Lidocaine Suppository: Package Insert / Prescribing Info
Package insert / product label
Dosage form: rectal suppository
Drug class: Topical anesthetics
Medically reviewed by Drugs.com. Last updated on Jun 2, 2025.
On This Page
Lidocaine Suppository Description
Each suppository for rectal administration contains 50 mg lidocaine in a specially blended hydrogenated vegetable base. Lidocaine is a local anesthetic of the amide type, which is chemically designated as acetamide, 2-(diethylamino)-N-(2,6-dimethylphenyl)-, and has the following structural formula:
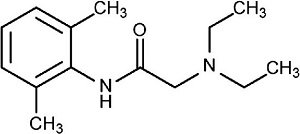
Lidocaine Suppository - Clinical Pharmacology
Mechanism of action
Lidocaine stabilizes the neuronal membrane by inhibiting the ionic fluxes required for the initiation and conduction of impulses, thereby effecting local anesthetic action.
Hemodynamics
Excessive blood levels may cause changes in cardiac output, total peripheral resistance, and mean arterial pressure. These changes may be attributable to a direct depressant effect of the local anesthetic agent on various components of the cardiovascular system.
Pharmacokinetics and metabolism
Lidocaine is absorbed following topical administration to mucous membranes, its rate and extent of absorption being dependent upon concentration and total dose administered, the specific site of application, and duration of exposure. In general, the rate of absorption of local anesthetic agents following topical application occurs most rapidly after intratracheal administration. Lidocaine is also well-absorbed from the gastrointestinal tract, but little intact drug appears in the circulation because of biotransformation in the liver.
Lidocaine is metabolized rapidly by the liver, and metabolites and unchanged drug are excreted by the kidneys. Biotransformation includes oxidative N-dealkylation, ring hydroxylation, cleavage of the amide linkage, and conjugation. N-dealkylation, a major pathway of biotransformation, yields the metabolites monoethylglycinexylidide and glycinexylidide. The pharmacological/toxicological actions of these metabolites are similar to, but less potent than, those of lidocaine. Lidocaine and its metabolites are excreted by the kidneys. Approximately 90% of lidocaine administered is excreted in the form of various metabolites, and less than 10% of lidocaine is excreted unchanged. The primary metabolite in urine is a conjugate of 4-hydroxy-2,6-dimethylaniline.
The plasma binding of lidocaine is dependent on drug concentration, and the fraction bound decreases with increasing concentration. At concentrations of 1 to 4 µg of free base per ml, 60 to 80 percent of lidocaine is protein bound. Binding is also dependent on the plasma concentration of the alpha-1-acid glycoprotein.
Lidocaine crosses the blood-brain and placental barriers, presumably by passive diffusion.
Studies of lidocaine metabolism following intravenous bolus injections have shown that the elimination half-life of this agent is typically 1.5 to 2 hours. Because of the rapid rate at which lidocaine is metabolized, any condition that affects liver function may alter lidocaine kinetics. The half-life may be prolonged two-fold or more in patients with liver dysfunction. Renal dysfunction does not affect lidocaine kinetics but may increase the accumulation of metabolites.
Factors such as acidosis and the use of CNS stimulants and depressants affect the CNS levels of lidocaine required to produce overt systemic effects. Objective adverse manifestations become increasingly apparent with increasing venous plasma levels above 6 mcg free base per mL. In the rhesus monkey arterial blood levels of 18 to 21 mcg/mL have been shown to be threshold for convulsive activity.
Indications and Usage for Lidocaine Suppository
Lidocaine suppositories are indicated for the symptomatic relief of pain in the anorectum.
Contraindications
Lidocaine is contraindicated in patients with a known history of hypersensitivity to local anesthetics of the amide type or to any other component of the product.
