Prograf: Package Insert / Prescribing Info
Package insert / product label
Generic name: tacrolimus
Dosage forms: capsule, gelatin coated, injection, solution
Drug class: Calcineurin inhibitors
J Codes (medical billing codes): J7507 (Per 1 mg, oral); J7521 (0.1 mg, granules, oral suspension); J7525 (5 mg, injection)
Medically reviewed by Drugs.com. Last updated on Oct 2, 2023.
On This Page
- Indications and Usage
- Dosage and Administration
- Dosage Forms and Strengths
- Contraindications
- Warnings and Precautions
- Adverse Reactions/Side Effects
- Drug Interactions
- Use In Specific Populations
- Overdosage
- Description
- Clinical Pharmacology
- Nonclinical Toxicology
- Clinical Studies
- References
- How Supplied/Storage and Handling
- Patient Counseling Information
Highlights of Prescribing Information
PROGRAF (tacrolimus) capsules, for oral use
PROGRAF (tacrolimus) injection, for intravenous use
PROGRAF Granules (tacrolimus for oral suspension)
Initial U.S. Approval: 1994
Recent Major Changes
Indications and Usage for Prograf
PROGRAF is a calcineurin-inhibitor immunosuppressant indicated for the prophylaxis of organ rejection in adult and pediatric patients receiving allogeneic liver, kidney, heart, or lung transplants, in combination with other immunosuppressants. (1.1)
Prograf Dosage and Administration
- •
- Intravenous (IV) use recommended for patients who cannot tolerate oral formulations (capsules or suspension). (2.1, 2.2)
- •
- Administer capsules or suspension consistently with or without food. (2.1)
- •
- Therapeutic drug monitoring is recommended. (2.1, 2.6)
- •
- Avoid eating grapefruit or drinking grapefruit juice. (2.1)
- •
- See dosage adjustments for African-American patients (2.2), hepatic and renal impaired. (2.4, 2.5)
- •
- For complete dosing information, see Full Prescribing Information.
| ADULT | ||
|---|---|---|
| Patient Population | Initial Oral Dosage (formulation) | Whole Blood Trough Concentration Range |
| Kidney Transplant | ||
| With azathioprine | 0.2 mg/kg/day capsules, divided in two doses, every 12 hours | Month 1-3: 7-20 ng/mL Month 4-12: 5-15 ng/mL |
| With MMF/IL-2 receptor antagonist | 0.1 mg/kg/day capsules, divided in two doses, every 12 hours | Month 1-12: 4-11 ng/mL |
| Liver Transplant | ||
| With corticosteroids only | 0.1-0.15 mg/kg/day capsules, divided in two doses, every 12 hours | Month 1-12: 5-20 ng/mL |
| Heart Transplant | ||
| With azathioprine or MMF | 0.075 mg/kg/day capsules, divided in two doses, every 12 hours | Month 1-3: 10-20 ng/mL Month ≥ 4: 5-15 ng/mL |
| Lung Transplant | ||
| With azathioprine or MMF | 0.075 mg/kg/day* capsules, divided in two doses, every 12 hours | Month 1-3: 10-15 ng/mL Month 4-12: 8-12 ng/mL |
| PEDIATRIC | ||
| Patient Population | Initial Oral Dosage (formulation) | Whole Blood Trough Concentration Range |
| Kidney Transplant | ||
| 0.3 mg/kg/day capsules or oral suspension, divided in two doses, every 12 hours | Month 1-12: 5-20 ng/mL | |
| Liver Transplant | ||
| 0.15-0.2 mg/kg/day capsules or 0.2 mg/kg/day oral suspension, divided in two doses, every 12 hours | Month 1-12: 5-20 ng/mL | |
| Heart Transplant | ||
| 0.3 mg/kg/day† capsules or oral suspension, divided in two doses, every 12 hours | Month 1-12: 5-20 ng/mL | |
| Lung Transplant | ||
| 0.3 mg/kg/day*, †capsules or oral suspension, divided in two doses, every 12 hours | Weeks 1-2: 10-20 ng/mL Week 2 to Month 12: 10-15 ng/mL | |
| MMF= Mycophenolate mofetil | ||
Dosage Forms and Strengths
Contraindications
- •
- Hypersensitivity to tacrolimus or HCO-60 (polyoxyl 60 hydrogenated castor oil). (4)
Warnings and Precautions
- •
- Not Interchangeable with Extended-Release Tacrolimus Products - Medication Errors: Instruct patients or caregivers to recognize the appearance of PROGRAF capsules. (5.3)
- •
- New Onset Diabetes After Transplant: Monitor blood glucose. (5.4)
- •
- Nephrotoxicity (acute and/or chronic): Reduce the dose; use caution with other nephrotoxic drugs. (5.5)
- •
- Neurotoxicity: Including risk of Posterior Reversible Encephalopathy Syndrome (PRES); monitor for neurologic abnormalities; reduce or discontinue PROGRAF. (5.6)
- •
- Hyperkalemia: Monitor serum potassium levels. Consider carefully before using with other agents also associated with hyperkalemia. (5.7)
- •
- Hypertension: May require antihypertensive therapy. Monitor relevant drug-drug interactions. (5.8)
- •
- Anaphylactic Reactions with IV formulation: Observe patients receiving PROGRAF injection for signs and symptoms of anaphylaxis. (5.9)
- •
- Not recommended for use with sirolimus: Not recommended in liver and heart transplant due to increased risk of serious adverse reactions. (5.10)
- •
- Myocardial Hypertrophy: Consider dose reduction/discontinuation. (5.13)
- •
- Immunizations: Avoid live vaccines. (5.14)
- •
- Pure Red Cell Aplasia: Consider discontinuation of PROGRAF. (5.15)
- •
- Thrombotic Microangiopathy, Including Hemolytic Uremic Syndrome and Thrombotic Thrombocytopenic Purpura: May occur, especially in patients with infections and certain concomitant medications. (5.16)
Adverse Reactions/Side Effects
The most common adverse reactions (≥ 15%) were abnormal renal function, hypertension, diabetes mellitus, fever, CMV infection, tremor, hyperglycemia, leukopenia, infection, anemia, bronchitis, pericardial effusion, urinary tract infection, constipation, diarrhea, headache, abdominal pain, insomnia, paresthesia, peripheral edema, nausea, hyperkalemia, hypomagnesemia, and hyperlipemia. (6.1)
To report SUSPECTED ADVERSE REACTIONS, contact Astellas Pharma US, Inc. at 1-800-727-7003 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
Drug Interactions
- •
- Mycophenolic Acid Products: Can increase MPA exposure after crossover from cyclosporine to PROGRAF; monitor for MPA-related adverse reactions and adjust MMF or MPA dose as needed. (7.1)
- •
- Nelfinavir and Grapefruit Juice: Increased tacrolimus concentrations via CYP3A inhibition; avoid concomitant use. (7.2)
- •
- CYP3A Inhibitors: Increased tacrolimus concentrations; monitor concentrations and adjust tacrolimus dose as needed. (5.11, 7.2)
- •
- CYP3A4 Inducers: Decreased tacrolimus concentrations; monitor concentrations and adjust tacrolimus dose as needed. (5.11, 7.2)
- •
- Therapeutic drug monitoring and dose reduction for PROGRAF should be considered when PROGRAF is co-administered with cannabidiol (5.17, 7.3).
Use In Specific Populations
See 17 for PATIENT COUNSELING INFORMATION and FDA-approved patient labeling.
Revised: 8/2023
Full Prescribing Information
WARNING: MALIGNANCIES AND SERIOUS INFECTIONS
Increased risk for developing serious infections and malignancies with PROGRAF or other immunosuppressants that may lead to hospitalization or death. (5.1, 5.2)
1. Indications and Usage for Prograf
1.1 Prophylaxis of Organ Rejection in Kidney, Liver, Heart, or Lung Transplant
PROGRAF® is indicated for the prophylaxis of organ rejection, in adult and pediatric patients receiving allogeneic kidney transplant [see Clinical Studies (14.1)], liver transplant [see Clinical Studies (14.2)], heart transplant [see Clinical Studies (14.3)], or lung transplant [see Clinical Studies (14.4)] in combination with other immunosuppressants.
2. Prograf Dosage and Administration
2.1 Important Administration Instructions
PROGRAF should not be used without supervision by a physician with experience in immunosuppressive therapy.
PROGRAF capsules and PROGRAF Granules are not interchangeable or substitutable for other tacrolimus extended-release products. This is because rate of absorption following the administration of an extended-release tacrolimus product is not equivalent to that of an immediate-release tacrolimus drug product. Under- or overexposure to tacrolimus may result in graft rejection or other serious adverse reactions. Changes between tacrolimus immediate-release and extended- release dosage forms must occur under physician supervision [see Warnings and Precautions (5.3)].
Intravenous Formulation - Administration Precautions due to Risk of Anaphylaxis
Intravenous use is recommended for patients who cannot tolerate oral formulations, and conversion from intravenous to oral PROGRAF is recommended as soon as oral therapy can be tolerated to minimize the risk of anaphylactic reactions that occurred with injectables containing castor oil derivatives [see Warnings and Precautions (5.9)].
Patients receiving PROGRAF injection should be under continuous observation for at least the first 30 minutes following the start of the infusion and at frequent intervals thereafter. If signs or symptoms of anaphylaxis occur, the infusion should be stopped. An aqueous solution of epinephrine should be available at the bedside as well as a source of oxygen.
Oral Formulations (Capsules and Oral Suspension)
If patients are able to initiate oral therapy, the recommended starting doses should be initiated. PROGRAF Granules for oral suspension or PROGRAF capsules may be taken with or without food. However, since the presence of food affects the bioavailability of PROGRAF, if taken with food, it should be taken consistently the same way each time [see Clinical Pharmacology (12.3)].
General Administration Instructions
Patients should not eat grapefruit or drink grapefruit juice in combination with PROGRAF [see Drug Interactions (7.2)].
PROGRAF should not be used simultaneously with cyclosporine. PROGRAF or cyclosporine should be discontinued at least 24 hours before initiating the other. In the presence of elevated PROGRAF or cyclosporine concentrations, dosing with the other drug usually should be further delayed.
Therapeutic drug monitoring (TDM) is recommended for all patients receiving PROGRAF [see Dosage and Administration (2.6)].
2.2 Dosage Recommendations for Adult Kidney, Liver, Heart, or Lung Transplant Patients - Capsules and Injection
Capsules
If patients are able to tolerate oral therapy, the recommended oral starting doses should be initiated. The initial dose of PROGRAF capsules should be administered no sooner than 6 hours after transplantation in the liver, heart, or lung transplant patients. In kidney transplant patients, the initial dose of PROGRAF capsules may be administered within 24 hours of transplantation, but should be delayed until renal function has recovered.
The initial oral PROGRAF capsule dosage recommendations for adult patients with kidney, liver, heart, or lung transplants and whole blood trough concentration range are shown in Table 1. Perform therapeutic drug monitoring (TDM) to ensure that patients are within the ranges listed in Table 1.
|
||
|
Patient Population |
PROGRAF Capsules* Initial Oral Dosage |
Whole Blood Trough Concentration Range |
|
Kidney Transplant |
||
|
With Azathioprine |
0.2 mg/kg/day, divided in two doses, administered every 12 hours |
Month 1-3: 7-20 ng/mL Month 4-12: 5-15 ng/mL |
|
With MMF/IL-2 receptor antagonist† |
0.1 mg/kg/day, divided in two doses, administered every 12 hours |
Month 1-12: 4-11 ng/mL |
|
Liver Transplant |
||
|
With corticosteroids only |
0.10-0.15 mg/kg/day, divided in two doses, administered every 12 hours |
Month 1-12: 5-20 ng/mL |
|
Heart Transplant |
||
|
With azathioprine or MMF |
0.075 mg/kg/day, divided in two doses, administered every 12 hours |
Month 1-3: 10-20 ng/mL Month ≥ 4: 5-15 ng/mL |
|
Lung Transplant |
||
|
With azathioprine or MMF |
0.075 mg/kg/day‡, divided in two doses, administered every 12 hours |
Month 1-3: 10-15 ng/mL Month 4-12: 8-12 ng/mL |
Dosage should be titrated based on clinical assessments of rejection and tolerability. PROGRAF dosages lower than the recommended initial dosage may be sufficient as maintenance therapy. Adjunct therapy with adrenal corticosteroids is recommended early post-transplant.
The data in kidney transplant patients indicate that the African-American patients required a higher dose to attain comparable trough concentrations compared to Caucasian patients (Table 2) [see Use in Specific Populations (8.8) and Clinical Pharmacology (12.3)].
|
Time After Transplant |
Caucasian N = 114 |
African-American N = 56 |
||
|
Dose (mg/kg) |
Trough Concentrations (ng/mL) |
Dose (mg/kg) |
Trough Concentrations (ng/mL) |
|
|
Day 7 |
0.18 |
12.0 |
0.23 |
10.9 |
|
Month 1 |
0.17 |
12.8 |
0.26 |
12.9 |
|
Month 6 |
0.14 |
11.8 |
0.24 |
11.5 |
|
Month 12 |
0.13 |
10.1 |
0.19 |
11.0 |
In lung transplantation, cystic fibrosis patients may have a reduced bioavailability of orally administered tacrolimus resulting in the need for higher doses to achieve target tacrolimus trough concentrations. Monitor tacrolimus trough concentrations and adjust the dose accordingly.
Intravenous Injection
PROGRAF injection should be used only as a continuous intravenous infusion and should be discontinued as soon as the patient can tolerate oral administration. The first dose of PROGRAF capsules should be given 8-12 hours after discontinuing the intravenous infusion.
The recommended starting dose of PROGRAF injection is 0.03-0.05 mg/kg/day in kidney or liver transplant, 0.01 mg/kg/day in heart transplant, and 0.01-0.03 mg/kg/day in lung transplant, given as a continuous intravenous infusion. Adult patients should receive doses at the lower end of the dosing range. Concomitant adrenal corticosteroid therapy is recommended early post-transplantation.
The whole blood trough concentration range described in Table 1 pertains to oral administration of PROGRAF only; while monitoring PROGRAF concentrations in patients receiving PROGRAF injection as a continuous intravenous infusion may have some utility, the observed concentrations will not represent comparable exposures to those estimated by the trough concentrations observed in patients on oral therapy.
Anaphylactic reactions have occurred with injectables containing castor oil derivatives, such as PROGRAF injection. Therefore, monitoring for signs and symptoms of anaphylaxis is recommended [see Warnings and Precautions (5.9)].
