Exchange Transfusion in Newborns
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
An exchange transfusion is a procedure to give your newborn baby donated blood. Your baby may need this procedure if he or she has jaundice or has a blood disorder such as Rh incompatibility or sickle cell anemia. Jaundice is caused by too much bilirubin in the blood. If your baby has jaundice, an exchange transfusion helps to remove bilirubin out of your baby's blood.
WHILE YOU ARE HERE:
Informed consent
is a legal document that explains the tests, treatments, or procedures that your child may need. Informed consent means you understand what will be done and can make decisions about what you want. You give your permission when you sign the consent form. You can have someone sign this form for you if you are not able to sign it. You have the right to understand your child's medical care in words you know. Before you sign the consent form, understand the risks and benefits of what will be done to your child. Make sure all of your questions are answered.
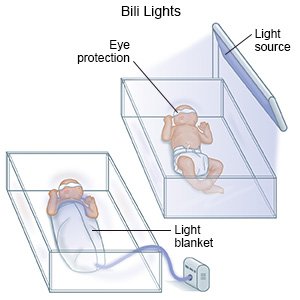
Bili lights:
Healthcare providers may use bili lights (phototherapy) or a lighted blanket to help decrease your baby's jaundice. Your baby may wear eye patches while he or she lies under or on the bili lights. Healthcare providers may keep the bili lights on during and after your baby's exchange transfusion.
 |
Blood tests:
Healthcare providers will take a sample of your baby's blood to test it before, during, and after the exchange transfusion. Blood gases help healthcare providers know how much oxygen, acids, and carbon dioxide are in your baby's blood. Other blood tests show healthcare providers how your baby's blood, heart, and other organs are doing. If your baby has jaundice, healthcare providers will watch his or her bilirubin level.
Heart monitor:
This is also called an ECG, or electrocardiogram. Sticky pads are placed on the chest or other parts of your baby's body. Each pad has a wire that is hooked to a monitor. This allows healthcare providers to see a tracing (picture) of your baby's heartbeat. Healthcare providers will watch the tracing closely during the procedure. The heart monitor helps healthcare providers make sure your baby is handling the procedure well.
Related medications
IV:
An IV will be placed in your baby's vein. Your baby may get medicine or liquids through the IV. Your baby will also get nutrition through the IV. Give your baby a pacifier to suck on if he or she is fussy or seems hungry. If you are breastfeeding, pump your breasts while your baby is using the IV. This helps your breasts to make milk even while your baby is not drinking it. Ask healthcare providers for information about pumping and storing breast milk. Keep your breast milk in a freezer until healthcare providers tell you that your baby can start drinking it.
Pulse oximeter:
A pulse oximeter is a device that measures the amount of oxygen in your baby's blood. A cord with a clip or sticky strip is placed on your baby's foot, toe, hand, finger, or earlobe. The other end of the cord is hooked to a machine. Never turn the pulse oximeter or alarm off. An alarm will sound if your baby's oxygen level is low or cannot be read.
During the procedure:
- Healthcare providers will place your baby on a flat bed with a heater over it. They will cover your baby's abdomen with a clean sheet that has a hole in the middle. Healthcare providers may put one or more IV tubes in your baby's umbilical cord stump. Healthcare providers will use these tubes to take your baby's blood out and put in healthy, new blood.
- Healthcare providers slowly remove a small amount of blood from your baby. Then they will slowly push the same amount of warm, new donor blood into your baby. They will repeat this until your baby has enough new, healthy blood. If your baby has polycythemia (blood that is too thick), healthcare providers may give IV fluid or plasma instead of blood. This helps your baby by making his or her blood a little thinner. Plasma is the clear part of the blood that does not have red blood cells in it.
After the procedure:
- Healthcare providers will do blood tests. They will watch your baby to make sure he or she does not need another exchange transfusion. They may then remove some of the IVs. When your baby is ready, healthcare providers may put him or her back in his or her regular bed.
- If your baby has jaundice, he or she will continue to lie on or under bili lights and have blood tests done. When his or her bilirubin level is low enough, healthcare providers will stop using the bili lights.
- Healthcare providers may start to feed milk or formula to your baby if he or she does not have other serious health problems. If your baby is full term, he or she may stay in the hospital 1 or 2 days after the procedure. If your baby has other health problems or was born prematurely, he or she may need to stay in the hospital longer.
RISKS:
Air bubbles or blood clots could form and cause heart or breathing problems. Your baby may develop bowel problems or get too warm or too cold. His or her blood could get too thick or too thin.
CARE AGREEMENT:
You have the right to help plan your baby's care. Learn about your baby's health condition and how it may be treated. Discuss treatment options with your baby's healthcare providers to decide what care you want for your baby.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
