Gangrene
Medically reviewed by Drugs.com. Last updated on Jun 2, 2025.
What is gangrene?
Gangrene is a condition that happens when tissue dies. Gangrene may be caused by conditions that stop blood flow, or a bacterial infection. Blood flow to tissues may be stopped by a blood clot or narrowed blood vessels. Bacteria may get into tissue through an incision or a wound, such as a burn, gunshot, or ulcer. Gangrene most commonly affects the hand, fingers, arm, foot, toes, or leg. Gangrene is a life-threatening condition that needs immediate treatment.
What increases my risk for gangrene?
- Diabetes
- Peripheral artery disease
- Conditions that cause your blood to clot easily, such as Factor V Leiden
- Conditions that cause a weak immune system, such as HIV
- Severe frostbite
- IV drug abuse
- Cancer
What are the signs and symptoms of gangrene?
Gangrene usually begins with fever, pain, and swelling. The pain and swelling usually get worse quickly. The area of dead tissue may look brown, red, purple, or black. It may drain red or yellow fluid that smells bad. You may have a fast heartbeat and feel weak or dizzy. If the infection spreads, you may be confused or lose consciousness.
How is gangrene diagnosed and treated?
Your healthcare provider will examine the area and take a sample of tissue. The tissue will be tested for bacteria. A blood sample may also be collected and tested for bacteria.
Related medications
Plavix
Plavix (clopidogrel) is used to prevent blood clots after a recent heart attack or stroke. Includes ...
Xarelto
Xarelto (rivaroxaban) is a factor Xa inhibitor used to reduce the risk of blood clots and stroke in ...
Ozempic
Learn about Ozempic (semaglutide) for type 2 diabetes treatment, weight management, cardiovascular ...
Zontivity
Zontivity is used for the prevention of cardiovascular events. Includes Zontivity side effects ...
Vorapaxar
Vorapaxar systemic is used for peripheral arterial disease, prevention of atherothrombotic events ...
Rivaroxaban
Rivaroxaban systemic is used for atrial fibrillation, cardiovascular risk reduction, congenital ...
Clopidogrel
Clopidogrel systemic is used for acute coronary syndrome, acute coronary syndrome, prophylaxis ...
How is gangrene treated?
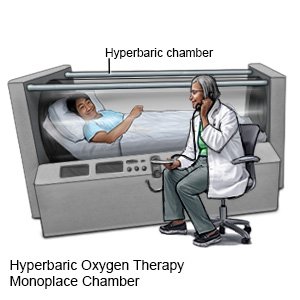
Gangrene is treated with surgery to remove the dead tissue. In severe cases, part of your arm or leg may also be removed. You may be given antibiotics to treat an infection. You will be given medicine to decrease pain and fever. Conditions that cause poor blood flow will also be treated. After surgery, you may need hyperbaric oxygen (HBO) therapy. HBO therapy helps the tissue heal by increasing blood flow and preventing the infection from getting worse. If the infection spreads to the rest of your body, you may need other treatments.
 |
Treatment options
The following list of medications are related to or used in the treatment of this condition.
How can I help prevent gangrene?
- Care for all wounds and incisions as directed. Always wash your hands before and after you touch your wound or incision. Use soap and water or an alcohol-based hand rub. Carefully wash around the wound or incision with soap and water. Dry the area and put on new, clean bandages as directed. Change your bandages when they get wet or dirty. Call your healthcare provider if your wound or incision becomes red, swollen, or drains pus. Early treatment can help prevent gangrene.
- Manage other health conditions. This includes diabetes, peripheral artery disease, and problems with blood clotting. These conditions can increase your risk for wound infections.
- Seek care immediately for symptoms of a blood clot or poor blood flow. Symptoms of a blood clot include an arm or leg that feels warm, tender, and painful. It may look swollen and red. Symptoms of poor blood flow include an arm or leg that is cold, pale, or numb.
What can I do to care for myself?
- Elevate your arm or leg above the level of your heart as often as you can. This will help decrease swelling and pain. Prop your arm or leg on pillows or blankets to keep it elevated comfortably.
- Rest as directed. Do not return to your usual activities until healthcare provider says it is okay. It may take several weeks for you to recover.
- Eat a variety of healthy foods. Healthy foods will help you heal. Healthy foods include fruits, vegetables, whole-grain breads, low-fat dairy products, beans, lean meats, and fish. Ask if you need to be on a special diet.
When should I seek immediate care?
- Your symptoms return or you have new symptoms.
When should I call my doctor?
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Gangrene
Treatment options
Care guides
Symptoms and treatments
Medicine.com guides (external)
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