2.3 Dosage Recommendations for Pediatric Kidney, Liver, Heart, or Lung Transplant Patients
Oral formulations (capsules or oral suspension)
Pediatric patients, in general, need higher tacrolimus doses compared to adults: the higher dose requirements may decrease as the child grows older. Recommendations for the initial oral dosage for pediatric transplant patients and whole blood trough concentration range are shown in Table 3. Perform TDM to ensure that patients are within the ranges listed in Table 3.
|
||
|
Patient Population |
Initial PROGRAF Capsule and PROGRAF Granules Dosing |
Whole Blood Trough Concentration Range |
|
Pediatric kidney transplant patients* |
0.3 mg/kg/day capsules or oral suspension, divided in two doses, administered every 12 hours |
Month 1-12: 5-20 ng/mL |
|
Pediatric liver transplant patients† |
0.15-0.2 mg/kg/day capsules or 0.2 mg/kg/day oral suspension, divided in two doses, administered every 12 hours |
Month 1-12: 5-20 ng/mL |
|
Pediatric heart transplant patients* |
0.3 mg/kg/day‡ capsules or oral suspension, divided in two doses, administered every 12 hours |
Month 1-12: 5-20 ng/mL |
|
Pediatric lung transplant patients |
0.3 mg/kg/day‡,§ capsules or oral suspension, divided in two doses, administered every 12 hours |
Week 1-2: 10-20 ng/mL Week 2 to Month 12: 10-15 ng/mL |
In lung transplantation, cystic fibrosis patients may have a reduced bioavailability of orally administered tacrolimus resulting in the need for higher doses to achieve target tacrolimus trough concentrations. Monitor tacrolimus trough concentrations and adjust the dose accordingly.
For conversion of pediatric patients from PROGRAF Granules to PROGRAF capsules or from PROGRAF capsules to PROGRAF Granules, the total daily dose should remain the same. Following conversion from one formulation to another formulation of tacrolimus, therapeutic drug monitoring is recommended [see Dosage and Administration (2.6)].
Intravenous Injection
If a patient is unable to receive an oral formulation, the patient may be started on PROGRAF injection. For pediatric liver transplant patients, the intravenous dose is 0.03-0.05 mg/kg/day.
2.4 Dosage Modification for Patients with Renal Impairment
Due to its potential for nephrotoxicity, consider dosing PROGRAF at the lower end of the therapeutic dosing range in patients who have received a liver, heart, or lung transplant, and have pre-existing renal impairment. Further reductions in dose below the targeted range may be required.
In kidney transplant patients with post-operative oliguria, the initial dose of PROGRAF should be administered no sooner than 6 hours and within 24 hours of transplantation, but may be delayed until renal function shows evidence of recovery [see Dosage and Administration (2.2), Warnings and Precautions (5.5), Use in Specific Populations (8.6), and Clinical Pharmacology (12.3)].
2.5 Dosage Modification for Patients with Hepatic Impairment
Due to the reduced clearance and prolonged half-life, patients with severe hepatic impairment (Child-Pugh ≥ 10) may require lower doses of PROGRAF. Close monitoring of blood concentrations is warranted.
The use of PROGRAF in liver transplant recipients experiencing post-transplant hepatic impairment may be associated with increased risk of developing renal insufficiency related to high whole blood concentrations of tacrolimus. These patients should be monitored closely, and dosage adjustments should be considered. Some evidence suggests that lower doses should be used in these patients [see Dosage and Administration (2.2), Warnings and Precautions (5.5), Use in Specific Populations (8.7), and Clinical Pharmacology (12.3)].
2.6 Therapeutic Drug Monitoring
Monitoring of tacrolimus blood concentrations in conjunction with other laboratory and clinical parameters is considered an essential aid to patient management for the evaluation of rejection, toxicity, dose adjustments, and compliance. Whole blood trough concentration range can be found in Table 1.
Factors influencing frequency of monitoring include but are not limited to hepatic or renal dysfunction, the addition or discontinuation of potentially interacting drugs and the post-transplant time. Blood concentration monitoring is not a replacement for renal and liver function monitoring and tissue biopsies. Data from clinical trials show that tacrolimus whole blood concentrations were most variable during the first week post-transplantation.
The relative risks of toxicity and efficacy failure are related to tacrolimus whole blood trough concentrations. Therefore, monitoring of whole blood trough concentrations is recommended to assist in the clinical evaluation of toxicity and efficacy failure.
Methods commonly used for the assay of tacrolimus include high-performance liquid chromatography with tandem mass spectrometric detection (HPLC/MS/MS) and immunoassays. Immunoassays may react with metabolites as well as parent compound. Therefore, assay results obtained with immunoassays may have a positive bias relative to results of HPLC/MS. The bias may depend upon the specific assay and laboratory. Comparison of the concentrations in published literature to patient concentrations using the current assays must be made with detailed knowledge of the assay methods and biological matrices employed. Whole blood is the matrix of choice and specimens should be collected into tubes containing ethylene diamine tetraacetic acid (EDTA) anticoagulant. Heparin anticoagulation is not recommended because of the tendency to form clots on storage. Samples which are not analyzed immediately should be stored at room temperature or in a refrigerator and assayed within 7 days; see assay instructions for specifics. If samples are to be kept longer, they should be deep frozen at -20°C. One study showed drug recovery > 90% for samples stored at -20°C for 6 months, with reduced recovery observed after 6 months.
2.7 Preparation and Administration Instructions of PROGRAF Injection for Pharmacists
Tacrolimus can cause fetal harm. Follow applicable special handling and disposal procedures1 [see How Supplied/ Storage and Handling (16.4)].
PROGRAF injection must be diluted with 0.9% Sodium Chloride Injection or 5% Dextrose Injection to a concentration between 0.004 mg/mL and 0.02 mg/mL prior to use. Diluted infusion solution should be stored in glass or polyethylene containers and should be discarded after 24 hours. The diluted infusion solution should not be stored in a polyvinyl chloride (PVC) container due to decreased stability and the potential for extraction of phthalates. In situations where more dilute solutions are utilized (e.g., pediatric dosing, etc.), PVC-free tubing should likewise be used to minimize the potential for significant drug adsorption onto the tubing.
Parenteral drug products should be inspected visually for particulate matter and discoloration prior to administration, whenever solution and container permit.
Due to the chemical instability of tacrolimus in alkaline media, PROGRAF injection should not be mixed or co-infused with solutions of pH 9 or greater (e.g., ganciclovir or acyclovir).
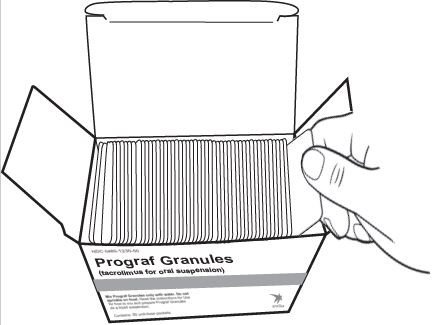
2.8 Preparation and Administration Instructions of PROGRAF Granules
Tacrolimus can cause fetal harm. Follow applicable special handling and disposal procedures1 [see How Supplied/ Storage and Handling (16.4)].
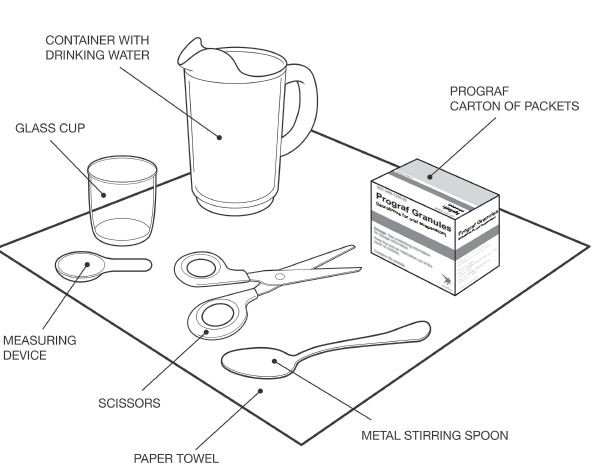
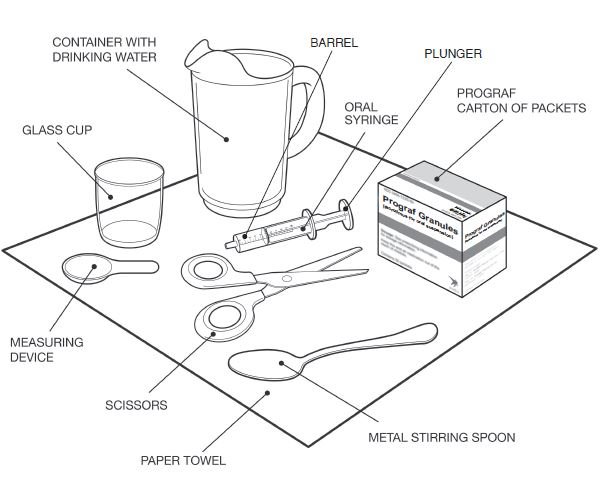
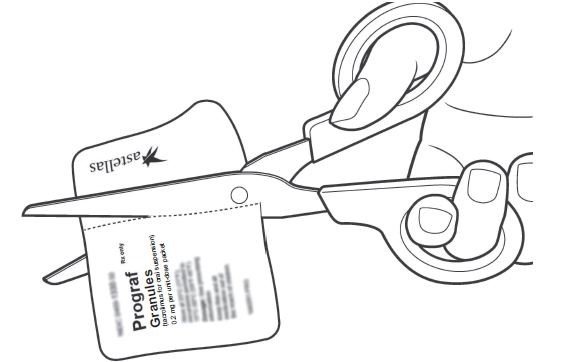
The required dose for PROGRAF Granules is calculated based on the weight of the patient. Use the minimum whole number of packets that corresponds to the required morning or evening dose. If the morning or evening dose is not covered by the whole number of packets, use one additional 0.2 mg packet to round up the dose. Do not use tubing, syringes and other equipment (cups) containing PVC to prepare or administer tacrolimus products. Do not sprinkle PROGRAF Granules on food. Prepare and administer PROGRAF Granules as follows:
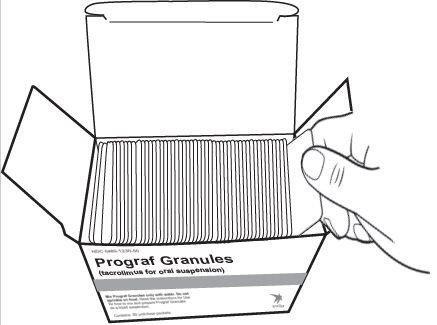
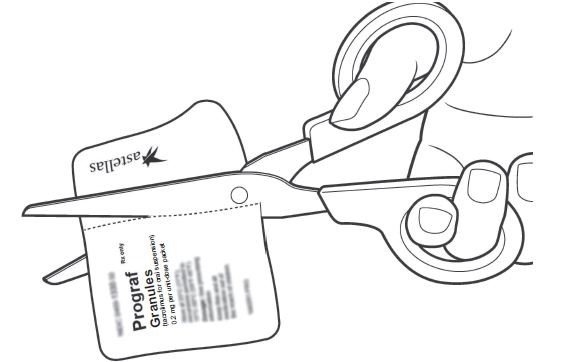
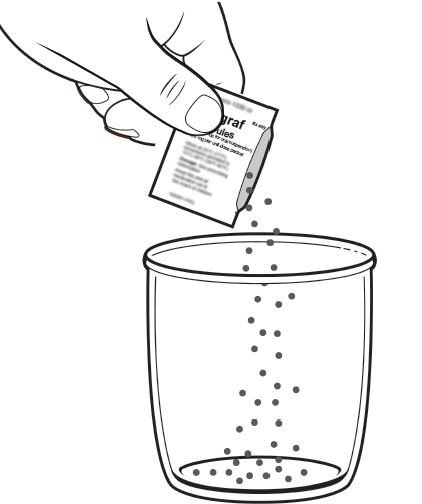
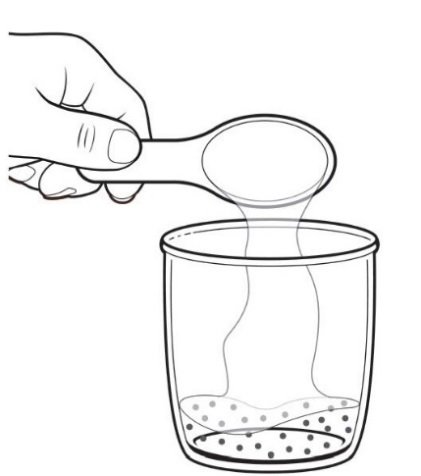
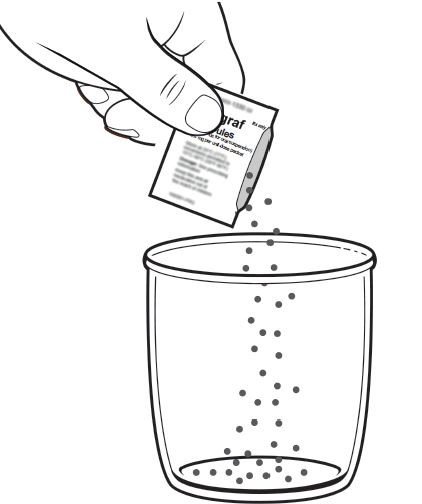
• To prepare the dose, empty the entire contents of each PROGRAF Granules packet into a glass cup. Check for any remaining granules in the packet(s) and empty these into the cup.
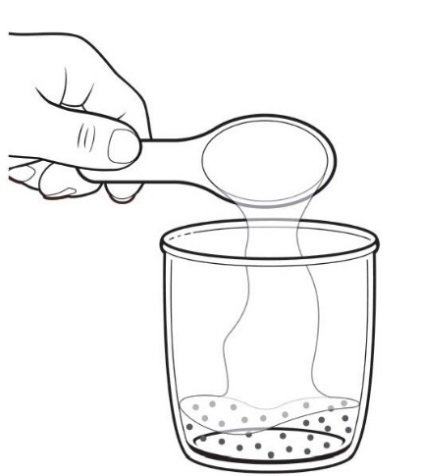
• Add 1 to 2 tablespoons (15 to 30 milliliters) of room temperature drinking water to the cup containing the PROGRAF Granules.
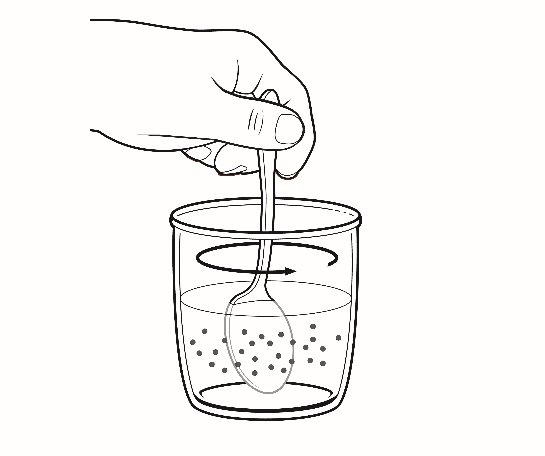
• Mix and administer the entire contents of the cup. The granules will not completely dissolve. The suspension should be given immediately after preparation.
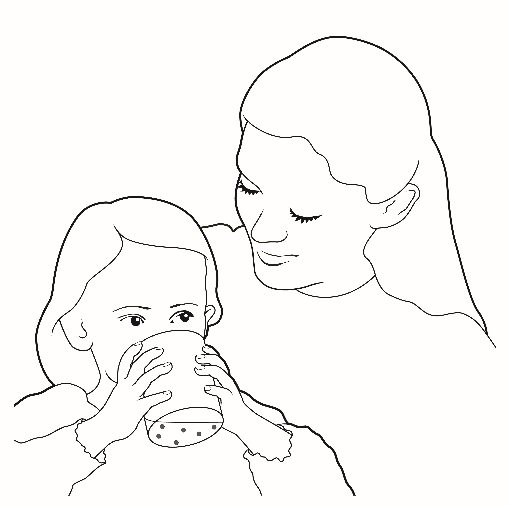
• For younger patients, the suspension can be drawn up via a non-PVC oral syringe that will be dispensed with the prescription.
