Adjustable Gastric Band Surgery
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
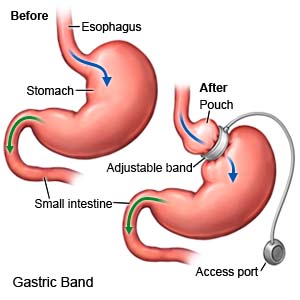
Gastric banding is a type of weight loss surgery. An adjustable band is placed around the top part of your stomach. This divides the stomach into one small pouch and one large pouch. Food collects in the small pouch when you eat. You will feel full quickly because the pouch is very small. An opening in the smaller pouch allows food to pass into the larger pouch. Between meals, the food moves slowly into the larger pouch and is digested normally. Your healthcare provider can tighten or loosen the band as needed after the surgery.
 |
DISCHARGE INSTRUCTIONS:
Call your local emergency number (911 in the US) for any of the following:
- You feel lightheaded or short of breath, or you have chest pain.
- You cough up blood.
Seek care immediately if:
- Your arm or leg feels warm, tender, and painful. It may look swollen and red.
- Blood soaks through your bandages.
- Your stitches or incisions come apart.
- You cannot stop vomiting.
Call your doctor or surgeon if:
- You have a fever higher than 100°F (37.8°C).
- You have pain or pressure in your abdomen or back, hiccups, and you feel restless.
- You have pain in your abdomen or on the right side of your body under your ribs.
- You have redness, swelling, or pus coming from your incisions.
- You have nausea and are vomiting.
- You feel your heart beating faster than usual.
- You have questions or concerns about your condition or care.
Related medications
Medicines:
You may need any of the following:
- Medicine may be given to lower the amount of stomach acid, or to relieve heartburn.
- Nausea medicine may be needed to help decrease nausea and prevent vomiting.
- Acetaminophen decreases pain and fever. It is available without a doctor's order. Ask how much to take and how often to take it. Follow directions. Read the labels of all other medicines you are using to see if they also contain acetaminophen, or ask your doctor or pharmacist. Acetaminophen can cause liver damage if not taken correctly.
- Prescription pain medicine may be given. Ask your healthcare provider how to take this medicine safely. Some prescription pain medicines contain acetaminophen. Do not take other medicines that contain acetaminophen without talking to your healthcare provider. Too much acetaminophen may cause liver damage. Prescription pain medicine may cause constipation. Ask your healthcare provider how to prevent or treat constipation.
- Blood thinners help prevent blood clots. Clots can cause strokes, heart attacks, and death. Many types of blood thinners are available. Your healthcare provider will give you specific instructions for the type you are given. The following are general safety guidelines to follow while you are taking a blood thinner:
- Watch for bleeding and bruising. Watch for bleeding from your gums or nose. Watch for blood in your urine and bowel movements. Use a soft washcloth on your skin, and a soft toothbrush to brush your teeth. This can keep your skin and gums from bleeding. If you shave, use an electric shaver. Do not play contact sports.
- Tell your dentist and other healthcare providers that you take a blood thinner. Wear a bracelet or necklace that says you take this medicine.
- Do not start or stop any other medicines or supplements unless your healthcare provider tells you to. Many medicines and supplements cannot be used with blood thinners.
- Take your blood thinner exactly as prescribed by your healthcare provider. Do not skip a dose or take less than prescribed. Tell your provider right away if you forget to take your blood thinner, or if you take too much.
- Take your medicine as directed. Contact your healthcare provider if you think your medicine is not helping or if you have side effects. Tell your provider if you are allergic to any medicine. Keep a list of the medicines, vitamins, and herbs you take. Include the amounts, and when and why you take them. Bring the list or the pill bottles to follow-up visits. Carry your medicine list with you in case of an emergency.
Follow your nutrition plan:
Ask your dietitian or nutritionist any questions you have about your nutrition plan. The plan will include which foods to eat and how much of each to eat during a meal.
- Eat slowly. Chew your food well before you swallow. Large bits of food may cause choking or may block your stomach. You may vomit or have abdominal pain or heartburn if you eat too quickly. You may also develop a stomach ulcer. Food that is not chewed well enough may get stuck in the opening between the small and large stomach pouches.
- Eat 3 small meals each day. You may stretch out your stomach pouch if you often eat too much. Do not eat snacks between meals unless your healthcare provider says it is okay. Stop eating when you feel full, even if you have not eaten all of your meal.
- Eat nutritious foods. Eat plenty of protein. Foods that contain protein include chicken, fish, eggs, and dairy products. You may need protein drinks for the first week after surgery. Avoid candy, cookies, ice cream, and fried foods.

- Drink liquids between meals. Wait at least 1 to 2 hours after a meal before you drink liquids. Do not drink liquids with meals. Drink water, diet drinks, or other drinks that have few or no calories. Do not drink carbonated liquids, such as soft drinks.
Self-care:
- Care for your surgery area as directed. When you allowed to bathe, carefully wash the area with soap and water. Dry the area and put on new, clean bandages as directed. Change your bandages when they get wet or dirty.
- Do activity or exercise as directed. Aim to get at least 150 minutes of physical activity each week, or 30 minutes on most days. You can break the 30 minutes into shorter periods of activity throughout the day. Ask your healthcare provider about the best exercise plan for you.

- Go to therapy. Therapy may include working with a counselor to understand your reasons for overeating. You may want to join a support group to talk with others who have had gastric band surgery.
Pregnancy after surgery:
If you are a woman of childbearing age, your healthcare provider will talk to you about family planning.
- Your provider may recommend that you do not get pregnant for 12 to 18 months after surgery. Then your pregnancy will be monitored for your safety and the safety of your baby. Your band will need to be adjusted during pregnancy. This helps your baby get enough calories and nutrition to develop properly.
- Tell your provider if you want to prevent pregnancy. He or she can help you choose the right kind of birth control.
Follow up with your doctor or surgeon as directed:
You will need to return in 1 to 2 weeks and then regularly for support and to have your gastric band checked or adjusted. Write down your questions so you remember to ask them during your visits.
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