Warnings
EXCESSIVE DOSAGE, OR SHORT INTERVALS BETWEEN DOSES, CAN RESULT IN INCREASED ABSORBTION AND SERIOUS ADVERSE EFFECTS. LIDOCAINE PLASMA CONCENTRATIONS ABOVE 5 mcg/mL MAY RESULT IN TOXICITY. PATIENTS SHOULD BE INSTRUCTED TO STRICTLY ADHERE TO THE RECOMMENDED DOSAGE AND ADMINISTRATION GUIDELINES AS SET FORTH IN THIS PACKAGE INSERT. THE MANAGEMENT OF SERIOUS ADVERSE REACTIONS MAY REQUIRE THE USE OF RESUSCITATIVE EQUIPMENT, OXYGEN, AND OTHER RESUSCITATIVE DRUGS.
Lidocaine should be used with extreme caution if the mucosa in the area of application has been traumatized, since under such conditions there is the potential for rapid systemic absorption.
Methemoglobinemia
Cases of methemoglobinemia have been reported in association with local anesthetic use. Although all patients are at risk for methemoglobinemia, patients with glucose-6-phosphate dehydrogenase deficiency, congenital or idiopathic methemoglobinemia, cardiac or pulmonary compromise, infants under 6 months of age, and concurrent exposure to oxidizing agents or their metabolites are more susceptible to developing clinical manifestations of the condition. If local anesthetics must be used in these patients, close monitoring for symptoms and signs of methemoglobinemia is recommended.
Signs of methemoglobinemia may occur immediately or may be delayed some hours after exposure and are characterized by a cyanotic skin discoloration and/or abnormal coloration of the blood. Methemoglobin levels may continue to rise; therefore, immediate treatment is required to avert more serious central nervous system and cardiovascular adverse effects, including seizures, coma, arrhythmias, and death. Discontinue Lidocaine Suppositories and any other oxidizing agents. Depending on the severity of the signs and symptoms, patients may respond to supportive care, i.e., oxygen therapy, hydration. A more severe clinical presentation may require treatment with methylene blue, exchange transfusion, or hyperbaric oxygen.
Precautions
General
The safety and effectiveness of lidocaine depend on proper dosage, correct technique, adequate precautions, and readiness for emergencies (see WARNINGS and ADVERSE REACTIONS). The lowest dosage that results in effective anesthesia should be used to avoid high plasma levels and serious adverse effects. Repeated doses of lidocaine may cause significant increases in blood levels with each repeated dose because of slow accumulation of the drug and/or its metabolites. Tolerance varies with the status of the patient. Debilitated, elderly patients, acutely ill patients, and children should be given reduced doses commensurate with their age, weight and physical condition. Lidocaine should also be used with caution in patients with severe shock or heart block.
Lidocaine should be used with caution in patients with known drug sensitivities. Patients allergic to paraaminobenzoic acid derivatives (procaine, tetracaine, benzocaine, etc.) have not shown cross sensitivity to lidocaine. Many drugs used during the conduct of anesthesia are considered potential triggering agents for familial malignant hyperthermia. Since it is not known whether amide-type local anesthetics may trigger this reaction and since the need for supplemental general anesthesia cannot be predicted in advance, it is suggested that a standard protocol for the management of malignant hyperthermia should be available. Early unexplained signs of tachycardia, tachypnea, labile blood pressure and metabolic acidosis may precede temperature elevation. Successful outcome is dependent on early diagnosis, prompt discontinuance of the suspect triggering agent(s) and institution of treatment, including oxygen therapy, indicated supportive measures and dantrolene (consult dantrolene sodium intravenous package insert before using).