• The cup or syringe should be rinsed with the same quantity of water (15 to 30 milliliters) and given to the patient to ensure all of the medication is taken.
• The pharmacy must dispense with the Instructions for Use. Alert the patient to read the Instructions for Use.
3. Dosage Forms and Strengths
PROGRAF is available in the following dosage forms and strengths:
4. Contraindications
PROGRAF is contraindicated in patients with a hypersensitivity to tacrolimus. PROGRAF injection is contraindicated in patients with a hypersensitivity to HCO-60 (polyoxyl 60 hydrogenated castor oil). Hypersensitivity symptoms reported include dyspnea, rash, pruritus, and acute respiratory distress syndrome [see Adverse Reactions (6)].
5. Warnings and Precautions
5.1 Lymphoma and Other Malignancies
Patients receiving immunosuppressants, including PROGRAF, are at increased risk of developing lymphomas and other malignancies, particularly of the skin. The risk appears to be related to the intensity and duration of immunosuppression rather than to the use of any specific agent.
As usual for patients with increased risk for skin cancer, examine patients for skin changes; exposure to sunlight and UV light should be limited by wearing protective clothing and using a broad-spectrum sunscreen with a high protection factor.
Post-transplant lymphoproliferative disorder (PTLD) has been reported in immunosuppressed organ transplant recipients. The majority of PTLD events appear related to Epstein-Barr Virus (EBV) infection. The risk of PTLD appears greatest in those individuals who are EBV seronegative, a population which includes many young children. Monitor EBV serology during treatment.
5.2 Serious Infections
Patients receiving immunosuppressants, including PROGRAF, are at increased risk of developing bacterial, viral, fungal, and protozoal infections, including opportunistic infections. These infections may lead to serious, including fatal, outcomes. Serious viral infections reported include:
- •
- Polyomavirus-associated nephropathy (PVAN), mostly due to BK virus infection
- •
- JC virus-associated progressive multifocal leukoencephalopathy (PML)
- •
- Cytomegalovirus infections: CMV seronegative transplant patients who receive an organ from a CMV seropositive donor disease are at higher risk of developing CMV viremia and CMV disease.
Monitor for the development of infection and adjust the immunosuppressive regimen to balance the risk of rejection with the risk of infection [see Adverse Reactions (6.1, 6.2)].
5.3 Not Interchangeable with Extended-Release Tacrolimus Products - Medication Errors
Medication errors, including substitution and dispensing errors, between tacrolimus immediate-release products and tacrolimus extended-release products were reported outside the U.S. This led to serious adverse reactions, including graft rejection, or other adverse reactions due to under- or overexposure to tacrolimus. PROGRAF is not interchangeable or substitutable for tacrolimus extended-release products. Changes between tacrolimus immediate-release and extended-release dosage forms must occur under physician supervision. Instruct patients and caregivers to recognize the appearance of PROGRAF dosage forms [see Dosage Forms and Strengths (3)] and to confirm with the healthcare provider if a different product is dispensed.
5.4 New Onset Diabetes After Transplant
PROGRAF was shown to cause new onset diabetes mellitus in clinical trials of kidney, liver, heart, or lung transplantation. New onset diabetes after transplantation may be reversible in some patients. African-American and Hispanic kidney transplant patients are at an increased risk. Blood glucose concentrations should be monitored closely in patients using PROGRAF [see Adverse Reactions (6.1)].
5.5 Nephrotoxicity due to PROGRAF and Drug Interactions
PROGRAF, like other calcineurin inhibitors, can cause acute or chronic nephrotoxicity in transplant patients due to its vasoconstrictive effect on renal vasculature, toxic tubulopathy and tubular-interstitial effects. Nephrotoxicity was reported in clinical trials [see Adverse Reactions (6.1)].
Acute renal impairment associated with tacrolimus toxicity can result in high serum creatinine, hyperkalemia, decreased secretion of urea and hyperuricemia, and is usually reversible. In patients with elevated serum creatinine and tacrolimus whole blood trough concentrations greater than the recommended range, consider dosage reduction or temporary interruption of tacrolimus administration.
The risk for nephrotoxicity may increase when PROGRAF is concomitantly administered with CYP3A inhibitors (by increasing tacrolimus whole blood concentrations) or drugs associated with nephrotoxicity (e.g., aminoglycosides, ganciclovir, amphotericin B, cisplatin, nucleotide reverse transcriptase inhibitors, protease inhibitors). When tacrolimus is used concurrently with other known nephrotoxic drugs, monitor renal function and tacrolimus blood concentrations, and adjust doses of both tacrolimus and/or concomitant medications during concurrent use [see Drug Interactions (7.2)].
5.6 Neurotoxicity
PROGRAF may cause a spectrum of neurotoxicities. The most severe neurotoxicities include posterior reversible encephalopathy syndrome (PRES), delirium, seizure and coma; others include tremors, paresthesias, headache, mental status changes, and changes in motor and sensory functions [see Adverse Reactions (6.1, 6.2)]. As symptoms may be associated with tacrolimus whole blood trough concentrations at or above the recommended range, monitor for neurologic symptoms and consider dosage reduction or discontinuation of PROGRAF if neurotoxicity occurs.
5.7 Hyperkalemia
Hyperkalemia has been reported with PROGRAF use. Serum potassium levels should be monitored. Careful consideration should be given prior to use of other agents also associated with hyperkalemia (e.g., potassium-sparing diuretics, ACE inhibitors, angiotensin receptor blockers) during PROGRAF therapy [see Adverse Reactions (6.1)]. Monitor serum potassium levels periodically during treatment.
5.8 Hypertension
Hypertension is a common adverse effect of PROGRAF therapy and may require antihypertensive therapy [see Adverse Reactions (6.1)]. The control of blood pressure can be accomplished with any of the common antihypertensive agents, though careful consideration should be given prior to use of antihypertensive agents associated with hyperkalemia (e.g., potassium-sparing diuretics, ACE inhibitors, angiotensin receptor blockers) [see Warnings and Precautions (5.7)]. Calcium-channel blocking agents may increase tacrolimus blood concentrations and therefore require dosage reduction of PROGRAF [see Drug Interactions (7.2)].
5.9 Anaphylactic Reactions with PROGRAF Injection
Anaphylactic reactions have occurred with injectables containing castor oil derivatives, including PROGRAF, in a small percentage of patients (0.6%). The exact cause of these reactions is not known. PROGRAF injection should be reserved for patients who are unable to take PROGRAF orally. Monitor patients for anaphylaxis when using the intravenous route of administration [see Dosage and Administration (2.1)].
5.10 Not Recommended for Use with Sirolimus
PROGRAF is not recommended for use with sirolimus:
• The use of sirolimus with PROGRAF in studies of de novo liver transplant patients was associated with an excess mortality, graft loss, and hepatic artery thrombosis (HAT), and is not recommended.
• The use of sirolimus (2 mg per day) with PROGRAF in heart transplant patients in a U.S. trial was associated with increased risk of renal function impairment, wound healing complications, and insulin-dependent post-transplant diabetes mellitus, and is not recommended [see Clinical Studies (14.3)].
• The use of sirolimus with PROGRAF may increase the risk of thrombotic microangiopathy [see Warnings and Precautions (5.16)].
5.11 Interactions with CYP3A4 Inhibitors and Inducers
When co-administering PROGRAF with strong CYP3A4 inhibitors (e.g., telaprevir, boceprevir, ritonavir, ketoconazole, itraconazole, voriconazole, clarithromycin) and strong inducers (e.g., rifampin, rifabutin), adjustments in the dosing regimen of PROGRAF and subsequent frequent monitoring of tacrolimus whole blood trough concentrations and tacrolimus-associated adverse reactions are recommended. A rapid, sharp rise in tacrolimus levels has been reported after co-administration with a strong CYP3A4 inhibitor, clarithromycin, despite an initial reduction of tacrolimus dose. Early and frequent monitoring of tacrolimus whole blood trough levels is recommended [see Drug Interactions (7.2)].
5.12 QT Prolongation
PROGRAF may prolong the QT/QTc interval and may cause Torsades de pointes. Avoid PROGRAF in patients with congenital long QT syndrome. In patients with congestive heart failure, bradyarrhythmias, those taking certain antiarrhythmic medications or other medicinal products that lead to QT prolongation, and those with electrolyte disturbances such as hypokalemia, hypocalcemia, or hypomagnesemia, consider obtaining electrocardiograms and monitoring electrolytes (magnesium, potassium, calcium) periodically during treatment.
When co-administering PROGRAF with other substrates and/or inhibitors of CYP3A4 that also have the potential to prolong the QT interval, a reduction in PROGRAF dose, frequent monitoring of tacrolimus whole blood concentrations, and monitoring for QT prolongation is recommended. Use of PROGRAF with amiodarone has been reported to result in increased tacrolimus whole blood concentrations with or without concurrent QT prolongation [see Drug Interactions (7.2)].
5.13 Myocardial Hypertrophy
Myocardial hypertrophy has been reported in infants, children, and adults, particularly those with high tacrolimus trough concentrations, and is generally manifested by echocardiographically demonstrated concentric increases in left ventricular posterior wall and interventricular septum thickness. This condition appears reversible in most cases following dose reduction or discontinuance of therapy. In patients who develop renal failure or clinical manifestations of ventricular dysfunction while receiving PROGRAF therapy, echocardiographic evaluation should be considered. If myocardial hypertrophy is diagnosed, dosage reduction or discontinuation of PROGRAF should be considered [see Adverse Reactions (6.2)].
5.14 Immunizations
Whenever possible, administer the complete complement of vaccines before transplantation and treatment with PROGRAF.
The use of live vaccines should be avoided during treatment with tacrolimus; examples include (not limited to) the following: intranasal influenza, measles, mumps, rubella, oral polio, BCG, yellow fever, varicella, and TY21a typhoid vaccines.
Inactivated vaccines noted to be safe for administration after transplantation may not be sufficiently immunogenic during treatment with PROGRAF.
5.15 Pure Red Cell Aplasia
Cases of pure red cell aplasia (PRCA) have been reported in patients treated with tacrolimus. A mechanism for tacrolimus-induced PRCA has not been elucidated. All patients reported risk factors for PRCA such as parvovirus B19 infection, underlying disease, or concomitant medications associated with PRCA. If PRCA is diagnosed, discontinuation of PROGRAF should be considered [see Adverse Reactions (6.2)].
5.16 Thrombotic Microangiopathy (Including Hemolytic Uremic Syndrome and Thrombotic Thrombocytopenic Purpura)
Cases of thrombotic microangiopathy (TMA), including hemolytic uremic syndrome (HUS) and thrombotic thrombocytopenic purpura (TTP), have been reported in patients treated with PROGRAF. TMA may have a multifactorial etiology. Risk factors for TMA that can occur in transplant patients include, for example, severe infections, graft-versus-host disease (GVHD), Human Leukocyte Antigen (HLA) mismatch, the use of calcineurin inhibitors and mammalian target of rapamycin (mTOR) inhibitors. These risk factors may, either alone or combined, contribute to the risk of TMA.
In patients with signs and symptoms of TMA, consider tacrolimus as a risk factor. Concurrent use of tacrolimus and mTOR inhibitors may contribute to the risk of TMA.
5.17 Cannabidiol Drug Interactions
When cannabidiol and PROGRAF are co-administered, closely monitor for an increase in tacrolimus blood levels and for adverse reactions suggestive of tacrolimus toxicity. A dose reduction of PROGRAF should be considered as needed when PROGRAF is co-administered with cannabidiol [see Dosage and Administration (2.2, 2.6) and Drug Interactions (7.3)].
6. Adverse Reactions/Side Effects
The following serious and otherwise important adverse drug reactions are discussed in greater detail in other sections of labeling:
- •
- Lymphoma and Other Malignancies [see Warnings and Precautions (5.1)]
- •
- Serious Infections [see Warnings and Precautions (5.2)]
- •
- New Onset Diabetes After Transplant [see Warnings and Precautions (5.4)]
- •
- Nephrotoxicity [see Warnings and Precautions (5.5)]
- •
- Neurotoxicity [see Warnings and Precautions (5.6)]
- •
- Hyperkalemia [see Warnings and Precautions (5.7)]
- •
- Hypertension [see Warnings and Precautions (5.8)]
- •
- Anaphylactic Reactions with PROGRAF Injection [see Warnings and Precautions (5.9)]
- •
- Myocardial Hypertrophy [see Warnings and Precautions (5.13)]
- •
- Pure Red Cell Aplasia [see Warnings and Precautions (5.15)]
- •
- Thrombotic Microangiopathy, Including Hemolytic Uremic Syndrome and Thrombotic Thrombocytopenic Purpura [see Warnings and Precautions (5.16)]
6.1 Clinical Studies Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice. In addition, the clinical trials were not designed to establish comparative differences across study arms with regards to the adverse reactions discussed below.
Kidney Transplantation
The incidence of adverse reactions was determined in three randomized kidney transplant trials. One of the trials used azathioprine (AZA) and corticosteroids and two of the trials used mycophenolate mofetil (MMF) and corticosteroids concomitantly for maintenance immunosuppression.
PROGRAF-based immunosuppression in conjunction with azathioprine and corticosteroids following kidney transplantation was assessed in a trial where 205 patients received PROGRAF-based immunosuppression and 207 patients received cyclosporine-based immunosuppression. The trial population had a mean age of 43 years (mean ± SD was 43 ± 13 years on PROGRAF and 44 ± 12 years on cyclosporine arm), the distribution was 61% male, and the composition was White (58%), African-American (25%), Hispanic (12%), and Other (5%). The 12-month post-transplant information from this trial is presented below.
The most common adverse reactions (≥ 30%) observed in PROGRAF-treated kidney transplant patients are: infection, tremor, hypertension, abnormal renal function, constipation, diarrhea, headache, abdominal pain, insomnia, nausea, hypomagnesemia, urinary tract infection, hypophosphatemia, peripheral edema, asthenia, pain, hyperlipidemia, hyperkalemia, and anemia. Based on reported adverse reaction terms related to decreased renal function, nephrotoxicity was reported in approximately 52% of kidney transplantation patients.
