethoprim (an inhibitor of these drug transporters) has been shown to increase lamivudine plasma concentrations. This interaction is not considered clinically significant as no dose adjustment of lamivudine is needed.
Lamivudine is a substrate of P-gp and BCRP; however, considering its absolute bioavailability (87%), it is unlikely that these transporters play a significant role in the absorption of lamivudine. Therefore, coadministration of drugs that are inhibitors of these efflux transporters is unlikely to affect the disposition and elimination of lamivudine.
Ethanol: Abacavir has no effect on the pharmacokinetic properties of ethanol. Ethanol decreases the elimination of abacavir causing an increase in overall exposure.
Interferon Alfa: There was no significant pharmacokinetic interaction between lamivudine and interferon alfa in a trial of 19 healthy male subjects.
Methadone: In a trial of 11 HIV‑1–infected subjects receiving methadone‑maintenance therapy (40 mg and 90 mg daily), with 600 mg of abacavir twice daily (twice the currently recommended dose), oral methadone clearance increased 22% (90% CI: 6% to 42%) [see Drug Interactions (7.3)]. The addition of methadone has no clinically significant effect on the pharmacokinetic properties of abacavir.
Ribavirin: In vitro data indicate ribavirin reduces phosphorylation of lamivudine, stavudine, and zidovudine. However, no pharmacokinetic (e.g., plasma concentrations or intracellular triphosphorylated active metabolite concentrations) or pharmacodynamic (e.g., loss of HIV‑1/HCV [hepatitis C virus] virologic suppression) interaction was observed when ribavirin and lamivudine (n = 18), stavudine (n = 10), or zidovudine (n = 6) were coadministered as part of a multi‑drug regimen to HIV‑1/HCV co‑infected subjects.
Sorbitol (Excipient): Lamivudine and sorbitol solutions were coadministered to 16 healthy adult subjects in an open-label, randomized-sequence, 4-period, crossover trial. Each subject received a single 300-mg dose of lamivudine oral solution alone or coadministered with a single dose of 3.2 g, 10.2 g, or 13.4 g of sorbitol in solution. Coadministration of lamivudine with sorbitol resulted in dose-dependent decreases of 20%, 39%, and 44% in the AUC(0-24); 14%, 32%, and 36% in the AUC(∞); and 28%, 52%, and 55% in the Cmax; of lamivudine, respectively.
Abacavir, Lamivudine, Zidovudine: Fifteen HIV‑1–infected subjects were enrolled in a crossover-designed drug interaction trial evaluating single doses of abacavir (600 mg), lamivudine (150 mg), and zidovudine (300 mg) alone or in combination. Analysis showed no clinically relevant changes in the pharmacokinetics of abacavir with the addition of lamivudine or zidovudine or the combination of lamivudine and zidovudine. Lamivudine exposure (AUC decreased 15%) and zidovudine exposure (AUC increased 10%) did not show clinically relevant changes with concurrent abacavir.
Lamivudine and Zidovudine: No clinically significant alterations in lamivudine or zidovudine pharmacokinetics were observed in 12 asymptomatic HIV‑1–infected adult patients given a single dose of zidovudine (200 mg) in combination with multiple doses of lamivudine (300 mg every 12 hours).
The effects of other coadministered drugs on abacavir or lamivudine are provided in Table 11.
| ↑ = Increase; ↔ = No significant change. a The drug-drug interaction was only evaluated in males. |
||||||||||||||||||||||||||
|
Coadministered Drug and Dose |
Drug and Dose |
n |
Concentrations of Abacavir or Lamivudine |
Concentration of Coadministered Drug |
||||||||||||||||||||||
|
AUC |
Variability |
|||||||||||||||||||||||||
|
Ethanol 0.7 g/kg |
Abacavir Single 600 mg |
24 |
↑41% |
90% CI: 35% to 48% |
↔a |
|||||||||||||||||||||
|
Nelfinavir 750 mg every 8 h x 7 to 10 days |
Lamivudine Single 150 mg |
11 |
↑10% |
95% CI: 1% to 20% |
↔ |
|||||||||||||||||||||
|
Trimethoprim 160 mg/ Sulfamethoxazole 800 mg daily x 5 days |
Lamivudine Single 300 mg |
14 |
↑43% |
90% CI: 32% to 55% |
↔ |
|||||||||||||||||||||
12.4 Microbiology
Mechanism of Action
Dolutegravir: Dolutegravir inhibits HIV integrase by binding to the integrase active site and blocking the strand transfer step of retroviral DNA integration which is essential for the HIV replication cycle. Strand transfer biochemical assays using purified recombinant HIV‑1 integrase and pre-processed substrate DNA resulted in IC50 values of 2.7 nM and 12.6 nM.
Abacavir: Abacavir is a carbocyclic synthetic nucleoside analogue. Abacavir is converted by cellular enzymes to the active metabolite, carbovir triphosphate (CBV‑TP), an analogue of deoxyguanosine‑5′‑triphosphate (dGTP). CBV‑TP inhibits the activity of HIV‑1 reverse transcriptase (RT) both by competing with the natural substrate dGTP and by its incorporation into viral DNA.