Drug Interactions
Patients who are administered local anesthetics are at increased risk of developing methemoglobinemia when concurrently exposed to the following drugs, which could include other local anesthetics:
Examples of Drugs Associated with Methemoglobinemia:
| Class | Examples |
|---|---|
| Nitrates/Nitrites | nitroglycerin, nitroprusside, nitric oxide, nitrous oxide |
| Local anesthetics | benzocaine, lidocaine, bupivacaine, mepivacaine, tetracaine, prilocaine, procaine, articaine |
| Antineoplastic agents | cyclophosphamide, flutamide, rasburicase, ifosfamide, hydroxyurea |
| Antibiotics | dapsone, sulfonamides, nitrofurantoin, para-aminosalicylic acid |
| Antimalarials | chloroquine, primaquine |
| Anticonvulsants | phenytoin, sodium valproate, phenobarbital |
| Other drugs | acetaminophen, metoclopramide, sulfa drugs (i.e., sulfasalazine), quinine |
Information for Patients
Application to broken or inflamed skin, although not tested, may result in higher blood concentrations of lidocaine from increased absorption.
Inform patients that use of local anesthetics may cause methemoglobinemia, a serious condition that must be treated promptly. Advise patients or caregivers to seek immediate medical attention if they or someone in their care experience the following signs or symptoms: pale, gray, or blue colored skin (cyanosis); headache; rapid heart rate; shortness of breath; lightheadedness; or fatigue.
PATIENTS SHOULD BE INSTRUCTED TO STRICTLY ADHERE TO DOSING INSTRUCTIONS, AND TO KEEP THE SUPPLY OF MEDICATION OUT OF THE REACH OF CHILDREN.
Carcinogenesis, Mutagenesis, Impairment of Fertility
Studies of lidocaine in animals to evaluate the carcinogenic and mutagenic potential or the effect on fertility have not been conducted.
Use in Pregnancy
Teratogenic Effects: Pregnancy Category B. Lidocaine suppository 50 mg has not been studied in pregnancy. Reproduction studies with lidocaine have been performed in rats at doses up to 30 mg/kg subcutaneously and have revealed no evidence of harm to the fetus due to lidocaine. There are, however, no adequate and well-controlled studies in pregnant women. Because animal reproduction studies are not always predictive of human response, lidocaine suppository 50 mg/dose should be used during pregnancy only if clearly needed.
Adverse Reactions/Side Effects
Adverse experiences following the administration of lidocaine are similar in nature to those observed with other amide local anesthetic agents. These adverse experiences are, in general, dose-related and may result from high plasma levels caused by excessive dosage or rapid absorption, or may result from a hypersensitivity, idiosyncrasy or diminished tolerance on the part of the patient. Serious adverse experiences are generally systemic in nature. The following types are those most commonly reported:
Central nervous system
CNS manifestations are excitatory and/or depressant and may be characterized by lightheadedness, nervousness, apprehension, euphoria, confusion, dizziness, drowsiness, tinnitus, blurred or double vision, vomiting, sensations of heat, cold or numbness, twitching, tremors, convulsions, unconsciousness, respiratory depression and arrest. The excitatory manifestations may be very brief or may not occur at all, in which case manifestation of toxicity may be drowsiness merging into unconsciousness and respiratory arrest. Drowsiness following the administration of lidocaine is usually an early sign of a high blood level of the drug and may occur as a consequence of rapid absorption.
Cardiovascular system
Cardiovascular manifestations are usually depressant and are characterized by bradycardia, hypotension, and cardiovascular collapse, which may lead to cardiac arrest.
Allergic
Allergic reactions are characterized by cutaneous lesions, urticaria, edema or anaphylactoid reactions. Allergic reactions may occur as a result of sensitivity either to the local anesthetic agent or to other components of this formulation. Allergic reactions as a result of sensitivity to lidocaine are extremely rare and, if they occur, should be managed by conventional means. The detection of sensitivity by skin testing is of doubtful value.
To report SUSPECTED ADVERSE REACTIONS, contact Burke Therapeutics at 1-501-620-4449 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
Related/similar drugs
Overdosage
Acute emergencies from local anesthetics are generally related to high plasma levels encountered during therapeutic use of local anesthetics. (See ADVERSE REACTIONS, WARNINGS and PRECAUTIONS)
Management of local anesthetic emergencies
The first consideration is prevention, best accomplished by careful and constant monitoring of cardiovascular and respiratory vital signs and the patient’s state of consciousness after each local anesthetic administration. At the first sign of change oxygen should be administered.