Adverse reactions that occurred in ≥ 15% of kidney transplant patients treated with PROGRAF in conjunction with azathioprine are presented below:
| PROGRAF/AZA
(N = 205) | Cyclosporine/AZA
(N = 207) |
|
|---|---|---|
|
Nervous System |
||
|
Tremor |
54% |
34% |
|
Headache |
44% |
38% |
|
Insomnia |
32% |
30% |
|
Paresthesia |
23% |
16% |
|
Dizziness |
19% |
16% |
|
Gastrointestinal |
||
|
Diarrhea |
44% |
41% |
|
Nausea |
38% |
36% |
|
Constipation |
35% |
43% |
|
Vomiting |
29% |
23% |
|
Dyspepsia |
28% |
20% |
|
Cardiovascular |
||
|
Hypertension |
50% |
52% |
|
Chest Pain |
19% |
13% |
|
Urogenital |
||
|
Creatinine Increased |
45% |
42% |
|
Urinary Tract Infection |
34% |
35% |
|
Metabolic and Nutritional |
||
|
Hypophosphatemia |
49% |
53% |
|
Hypomagnesemia |
34% |
17% |
|
Hyperlipemia |
31% |
38% |
|
Hyperkalemia |
31% |
32% |
|
Diabetes Mellitus |
24% |
9% |
|
Hypokalemia |
22% |
25% |
|
Hyperglycemia |
22% |
16% |
|
Edema |
18% |
19% |
|
Hemic and Lymphatic |
||
|
Anemia |
30% |
24% |
|
Leukopenia |
15% |
17% |
|
Miscellaneous |
||
|
Infection |
45% |
49% |
|
Peripheral Edema |
36% |
48% |
|
Asthenia |
34% |
30% |
|
Abdominal Pain |
33% |
31% |
|
Pain |
32% |
30% |
|
Fever |
29% |
29% |
|
Back Pain |
24% |
20% |
|
Respiratory System |
||
|
Dyspnea |
22% |
18% |
|
Cough Increased |
18% |
15% |
|
Musculoskeletal |
||
|
Arthralgia |
25% |
24% |
|
Skin |
||
|
Rash |
17% |
12% |
|
Pruritus |
15% |
7% |
Two trials were conducted for PROGRAF-based immunosuppression in conjunction with MMF and corticosteroids. In the non-US trial (Study 1), the incidence of adverse reactions was based on 1195 kidney transplant patients that received PROGRAF (Group C, n = 403), or one of two cyclosporine (CsA) regimens (Group A, n = 384 and Group B, n = 408) in combination with MMF and corticosteroids; all patients, except those in one of the two cyclosporine groups, also received induction with daclizumab. The trial population had a mean age of 46 years (range 17 to 76); the distribution was 65% male, and the composition was 93% Caucasian. The 12-month post-transplant information from this trial is presented below.
Adverse reactions that occurred in ≥ 10% of kidney transplant patients treated with PROGRAF in conjunction with MMF in Study 1 [Note: This trial was conducted entirely outside of the United States. Such trials often report a lower incidence of adverse reactions in comparison to U.S. trials] are presented below:
|
|
PROGRAF
(N = 403) |
Cyclosporine
(N = 384) |
Cyclosporine
(N = 408) |
|
Diarrhea |
25% |
16% |
13% |
|
Urinary Tract Infection |
24% |
28% |
24% |
|
Anemia |
17% |
19% |
17% |
|
Hypertension |
13% |
14% |
12% |
|
Leukopenia |
13% |
10% |
10% |
|
Edema Peripheral |
11% |
12% |
13% |
|
Hyperlipidemia |
10% |
15% |
13% |
|
Key: Group A = CsA/MMF/CS, B = CsA/MMF/CS/Daclizumab, C = Tac/MMF/CS/Daclizumab |
|||
In the U.S. trial (Study 2) with PROGRAF-based immunosuppression in conjunction with MMF and corticosteroids, 424 kidney transplant patients received PROGRAF (n = 212) or cyclosporine (n = 212) in combination with MMF 1 gram twice daily, basiliximab induction, and corticosteroids. The trial population had a mean age of 48 years (range 17 to 77); the distribution was 63% male, and the composition was White (74%), African-American (20%), Asian (3%), and Other (3%). The 12-month post-transplant information from this trial is presented below.
Adverse reactions that occurred in ≥ 15% of kidney transplant patients treated with PROGRAF in conjunction with MMF in Study 2 are presented below:
| PROGRAF/MMF | Cyclosporine/MMF | |
|---|---|---|
| (N = 212) | (N = 212) | |
|
Gastrointestinal Disorders | ||
|
Diarrhea |
44% |
26% |
|
Nausea |
39% |
47% |
|
Constipation |
36% |
41% |
|
Vomiting |
26% |
25% |
|
Dyspepsia |
18% |
15% |
|
Injury, Poisoning, and Procedural Complications | ||
|
Post-Procedural Pain |
29% |
27% |
|
Incision Site Complication |
28% |
23% |
|
Graft Dysfunction |
24% |
18% |
|
Metabolism and Nutrition Disorders | ||
|
Hypomagnesemia |
28% |
22% |
|
Hypophosphatemia |
28% |
21% |
|
Hyperkalemia |
26% |
19% |
|
Hyperglycemia |
21% |
15% |
|
Hyperlipidemia |
18% |
25% |
|
Hypokalemia |
16% |
18% |
|
Nervous System Disorders | ||
|
Tremor |
34% |
20% |
|
Headache |
24% |
25% |
|
Blood and Lymphatic System Disorders | ||
|
Anemia |
30% |
28% |
|
Leukopenia |
16% |
12% |
|
Miscellaneous | ||
|
Edema Peripheral |
35% |
46% |
|
Hypertension |
32% |
35% |
|
Insomnia |
30% |
21% |
|
Urinary Tract Infection |
26% |
22% |
|
Blood Creatinine Increased |
23% |
23% |
Less frequently observed adverse reactions in kidney transplantation patients are described under the subsection “Less Frequently Reported Adverse Reactions (> 3% and < 15%) in Liver, Kidney, and Heart Transplant Studies.”
Liver Transplantation
There were two randomized comparative liver transplant trials. In the U.S. trial, 263 adult and pediatric patients received tacrolimus and steroids and 266 patients received cyclosporine-based immunosuppressive regimen (CsA/AZA). The trial population had a mean age of 44 years (range 0.4 to 70); the distribution was 52% male, and the composition was White (78%), African-American (5%), Asian (2%), Hispanic (13%), and Other (2%). In the European trial, 270 patients received tacrolimus and steroids and 275 patients received CsA/AZA. The trial population had a mean age of 46 years (range 15 to 68); the distribution was 59% male, and the composition was White (95.4%), Black (1%), Asian (2%), and Other (2%).
The proportion of patients reporting more than one adverse event was > 99% in both the tacrolimus group and the CsA/AZA group. Precautions must be taken when comparing the incidence of adverse reactions in the U.S. trial to that in the European trial. The 12-month post-transplant information from the U.S. trial and from the European trial is presented below. The two trials also included different patient populations and patients were treated with immunosuppressive regimens of differing intensities. Adverse reactions reported in ≥ 15% in tacrolimus patients (combined trial results) are presented below for the two controlled trials in liver transplantation.
The most common adverse reactions (≥ 40%) observed in PROGRAF-treated liver transplant patients are: tremor, headache, diarrhea, hypertension, nausea, abnormal renal function, abdominal pain, insomnia, paresthesia, anemia, pain, fever, asthenia, hyperkalemia, hypomagnesemia, and hyperglycemia. These all occur with oral and IV administration of PROGRAF and some may respond to a reduction in dosing (e.g., tremor, headache, paresthesia, hypertension). Diarrhea was sometimes associated with other gastrointestinal complaints such as nausea and vomiting. Based on reported adverse reaction terms related to decreased renal function, nephrotoxicity was reported in approximately 40% and 36% of liver transplantation patients receiving PROGRAF in the U.S. and European randomized trials.
| U.S. TRIAL | EUROPEAN TRIAL | |||
|---|---|---|---|---|
| PROGRAF
(N = 250) | Cyclosporine/
AZA (N = 250) | PROGRAF
(N = 264) | Cyclosporine/
AZA (N = 265) |
|
|
Nervous System |
||||
|
Headache |
64% |
60% |
37% |
26% |
|
Insomnia |
64% |
68% |
32% |
23% |
|
Tremor |
56% |
46% |
48% |
32% |
|
Paresthesia |
40% |
30% |
17% |
17% |
|
Gastrointestinal |
||||
|
Diarrhea |
72% |
47% |
37% |
27% |
|
Nausea |
46% |
37% |
32% |
27% |
|
LFT Abnormal |
36% |
30% |
6% |
5% |
|
Anorexia |
34% |
24% |
7% |
5% |
|
Vomiting |
27% |
15% |
14% |
11% |
|
Constipation |
24% |
27% |
23% |
21% |
|
Cardiovascular |
||||
|
Hypertension |
47% |
56% |
38% |
43% |
|
Urogenital |
||||
|
Kidney Function Abnormal |
40% |
27% |
36% |
23% |
|
Creatinine Increased |
39% |
25% |
24% |
19% |
|
BUN Increased |
30% |
22% |
12% |
9% |
|
Oliguria |
18% |
15% |
19% |
12% |
|
Urinary Tract Infection |
16% |
18% |
21% |
19% |
|
Metabolic and Nutritional |
||||
|
Hypomagnesemia |
48% |
45% |
16% |
9% |
|
Hyperglycemia |
47% |
38% |
33% |
22% |
|
Hyperkalemia |
45% |
26% |
13% |
9% |
|
Hypokalemia |
29% |
34% |
13% |
16% |
|
Hemic and Lymphatic |
||||
|
Anemia |
47% |
38% |
5% |
1% |
|
Leukocytosis |
32% |
26% |
8% |
8% |
|
Thrombocytopenia |
24% |
20% |
14% |
19% |
|
Miscellaneous |
||||
|
Pain |
63% |
57% |
24% |
22% |
|
Abdominal Pain |
59% |
54% |
29% |
22% |
|
Asthenia |
52% |
48% |
11% |
7% |
|
Fever |
48% |
56% |
19% |
22% |
|
Back Pain |
30% |
29% |
17% |
17% |
|
Ascites |
27% |
22% |
7% |
8% |
|
Peripheral Edema |
26% |
26% |
12% |
14% |
|
Respiratory System |
||||
|
Pleural Effusion |
30% |
32% |
36% |
35% |
|
Dyspnea |
29% |
23% |
5% |
4% |
|
Atelectasis |
28% |
30% |
5% |
4% |
|
Skin and Appendages |
||||
|
Pruritus |
36% |
20% |
15% |
7% |
|
Rash |
24% |
19% |
10% |
4% |
| PROGRAF Granules
(N = 91) | Cyclosporine
(N = 90) |
|
|---|---|---|
|
Body as a Whole |
||
|
Fever |
46% |
51% |
|
Infection |
25% |
29% |
|
Sepsis |
22% |
20% |
|
CMV Infection |
15% |
24% |
|
EBV Infection |
26% |
11% |
|
Ascites |
17% |
20% |
|
Peritonitis |
12% |
7% |
|
Cardiovascular System |
||
|
Hypertension |
39% |
47% |
|
Digestive System |
||
|
Liver Function Tests Abnormal |
37% |
28% |
|
Diarrhea |
26% |
26% |
|
Vomiting |
15% |
13% |
|
Gastrointestinal Hemorrhage |
11% |
12% |
|
Bile Duct Disorder |
12% |
8% |
|
Gastroenteritis |
12% |
4% |
|
Hemic and Lymphatic System |
||
|
Anemia |
29% |
19% |
|
Metabolic and Nutritional Disorders |
||
|
Hypomagnesemia |
40% |
29% |
|
Acidosis |
26% |
17% |
|
Hyperkalemia |
12% |
10% |
|
Respiratory System |
||
|
Pleural Effusion |
22% |
19% |
|
Bronchitis |
11% |
8% |
|
Urogenital System |
||
|
Kidney Function Abnormal |
13% |
14% |
Less frequently observed adverse reactions in liver transplantation patients are described under the subsection “Less Frequently Reported Adverse Reactions (> 3% and < 15%) in Liver, Kidney, and Heart Transplant Studies.”
Heart Transplantation
The incidence of adverse reactions was determined based on two trials in primary orthotopic heart transplantation. In a trial conducted in Europe, 314 patients received a regimen of antibody induction, corticosteroids, and azathioprine (AZA) in combination with PROGRAF (n = 157) or cyclosporine (n = 157) for 18 months. The trial population had a mean age of 51 years (range 18 to 65); the distribution was 82% male, and the composition was White (96%), Black (3%), and Other (1%).
The most common adverse reactions (≥ 15%) observed in PROGRAF-treated heart transplant patients are: abnormal renal function, hypertension, diabetes mellitus, CMV infection, tremor, hyperglycemia, leukopenia, infection, anemia, bronchitis, pericardial effusion, urinary tract infection, and hyperlipemia. Based on reported adverse reaction terms related to decreased renal function, nephrotoxicity was reported in approximately 59% of heart transplantation patients in the European trial.
Adverse reactions in heart transplant patients in the European trial are presented below:
| PROGRAF/AZA
(N = 157) | Cyclosporine/AZA
(N = 157) |
|
|---|---|---|
|
Cardiovascular System |
||
|
Hypertension |
62% |
69% |
|
Pericardial Effusion |
15% |
14% |
|
Body as a Whole |
||
|
CMV Infection |
32% |
30% |
|
Infection |
24% |
21% |
|
Metabolic and Nutritional Disorders |
||
|
Diabetes Mellitus |
26% |
16% |
|
Hyperglycemia |
23% |
17% |
|
Hyperlipemia |
18% |
27% |
|
Hemic and Lymphatic System |
||
|
Anemia |
50% |
36% |
|
Leukopenia |
48% |
39% |
|
Urogenital System |
||
|
Kidney Function Abnormal |
56% |
57% |
|
Urinary Tract Infection |
16% |
12% |
|
Respiratory System |
||
|
Bronchitis |
17% |
18% |
|
Nervous System |
||
|
Tremor |
15% |
6% |
In the European trial, the cyclosporine trough concentrations were above the pre-defined target range (i.e., 100 to 200 ng/mL) at Day 122 and beyond in 32% to 68% of the patients in the cyclosporine treatment arm, whereas the tacrolimus trough concentrations were within the pre-defined target range (i.e., 5 to 15 ng/mL) in 74% to 86% of the patients in the tacrolimus treatment arm.
In a U.S. trial, the incidence of adverse reactions was based on 331 heart transplant patients that received corticosteroids and PROGRAF in combination with sirolimus (n=109), PROGRAF in combination with MMF (n=107) or cyclosporine modified in combination with MMF (n=115) for 1 year. The trial population had a mean age of 53 years (range 18 to 75); the distribution was 78% male, and the composition was White (83%), African-American (13%) and Other (4%).
Only selected targeted treatment-emergent adverse reactions were collected in the U.S. heart transplantation trial. Those reactions that were reported at a rate of 15% or greater in patients treated with PROGRAF and MMF include the following: any target adverse reactions (99%), hypertension (89%), hyperglycemia requiring antihyperglycemic therapy (70%), hypertriglyceridemia (65%), anemia (hemoglobin < 10.0 g/dL) (65%), fasting blood glucose > 140 mg/dL (on two separate occasions) (61%), hypercholesterolemia (57%), hyperlipidemia (34%), WBCs < 3000 cells/mcL (34%), serious bacterial infections (30%), magnesium < 1.2 mEq/L (24%), platelet count < 75,000 cells/mcL (19%), and other opportunistic infections (15%).
Other targeted treatment-emergent adverse reactions in PROGRAF-treated patients occurred at a rate of less than 15%, and include the following: Cushingoid features, impaired wound healing, hyperkalemia, Candida infection, and CMV infection/syndrome. Other less frequently observed adverse reactions in heart transplantation patients are described under the subsection “Less Frequently Reported Adverse Reactions (> 3% and < 15%) in Liver, Kidney and Heart Transplant Studies.”