Lamivudine: Lamivudine is a synthetic nucleoside analogue. Intracellularly lamivudine is phosphorylated to its active 5′-triphosphate metabolite, lamivudine triphosphate (3TC‑TP). The principal mode of action of 3TC‑TP is inhibition of RT via DNA chain termination after incorporation of the nucleotide analogue.
Antiviral Activity in Cell Culture
Dolutegravir: Dolutegravir exhibited antiviral activity against laboratory strains of wild-type HIV‑1 with mean concentration of drug necessary to affect viral replication by 50% (EC50) values of 0.5 nM (0.21 ng/mL) to 2.1 nM (0.85 ng/mL) in peripheral blood mononuclear cells (PBMCs) and MT-4 cells. Dolutegravir exhibited antiviral activity against 13 clinically diverse clade B isolates with a median EC50 value of 0.54 nM (range: 0.41 to 0.60 nM) in a viral susceptibility assay using the integrase coding region from clinical isolates. Dolutegravir demonstrated antiviral activity in cell culture against a panel of HIV‑1 clinical isolates with median EC50 values of 0.18 nM (n = 3, range: 0.09 to 0.5 nM), 0.08 nM (n = 5, range: 0.05 to 2.14 nM), 0.12 nM (n = 4, range: 0.05 to 0.51 nM), 0.17 nM (n = 3, range: 0.16 to 0.35 nM), 0.24 nM (n = 3, range: 0.09 to 0.32 nM), 0.17 nM (n = 4, range: 0.07 to 0.44 nM), 0.2 nM (n = 3, range: 0.02 to 0.87 nM), and 0.42 nM (n = 3, range: 0.41 to 1.79 nM) for clades A, B, C, D, E, F, and G, and group O viruses, respectively. Dolutegravir EC50 values against three HIV-2 clinical isolates in PBMC assays ranged from 0.09 nM to 0.61 nM.
Abacavir: The antiviral activity of abacavir against HIV‑1 was assessed in a number of cell lines including in primary monocytes/macrophages and PBMCs. EC50 values ranged from 3,700 to 5,800 nM (1 nM = 0.28 ng/mL) and 70 to 1,000 nM against HIV‑1IIIB and HIV‑1BaL, respectively, and the mean EC50 value was 260 ± 180 nM against 8 clinical isolates. The median EC50 values of abacavir were 344 nM (range: 14.8 to 676 nM), 16.9 nM (range: 5.9 to 27.9 nM), 8.1 nM (range: 1.5 to 16.7 nM), 356 nM (range: 35.7 to 396 nM), 105 nM (range: 28.1 to 168 nM), 47.6 nM (range: 5.2 to 200 nM), 51.4 nM (range: 7.1 to 177 nM), and 282 nM (range: 22.4 to 598 nM) against HIV‑1 clades A-G and group O viruses (n = 3 except n = 2 for clade B), respectively. The EC50 values against HIV‑2 isolates (n = 4), ranged from 24 to 490 nM.
Lamivudine: The antiviral activity of lamivudine against HIV‑1 was assessed in a number of cell lines including monocytes and PBMCs using standard susceptibility assays. EC50 values were in the range of 3 to 15,000 nM (1 nM = 0.23 ng/mL). The median EC50 values of lamivudine were 60 nM (range: 20 to 70 nM), 35 nM (range: 30 to 40 nM), 30 nM (range: 20 to 90 nM), 20 nM (range: 3 to 40 nM), 30 nM (range: 1 to 60 nM), 30 nM (range: 20 to 70 nM), 30 nM (range: 3 to 70 nM), and 30 nM (range: 20 to 90 nM) against HIV‑1 clades A-G and group O viruses (n = 3 except n = 2 for clade B) respectively. The EC50 values against HIV‑2 isolates (n = 4) from 3 to 120 nM in PBMCs. Ribavirin (50,000 nM) used in the treatment of chronic HCV infection decreased the anti-HIV‑1 activity of lamivudine by 3.5‑fold in MT‑4 cells.
Antiviral Activity in Combination with Other Antiviral Agents
Neither dolutegravir, abacavir, nor lamivudine were antagonistic to all tested anti-HIV agents. See full prescribing information for ZIAGEN (abacavir), TIVICAY (dolutegravir), and EPIVIR (lamivudine).
Resistance in Cell Culture
Dolutegravir: Dolutegravir-resistant viruses were selected in cell culture starting from different wild-type HIV‑1 strains and clades. Amino acid substitutions E92Q, G118R, S153F or Y, G193E or R263K emerged in different passages and conferred decreased susceptibility to dolutegravir of up to 4-fold.
