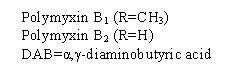Neomycin,Polymyxin B,Dexamethasone Ointment: Package Insert / Prescribing Info
Package insert / product label
Generic name: neomycin sulfate, polymyxin b sulfate, and dexamethasone
Dosage form: ophthalmic ointment
Drug class: Ophthalmic steroids with anti-infectives
Medically reviewed by Drugs.com. Last updated on Nov 28, 2024.
On This Page
Neomycin,Polymyxin B,Dexamethasone Ointment Description
Neomycin and polymyxin B sulfates and dexamethasone ophthalmic ointment is a multiple dose anti-infective steroid combination in sterile ointment form for topical application.
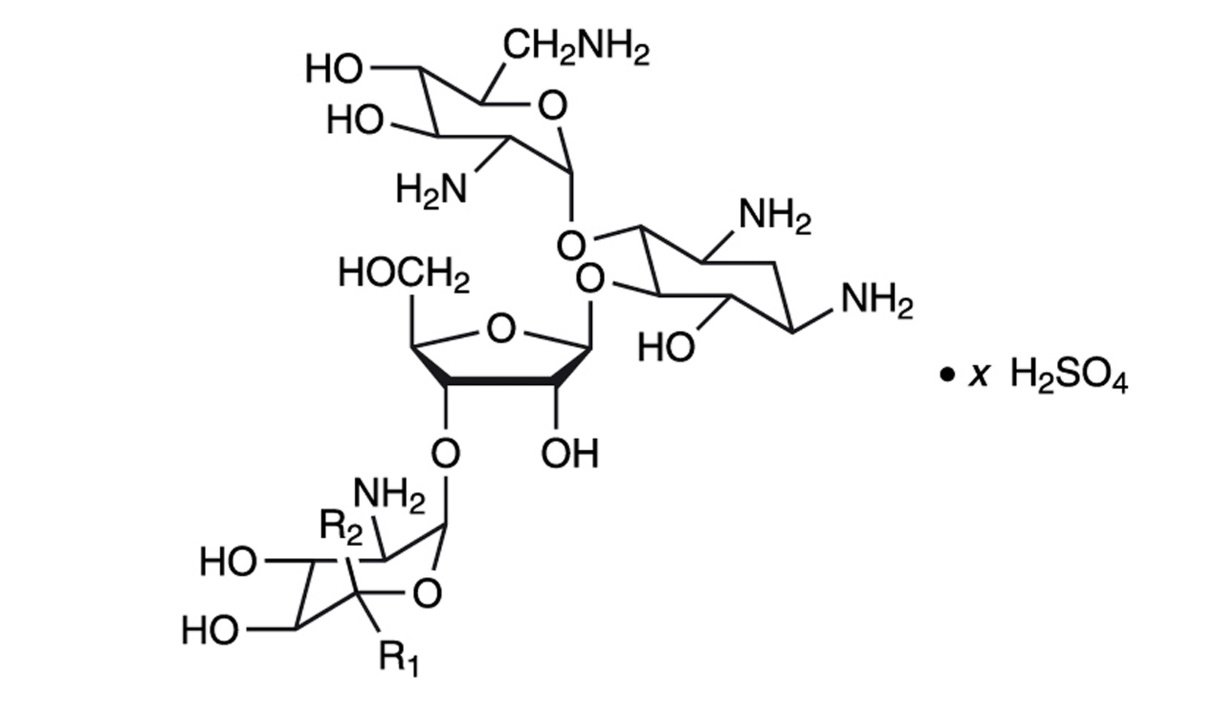
The chemical structure for the active ingredient Neomycin Sulfate is:
Neomycin B (R1=H, R2=CH2NH2)
Neomycin C (R1=CH2NH2, R2=H)
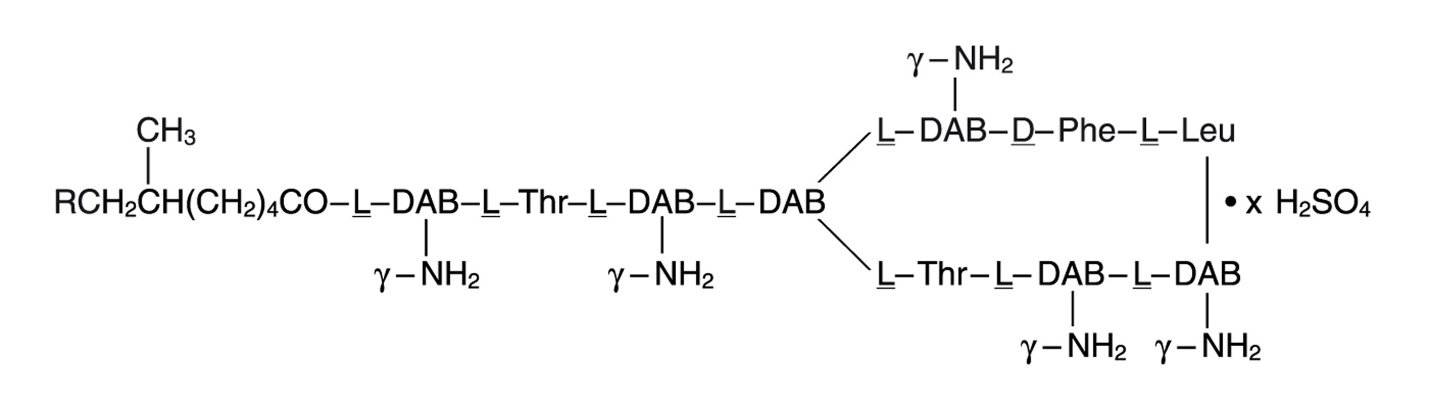
The chemical structure for the active ingredient Polymyxin B Sulfate is:
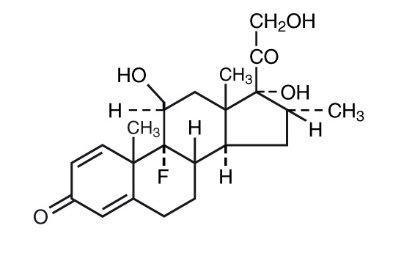
The chemical structure for the active ingredient Dexamethasone is:
C22H29FO5
Molecular Weight = 392.47 g/mol
Established name: dexamethasone
Chemical name: pregna-1, 4-diene-3, 20-dione,9-fluoro-11,17, 21-trihydroxy-16-methyl-, (11β, 16α)-.
Each gram of neomycin and polymyxin B sulfates and dexamethasone ophthalmic ointment contains: Active: neomycin sulfate equivalent to neomycin 3.5 mg, polymyxin B sulfate 10,000 units, dexamethasone 0.1%. Preservatives: methylparaben 0.05%, propylparaben 0.01%. Inactives: anhydrous liquid lanolin and white petrolatum.
Neomycin,Polymyxin B,Dexamethasone Ointment - Clinical Pharmacology
Corticosteroids suppress the inflammatory response to a variety of agents and they probably delay or slow healing. Since corticosteroids may inhibit the body's defense mechanism against infection, a concomitant antimicrobial drug may be used when this inhibition is considered to be clinically significant in a particular case.