New Onset Diabetes After Transplant
Kidney Transplantation
New Onset Diabetes After Transplant (NODAT) is defined as a composite of fasting plasma glucose ≥ 126 mg/dL, HbA1C ≥ 6%, insulin use ≥ 30 days, or oral hypoglycemic use. In a trial in kidney transplant patients (Study 2), NODAT was observed in 75% in the PROGRAF-treated and 61% in the NEORAL-treated patients without pre-transplant history of diabetes mellitus (Table 10) [see Clinical Studies (14.1)].
| Parameter | Treatment Group | |
|---|---|---|
| PROGRAF/MMF
(N = 212) | NEORAL/MMF
(N = 212) |
|
|
NODAT |
112/150 (75%) |
93/152 (61%) |
|
Fasting Plasma Glucose ≥ 126 mg/dL |
96/150 (64%) |
80/152 (53%) |
|
HbA1C ≥ 6% |
59/150 (39%) |
28/152 (18%) |
|
Insulin Use ≥ 30 days |
9/150 (6%) |
4/152 (3%) |
|
Oral Hypoglycemic Use |
15/150 (10%) |
5/152 (3%) |
In early trials of PROGRAF, Post-Transplant Diabetes Mellitus (PTDM) was evaluated with a more limited criterion of “use of insulin for 30 or more consecutive days with < 5-day gap” in patients without a prior history of insulin-dependent diabetes mellitus or non-insulin dependent diabetes mellitus. Data are presented in Tables 11 to 14. PTDM was reported in 20% of PROGRAF/Azathioprine (AZA)-treated kidney transplant patients without pre-transplant history of diabetes mellitus in a Phase 3 trial (Table 11). The median time to onset of PTDM was 68 days. Insulin dependence was reversible in 15% of these PTDM patients at one year and in 50% at 2 years post-transplant. African-American and Hispanic kidney transplant patients were at an increased risk of development of PTDM (Table 12).
| Status of PTDM* | PROGRAF/AZA | CsA/AZA |
|---|---|---|
|
||
|
Patients without pre-transplant history of diabetes mellitus |
151 |
151 |
|
New onset PTDM*, 1st Year |
30/151 (20%) |
6/151 (4%) |
|
Still insulin-dependent at one year in those without prior history of diabetes |
25/151 (17%) |
5/151 (3%) |
|
New onset PTDM* post 1 year |
1 |
0 |
|
Patients with PTDM* at 2 years |
16/151 (11%) |
5/151 (3%) |
| Patient Race | Patients Who Developed PTDM* | |
|---|---|---|
| PROGRAF | Cyclosporine | |
|
||
|
African-American |
15/41 (37%) |
3 (8%) |
|
Hispanic |
5/17 (29%) |
1 (6%) |
|
Caucasian |
10/82 (12%) |
1 (1%) |
|
Other |
0/11 (0%) |
1 (10%) |
|
Total |
30/151 (20%) |
6 (4%) |
Liver Transplantation
Insulin-dependent PTDM was reported in 18% and 11% of PROGRAF-treated liver transplant patients and was reversible in 45% and 31% of these patients at 1 year post-transplant, in the U.S. and European randomized trials, respectively (Table 13). Hyperglycemia was associated with the use of PROGRAF in 47% and 33% of liver transplant recipients in the U.S. and European randomized trials, respectively, and may require treatment [see Adverse Reactions (6.1)].
| Status of PTDM* | US Trial | European Trial | ||
|---|---|---|---|---|
| PROGRAF | Cyclosporine | PROGRAF | Cyclosporine | |
|
Patients at risk† |
239 |
236 |
239 |
249 |
|
New Onset PTDM* |
42 (18%) |
30 (13%) |
26 (11%) |
12 (5%) |
|
Patients still on insulin at 1 year |
23 (10%) |
19 (8%) |
18 (8%) |
6 (2%) |
Heart Transplantation
Insulin-dependent PTDM was reported in 13% and 22% of PROGRAF-treated heart transplant patients receiving mycophenolate mofetil (MMF) or azathioprine (AZA) and was reversible in 30% and 17% of these patients at one year post-transplant, in the U.S. and European randomized trials, respectively (Table 14). Hyperglycemia, defined as two fasting plasma glucose levels ≥ 126 mg/dL, was reported with the use of PROGRAF plus MMF or AZA in 32% and 35% of heart transplant recipients in the U.S. and European randomized trials, respectively, and may require treatment [see Adverse Reactions (6.1)].
| Status of PTDM* | US Trial | European Trial | ||
|---|---|---|---|---|
| PROGRAF/MMF | Cyclosporine/MMF | PROGRAF/AZA | Cyclosporine/AZA | |
|
Patients at risk† |
75 |
83 |
132 |
138 |
|
New Onset PTDM* |
10 (13%) |
6 (7%) |
29 (22%) |
5 (4%) |
|
Patients still on insulin at 1 year‡ |
7 (9%) |
1 (1%) |
24 (18%) |
4 (3%) |
Less Frequently Reported Adverse Reactions (> 3% and < 15%) in Liver, Kidney, and Heart Transplant Studies
The following adverse reactions were reported in either liver, kidney, and/or heart transplant recipients who were treated with tacrolimus in clinical trials.
- •
- Nervous System: Abnormal dreams, agitation, amnesia, anxiety, confusion, convulsion, crying, depression, elevated mood, emotional lability, encephalopathy, hemorrhagic stroke, hallucinations, hypertonia, incoordination, monoparesis, myoclonus, nerve compression, nervousness, neuralgia, neuropathy, paralysis flaccid, psychomotor skills impaired, psychosis, quadriparesis, somnolence, thinking abnormal, vertigo, writing impaired
- •
- Special Senses: Abnormal vision, amblyopia, ear pain, otitis media, tinnitus
- •
- Gastrointestinal: Cholangitis, cholestatic jaundice, duodenitis, dysphagia, esophagitis, flatulence, gastritis, gastroesophagitis, gastrointestinal hemorrhage, GGT increase, GI disorder, GI perforation, hepatitis, hepatitis granulomatous, ileus, increased appetite, jaundice, liver damage, esophagitis ulcerative, oral moniliasis, pancreatic pseudocyst, stomatitis
- •
- Cardiovascular: Abnormal ECG, angina pectoris, arrhythmia, atrial fibrillation, atrial flutter, bradycardia, cardiac fibrillation, cardiopulmonary failure, congestive heart failure, deep thrombophlebitis, echocardiogram abnormal, electrocardiogram QRS complex abnormal, electrocardiogram ST segment abnormal, heart failure, heart rate decreased, hemorrhage, hypotension, phlebitis, postural hypotension, syncope, tachycardia, thrombosis, vasodilatation
- •
- Urogenital: Acute kidney failure, albuminuria, BK nephropathy, bladder spasm, cystitis, dysuria, hematuria, hydronephrosis, kidney failure, kidney tubular necrosis, nocturia, pyuria, toxic nephropathy, urge incontinence, urinary frequency, urinary incontinence, urinary retention, vaginitis
- •
- Metabolic/Nutritional: Acidosis, alkaline phosphatase increased, alkalosis, ALT (SGPT) increased, AST (SGOT) increased, bicarbonate decreased, bilirubinemia, dehydration, GGT increased, gout, healing abnormal, hypercalcemia, hypercholesterolemia, hyperphosphatemia, hyperuricemia, hypervolemia, hypocalcemia, hypoglycemia, hyponatremia, hypoproteinemia, lactic dehydrogenase increased, weight gain
- •
- Endocrine: Cushing’s syndrome
- •
- Hemic/Lymphatic: Coagulation disorder, ecchymosis, hematocrit increased, hypochromic anemia, leukocytosis, polycythemia, prothrombin decreased, serum iron decreased
- •
- Miscellaneous: Abdomen enlarged, abscess, accidental injury, allergic reaction, cellulitis, chills, fall, flu syndrome, generalized edema, hernia, mobility decreased, peritonitis, photosensitivity reaction, sepsis, temperature intolerance, ulcer
- •
- Musculoskeletal: Arthralgia, cramps, generalized spasm, leg cramps, myalgia, myasthenia, osteoporosis
- •
- Respiratory: Asthma, emphysema, hiccups, lung function decreased, pharyngitis, pneumonia, pneumothorax, pulmonary edema, rhinitis, sinusitis, voice alteration
- •
- Skin: Acne, alopecia, exfoliative dermatitis, fungal dermatitis, herpes simplex, herpes zoster, hirsutism, neoplasm skin benign, skin discoloration, skin ulcer, sweating
Lung Transplantation
Adverse reactions in lung transplant patients were similar to those in kidney, liver, or heart transplant patients treated with PROGRAF [see Adverse Reactions (6.2)].
6.2 Postmarketing Experience
The following adverse reactions have been reported from worldwide marketing experience with tacrolimus. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure. Decisions to include these reactions in labeling are typically based on one or more of the following factors: (1) seriousness of the reaction, (2) frequency of the reporting, or (3) strength of causal connection to the drug.
Other reactions include:
- •
- Cardiovascular: Atrial fibrillation, atrial flutter, cardiac arrhythmia, cardiac arrest, electrocardiogram T wave abnormal, flushing, myocardial infarction, myocardial ischemia, pericardial effusion, QT prolongation, Torsades de pointes, venous thrombosis deep limb, ventricular extrasystoles, ventricular fibrillation, myocardial hypertrophy
- •
- Gastrointestinal: Bile duct stenosis, colitis, enterocolitis, gastroenteritis, gastroesophageal reflux disease, hepatic cytolysis, hepatic necrosis, hepatotoxicity, impaired gastric emptying, liver fatty, mouth ulceration, pancreatitis hemorrhagic, pancreatitis necrotizing, stomach ulcer, veno-occlusive liver disease
- •
- Hemic/Lymphatic: Agranulocytosis, disseminated intravascular coagulation, hemolytic anemia, neutropenia, febrile neutropenia, pancytopenia, thrombocytopenic purpura, thrombotic thrombocytopenic purpura, pure red cell aplasia, thrombotic microangiopathy
- •
- Infections: Cases of progressive multifocal leukoencephalopathy (PML), sometimes fatal; polyoma virus-associated nephropathy (PVAN) including graft loss
- •
- Metabolic/Nutritional: Glycosuria, increased amylase including pancreatitis, weight decreased
- •
- Miscellaneous: Feeling hot and cold, feeling jittery, hot flushes, multi-organ failure, primary graft dysfunction
- •
- Musculoskeletal and Connective Tissue Disorders: Pain in extremity including Calcineurin-Inhibitor Induced Pain Syndrome (CIPS)
- •
- Nervous System: Carpal tunnel syndrome, cerebral infarction, hemiparesis, leukoencephalopathy, mental disorder, mutism, posterior reversible encephalopathy syndrome (PRES), progressive multifocal leukoencephalopathy (PML), quadriplegia, speech disorder, syncope
- •
- Respiratory: Acute respiratory distress syndrome, interstitial lung disease, lung infiltration, respiratory distress, respiratory failure
- •
- Skin: Stevens-Johnson syndrome, toxic epidermal necrolysis
- •
- Special Senses: Blindness, optic neuropathy, blindness cortical, hearing loss including deafness, photophobia
- •
- Urogenital: Acute renal failure, cystitis hemorrhagic, hemolytic-uremic syndrome
Postmarketing Adverse Reactions in Lung Transplantation
Based on U.S. Scientific Registry of Transplant Recipients (SRTR) data, published clinical trials, and postmarketing reports, the safety profile for lung transplant patients treated with PROGRAF is consistent with the safety profile in kidney, liver, and heart transplant patients treated with PROGRAF. The primary adverse reactions described include renal dysfunction, infection, diabetes, gastrointestinal disturbances (e.g., diarrhea), hypertension, and neurological events (e.g., tremor). As expected, lung transplant patients have a higher incidence of pulmonary complications (e.g., pneumonia, bronchiolitis obliterans syndrome) than other solid organ transplant patients, which is in part due to the underlying disease and to the nature of the transplanted organ.
Related/similar drugs
7. Drug Interactions
7.1 Mycophenolic Acid
When PROGRAF is prescribed with a given dose of a mycophenolic acid (MPA) product, exposure to MPA is higher with PROGRAF co-administration than with cyclosporine co-administration with MPA, because cyclosporine interrupts the enterohepatic recirculation of MPA while tacrolimus does not. Monitor for MPA-associated adverse reactions and reduce the dose of concomitantly administered mycophenolic acid products as needed.
7.2 Effects of Other Drugs on PROGRAF
Table 15 displays the effects of other drugs on PROGRAF.
| Drug/Substance Class or Name | Drug Interaction Effect | Recommendations |
|---|---|---|
|
||
|
Grapefruit or grapefruit juice† |
May increase tacrolimus whole blood trough concentrations and increase the risk of serious adverse reactions (e.g., neurotoxicity, QT prolongation) [see Warnings and Precautions (5.6, 5.11, 5.12)]. |
Avoid grapefruit or grapefruit juice. |
|
Strong CYP3A Inducers‡:
|
May decrease tacrolimus whole blood trough concentrations and increase the risk of rejection [see Warnings and Precautions (5.11)]. |
Increase PROGRAF dose and monitor tacrolimus whole blood trough concentrations [see Dosage and Administration (2.2, 2.6) and Clinical Pharmacology (12.3)]. |
|
Strong CYP3A Inhibitors‡:
|
May increase tacrolimus whole blood trough concentrations and increase the risk of serious adverse reactions (e.g., neurotoxicity, QT prolongation). A rapid, sharp rise in tacrolimus levels may occur early, despite an immediate reduction of tacrolimus dose [see Warnings and Precautions (5.6, 5.11, 5.12)]. |
Reduce PROGRAF dose (for voriconazole and posaconazole, give one-third of the original dose) and adjust dose based on tacrolimus whole blood trough concentrations [see Dosage and Administration (2.2, 2.6) and Clinical Pharmacology (12.3)]. Early and frequent monitoring of tacrolimus whole blood trough levels should start within 1-3 days and continue monitoring as necessary [see Warnings and Precautions (5.11)]. |
|
Mild or Moderate CYP3A Inhibitors:
|
May increase tacrolimus whole blood trough concentrations and increase the risk of serious adverse reactions (e.g., neurotoxicity, QT prolongation) [see Warnings and Precautions (5.6, 5.11, 5.12)]. |
Monitor tacrolimus whole blood trough concentrations and reduce PROGRAF dose if needed [see Dosage and Administration (2.2, 2.6) and Clinical Pharmacology (12.3)]. |
|
Other drugs, such as:
|
May increase tacrolimus whole blood trough concentrations and increase the risk of serious adverse reactions (e.g., neurotoxicity, QT prolongation) [see Warnings and Precautions (5.6, 5.11, 5.12)]. |
Monitor tacrolimus whole blood trough concentrations and reduce PROGRAF dose if needed [see Dosage and Administration (2.2, 2.6) and Clinical Pharmacology (12.3)]. |
|
Mild or Moderate CYP3A Inducers
|
May decrease tacrolimus whole blood trough concentrations. |
Monitor tacrolimus whole blood trough concentrations and adjust PROGRAF dose if needed [see Dosage and Administration (2.2, 2.6)]. |
|
Caspofungin |
May decrease tacrolimus whole blood trough concentrations. |
Monitor tacrolimus whole blood trough concentrations and adjust PROGRAF dose if needed [see Dosage and Administration (2.2, 2.6)]. |
Direct Acting Antiviral (DAA) Therapy
The pharmacokinetics of tacrolimus may be impacted by changes in liver function during DAA therapy, related to clearance of HCV virus. Close monitoring and potential dose adjustment of PROGRAF is warranted to ensure continued efficacy and safety [see Dosage and Administration (2.2, 2.6)].