Abacavir and Lamivudine: HIV-1 isolates with reduced susceptibility to the combination of abacavir and lamivudine have been selected in cell culture with amino acid substitutions K65R, L74V, Y115F, and M184V/I in HIV-1 RT. M184V or I substitutions resulted in high-level resistance to lamivudine and approximately 2-fold decrease in susceptibility to abacavir. Substitutions K65R, L74V, or Y115F with M184V or I conferred a 7- to 8-fold reduction in abacavir susceptibility, and combinations of three substitutions were required to confer more than an 8-fold reduction in susceptibility.
Resistance in Clinical Subjects
No subjects in the treatment arm receiving dolutegravir + EPZICOM in SINGLE (treatment- naive trial) had a detectable decrease in susceptibility to dolutegravir or background NRTIs in the resistance analysis subset (n = 11 with HIV-1 RNA >400 copies/mL at failure or last visit and having resistance data). Two virologic failure subjects in SINGLE had treatment-emergent G/D/E193D and G193G/E integrase substitutions at Week 84 and Week 108, respectively, and 1 subject with 275 copies/mL HIV-1 RNA had a treatment-emergent Q157Q/P integrase substitution detected at Week 24. None of these subjects had a corresponding decrease in dolutegravir susceptibility. No treatment-emergent genotypic resistance to abacavir and lamivudine, components of TRIUMEQ and TRIUMEQ PD, was observed in the arm receiving dolutegravir + EPZICOM in the SINGLE trial through Week 144. One ART-naïve subject receiving TRIUMEQ PD in the pediatric IMPAACT 2019 trial experienced confirmed virologic failure at Week 24 but subsequently suppressed to 76 copies/mL by Week 48 while on continued study treatment. The subject’s entry specimen (HIV-1 subtype AE) had the presence of baseline integrase substitution L74I polymorphism. Genotypic sequencing and phenotypic analyses failed at the confirmed virologic failure timepoint for this subject.
Cross-Resistance
Dolutegravir: Cross-resistance has been observed among INSTIs. The single INSTI-resistance substitutions T66K, I151L, and S153Y conferred a >2-fold decrease in dolutegravir susceptibility (range: 2.3-fold to 3.6-fold from reference). Combinations of multiple substitutions T66K/L74M, E92Q/N155H, G140C/Q148R, G140S/Q148H, R or K, Q148R/N155H, T97A/G140S/Q148, and substitutions at E138/G140/Q148 showed a >2-fold decrease in dolutegravir susceptibility (range: 2.5-fold to 21-fold from reference). In HIV-2 mutants, combinations of substitutions A153G/N155H/S163G and E92Q/T97A/N155H/S163D conferred 4-fold decreases in dolutegravir susceptibility, and E92Q/N155H and G140S/Q148R showed 8.5-fold and 17-fold decreases in dolutegravir susceptibility, respectively.
Abacavir and Lamivudine: Cross‑resistance has been observed among NRTIs. The combination of abacavir/lamivudine has demonstrated decreased susceptibility to viruses with a K65R substitution with or without an M184V/I substitution, viruses with L74V plus the M184V/I substitution, and viruses with thymidine analog mutation (TAM) substitutions (M41L, D67N, K70R, L210W, T215Y/F, K219 E/R/H/Q/N) plus M184V. An increasing number of TAMs is associated with a progressive reduction in abacavir susceptibility.
13. Nonclinical Toxicology
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Carcinogenicity
Dolutegravir: Two-year carcinogenicity studies in mice and rats were conducted with dolutegravir. Mice were administered doses of up to 500 mg/kg, and rats were administered doses of up to 50 mg/kg. In mice, no significant increases in the incidence of drug-related neoplasms were observed at the highest doses tested, resulting in dolutegravir AUC exposures approximately 26-fold higher than those in humans at the recommended dose of 50 mg once daily. In rats, no increases in the incidence of drug-related neoplasms were observed at the highest dose tested, resulting in dolutegravir AUC exposures 17-fold and 30-fold higher in males and females, respectively, than those in humans at the recommended dose of 50 mg once daily.
Abacavir: Abacavir was administered orally at 3 dosage levels to separate groups of mice and rats in 2‑year carcinogenicity studies. Results showed an increase in the incidence of malignant and non‑malignant tumors. Malignant tumors occurred in the preputial gland of males and the clitoral gland of females of both species, and in the liver of female rats. In addition, non‑malignant tumors also occurred in the liver and thyroid gland of female rats. These observations were made at systemic exposures in the range of 7 to 28 times the human exposure at the recommended dose of 600 mg.
Lamivudine: Long‑term carcinogenicity studies with lamivudine in mice and rats showed no evidence of carcinogenic potential at exposures up to 12 times (mice) and 57 times (rats) the human exposures at the recommended dose of 300 mg.
Mutagenicity
Dolutegravir: Dolutegravir was not genotoxic in the bacterial reverse mutation assay, mouse lymphoma assay, or in the in vivo rodent micronucleus assay.
Abacavir: Abacavir induced chromosomal aberrations both in the presence and absence of metabolic activation in an in vitro cytogenetic study in human lymphocytes. Abacavir was mutagenic in the absence of metabolic activation, although it was not mutagenic in the presence of metabolic activation in an L5178Y mouse lymphoma assay. Abacavir was clastogenic in males and not clastogenic in females in an in vivo mouse bone marrow micronucleus assay. Abacavir was not mutagenic in bacterial mutagenicity assays in the presence and absence of metabolic activation.