The first step in the management of convulsions consist of immediate attention to the maintenance of a patent airway and assisted or controlled ventilation with oxygen. In situations where trained personnel are readily available, ventilation should be maintained and oxygen should be delivered by a delivery system capable of permitting immediate positive airway pressure by mask. Immediately after the institution of these ventilatory measures, the adequacy of the circulation should be evaluated, keeping in mind that drugs used to treat convulsions sometimes depress the circulation when administered intravenously. Should convulsions persist despite adequate respiratory support, and if the status of the circulation permits, small increments of an ultra-short acting barbiturate (such as thiopental or thiamylal) or a benzodiazepine (such as diazepam) may be administered intravenously. The clinician should be familiar, prior to use of local anesthetics, with these anticonvulsant drugs. Supportive treatment of circulatory depression may require administration of intravenous fluids and, when appropriate, a vasopressor as indicated by the clinical situation (e.g., ephedrine).
If not treated immediately, both convulsions and cardiovascular depression can result in hypoxia, acidosis, bradycardia, arrhythmias and cardiac arrest. If cardiac arrest should occur, standard cardiopulmonary resuscitative measures should be instituted.
Dialysis is of negligible value in the treatment of acute overdosage with lidocaine.
The oral LD 50 of lidocaine in non-fasted female rats is 459 (346-773) mg/kg (as the salt) and 214 (159-324) mg/kg (as the salt) in fasted female rats.
Lidocaine Suppository Dosage and Administration
When Lidocaine Suppository 50 mg is used concomitantly with other products containing lidocaine, the total dose contributed by all formulations must be kept in mind.
Adult
The maximum recommended single dose of Lidocaine Suppository 50 mg/dose is one suppository, or 50 mg of lidocaine base. The patient should not exceed a maximum of four (4) suppositories in a 24 hour period.
The dosage should be adjusted commensurate with the patient’s age, weight and physical condition (see PRECAUTIONS).
How is Lidocaine Suppository supplied
Suppositories: Supplied in cartons of 24 count NDC 69101-150-24.
Appearance: White waxy cylinders rounded on one end.
Storage and Handling
Store at 20°C to 25°C (68°F to 77°F); excursions permitted to 15°C -30°C (59°-86°F) [See USP Controlled Room Temperature]. Store away from heat.
KEEP THIS AND ALL DRUGS OUT OF THE REACH OF CHILDREN. In case of accidental ingestion, seek professional assistance or contact a Poison Control Center immediately.
Pharmacist: This product is not an Orange Book rated product, therefore all prescriptions using this product shall be subject to state and federal statutes as applicable. This product has not been subjected to FDA therapeutic or other equivalency testing. There are no claims of bioequivalence or therapeutic equivalence. Each person recommending a prescription substitution using this product shall make such recommendation based on his/her professional knowledge and opinion, upon evaluating the active ingredients, inactive ingredients, excipients and chemical information contained within the enclosed prescribing information.
| LIDOCAINE
lidocaine suppository |
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
| Labeler - Burke Therapeutics, LLC (079259903) |
More about lidocaine topical
- Check interactions
- Compare alternatives
- Pricing & coupons
- Reviews (248)
- Latest FDA alerts (8)
- Side effects
- Dosage information
- During pregnancy
- Drug class: topical anesthetics
- Breastfeeding
Patient resources
Professional resources
- Lidocaine (Topical) monograph
- Lidocaine Cream (FDA)
- Lidocaine Gel (FDA)
- Lidocaine Jelly (FDA)
- Lidocaine Lotion (FDA)
Other brands
Lidocaine Viscous, Lidocan Patch, ZTlido, Xylocaine Jelly, ... +35 more