7.3 Cannabidiol
The blood levels of tacrolimus may increase upon concomitant use with cannabidiol. When cannabidiol and PROGRAF are co-administered, closely monitor for an increase in tacrolimus blood levels and for adverse reactions suggestive of tacrolimus toxicity. A dose reduction of PROGRAF should be considered as needed when PROGRAF is co-administered with cannabidiol [see Dosage and Administration (2.2, 2.6) and Warnings and Precautions (5.17)].
8. Use In Specific Populations
8.1 Pregnancy
Pregnancy Exposure Registry
There is a pregnancy registry that monitors pregnancy outcomes in women exposed to PROGRAF during pregnancy.
The Transplantation Pregnancy Registry International (TPRI) is a voluntary pregnancy exposure registry that monitors outcomes of pregnancy in female transplant recipients and those fathered by male transplant recipients exposed to immunosuppressants including tacrolimus. Healthcare providers are encouraged to advise their patients to register by contacting the Transplantation Pregnancy Registry International at 1-877-955-6877 or https://www.transplantpregnancyregistry.org/.
Risk Summary
Tacrolimus can cause fetal harm when administered to a pregnant woman. Data from postmarketing surveillance and TPRI suggest that infants exposed to tacrolimus in utero are at a risk of prematurity, birth defects/congenital anomalies, low birth weight, and fetal distress [see Human Data]. Advise pregnant women of the potential risk to the fetus.
Administration of oral tacrolimus to pregnant rabbits and rats throughout the period of organogenesis was associated with maternal toxicity/lethality, and an increased incidence of abortion, malformation and embryofetal death at clinically relevant doses (0.5 to 6.9 times the recommended clinical dose range [0.2 to 0.075 mg/kg/day], on a mg/m2 basis).
Administration of oral tacrolimus to pregnant rats after organogenesis and throughout lactation produced maternal toxicity, effects on parturition, reduced pup viability and reduced pup weight at clinically relevant doses (0.8 to 6.9 times the recommended clinical dose range, on a mg/m2 basis). Administration of oral tacrolimus to rats prior to mating, and throughout gestation and lactation produced maternal toxicity/lethality, marked effects on parturition, embryofetal loss, malformations, and reduced pup viability at clinically relevant doses (0.8 to 6.9 times the recommended clinical dose range, on a mg/m2 basis). Interventricular septal defects, hydronephrosis, craniofacial malformations and skeletal effects were observed in offspring that died [see Animal Data].
The background risk of major birth defects and miscarriage in the indicated population is unknown. In the U.S. general population, the estimated background risk of major birth defects and miscarriage in clinically recognized pregnancies is 2 to 4% and 15 to 20%, respectively.
Clinical Considerations
Disease-Associated Maternal and/or Embryo-Fetal Risk
Risks during pregnancy are increased in organ transplant recipients.
The risk of premature delivery following transplantation is increased. Pre-existing hypertension and diabetes confer additional risk to the pregnancy of an organ transplant recipient. Pre-gestational and gestational diabetes are associated with birth defects/congenital anomalies, hypertension, low birth weight and fetal death.
Cholestasis of pregnancy (COP) was reported in 7% of liver or liver-kidney (LK) transplant recipients, compared with approximately 1% of pregnancies in the general population. However, COP symptoms resolved postpartum and no long-term effects on the offspring were reported.
Maternal Adverse Reactions
PROGRAF may increase hyperglycemia in pregnant women with diabetes (including gestational diabetes). Monitor maternal blood glucose levels regularly [see Warnings and Precautions (5.4)].
PROGRAF may exacerbate hypertension in pregnant women and increase pre-eclampsia. Monitor and control blood pressure [see Warnings and Precautions (5.7, 5.8)].
Fetal/Neonatal Adverse Reactions
Renal dysfunction, transient neonatal hyperkalemia and low birth weight have been reported at the time of delivery in infants of mothers taking PROGRAF.
Labor or Delivery
There is an increased risk for premature delivery (< 37 weeks) following transplantation and maternal exposure to PROGRAF.
Data
Human Data
There are no adequate and well controlled studies on the effects of tacrolimus in human pregnancy. Safety data from the TPRI and postmarketing surveillance suggest infants exposed to tacrolimus in utero have an increased risk for miscarriage, pre-term delivery (< 37 weeks), low birth weight (< 2500 g), birth defects/congenital anomalies and fetal distress.
TPRI reported 450 and 241 total pregnancies in kidney and liver transplant recipients exposed to tacrolimus, respectively. The TPRI pregnancy outcomes are summarized in Table 16. In the table below, the number of recipients exposed to tacrolimus concomitantly with mycophenolic acid (MPA) products during the preconception and first trimester periods is high (27% and 29% for renal and liver transplant recipients, respectively). Because MPA products may also cause birth defects, the birth defect rate may be confounded and this should be taken into consideration when reviewing the data, particularly for birth defects. Birth defects observed include cardiac malformations, craniofacial malformations, renal/urogenital disorders, skeletal abnormalities, neurological abnormalities and multiple malformations.
| Kidney | Liver | |
|---|---|---|
|
Pregnancy Outcomes* |
462 |
253 |
|
Miscarriage |
24.5% |
25% |
|
Live births |
331 |
180 |
|
Pre-term delivery (< 37 weeks) |
49% |
42% |
|
Low birth weight (< 2500 g) |
42% |
30% |
|
Birth defects |
8%† |
5% |
Additional information reported by TPRI in pregnant transplant patients receiving tacrolimus included diabetes during pregnancy in 9% of kidney recipients and 13% of liver recipients, and hypertension during pregnancy in 53% of kidney recipients and 16.2% of liver recipients.
Animal Data
Administration of oral tacrolimus to pregnant rabbits throughout organogenesis produced maternal toxicity and abortion at 0.32 mg/kg (0.5 to 1.4 times the recommended clinical dose range [0.2 to 0.075 mg/kg/day], on a mg/m2 basis). At 1 mg/kg (1.6 to 4.3 times the recommended clinical dose range), embryofetal lethality and fetal malformations (ventricular hypoplasia, interventricular septal defect, bulbous aortic arch, stenosis of ductus arteriosus, omphalocele, gallbladder agenesis, skeletal anomalies) were observed. Administration of 3.2 mg/kg oral tacrolimus (2.6 to 6.9 times the recommended clinical dose range) to pregnant rats throughout organogenesis produced maternal toxicity/lethality, embryofetal lethality and decreased fetal body weight in the offspring of C-sectioned dams; and decreased pup viability and interventricular septal defect in offspring of dams that delivered.
In a peri-/postnatal development study, oral administration of tacrolimus to pregnant rats during late gestation (after organogenesis) and throughout lactation produced maternal toxicity, effects on parturition, and reduced pup viability at 3.2 mg/kg (2.6 to 6.9 times the recommended clinical dose range); among these pups that died early, an increased incidence of kidney hydronephrosis was observed. Reduced pup weight was observed at 1.0 mg/kg (0.8 to 2.2 times the recommended clinical dose range).
Administration of oral tacrolimus to rats prior to mating, and throughout gestation and lactation, produced maternal toxicity/lethality, embryofetal loss and reduced pup viability at 3.2 mg/kg (2.6 to 6.9 times the recommended clinical dose range). Interventricular septal defects, hydronephrosis, craniofacial malformations and skeletal effects were observed in offspring that died. Effects on parturition (incomplete delivery of nonviable pups) were observed at 1 mg/kg (0.8 to 2.2 times the recommended clinical dose range) [see Nonclinical Toxicology (13.1)].
8.2 Lactation
Risk Summary
Controlled lactation studies have not been conducted in humans; however, tacrolimus has been reported to be present in human milk. The effects of tacrolimus on the breastfed infant, or on milk production have not been assessed. Tacrolimus is excreted in rat milk and in peri-/postnatal rat studies; exposure to tacrolimus during the postnatal period was associated with developmental toxicity in the offspring at clinically relevant doses [see Use in Specific Populations (8.1) and Nonclinical Toxicology (13.1)].
The developmental and health benefits of breastfeeding should be considered along with the mother’s clinical need for PROGRAF and any potential adverse effects on the breastfed child from PROGRAF or from the underlying maternal condition.
8.3 Females and Males of Reproductive Potential
Contraception
PROGRAF can cause fetal harm when administered to pregnant women. Advise female and male patients of reproductive potential to speak to their healthcare provider on family planning options including appropriate contraception prior to starting treatment with PROGRAF [see Use in Specific Populations (8.1) and Nonclinical Toxicology (13.1)].
Infertility
Based on findings in animals, male and female fertility may be compromised by treatment with PROGRAF [see Nonclinical Toxicology (13.1)].
8.4 Pediatric Use
Safety and effectiveness have been established in pediatric liver, kidney, heart, and lung transplant patients.
Liver Transplantation
Safety and efficacy using PROGRAF Granules in pediatric de novo liver transplant patients less than 16 years of age are based on evidence from active controlled studies that included 56 pediatric patients, 31 of which received PROGRAF, and supported by two pharmacokinetic and safety studies in 151 children who received PROGRAF. Additionally, 122 pediatric patients were studied in an uncontrolled trial of tacrolimus in living related donor liver transplantation. Dose adjustments were made in the PK studies based on clinical status and whole blood concentrations. Pediatric patients generally required higher doses of PROGRAF to maintain blood trough concentrations of tacrolimus similar to adult patients [see Dosage and Administration (2.3), Adverse Reactions (6.1), Clinical Pharmacology (12.3) and Clinical Studies (14.2)].
Kidney and Heart Transplantation
Use of PROGRAF capsules and PROGRAF Granules in pediatric kidney and heart transplant patients is supported by adequate and well-controlled studies and pharmacokinetic data in adult kidney and heart transplant patients with additional pharmacokinetic data in pediatric kidney and heart transplant patients and safety data in pediatric liver transplant patients [see Dosage and Administration (2.3) and Clinical Pharmacology (12.3)].
Lung Transplantation
The use of PROGRAF capsules and PROGRAF Granules in pediatric lung transplantation is supported by the experience in the U.S. Scientific Registry of Transplant Recipients (SRTR) including 450 pediatric patients receiving tacrolimus immediate-release products in combination with mycophenolate mofetil and 72 pediatric patients receiving tacrolimus immediate-release products in combination with azathioprine between 1999-2017.
8.5 Geriatric Use
Clinical trials of PROGRAF did not include sufficient numbers of subjects aged 65 and over to determine whether they respond differently from younger subjects. Other reported clinical experience has not identified differences in responses between the elderly and younger patients. In general, dose selection for an elderly patient should be cautious, usually starting at the low end of the dosing range, reflecting the greater frequency of decreased hepatic, renal, or cardiac function, and of concomitant disease or other drug therapy.
8.6 Renal Impairment
The pharmacokinetics of PROGRAF in patients with renal impairment was similar to that in healthy volunteers with normal renal function. However, consideration should be given to dosing PROGRAF at the lower end of the therapeutic dosing range in patients who have received a liver or heart transplant and have pre-existing renal impairment. Further reductions in dose below the targeted range may be required [see Dosage and Administration (2.4) and Clinical Pharmacology (12.3)].
8.7 Hepatic Impairment
The mean clearance of tacrolimus was substantially lower in patients with severe hepatic impairment (mean Child-Pugh score: > 10) compared to healthy volunteers with normal hepatic function. Close monitoring of tacrolimus trough concentrations is warranted in patients with hepatic impairment [see Clinical Pharmacology (12.3)].
The use of PROGRAF in liver transplant recipients experiencing post-transplant hepatic impairment may be associated with increased risk of developing renal insufficiency related to high whole blood trough concentrations of tacrolimus. These patients should be monitored closely and dosage adjustments should be considered. Some evidence suggests that lower doses should be used in these patients [see Dosage and Administration (2.5) and Clinical Pharmacology (12.3)].
8.8 Race or Ethnicity
African-American patients may need to be titrated to higher dosages to attain comparable trough concentrations compared to Caucasian patients [see Dosage and Administration (2.2) and Clinical Pharmacology (12.3)].
African-American and Hispanic patients are at increased risk for new onset diabetes after transplant. Monitor blood glucose concentrations and treat appropriately [see Warnings and Precautions (5.4)].
10. Overdosage
Limited overdosage experience is available. Acute overdosages of up to 30 times the intended dose have been reported. Almost all cases have been asymptomatic and all patients recovered with no sequelae. Acute overdosage was sometimes followed by adverse reactions consistent with those reported with the use of PROGRAF [see Adverse Reactions (6.1, 6.2)], including tremors, abnormal renal function, hypertension, and peripheral edema; in one case of acute overdosage, transient urticaria and lethargy were observed. Based on the poor aqueous solubility and extensive erythrocyte and plasma protein binding, it is anticipated that tacrolimus is not dialyzable to any significant extent; there is no experience with charcoal hemoperfusion. The oral use of activated charcoal has been reported in treating acute overdoses, but experience has not been sufficient to warrant recommending its use. General supportive measures and treatment of specific symptoms should be followed in all cases of overdosage.
11. Prograf Description
Tacrolimus, previously known as FK506, is the active ingredient in PROGRAF. Tacrolimus is a calcineurin-inhibitor immunosuppressant produced by Streptomyces tsukubaensis. Chemically, tacrolimus is designated as [3S-[3R*[E(1S*,3S*,4S*)], 4S*,5R*,8S*,9E,12R*,14R*,15S*,16R*,18S*,19S*,26aR*]] -5,6,8,11,12,13,14,15,16,17,18,19,24,25,26,26a-hexadecahydro-5,19-dihydroxy-3-[2-(4-hydroxy-3-methoxycyclohexyl)-1-methylethenyl]-14,16-dimethoxy-4,10,12,18-tetramethyl-8-(2-propenyl)-15,19-epoxy-3H-pyrido[2,1-c][1,4] oxaazacyclotricosine-1,7,20,21(4H,23H)-tetrone, monohydrate.
The chemical structure of tacrolimus is:
Tacrolimus has an empirical formula of C44H69NO12•H2O and a formula weight of 822.03. Tacrolimus appears as white crystals or crystalline powder. It is practically insoluble in water, freely soluble in ethanol, and very soluble in methanol and chloroform.
PROGRAF is available for oral administration as capsules (tacrolimus capsules USP) containing the equivalent of 0.5 mg, 1 mg or 5 mg of anhydrous tacrolimus USP. Inactive ingredients include croscarmellose sodium NF, hypromellose USP, lactose monohydrate NF, and magnesium stearate NF. The 0.5 mg capsule shell contains ferric oxide NF, gelatin NF and titanium dioxide USP, the 1 mg capsule shell contains gelatin NF and titanium dioxide USP, and the 5 mg capsule shell contains ferric oxide NF, gelatin NF, and titanium dioxide USP.