Lamivudine: Lamivudine was mutagenic in an L5178Y mouse lymphoma assay and clastogenic in a cytogenetic assay using cultured human lymphocytes. Lamivudine was not mutagenic in a microbial mutagenicity assay, in an in vitro cell transformation assay, in a rat micronucleus test, in a rat bone marrow cytogenetic assay, and in an assay for unscheduled DNA synthesis in rat liver.
Impairment of Fertility
Dolutegravir, abacavir, or lamivudine did not affect male or female fertility in rats at doses associated with exposures approximately 44, 9, or 112 times (respectively) higher than the exposures in humans at the doses of 50 mg, 600 mg, and 300 mg (respectively).
13.2 Animal Toxicology and/or Pharmacology
Myocardial degeneration was found in mice and rats following administration of abacavir for 2 years. The systemic exposures were equivalent to 7 to 21 times the expected systemic exposure in humans at a dose of 600 mg. The clinical relevance of this finding has not been determined.
14. Clinical Studies
14.1 Adult Subjects
The efficacy of TRIUMEQ is supported by data from a randomized, controlled trial (double-blind through 96 weeks and open-label phase from 96 to 144 weeks) in antiretroviral treatment-naive subjects, SINGLE (ING114467, NCT01263015) and other trials in treatment-naive subjects. See full prescribing information for TIVICAY. The efficacy of dolutegravir, in combination with at least two active background regimens in treatment-experienced, INSTI- naive subjects is supported by data from SAILING (ING111762, NCT01231516) (refer to the prescribing information for TIVICAY).
Treatment-Naive Subjects
In SINGLE, 833 subjects were randomized and received at least 1 dose of either TIVICAY 50 mg once daily with fixed-dose abacavir and lamivudine (EPZICOM) or fixed-dose efavirenz/emtricitabine/tenofovir disoproxil fumarate (ATRIPLA). At baseline, the median age of subjects was 35 years, 16% female, 32% non-white, 7% had hepatitis C co-infection (hepatitis B virus co-infection was excluded), 4% were CDC Class C (AIDS), 32% had HIV‑1 RNA >100,000 copies/mL, and 53% had CD4+ cell count <350 cells/mm3; these characteristics were similar between treatment groups.
Week 144 (open-label-phase analysis which followed the Week 96 double-blind phase) outcomes for SINGLE are provided in Table 12.
| a Adjusted for pre-specified stratification factors. b Includes subjects who discontinued due to an adverse event or death at any time point if this resulted in no virologic data on treatment during the analysis window. c Other includes reasons such as withdrew consent, loss to follow-up, moved, and protocol deviation. d The primary endpoint was assessed at Week 48 and the virologic success rate was 88% in the group receiving TIVICAY and 81% in the ATRIPLA group, with a treatment difference of 7.4% and 95% CI of (2.5%, 12.3%). |
||
|
TIVICAY + EPZICOM Once Daily (n = 414) |
ATRIPLA Once Daily (n = 419) |
|
|
HIV‑1 RNA <50 copies/mL |
71% |
63% |
|
Treatment differencea |
8.3% (95% CI: 2.0%, 14.6%)d |
|
|
Virologic nonresponse |
10% |
7% |
|
Data in window not <50 copies/mL |
4% |
<1% |
|
Discontinued for lack of efficacy |
3% |
3% |
|
Discontinued for other reasons while not suppressed |
3% |
4% |
|
No virologic data |
18% |
30% |
|
Reasons | ||
|
Discontinued study/study drug due to adverse event or deathb |
4% |
14% |
|
Discontinued study/study drug for other reasonsc |
12% |
13% |
|
Missing data during window but on study |
2% |
3% |
|
Proportion (%) of Subjects with HIV‑1 RNA <50 copies/mL by Baseline Category |
||
|
Plasma viral load (copies/mL) | ||
|
≤100,000 |
73% |
64% |
|
≥100,000 |
69% |
61% |
|
Gender | ||
|
Male |
72% |
66% |
|
Female |
69% |
48% |
|
Race | ||
|
White |
72% |
71% |
|
African American/African Heritage/Other |
71% |
47% |
Treatment differences were maintained across baseline characteristics including baseline viral load, CD4+ cell count, age, gender, and race. The adjusted mean changes in CD4+ cell counts from baseline were 378 cells/mm3 in the group receiving TIVICAY + EPZICOM and 332 cells/mm3 for the ATRIPLA group at 144 weeks. The adjusted difference between treatment arms and 95% CI was 46.9 cells/mm3 (15.6 cells/mm3, 78.2 cells/mm3) (adjusted for pre-specified stratification factors: baseline HIV‑1 RNA, and baseline CD4+ cell count).
