Appendicitis in Children
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is appendicitis?
Appendicitis is inflammation of your child's appendix. The appendix is a small pouch in the lower right side of the abdomen. It is attached to the first part of the large intestine. The appendix may get blocked or infected and become inflamed. Inflammation may cause your child's appendix to swell, fill with pus and burst. Your child will need immediate care to prevent a ruptured appendix. A ruptured appendix can cause bacteria to flow into the abdomen. This can lead to a serious infection called peritonitis.
 |
What are the signs and symptoms of appendicitis?
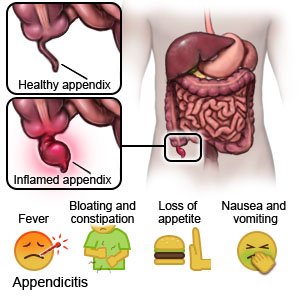
The most common symptom is pain that starts at the belly button and moves to the lower right side of the abdomen. Symptoms may start suddenly and get worse quickly. The pain worsens when your child touches his or her abdomen, moves, sneezes, coughs, or takes a deep breath. Appendicitis may be difficult to recognize in young children. Your young child may cry constantly or not want to be held or moved. Your older child may be able to tell you about any symptoms. Your child may also have any of the following:
- Abdominal swelling (most common in infants)
- Abdomen that feels hard or tender
- Diarrhea or constipation
- Loss of appetite
- Nausea or vomiting
- Fever
 |
How is appendicitis diagnosed?
Your healthcare provider will examine your child and check for pain or tenderness in the abdomen. Any of the following may also be needed:
- Blood tests may be used to check for signs of infection or inflammation.
- CT, ultrasound, or MRI pictures of your child's abdomen may be used to check the appendix. Your child may be given contrast liquid to help the appendix show up better in the pictures. Tell the healthcare provider if your child has ever had an allergic reaction to contrast liquid. Do not let your child enter the MRI room with anything metal. Metal can cause serious injury. Tell the healthcare provider if there is any metal in or on your child's body.
- A fluid culture test may be used if your child's appendix bursts. The provider may take a fluid sample from your child's abdomen during a drainage procedure or appendectomy. This test will show which bacteria is causing the infection.
Related medications
How is appendicitis treated?
- Medicines may be given to prevent or treat an infection, or to manage pain.
- Drainage may be needed if your child develops an abscess after a burst appendix. To drain the abscess, a tube is guided through the skin and into the abscess. Infected fluid drains through the tube.
- An appendectomy is surgery to remove your child's appendix. The appendix may be removed through small incisions in your child's abdomen. If your child's appendix has burst, he or she may need an open appendectomy. A single, larger incision is made to remove the appendix and clean out the abdomen.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
When should I seek immediate care?
- Your child has abdominal pain that gets worse or does not go away, even after he or she takes pain medicine.
- Your child is vomiting and cannot keep food down.
When should I call my child's doctor?
- Your child has a fever or shaking chills.
- Your child feels weak or sleepy.
- Your child is irritable and achy.
- Your child has trouble having a bowel movement, or has diarrhea.
- You have questions or concerns about your child's condition or care.
Care Agreement
You have the right to help plan your child's care. Learn about your child's health condition and how it may be treated. Discuss treatment options with your child's healthcare providers to decide what care you want for your child. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Appendicitis
Treatment options
Care guides
Symptoms and treatments
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