PROGRAF is also available as a sterile solution (tacrolimus injection) containing the equivalent of 5 mg anhydrous tacrolimus USP in 1 mL for administration by intravenous infusion only. Each mL contains the following inactive ingredients: dehydrated alcohol USP, 80.0% v/v and polyoxyl 60 hydrogenated castor oil (HCO-60), 200 mg. PROGRAF injection must be diluted with 0.9% Sodium Chloride Injection or 5% Dextrose Injection before use.
PROGRAF Granules is available for oral administration as a suspension containing the equivalent of 0.2 mg or 1 mg of anhydrous tacrolimus USP. Inactive ingredients include croscarmellose sodium NF, hypromellose USP, and lactose monohydrate NF.
12. Prograf - Clinical Pharmacology
12.1 Mechanism of Action
Tacrolimus binds to an intracellular protein, FKBP-12. A complex of tacrolimus-FKBP-12, calcium, calmodulin, and calcineurin (a ubiquitous mammalian intracellular enzyme) is then formed, after which the phosphatase activity of calcineurin is inhibited. Such inhibition prevents the dephosphorylation and translocation of various factors such as the nuclear factor of activated T-cells (NF-AT), and nuclear factor kappa-light-chain enhancer of activated B-cells (NF-κB).
Tacrolimus inhibits the expression and/or production of several cytokines that include interleukin (IL)-1 beta, IL-2, IL-3, IL-4, IL-5, IL-6, IL-8, IL-10, gamma interferon, tumor necrosis factor-alpha, and granulocyte macrophage colony-stimulating factor. Tacrolimus also inhibits IL-2 receptor expression and nitric oxide release, induces apoptosis and production of transforming growth factor beta that can lead to immunosuppressive activity. The net result is the inhibition of T-lymphocyte activation and proliferation, as well as T-helper-cell-dependent B-cell response (i.e., immunosuppression).
12.3 Pharmacokinetics
Tacrolimus activity is primarily due to the parent drug. The pharmacokinetic parameters (mean ± S.D.) of tacrolimus have been determined following intravenous (IV) and/or oral (PO) administration in healthy volunteers, and in kidney transplant, liver transplant, and heart transplant patients (Table 17).
| Population | N | Route
(Dose) | Parameters | |||||
|---|---|---|---|---|---|---|---|---|
| Cmax
(ng/mL) | Tmax
(hr) | AUC
(ng•hr/mL) | t1/2
(hr) | CL
(L/hr/kg) | V
(L/kg) |
|||
|
Healthy Volunteers |
8 |
IV (0.025 mg/kg/4 hr) |
652† ± 156 |
34.2 ± 7.7 |
0.040 ± 0.009 |
1.91 ± 0.31 |
||
|
30 |
PO (5 mg) (granules) |
35.6 ± 10.9 |
1.3 ± 0.5 |
320† ± 164 |
32.1 ± 5.9 | |||
|
PO (5 mg) (capsules) |
28.8 ± 8.9 |
1.5 ± 0.7 |
266† ± 95 |
32.3 ± 8.8 | ||||
|
Kidney Transplant Patients |
26 |
IV (0.02 mg/kg/12 hr) |
294† ± 262 |
18.8 ± 16.7 |
0.083 ± 0.050 |
1.41 ± 0.66 |
||
|
PO (0.2 mg/kg/day) |
19.2 ± 10.3 |
3.0 |
203† ± 42 | |||||
|
PO (0.3 mg/kg/day) |
24.2 ± 15.8 |
1.5 |
288† ± 93 | |||||
|
Liver Transplant Patients |
17 |
IV (0.05 mg/kg/12 hr) |
3300† ± 2130 |
11.7 ± 3.9 |
0.053 ± 0.017 |
0.85 ± 0.30 |
||
|
PO (0.3 mg/kg/day) |
68.5 ± 30.0 |
2.3 ± 1.5 |
519† ± 179 | |||||
|
Heart Transplant Patients |
11 |
IV (0.01 mg/kg/day as a continuous infusion) |
954§ ± 334 |
23.6 ± 9.22 |
0.051 ± 0.015 | |||
|
11 |
PO (0.075 mg/kg/day)¶ |
14.7 ± 7.79 |
2.1 |
82.7Þ ± 63.2 | ||||
|
14 |
PO (0.15 mg/kg/day)¶ |
24.5 ± 13.7 |
1.5 |
142Þ ± 116 | ||||
Due to intersubject variability in tacrolimus pharmacokinetics, individualization of the dosing regimen is necessary for optimal therapy [see Dosage and Administration (2.6)]. Pharmacokinetic data indicate that whole blood concentrations rather than plasma concentrations serve as the more appropriate sampling compartment to describe tacrolimus pharmacokinetics.
Absorption
Absorption of tacrolimus from the gastrointestinal tract after oral administration is incomplete and variable. The absolute bioavailability of tacrolimus was 17 ± 10% in adult kidney transplant patients (N = 26), 22 ± 6% in adult liver transplant patients (N = 17), 23 ± 9% in adult heart transplant patients (N = 11) and 18 ± 5% in healthy volunteers (N = 16).
A single dose trial conducted in 32 healthy volunteers established the bioequivalence of the 1 mg and 5 mg capsules. Another single dose trial in 32 healthy volunteers established the bioequivalence of the 0.5 mg and 1 mg capsules. Tacrolimus maximum blood concentrations (Cmax) and area under the curve (AUC) appeared to increase in a dose-proportional fashion in 18 fasted healthy volunteers receiving a single oral dose of 3, 7, and 10 mg.
In 18 kidney transplant patients, tacrolimus trough concentrations from 3 to 30 ng/mL measured at 10-12 hours post-dose (Cmin) correlated well with the AUC (correlation coefficient 0.93). In 24 liver transplant patients over a concentration range of 10 to 60 ng/mL, the correlation coefficient was 0.94. In 25 heart transplant patients over a concentration range of 2 to 24 ng/mL, the correlation coefficient was 0.89 after an oral dose of 0.075 or 0.15 mg/kg/day at steady-state.
In a healthy volunteer adult study, the systemic exposure to tacrolimus (AUC) for PROGRAF Granules was approximately 16% higher than that for PROGRAF capsules when administered as single doses. If pediatric patients are converted between formulations, therapeutic drug monitoring must be performed and dose adjustments made to ensure that systemic exposure to tacrolimus is maintained.
Food Effects
The rate and extent of tacrolimus absorption were greatest under fasted conditions. The presence and composition of food decreased both the rate and extent of tacrolimus absorption when administered to 15 healthy volunteers.
The effect was most pronounced with a high-fat meal (848 kcal, 46% fat): mean AUC and Cmax were decreased 37% and 77%, respectively; Tmax was lengthened 5-fold. A high-carbohydrate meal (668 kcal, 85% carbohydrate) decreased mean AUC and mean Cmax by 28% and 65%, respectively.
In healthy volunteers (N = 16), the time of the meal also affected tacrolimus bioavailability. When given immediately following the meal, mean Cmax was reduced 71%, and mean AUC was reduced 39%, relative to the fasted condition. When administered 1.5 hours following the meal, mean Cmax was reduced 63%, and mean AUC was reduced 39%, relative to the fasted condition.
In 11 liver transplant patients, PROGRAF administered 15 minutes after a high fat (400 kcal, 34% fat) breakfast, resulted in decreased AUC (27 ± 18%) and Cmax (50 ± 19%), as compared to a fasted state.
PROGRAF capsules should be taken consistently every day either with or without food because the presence and composition of food decreases the bioavailability of PROGRAF [see Dosage and Administration (2.1)].
Distribution
The plasma protein binding of tacrolimus is approximately 99% and is independent of concentration over a range of 5‑50 ng/mL. Tacrolimus is bound mainly to albumin and alpha-1-acid glycoprotein, and has a high level of association with erythrocytes. The distribution of tacrolimus between whole blood and plasma depends on several factors, such as hematocrit, temperature at the time of plasma separation, drug concentration, and plasma protein concentration. In a U.S. trial, the ratio of whole blood concentration to plasma concentration averaged 35 (range 12 to 67).
Elimination
Metabolism
Tacrolimus is extensively metabolized by the mixed-function oxidase system, primarily the cytochrome P-450 system (CYP3A4 and CYP3A5). A metabolic pathway leading to the formation of 8 possible metabolites has been proposed. Demethylation and hydroxylation were identified as the primary mechanisms of biotransformation in vitro. The major metabolite identified in incubations with human liver microsomes is 13-demethyl tacrolimus. In in vitro studies, a 31‑demethyl metabolite has been reported to have the same activity as tacrolimus.
Excretion
The mean clearance following IV administration of tacrolimus is 0.040, 0.083, 0.053, and 0.051 L/hr/kg in healthy volunteers, adult kidney transplant patients, adult liver transplant patients, and adult heart transplant patients, respectively. In man, less than 1% of the dose administered is excreted unchanged in urine.
In a mass balance study of IV-administered radiolabeled tacrolimus to 6 healthy volunteers, the mean recovery of radiolabel was 77.8 ± 12.7%. Fecal elimination accounted for 92.4 ± 1.0% and the elimination half-life based on radioactivity was 48.1 ± 15.9 hours whereas it was 43.5 ± 11.6 hours based on tacrolimus concentrations. The mean clearance of radiolabel was 0.029 ± 0.015 L/hr/kg and clearance of tacrolimus was 0.029 ± 0.009 L/hr/kg. When administered PO, the mean recovery of the radiolabel was 94.9 ± 30.7%. Fecal elimination accounted for 92.6 ± 30.7%, urinary elimination accounted for 2.3 ± 1.1% and the elimination half-life based on radioactivity was 31.9 ± 10.5 hours whereas it was 48.4 ± 12.3 hours based on tacrolimus concentrations. The mean clearance of radiolabel was 0.226 ± 0.116 L/hr/kg and clearance of tacrolimus was 0.172 ± 0.088 L/hr/kg.
Specific Populations
Pediatric Patients
PROGRAF capsules Pharmacokinetics in Pediatric Patients
Pharmacokinetics of tacrolimus have been studied in liver transplantation patients, 0.7 to 13.2 years of age. Following IV administration of a 0.037 mg/kg/day dose to 12 pediatric patients, mean terminal half-life, volume of distribution and clearance were 11.5 ± 3.8 hours, 2.6 ± 2.1 L/kg and 0.138 ± 0.071 L/hr/kg, respectively. Following oral administration to 9 patients, mean AUC and Cmax were 337 ± 167 ng·hr/mL and 48.4 ± 27.9 ng/mL, respectively. The absolute bioavailability was 31 ± 24%.
Pharmacokinetics of tacrolimus have also been studied in kidney transplantation patients, 8.2 ± 2.4 years of age. Following IV infusion of a 0.06 mg/kg/day to 12 pediatric patients (8 male and 4 female), mean terminal half-life and clearance were 10.2 ± 5.0 hours and 0.12 ± 0.04 L/hr/kg, respectively. Following oral administration to the same patients, mean AUC and Cmax were 181 ± 65 ng·hr/mL and 30 ± 11 ng/mL, respectively. The absolute bioavailability was 19 ± 14%.
Whole blood trough concentrations from 31 patients less than 12 years old showed that pediatric patients needed higher doses than adults to achieve similar tacrolimus trough concentrations [see Dosage and Administration (2.3)].
PROGRAF Granules Pharmacokinetics in Pediatric Patients
A multicenter, open-label, single arm, pharmacokinetic study (OPTION, NCT01371331) was conducted using tacrolimus granules for oral suspension in pediatric patients undergoing de novo liver, kidney, or heart transplant. After an initial 24‑hour continuous IV infusion of tacrolimus (0.025 mg/kg/hour) for 12 hours to 4 days, oral PROGRAF Granules were dosed at 0.3 mg/kg/day in divided doses twice daily. Tacrolimus whole blood trough concentrations ranged from 5‑15 ng/mL for the first month post-transplant, and 5-10 ng/mL thereafter. Two pharmacokinetic (PK) profiles, AUC, Cmax, Tmax and Ctrough, were taken after the first oral dose (Day 1) and at steady state (Day 7). Subsequent oral doses of PROGRAF Granules were adjusted based on clinical evidence of efficacy, the whole-blood trough levels, and/or occurrence of adverse events. Of 52 patients enrolled, thirty-eight (38) had an evaluable PK profile. The mean pediatric age was 6.1 years for heart transplant, 1.1 years for liver transplant and 3.6 years for kidney transplant. Summary results of PK parameters are presented in Table 18.
|
Population |
N (age range) |
Parameters |
||||
|
AUCtau [hr*ng/mL] mean ± SD |
Cmax [ng/mL] mean ± SD |
Tmax [hr] mean ± SD |
Ctrough [ng/mL] mean ± SD |
|||
|
Heart Transplant Patients |
12 (0.58-13 years) |
Day 1 Day 7 |
224.13 ± 114.30 165.17 ± 39.12 |
45.61 ± 19.55 32.69 ± 9.78 |
2.95 ± 4.33 0.84 ± 0.44 |
12.60 ± 13.40 7.57 ± 1.80 |
|
Liver Transplant Patients |
14 (0.33-12 years) |
Day 1 Day 7 |
210.56 ± 84.01 195.08 ± 94.63 |
25.11 ± 10.78 30.52 ± 19.35 |
2.73 ± 1.84 1.71 ± 1.12 |
13.41 ± 7.11 9.71 ± 4.03 |
|
Kidney Transplant Patients |
12 (2.42-11 years) |
Day 1 Day 7 |
97.40 ± 36.77 208.32 ± 68.75 |
18.04 ± 8.10 36.63 ± 13.97 |
1.78 ± 0.88 1.09 ± 0.61 |
3.54 ± 1.45 8.92 ± 3.59 |
Renal and Hepatic Impaired Patients
The mean pharmacokinetic parameters for tacrolimus following single administrations to adult patients with renal and hepatic impairment are given in Table 19.
|
Population (No. of Patients) |
Dose |
AUC0-t (ng·hr/mL) |
t1/2 (hr) |
V (L/kg) |
CI (L/hr/kg) |
|
Renal Impairment (n = 12) |
0.02 mg/kg/4 hr IV |
393 ± 123 (t = 60 hr) |
26.3 ± 9.2 |
1.07 ± 0.20 |
0.038 ± 0.014 |
|
Mild Hepatic Impairment (n = 6) |
0.02 mg/kg/4 hr IV |
367 ± 107 (t = 72 hr) |
60.6 ± 43.8 Range: 27.8 – 141 |
3.1 ± 1.6 |
0.042 ± 0.02 |
|
7.7 mg PO |
488 ± 320 (t = 72 hr) |
66.1 ± 44.8 Range: 29.5 – 138 |
3.7 ± 4.7* |
0.034 ± 0.019* |
|
|
Severe Hepatic Impairment (n = 6, IV) |
0.02 mg/kg/4 hr IV (n = 2) IV (n = 4) |
762 ± 204 (t = 120 hr) (t = 144 hr) |
198 ± 158 Range: 81 – 436 |
3.9 ± 1.0 |
0.017 ± 0.013 |
|
(n = 5, PO)† |
8 mg PO (n = 1) (n = 4) 4 mg PO (n = 1) |
658 (t = 120 hr) (t = 144 hr) |
119 ± 35 Range: 85 – 178 |
3.1 ± 3.4* |
0.016 ± 0.011* |
Patients with Renal Impairment
Tacrolimus pharmacokinetics, following a single IV administration, were determined in 12 patients (7 not on dialysis and 5 on dialysis, serum creatinine of 3.9 ± 1.6 and 12.0 ± 2.4 mg/dL, respectively) prior to their kidney transplant. The pharmacokinetic parameters obtained were similar for both groups. The mean clearance of tacrolimus in patients with renal dysfunction was similar to that in normal volunteers (Table 19) [see Dosage and Administration (2.2) and Use in Specific Populations (8.6)].