Treatment-Experienced
In SAILING, there were 715 subjects included in the efficacy and safety analyses (see full prescribing information for TIVICAY). At Week 48, 71% of subjects randomized to TIVICAY plus background regimen versus 64% of subjects randomized to raltegravir plus background regimen had HIV‑1 RNA <50 copies/mL (treatment difference and 95% CI: 7.4% [0.7%, 14.2%]).
14.2 Pediatric Subjects
The efficacy of TRIUMEQ, TRIUMEQ PD and/or their individual components for the treatment of HIV-1 infection was evaluated in pediatric patients enrolled in the IMPAACT 2019 trial (NCT03760458), ARROW trial (NCT02028676) and IMPAACT P1093 trial (NCT01302847), as summarized below.
- •
- TRIUMEQ and TRIUMEQ PD were evaluated in treatment-naive or treatment-experienced, HIV-1–infected subjects younger than 12 years in an open-label, multicenter clinical trial (IMPAACT 2019). Subjects were stratified by weight band and enrolled in one of five groups. Fifty-seven subjects, with a median age of 6.4 years (range: 1 to 11.3) and median weight of 17 kg (range: 8.2 to 39.3), received the recommended dose (determined by weight) and formulation, and contributed to the efficacy analysis at Week 48. At this timepoint, 79% of subjects achieved HIV-1 RNA less than 50 copies/mL and 95% achieved HIV-1 RNA less than 200 copies/mL (Snapshot algorithm).
- •
- Abacavir and lamivudine once daily, in combination with a third antiretroviral drug, were evaluated in a randomized, multicenter trial (ARROW) in treatment-naive pediatric subjects with HIV-1 infection. Subjects randomized to once-daily dosing (n = 336) and who weighed at least 25 kg received abacavir 600 mg and lamivudine 300 mg, as either the single entities or as EPZICOM. At Week 96, 67% of subjects receiving abacavir and lamivudine once-daily in combination with a third antiretroviral drug, had HIV-1 RNA <80 copies/mL.
- •
- Dolutegravir (TIVICAY or TIVICAY PD), in combination with other antiretroviral drugs, was evaluated in treatment-naive or treatment-experienced, INSTI-naive, HIV-1–infected subjects aged at least 4 weeks to 18 years in an ongoing open-label, multicenter, dose-finding clinical trial, IMPAACT P1093. Subjects were stratified by age from 4 weeks to younger than 18 years and enrolled in one of five age cohorts. Thirty-six subjects weighing at least 6 kg who received the recommended dose (determined by weight and age) and formulation contributed to the efficacy analysis at Week 48. At this timepoint, 72% (26/36) of subjects weighing at least 6 kg achieved HIV‑1 RNA <50 copies/mL (Snapshot algorithm).
16. How is Triumeq supplied
TRIUMEQ tablets
TRIUMEQ tablets are purple, oval, film-coated, biconvex tablets debossed with “572 Tri” on one side and contain 600 mg of abacavir (as abacavir sulfate), 50 mg of dolutegravir (as dolutegravir sodium), and 300 mg lamivudine.
Bottle of 30 tablets with desiccant and child-resistant closure. NDC 49702-231-13.
Store and dispense in the original package, protect from moisture, and keep the bottle tightly closed. Do not remove desiccant.
Store at 20°C to 25°C (68°F to 77°F); excursions permitted between 15°C and 30°C (59°F to 86°F). [See USP Controlled Room Temperature].
TRIUMEQ PD tablets for oral suspension
TRIUMEQ PD tablets for oral suspension, are yellow, capsule-shaped, strawberry cream flavored, film-coated, biconvex tablets debossed with “SV WTU” on one side and contain 60 mg of abacavir (as abacavir sulfate), 5 mg of dolutegravir (as dolutegravir sodium), and 30 mg lamivudine.
Bottle of 90 tablets (NDC 49702-272-59) with desiccant and child-resistant closure. Each bottle is packaged as a kit (NDC 49702-258-37) with one 40-mL dosing cup.
Store at 20°C to 25°C (68°F to 77°F); excursions permitted between 15°C and 30°C (59°F to 86°F). [See USP Controlled Room Temperature]. Store and dispense in the original bottle, protect from moisture, and keep the bottle tightly closed. Do not remove desiccant.
17. Patient Counseling Information
Advise the patient to read the FDA-approved patient labeling (Medication Guide and Instructions for Use).
Drug Interactions
TRIUMEQ or TRIUMEQ PD may interact with many drugs; therefore, advise patients to report to their healthcare provider the use of any other prescription or nonprescription medication or herbal products, including St. John’s wort [see Contraindications (4), Warnings and Precautions (5.5), Drug Interactions (7)].
Hypersensitivity Reaction
Inform patients:
- •
- that a Medication Guide and Warning Card summarizing the symptoms of the abacavir hypersensitivity reaction and other product information will be dispensed by the pharmacist with each new prescription and refill of TRIUMEQ or TRIUMEQ PD, and instruct the patient to read the Medication Guide and Warning Card every time to obtain any new information that may be present about TRIUMEQ or TRIUMEQ PD. The complete text of the Medication Guide is reprinted at the end of this document.