When a decision to administer both a corticosteroid and an antimicrobial is made, the administration of such drugs in combination has the advantage of greater patient compliance and convenience, with the added assurance that the appropriate dosage of both drugs is administered, plus assured compatibility of ingredients when both types of drugs are in the same formulation and, particularly, that the correct volume of drug is delivered and retained.
The relative potency of corticosteroids depends on the molecular structure, concentration and release from the vehicle.
Indications and Usage for Neomycin,Polymyxin B,Dexamethasone Ointment
For steroid-responsive inflammatory ocular conditions for which a corticosteroid is indicated and where bacterial infection or a risk of bacterial ocular infection exists.
Ocular steroids are indicated in inflammatory conditions of the palpebral and bulbar conjunctiva, cornea, and anterior segment of the globe where the inherent risk of steroid use in certain infective conjunctivitides is accepted to obtain a diminution in edema and inflammation. They are also indicated in chronic anterior uveitis and corneal injury from chemical, radiation or thermal burns; or penetration of foreign bodies.
The use of a combination drug with an anti-infective component is indicated where the risk of infection is high or where there is an expectation that potentially dangerous numbers of bacteria will be present in the eye.
The particular anti-infective drug in this product is active against the following common bacterial eye pathogens: Staphylococcus aureus, Escherichia coli, Haemophilus influenzae, Klebsiella/Enterobacter species, Neisseria species, and Pseudomonas aeruginosa.
This product does not provide adequate coverage against: Serratia marcescens and Streptococci, including Streptococcus pneumoniae.
