Cirrhosis of the Liver
Medically reviewed by Drugs.com. Last updated on Nov 10, 2025.
What is cirrhosis?
Cirrhosis is long-term scarring of the liver. The liver makes enzymes and bile that help digest food and gives your body energy. It also removes harmful material from your body, such as alcohol and other chemicals. Cirrhosis is caused by repeated damage to your liver over time. Scar tissue starts to replace healthy liver tissue. The scar tissue prevents the liver from working properly.
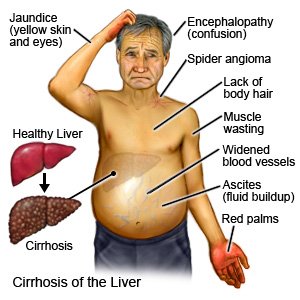 |
What increases my risk for cirrhosis?
- Long-term alcohol use
- Hepatitis B or C infection
- Fat or iron buildup in the liver
- A disease such as type 2 diabetes, cystic fibrosis, or a family history of liver cancer
- Long-term use of certain medicines, such as acetaminophen or anabolic steroids
- Damage to the bile ducts that blocks the flow of bile
- Obesity
What are the signs and symptoms of cirrhosis?
You may not have any signs or symptoms until your liver damage is severe. You may have any of the following:
- Fatigue (being mentally and physically tired)
- Bleeding and bruising easily
- Swelling of your feet, legs, or abdomen
- Nausea and vomiting, loss of appetite, and weight loss without trying
- Itching skin or jaundice (yellowing of your skin or the whites of your eyes)
- Pain or discomfort in the upper right part of your abdomen
- Black bowel movements or dark urine
How is cirrhosis diagnosed?
- Blood tests may be used to check your liver enzymes.
- An ultrasound may be used to check for damage to your liver or other tissues or organs.
- CT or MRI pictures may be taken of your liver. You may be given IV contrast liquid to help your liver show up better in the pictures. Tell the healthcare provider if you have ever had an allergic reaction to contrast liquid. Do not enter the MRI room with anything made of metal. Metal can cause serious injury. Tell the healthcare provider if you have any metal in or on your body.
- A liver biopsy is a procedure used to take a small piece of your liver to be tested for liver damage.
Related medications
How is cirrhosis treated?
- Medicines may be used to treat high blood pressure in the portal vein (the vein that goes to your liver). You may also need medicine to decrease extra fluid that collects in an area such as your legs or abdomen. Medicines may be used to decrease itching, or to treat a bacterial or viral infection.
- Surgery may be used to create a channel inside your liver to increase blood flow. This will help decrease swelling in your abdomen and lower blood pressure in the portal vein. Your risk for bleeding in your esophagus and stomach will also be decreased. You may need a liver transplant if your liver fails.
What can I do to manage or prevent cirrhosis?
- Do not drink alcohol. Alcohol will cause more damage to your liver. Ask your healthcare provider for information if you currently drink alcohol and need help to quit.
- Do not smoke. Nicotine and other chemicals in cigarettes and cigars can cause blood vessel and lung damage. Ask your provider for information if you currently smoke and need help to quit. E-cigarettes and smokeless tobacco still contain nicotine. Talk to your provider before you use these products.
- Eat a variety of healthy foods. Healthy foods include fruits, vegetables, whole-grain breads, low-fat dairy products, beans, lean meat, and fish. Ask if you need to be on a special diet.

- Reach or maintain a healthy weight. You may develop fatty liver disease if you are overweight. Ask your provider what a healthy weight is for you. Your provider can help you create a safe weight loss plan, if needed.
- Limit sodium (salt). You may need to decrease the amount of sodium you eat if you have swelling caused by fluid buildup. Sodium is found in table salt and salty foods such as canned foods, frozen foods, and potato chips.
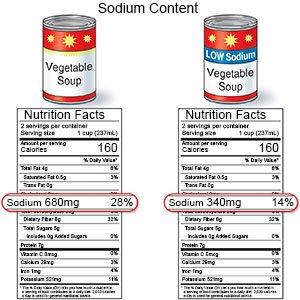
- Drink liquids as directed. Water and other liquids can help your liver work better. Ask how much liquid to drink each day and which liquids are best for you.
- Ask about vaccines. You may have a hard time fighting infection because of cirrhosis. Vaccines help protect you against viruses that can cause diseases such as the flu or hepatitis. Viral hepatitis is caused by a virus that leads to inflammation of the liver. You may need a hepatitis A or B vaccine. No vaccine is available for hepatitis C. Your provider can give you information on how to prevent a hepatitis C infection. You may also need a pneumonia vaccine. Always get a flu vaccine as soon as recommended each year, usually in September or October.
- Ask about medicines. Some medicines can harm your liver. Acetaminophen is an example. Talk to your provider about all your medicines. Do not take any over-the-counter medicine or herbal supplements until your provider says it is okay.
Call your local emergency number (911 in the US) or have someone call if:
- You have a seizure.
- You lose consciousness or cannot be woken.
- You have sudden shortness of breath or trouble breathing.
When should I seek immediate care?
- You have pain during a bowel movement and it is black or contains blood.
- You have a fast heart rate and fast breathing.
- You are dizzy or confused.
- You have severe pain in your abdomen.
- Your vomit looks like it has coffee grinds or blood in it.
Call your doctor if:
- You have a fever.
- You have red or itchy skin.
- You are in pain and feel weak.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Cirrhosis of the Liver
Treatment options
- Medications for Alcoholic Cirrhosis
- Medications for Cirrhosis
- Medications for Primary Biliary Cholangitis
Symptoms and treatments
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