- •
- to carry the Warning Card with them.
- •
- how to identify a hypersensitivity reaction [see Warnings and Precautions (5.1), Medication Guide].
- •
- that if they develop symptoms consistent with a hypersensitivity reaction they should call their healthcare provider right away to determine if they should stop taking TRIUMEQ or TRIUMEQ PD.
- •
- that a hypersensitivity reaction can worsen and lead to hospitalization or death if TRIUMEQ or TRIUMEQ PD is not immediately discontinued.
- •
- to not restart TRIUMEQ or TRIUMEQ PD or any other abacavir‑containing product following a hypersensitivity reaction because more severe symptoms can occur within hours and may include life‑threatening hypotension and death.
- •
- that if they have a hypersensitivity reaction, they should dispose of any unused TRIUMEQ or TRIUMEQ PD to avoid restarting abacavir.
- •
- that a hypersensitivity reaction is usually reversible if it is detected promptly and TRIUMEQ or TRIUMEQ PD is stopped right away.
- •
- that if they have interrupted TRIUMEQ or TRIUMEQ PD for reasons other than symptoms of hypersensitivity (for example, those who have an interruption in drug supply), a serious or fatal hypersensitivity reaction may occur with reintroduction of abacavir.
- •
- to not restart TRIUMEQ or TRIUMEQ PD or any other abacavir‑containing product without medical consultation and only if medical care can be readily accessed by the patient or others.
- •
- to not restart TRIUMEQ or TRIUMEQ PD or any other dolutegravir-containing product following a hypersensitivity reaction to TRIUMEQ or TRIUMEQ PD.
Hepatotoxicity
Inform patients that hepatotoxicity has been reported with dolutegravir, a component of TRIUMEQ and TRIUMEQ PD [see Warnings and Precautions (5.3), Adverse Reactions (6.1)]. Inform patients that monitoring for hepatotoxicity during therapy with TRIUMEQ or TRIUMEQ PD is recommended.
Severe Acute Exacerbations of Hepatitis in Patients with HBV Co-infection
Advise all patients with HIV-1 to be tested for the presence of HBV prior to or when initiating TRIUMEQ or TRIUMEQ PD. Advise patients co‑infected with HIV‑1 and HBV that worsening of liver disease has occurred in some cases when treatment with lamivudine was discontinued. Advise patients to discuss any changes in regimen with their physician [see Warnings and Precautions (5.2)].
Lactic Acidosis/Hepatomegaly
Inform patients that some HIV medicines, including TRIUMEQ and TRIUMEQ PD, can cause a rare, but serious condition called lactic acidosis with liver enlargement (hepatomegaly) [see Boxed Warning, Warnings and Precautions (5.4)].
Immune Reconstitution Syndrome
Advise patients to inform their healthcare provider immediately of any signs and symptoms of infection as inflammation from previous infection may occur soon after combination antiretroviral therapy, including when TRIUMEQ or TRIUMEQ PD is started [see Warnings and Precautions (5.6)].
TRIUMEQ Tablets and TRIUMEQ PD Tablets for Oral Suspension Are Not Bioequivalent
Advise patients that TRIUMEQ and TRIUMEQ PD are not bioequivalent and are not substitutable on a milligram-per-milligram basis. Advise patients or their care provider that patients switching from the tablets for oral suspension to the tablets must adjust the dose [see Dosage and Administration (2.3) and Warnings and Precautions (5.7)].
Pregnancy Registry
Inform patients that there is an antiretroviral pregnancy registry to monitor fetal outcomes in those exposed to TRIUMEQ during pregnancy [see Use in Specific Populations (8.1)].
Lactation
Inform individuals with HIV-1 infection that the potential risks of breastfeeding include: (1) HIV-1 transmission (in HIV-1–negative infants), (2) developing viral resistance (in HIV-1–positive infants), and (3) adverse reactions in a breastfed infant similar to those seen in adults [see Use in Specific Populations (8.2)].
Administration Instructions
To avoid a dosing error from using the wrong formulation of TRIUMEQ, strongly advise patients and caregivers to visually inspect the tablets to verify the correct formulation each time the prescription is filled [see Dosage and Administration (2), Warnings and Precautions (5.7), How Supplied/Storage and Handling (16)].
Inform patients and caregivers that TRIUMEQ PD tablets for oral suspension should be dispersed in drinking water and should not be chewed, cut, crushed, or swallowed whole [see Dosage and Administration (2.5)]. Inform patients and caregivers that an appropriate-sized syringe may be used to administer the oral suspension if the patient is unable to use the supplied cup [see Dosage and Administration (2.5)].
Instruct patients and caregivers that if a dose of TRIUMEQ or TRIUMEQ PD is missed, to take it as soon as they remember. Advise patients and caregivers not to double the next dose or take more than the prescribed dose [see Dosage and Administration (2)].
Availability of Medication Guide
Instruct patients and caregivers to read the Medication Guide before starting TRIUMEQ or TRIUMEQ PD and to re-read it each time the prescription is renewed. Instruct patients to inform their physician or pharmacist if they develop any unusual symptom, or if any known symptom persists or worsens.