Contraindications
Neomycin and polymyxin B sulfates and dexamethasone ophthalmic ointment is contraindicated in epithelial herpes simplex keratitis (dendritic keratitis), vaccinia, varicella, and many other viral diseases of the cornea and conjunctiva. Mycobacterial infection of the eye. Fungal diseases of ocular structures. Neomycin and polymyxin B sulfates and dexamethasone ophthalmic ointment is also contraindicated in individuals with known or suspected hypersensitivity to a component of the medication. (Hypersensitivity to the antibiotic component occurs at a higher rate than for other components.)
Warnings
NOT FOR INJECTION. Use of ocular steroids may prolong the course and may exacerbate the severity of many viral infections of the eye (including herpes simplex). Employment of steroid medication in the treatment of herpes simplex requires great caution; frequent slit lamp microscopy is recommended.
Prolonged use may result in glaucoma, with damage to the optic nerve, defects in visual acuity and fields of vision, and posterior subcapsular cataract formation. Prolonged use may suppress the host response and thus increase the hazard of secondary ocular infections. In acute purulent conditions or parasitic infections of the eye, steroids may mask infection or enhance existing infection.
In those diseases causing thinning of the cornea or sclera, perforations have been known to occur with the use of topical steroids.
If this product is used for 10 days or longer, intraocular pressure (IOP) should be routinely monitored even though it may be difficult in children and uncooperative patients. Steroids should be used with caution in the presence of glaucoma. IOP should be checked frequently.
The use of steroids after cataract surgery may delay healing and increase the incidence of bleb formation.
Products containing neomycin sulfate may cause cutaneous sensitization. Sensitivity to topically administered aminoglycosides, such as neomycin, may occur in some patients. Severity of hypersensitivity reactions may vary from local effects to generalized reactions such as erythema, itching, urticaria, skin rash, anaphylaxis, anaphylactoid reactions, or bullous reactions. If hypersensitivity develops during use of the product, treatment should be discontinued. Cross-hypersensitivity to other aminoglycosides can occur, and the possibility that patients who become sensitized to topical neomycin may also be sensitive to other topical and/or systemic aminoglycosides should be considered.
Precautions
General
The initial prescription and renewal of the medication order beyond 8 g of neomycin and polymyxin B sulfates and dexamethasone ophthalmic ointment should be made by a physician only after examination of the patient with the aid of magnification, such as a slit lamp biomicroscopy and, where appropriate, fluorescein staining.
The possibility of persistent fungal infections of the cornea should be considered after prolonged steroid dosing. Fungal infection should be suspected in patients with persistent corneal ulceration.
Information for Patients
If inflammation or pain persists longer than 48 hours or becomes aggravated, the patient should be advised to discontinue use of the medication and consult a physician.
This product is sterile when packaged. To prevent contamination, care should be taken to avoid touching the tube tip to eyelids or to any other surface. The use of this tube by more than one person may spread infection. Keep tube tightly closed when not in use. Keep out of reach of children.
Patients should be advised that their vision may be temporarily blurred following dosing with neomycin and polymyxin B sulfates and dexamethasone ophthalmic ointment. Care should be exercised in operating machinery or driving a motor vehicle.
Carcinogenesis, Mutagenesis, Impairment of Fertility
Long-term studies in animals to evaluate carcinogenic or mutagenic potential have not been conducted with polymyxin B sulfate. Treatment of cultured human lymphocytes in vitro with neomycin increased the frequency of chromosome aberrations at the highest concentration (80 mcg/mL) tested. However, the effects of neomycin on carcinogenesis and mutagenesis in humans are unknown. Polymyxin B has been reported to impair the motility of equine sperm, but its effects on male or female fertility are unknown.
Pregnancy
Dexamethasone has been shown to be teratogenic in mice and rabbits following topical ophthalmic application in multiples of the therapeutic dose.
In the mouse, corticosteroids produce fetal resorptions and a specific abnormality, cleft palate. In the rabbit, corticosteroids have produced fetal resorptions and multiple abnormalities involving the head, ears, limbs, palate, etc.
There are no adequate or well-controlled studies in pregnant women. However, prolonged or repeated corticoid use during pregnancy has been associated with an increased risk of intra-uterine growth retardation. Neomycin and polymyxin B sulfates and dexamethasone ophthalmic ointment should be used during pregnancy only if the potential benefit to the mother justifies the potential risk to the embryo or fetus. Infants born of mothers who have received substantial doses of corticosteroids during pregnancy should be observed carefully for signs of hypoadrenalism.
