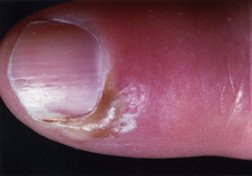
Paronychia
Medically reviewed by Drugs.com. Last updated on Nov 21, 2023.
What is Paronychia?

A paronychia is an infection of the skin that surrounds a toenail or fingernail. There are two different types of paronychia, acute and chronic:
|
|
- Acute paronychia — This usually appears as a sudden, very painful area of swelling, warmth and redness around a fingernail or toenail, usually after an injury to the area. An acute paronychia typically is caused by an infection with bacteria that invade the skin where it was injured. The injury can be caused by overaggressive manicuring (especially cutting or tearing the cuticle, which is the rim of paper-thin skin that outlines the outer margins of your nail). It can also result from biting the edges of the nails or the skin around the nails, picking at the skin near the nails or sucking on the fingers.
- Chronic paronychia — The condition is caused by inflammation that usually develops slowly, causing gradual swelling, tenderness and redness of the skin around the nails. It often affects several fingers on the same hand. People who are more likely to get this condition include those with diabetes, or workers whose jobs constantly expose their hands to water, chemicals, or substances to which they are allergic. Such jobs include bartending, house cleaning, janitorial work, dentistry, nursing, food service, dishwashing and hairdressing. Most often Candida (yeast) can be cultured from the area but appears not to be the cause in most cases.
Symptoms
An acute paronychia causes throbbing pain, redness, warmth and swelling in the skin around a nail. In some cases, a small collection of pus forms under the skin next to the nail, or underneath the nail itself. Often, only one nail is affected.
A chronic paronychia usually causes less dramatic symptoms than an acute paronychia. Typically, the area around the nail is tender, red and mildly swollen; the cuticle is missing; and the skin around the nail feels moist or "boggy." Several nails on the same hand may be affected at the same time.
Diagnosis
If you have a mild acute paronychia, you usually can make the diagnosis yourself. Look for throbbing pain, swelling and redness in an area of damaged skin around a nail.
If you are diabetic, have several affected fingers or toes, or have severe symptoms (pus, fever, severe pain), you must be evaluated by a doctor. In most cases, your doctor can make the diagnosis by examining the affected area. However, if there is an accumulation of pus, the doctor may take a sample of the pus to be tested in the laboratory for bacteria or fungi.
Expected duration
How long a paronychia lasts depends on the type of paronychia. With proper treatment, an acute paronychia usually heals within 5 to 10 days. A chronic paronychia may require several weeks of antifungal medication. Even after proper medical therapy, a paronychia may return if you injure the skin again or forget to keep the nail area dry.
Prevention
To prevent paronychia, try the following:
- Keep your hands and feet dry and clean.
- Wear rubber gloves with an absorbent cotton lining if your hands are exposed routinely to water or harsh chemicals.
- Be gentle when you manicure your nails. Avoid cutting your cuticles or pushing them back.
- Avoid biting your nails and picking at the skin around your nails.
- If you have diabetes, keep your blood sugar levels within a normal range by following your diet and taking your medications.
Drugs used to treat this and similar conditions
Treatment
The type of treatment depends on the type of paronychia:
- Acute paronychia — You can begin treating yourself by soaking the finger or toe in warm water. Do this for at least 15 minutes, two to four times a day. If your symptoms do not improve with this treatment, or if pus develops near the nail, call your doctor. If you have a moderate or severe paronychia, your doctor may treat it with an oral antibiotic. If pus has accumulated near the nail, the doctor will numb the area and drain the pus, and may prescribe a topical or oral antibiotic. If necessary, a small part of your nail will be removed to make sure that the area drains completely.
- Chronic paronychia — Since most cases of chronic paronychia are caused by inflammation with or without an allergic reaction, your doctor will likely recommend treatment with a topical corticosteroid ointment or cream with or without a topical antifungal agent. You also will be reminded to keep the skin clean and dry and wear gloves when potentially exposed to any irritants. Rarely, in severe cases, you will need to take antifungal drugs or steroids by mouth.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
When to call a professional
Call your doctor if you have symptoms of a paronychia and:
- you have diabetes
- you have an accumulation of pus near your nail or under it
- you have a fever
- the area of redness near your nail begins to spread up your finger
- you have milder symptoms (tenderness, mild redness, minimal swelling) that last for seven days or more.
Prognosis
With proper treatment, the outlook is usually very good. In most cases, an acute paronychia heals within 5 to 10 days with no permanent damage to the nail. Rarely, very severe cases may progress to osteomyelitis (a bone infection) of the finger or toe.
Although a chronic paronychia may take several weeks to heal, the skin and nail usually will return to normal eventually. However, you must remember to apply medication as directed, and to keep the affected area dry.
Additional info
National Institute of Arthritis and Musculoskeletal and Skin Diseases
https://www.niams.nih.gov/
American Academy of Dermatology
https://www.aad.org/
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.