Storage
Instruct patients and caregivers to store TRIUMEQ and TRIUMEQ PD tablets for oral suspension in the original package, protect from moisture, and keep the bottle tightly closed. Do not remove desiccant.
EPIVIR, EPZICOM, TIVICAY, TIVICAY PD, TRIUMEQ, TRIUMEQ PD, and ZIAGEN are trademarks owned by or licensed to the ViiV Healthcare group of companies.
EPIVIR-HBV is a trademark owned by or licensed to the GSK group of companies.
The other brands listed are trademarks owned by or licensed to their respective owners and are not owned by or licensed to the ViiV Healthcare group of companies. The makers of these brands are not affiliated with and do not endorse the ViiV Healthcare group of companies or its products.
Manufactured for:
ViiV Healthcare
Durham, NC 27701
©2024 ViiV Healthcare group of companies or its licensor.
TRM:18PI
|
MEDICATION GUIDE |
|||
|
TRIUMEQ (TRI-u-meck) (abacavir, dolutegravir, and lamivudine) tablets |
TRIUMEQ PD (TRI-u-meck Pe De) (abacavir, dolutegravir, and lamivudine) tablets for oral suspension |
||
|
What is the most important information I should know about TRIUMEQ and TRIUMEQ PD? TRIUMEQ and TRIUMEQ PD can cause serious side effects, including:
|
|||
|
Symptom(s) | |||
|
Group 1 |
Fever | ||
|
Group 2 |
Rash | ||
|
Group 3 |
Nausea, vomiting, diarrhea, abdominal (stomach area) pain | ||
|
Group 4 |
Generally ill feeling, extreme tiredness, or achiness | ||
|
Group 5 |
Shortness of breath, cough, sore throat | ||
|
A list of these symptoms is on the Warning Card your pharmacist gives you. Carry this Warning Card with you at all times. If you stop TRIUMEQ or TRIUMEQ PD because of an allergic reaction, never take TRIUMEQ, TRIUMEQ PD (abacavir, dolutegravir and lamivudine), or any other medicine that contains abacavir or dolutegravir (DOVATO, EPZICOM, JULUCA, TIVICAY, TIVICAY PD, TRIZIVIR, or ZIAGEN) again.
If your healthcare provider tells you that you can take TRIUMEQ or TRIUMEQ PD again, start taking it when you are around medical help or people who can call a healthcare provider if you need one. |
|||
|
|||
|
What is TRIUMEQ and TRIUMEQ PD? TRIUMEQ and TRIUMEQ PD are prescription medicines used to treat HIV-1 infection in adults and children who are at least 3 months of age and weigh at least 13.2 pounds (6 kg). HIV-1 is the virus that causes Acquired Immune Deficiency Syndrome (AIDS). TRIUMEQ and TRIUMEQ PD contain the prescription medicines abacavir, dolutegravir, and lamivudine.
It is not known if TRIUMEQ PD is safe and effective in children who are less than 3 months of age or weigh less than 13.2 pounds (6 kg). |
|||
|
Do not take TRIUMEQ or TRIUMEQ PD if you:
|
|||
|
Before you take TRIUMEQ or TRIUMEQ PD, tell your healthcare provider about all of your medical conditions, including if you:
Pregnancy Registry. There is a pregnancy registry for those who take TRIUMEQ during pregnancy. The purpose of this registry is to collect information about the health of you and your baby. Talk with your healthcare provider about how you can take part in this registry.
Tell your healthcare provider about all the medicines you take, including prescription and over-the-counter medicines, vitamins, and herbal supplements. Some medicines interact with TRIUMEQ or TRIUMEQ PD. Keep a list of your medicines to show your healthcare provider and pharmacist when you get a new medicine.
|
|||
|
How should I take TRIUMEQ or TRIUMEQ PD? Read the Instructions for Use at the end of this Medication Guide for detailed instructions on how to prepare a dose of TRIUMEQ PD tablets for oral suspension.
|
|||
|
What are the possible side effects of TRIUMEQ or TRIUMEQ PD? TRIUMEQ or TRIUMEQ PD can cause serious side effects, including:
|
|||
|
|
||
|
|||
|
|
||
|
|||
|
|
|
|
|
These are not all the possible side effects of TRIUMEQ or TRIUMEQ PD. Call your doctor for medical advice about side effects. You may report side effects to FDA at 1‑800‑FDA‑1088. |
|||
|
How should I store TRIUMEQ or TRIUMEQ PD?