Nursing Mothers
Systemically administered corticosteroids appear in human milk, could suppress growth, interfere with endogenous corticosteroid production, or cause other untoward effects. It is not known whether topical administration of corticosteroids could result in sufficient systemic absorption to produce detectable quantities in human milk. Because many drugs are excreted in human milk, caution should be exercised when neomycin and polymyxin B sulfates and dexamethasone ophthalmic ointment is administered to a nursing woman.
Pediatric Use
Safety and effectiveness in pediatric patients have not been established.
Geriatric Use
No overall clinical differences in safety or effectiveness have been observed between the elderly and other adult patients.
Adverse Reactions/Side Effects
Adverse reactions have occurred with steroid/anti-infective combination drugs which can be attributed to the steroid component, the anti-infective component, or the combination. Exact incidence figures are not available since no denominator of treated patients is available.
Reactions occurring most often from the presence of the anti-infective ingredient are allergic sensitizations. The reactions due to the steroid component are: elevation of IOP with possible development of glaucoma, and infrequent optic nerve damage; posterior subcapsular cataract formation; and delayed wound healing.
Secondary Infection: The development of secondary infection has occurred after use of combinations containing steroids and antimicrobials. Fungal infections of the cornea are particularly prone to develop coincidentally with long-term applications of steroid. The possibility of fungal invasion must be considered in any persistent corneal ulceration where steroid treatment has been used. Keratitis, conjunctivitis, corneal ulcers, and conjunctival hyperemia have occasionally been reported following use of steroids. Secondary bacterial ocular infection following suppression of host responses also occurs.
Additional adverse reactions identified from post marketing use include ulcerative keratitis, headache, and Stevens-Johnson syndrome.
The following additional adverse reactions have been reported with dexamethasone use:
Cushing’s syndrome and adrenal suppression may occur after use of dexamethasone in excess of the listed dosing instructions in predisposed patients, including children and patients treated with CYP3A4 inhibitors.
Related/similar drugs
Neomycin,Polymyxin B,Dexamethasone Ointment Dosage and Administration
Apply a small amount into the conjunctival sac(s) up to three or four times daily, or may be used adjunctively with Neomycin and Polymyxin B Sulfates and Dexamethasone Ophthalmic Suspension at bedtime.
How to Apply Neomycin and polymyxin B sulfates and dexamethasone ophthalmic ointment:
1. Tilt your head back.
2. Place a finger on your cheek just under your eye and gently pull down until a "V" pocket is formed between your eyeball and your lower lid.
3. Place a small amount (about 1/2 inch) of neomycin and polymyxin B sulfates and dexamethasone ophthalmic ointment in the "V" pocket. Do not let the tip of the tube touch your eye.
4. Look downward before closing your eye.
Not more than 8 g should be prescribed initially and the prescription should not be refilled without further evaluation as outlined in PRECAUTIONS above.
How is Neomycin,Polymyxin B,Dexamethasone Ointment supplied
Neomycin and polymyxin B sulfates and dexamethasone ophthalmic ointment is supplied as a STERILE ointment in an aluminum tube with a white polyethylene tip and white polyethylene cap as follows:
- 3.5 g in an aluminum tube NDC 61314-631-36
Storage: Store at 2°C to 25°C (36°F to 77°F).
After opening, neomycin and polymyxin B sulfates and dexamethasone ophthalmic ointment can be used until the expiration date on the tube.
Manufactured by
Novartis Manufacturing NV
Puurs-Sint-Amands, Belgium for
Sandoz Inc., Princeton, NJ 08540
Rev. 07/2024
9103458 US
| NEOMYCIN AND POLYMYXIN B SULFATES AND DEXAMETHASONE
neomycin and polymyxin b sulfates and dexamethasone ointment |
|||||||||||||||
|
|||||||||||||||
|
|||||||||||||||
|
|||||||||||||||
|
|||||||||||||||
|
|||||||||||||||
| Labeler - Sandoz Inc (005387188) |
More about dexamethasone / neomycin / polymyxin b ophthalmic
- Check interactions
- Compare alternatives
- Pricing & coupons
- Reviews (13)
- Side effects
- Dosage information
- During pregnancy
- Drug class: ophthalmic steroids with anti-infectives
- En español