Keep TRIUMEQ, TRIUMEQ PD, and all medicines out of the reach of children. |
|||
|
General information about the safe and effective use of TRIUMEQ or TRIUMEQ PD. Medicines are sometimes prescribed for purposes other than those listed in a Medication Guide. Do not use TRIUMEQ or TRIUMEQ PD for a condition for which it was not prescribed. Do not give TRIUMEQ or TRIUMEQ PD to other people, even if they have the same symptoms that you have. It may harm them. You can ask your pharmacist or healthcare provider for information about TRIUMEQ or TRIUMEQ PD that is written for health professionals. |
|||
|
What are the ingredients in TRIUMEQ and TRIUMEQ PD? Active ingredients: abacavir, dolutegravir, and lamivudine Inactive ingredients: TRIUMEQ tablets: D-mannitol, magnesium stearate, microcrystalline cellulose, povidone, and sodium starch glycolate. Tablet film‑coating contains: iron oxide black, iron oxide red, macrogol/PEG, polyvinyl alcohol–part hydrolyzed, talc, and titanium oxide. TRIUMEQ PD tablets for oral suspension: acesulfame potassium, crospovidone, mannitol, microcrystalline cellulose, povidone K29/32, silicified microcrystalline cellulose, sodium starch glycolate, sodium stearyl fumarate, strawberry cream flavor, and sucralose. Tablet film‑coating contains: ferric oxide yellow, macrogol/PEG, polyvinyl alcohol-part hydrolyzed, talc, and titanium dioxide. |
|||
|
Manufactured for: ViiV Healthcare Durham, NC 27701 |
|||
|
DOVATO, EPZICOM, JULUCA, TIVICAY, TIVICAY PD, TRIUMEQ, TRIUMEQ PD, TRIZIVIR, and ZIAGEN are trademarks owned by or licensed to the ViiV Healthcare group of companies. ©2024 ViiV Healthcare group of companies or its licensor. TRM:17MG For more information go to www.TRIUMEQ.com or call 1-877-844-8872. |
|||
|
This Medication Guide has been approved by the U.S. Food and Drug Administration. |
Revised: 4/2024 |
||
PRINICPAL DISPLAY PANEL
NDC 49702-231-13
Triumeq
(abacavir, dolutegravir, and lamivudine) Tablets
600 mg/50 mg/300 mg
Rx only
Triumeq and Triumeq PD are not interchangeable.
Notice ot Authorized Dispenser:
Each time TRIUMEQ is dispensed, give the patient a Medication Guide and Warning Card.
30 Tablets
Each film-coated tablet contains 600 mg of abacavir (equivalent to 702 mg of abacavir sulfate), 50 mg of dolutegravir (equivalent to 52.6 mg of dolutegravir sodium), and 300 mg of lamivudine.
Store at 20°C to 25°C (68°F to 77°F); excursions permitted to 15° to 30°C (59° to 86°F) [See USP Controlled Room Temperature].
Keep bottle tightly closed; protect from moisture. Do not remove desiccant.
This package is child-resistant. Keep out of reach of children. See prescribing information for dosage information.
Do not accept if membrane seal under cap is missing or broken.
Manufactured for:
ViiV Healthcare
Durham, NC 27701
Trademarks owned or licensed by ViiV Healthcare.
©2023 ViiV Healthcare or licensor.
www.triumeq.com
- Rev. 1/23
- 62000000084540
PRINICPAL DISPLAY PANEL
NDC 49702-258-37
Triumeq PD
(abacavir, dolutegravir, and lamivudine)
Tablets of Oral Suspension
60 mg/5 mg/30 mg
Rx Only
Triumeq and Triumeq PD are not interchangeable.
Notice of Authorized Dispenser:
Each time Triumeq PD is dispensed, give the patient a Medication Guide and the Warning Card from the carton.
See prescribing information for dosage information.
Contents:
- •
- 1 Bottle of 90 tablets
- •
- 1 Dosing cup
- •
- Prescribing Information
- •
- Medication Guide
- •
- Instructions for Use
90 tablets
ViiV Healthcare
©2022 ViiV Healthcare group of companies or its licensor.
Made in UK
- 62000000084619 Rev. 12/22
| TRIUMEQ
abacavir sulfate, dolutegravir sodium, lamivudine tablet, film coated |
||||||||||||||||||||||||||
|
||||||||||||||||||||||||||
|
||||||||||||||||||||||||||
|
||||||||||||||||||||||||||
|
||||||||||||||||||||||||||
|
||||||||||||||||||||||||||
|
||||||||||||||||||||||||||
| TRIUMEQ PD
abacavir sulfate, dolutegravir sodium, lamivudine kit |
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
| Labeler - ViiV Healthcare Company (027295585) |
Frequently asked questions
- Can Triumeq be used for PrEP?
- Triumeq vs Genvoya. How do they compare?
- Does Triumeq cause erectile dysfunction?
- Can Triumeq be crushed or split?
- How long does it take for Triumeq to work?
- Does Triumeq cause weight gain?
- Does Triumeq cause hair loss?
- Is Triumeq an immunosuppressant?
- Is Triumeq a protease inhibitor?
More about Triumeq (abacavir / dolutegravir / lamivudine)
- Check interactions
- Compare alternatives
- Pricing & coupons
- Reviews (127)
- Drug images
- Side effects
- Dosage information
- Patient tips
- During pregnancy
- Support group
- FDA approval history
- Drug class: antiviral combinations
- En español