Patients with Hepatic Impairment
Tacrolimus pharmacokinetics have been determined in six patients with mild hepatic dysfunction (mean Pugh score: 6.2) following single IV and oral administrations. The mean clearance of tacrolimus in patients with mild hepatic dysfunction was not substantially different from that in normal volunteers (see previous table). Tacrolimus pharmacokinetics were studied in 6 patients with severe hepatic dysfunction (mean Pugh score: > 10). The mean clearance was substantially lower in patients with severe hepatic dysfunction, irrespective of the route of administration [see Dosage and Administration (2.5) and Use in Specific Populations (8.7)].
Patients with Cystic Fibrosis
Lower bioavailability of tacrolimus has been reported in patients with cystic fibrosis [see Dosage and Administration (2.2, 2.3)].
Racial or Ethnic Groups
The pharmacokinetics of tacrolimus have been studied following single IV and oral administration of PROGRAF to 10 African-American, 12 Latino-American, and 12 Caucasian healthy volunteers. There were no significant pharmacokinetic differences among the three ethnic groups following a 4-hour IV infusion of 0.015 mg/kg. However, after single oral administration of 5 mg, mean (± SD) tacrolimus Cmax in African-Americans (23.6 ± 12.1 ng/mL) was significantly lower than in Caucasians (40.2 ± 12.6 ng/mL) and the Latino-Americans (36.2 ± 15.8 ng/mL) (p < 0.01). Mean AUC0-inf tended to be lower in African-Americans (203 ± 115 ng·hr/mL) than Caucasians (344 ± 186 ng·hr/mL) and Latino-Americans (274 ± 150 ng·hr/mL). The mean (± SD) absolute oral bioavailability (F) in African-Americans (12 ± 4.5%) and Latino-Americans (14 ± 7.4%) was significantly lower than in Caucasians (19 ± 5.8%, p = 0.011). There was no significant difference in mean terminal T1/2 among the three ethnic groups (range from approximately 25 to 30 hours). A retrospective comparison of African-American and Caucasian kidney transplant patients indicated that African-American patients required higher tacrolimus doses to attain similar trough concentrations [see Dosage and Administration (2.2)].
Male and Female Patients
A formal trial to evaluate the effect of gender on tacrolimus pharmacokinetics has not been conducted, however, there was no difference in dosing by gender in the kidney transplant trial. A retrospective comparison of pharmacokinetics in healthy volunteers, and in kidney, liver, and heart transplant patients indicated no gender-based differences.
Drug Interaction Studies
Frequent monitoring of whole blood concentrations and appropriate dosage adjustments of tacrolimus are recommended when concomitant use of the following drugs with tacrolimus is initiated or discontinued [see Drug Interactions (7)].
- •
- Telaprevir: In a single-dose study in 9 healthy volunteers, co-administration of tacrolimus (0.5 mg single dose) with telaprevir (750 mg three times daily for 13 days) increased the tacrolimus dose-normalized Cmax by 9.3-fold and AUC by 70-fold compared to tacrolimus alone [see Drug Interactions (7.2)].
- •
- Boceprevir: In a single-dose study in 12 subjects, co-administration of tacrolimus (0.5 mg single dose) with boceprevir (800 mg three times daily for 11 days) increased tacrolimus Cmax by 9.9-fold and AUC by 17-fold compared to tacrolimus alone [see Drug Interactions (7.2)].
- •
- Nelfinavir: Based on a clinical study of 5 liver transplant recipients, co-administration of tacrolimus with nelfinavir increased blood concentrations of tacrolimus significantly and, as a result, a reduction in the tacrolimus dose by an average of 16-fold was needed to maintain mean trough tacrolimus blood concentrations of 9.7 ng/mL. It is recommended to avoid concomitant use of PROGRAF and nelfinavir unless the benefits outweigh the risks [see Drug Interactions (7.2)].
- •
- Rifampin: In a study of 6 normal volunteers, a significant decrease in tacrolimus oral bioavailability (14 ± 6% vs. 7 ± 3%) was observed with concomitant rifampin administration (600 mg). In addition, there was a significant increase in tacrolimus clearance (0.036 ± 0.008 L/hr/kg vs. 0.053 ± 0.010 L/hr/kg) with concomitant rifampin administration [see Drug Interactions (7.2)].
- •
- Magnesium and Aluminum-hydroxide: In a single-dose crossover study in healthy volunteers, co-administration of tacrolimus and magnesium-aluminum-hydroxide resulted in a 21% increase in the mean tacrolimus AUC and a 10% decrease in the mean tacrolimus Cmax relative to tacrolimus administration alone [see Drug Interactions (7.2)].
- •
- Ketoconazole: In a study of 6 normal volunteers, a significant increase in tacrolimus oral bioavailability (14 ± 5% vs. 30 ± 8%) was observed with concomitant ketoconazole administration (200 mg). The apparent oral clearance of tacrolimus during ketoconazole administration was significantly decreased compared to tacrolimus alone (0.430 ± 0.129 L/hr/kg vs. 0.148 ± 0.043 L/hr/kg). Overall, IV clearance of tacrolimus was not significantly changed by ketoconazole co-administration, although it was highly variable between patients [see Drug Interactions (7.2)].
- •
- Voriconazole (see complete prescribing information for VFEND): Repeat oral dose administration of voriconazole (400 mg every 12 hours for one day, then 200 mg every 12 hours for 6 days) increased tacrolimus (0.1 mg/kg single dose) Cmax and AUCτ in healthy subjects by an average of 2-fold (90% CI: 1.9, 2.5) and 3-fold (90% CI: 2.7, 3.8), respectively [see Drug Interactions (7.2)].
- •
- Posaconazole (see complete prescribing information for Noxafil): Repeat oral administration of posaconazole (400 mg twice daily for 7 days) increased tacrolimus (0.05 mg/kg single dose) Cmax and AUC in healthy subjects by an average of 2-fold (90% CI: 2.01, 2.42) and 4.5-fold (90% CI 4.03, 5.19), respectively [see Drug Interactions (7.2)].
- •
- Caspofungin (see complete prescribing information for CANCIDAS): Caspofungin reduced the blood AUC0-12 of tacrolimus by approximately 20%, peak blood concentration (Cmax) by 16%, and 12-hour blood concentration (C12hr) by 26% in healthy adult subjects when tacrolimus (2 doses of 0.1 mg/kg 12 hours apart) was administered on the 10th day of CANCIDAS 70 mg daily, as compared to results from a control period in which tacrolimus was administered alone [see Drug Interactions (7.2)]. The mechanism of interaction has not been confirmed.
13. Nonclinical Toxicology
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Carcinogenesis
Carcinogenicity studies were conducted in male and female rats and mice. In the 80-week mouse oral study and in the 104-week rat oral study, no relationship of tumor incidence to tacrolimus dosage was found. The highest dose used in the mouse was 3.0 mg/kg/day (0.9 to 2.2 times the AUC at clinical doses of 0.075 to 0.2 mg/kg/day) and in the rat was 5.0 mg/kg/day (0.265 to 0.65 times the AUC at clinical doses of 0.075 to 0.2 mg/kg/day) [see Warnings and Precautions (5.1)].
A 104-week dermal carcinogenicity study was performed in mice with tacrolimus ointment (0.03% - 3%), equivalent to tacrolimus doses of 1.1-118 mg/kg/day or 3.3-354 mg/m2/day. In the study, the incidence of skin tumors was minimal and the topical application of tacrolimus was not associated with skin tumor formation under ambient room lighting. However, a statistically significant elevation in the incidence of pleomorphic lymphoma in high-dose male (25/50) and female animals (27/50) and in the incidence of undifferentiated lymphoma in high-dose female animals (13/50) was noted in the mouse dermal carcinogenicity study. Lymphomas were noted in the mouse dermal carcinogenicity study at a daily dose of 3.5 mg/kg (0.1% tacrolimus ointment). No drug-related tumors were noted in the mouse dermal carcinogenicity study at a daily dose of 1.1 mg/kg (0.03% tacrolimus ointment). The relevance of topical administration of tacrolimus in the setting of systemic tacrolimus use is unknown.
The implications of these carcinogenicity studies to the human condition are limited; doses of tacrolimus were administered that likely induced immunosuppression in these animals, impairing their immune system’s ability to inhibit unrelated carcinogenesis.
Mutagenesis
No evidence of genotoxicity was seen in bacterial (Salmonella and E. coli) or mammalian (Chinese hamster lung-derived cells) in vitro assays of mutagenicity, the in vitro CHO/HGPRT assay of mutagenicity, or in vivo clastogenicity assays performed in mice; tacrolimus did not cause unscheduled DNA synthesis in rodent hepatocytes.
Impairment of Fertility
Tacrolimus, subcutaneously administered to male rats at paternally toxic doses of 2 mg/kg/day (1.6 to 4.3 times the recommended clinical dose range [0.2 to 0.075 mg/kg/day] on a mg/m2 basis) or 3 mg/kg/day (2.4 to 6.4 times the recommended clinical dose range), resulted in a dose-related decrease in sperm count. Tacrolimus, administered orally at 1.0 mg/kg (0.8 to 2.2 times the clinical dose range) to male and female rats, prior to and during mating, as well as to dams during gestation and lactation, was associated with embryolethality and adverse effects on female reproduction. Effects on female reproductive function (parturition) and embryolethal effects were indicated by a higher rate of pre- and post-implantation loss and increased numbers of undelivered and nonviable pups. When administered at 3.2 mg/kg (2.6 to 6.9 times the clinical dose range based on body surface area), tacrolimus was associated with maternal and paternal toxicity as well as reproductive toxicity including marked adverse effects on estrus cycles, parturition, pup viability, and pup malformations.
14. Clinical Studies
14.1 Kidney Transplantation
PROGRAF/Azathioprine (AZA)
PROGRAF-based immunosuppression in conjunction with azathioprine and corticosteroids following kidney transplantation was assessed in a randomized, multicenter, non-blinded, prospective trial. There were 412 kidney transplant patients enrolled at 19 clinical sites in the United States. Study therapy was initiated when renal function was stable as indicated by a serum creatinine ≤ 4 mg/dL (median of 4 days after transplantation, range 1 to 14 days). Patients less than 6 years of age were excluded.
There were 205 patients randomized to PROGRAF-based immunosuppression and 207 patients were randomized to cyclosporine-based immunosuppression. All patients received prophylactic induction therapy consisting of an antilymphocyte antibody preparation, corticosteroids, and azathioprine. Overall, 1-year patient and graft survivals were 96.1% and 89.6%, respectively.
Data from this trial of PROGRAF in conjunction with azathioprine indicate that during the first 3 months of that trial, 80% of the patients maintained trough concentrations between 7-20 ng/mL, and then between 5-15 ng/mL, through 1 year.
PROGRAF/Mycophenolate Mofetil (MMF)
PROGRAF-based immunosuppression in conjunction with MMF, corticosteroids, and induction has been studied. In a randomized, open-label, multicenter trial (Study 1), 1589 kidney transplant patients received PROGRAF (Group C, n = 401), sirolimus (Group D, n = 399), or one of two cyclosporine (CsA) regimens (Group A, n = 390 and Group B, n = 399) in combination with MMF and corticosteroids; all patients, except those in one of the two cyclosporine groups, also received induction with daclizumab. The trial was conducted outside the United States; the trial population was 93% Caucasian. In this trial, mortality at 12 months in patients receiving PROGRAF/MMF was similar (3%) compared to patients receiving cyclosporine/MMF (3% and 2%) or sirolimus/MMF (3%). Patients in the PROGRAF group exhibited higher estimated creatinine clearance rates (eCLcr) using the Cockcroft-Gault formula (Table 20) and experienced fewer efficacy failures, defined as biopsy-proven acute rejection (BPAR), graft loss, death, and/or loss to follow-up (Table 21) in comparison to each of the other three groups. Patients randomized to PROGRAF/MMF were more likely to develop diarrhea and diabetes after the transplantation and experienced similar rates of infections compared to patients randomized to either cyclosporine/MMF regimen [see Adverse Reactions (6.1)].
| Group | eCLcr [mL/min] at Month 12* | ||||
|---|---|---|---|---|---|
| N | MEAN | SD | MEDIAN | Treatment Difference with Group C (99.2% CI†) |
|
|
|||||
|
(A) CsA/MMF/CS |
390 |
56.5 |
25.8 |
56.9 |
-8.6 (-13.7, -3.7) |
|
(B) CsA/MMF/CS/Daclizumab |
399 |
58.9 |
25.6 |
60.9 |
-6.2 (-11.2, -1.2) |
|
(C) Tac/MMF/CS/Daclizumab |
401 |
65.1 |
27.4 |
66.2 |
- |
|
(D) Siro/MMF/CS/Daclizumab |
399 |
56.2 |
27.4 |
57.3 |
-8.9 (-14.1, -3.9) |
|
Total |
1589 |
59.2 |
26.8 |
60.5 | |
|
Key: CsA = Cyclosporine, CS = Corticosteroids, Tac = Tacrolimus, Siro = Sirolimus |
|||||
| Group A
N = 390 | Group B
N = 399 | Group C
N = 401 | Group D
N = 399 |
|
|---|---|---|---|---|
|
||||
|
Overall Failure |
141 (36.2%) |
126 (31.6%) |
82 (20.4%) |
185 (46.4%) |
|
Components of efficacy failure | ||||
|
BPAR |
113 (29.0%) |
106 (26.6%) |
60 (15.0%) |
152 (38.1%) |
|
Graft loss excluding death |
28 (7.2%) |
20 (5.0%) |
12 (3.0%) |
30 (7.5%) |
|
Mortality |
13 (3.3%) |
7 (1.8%) |
11 (2.7%) |
12 (3.0%) |
|
Lost to follow-up |
5 (1.3%) |
7 (1.8%) |
5 (1.3%) |
6 (1.5%) |
|
Treatment Difference of efficacy failure compared to Group C (99.2% CI*) |
15.8% (7.1%, 24.3%) |
11.2% (2.7%, 19.5%) |
- |
26.0% (17.2%, 34.7%) |
|
Key: Group A = CsA/MMF/CS, B = CsA/MMF/CS/Daclizumab, C = Tac/MMF/CS/Daclizumab, and D = Siro/MMF/CS/Daclizumab |
||||
The protocol-specified target tacrolimus trough concentrations (Ctrough,Tac) were 3-7 ng/mL; however, the observed median Ctroughs,Tac approximated 7 ng/mL throughout the 12-month trial (Table 22). Approximately 80% of patients maintained tacrolimus whole blood concentrations between 4-11 ng/mL through 1 year post-transplant.
| Time | Median (P10-P90*) tacrolimus whole blood trough concentration range
(ng/mL) |
|---|---|
|
|
|
Day 30 (N = 366) |
6.9 (4.4 – 11.3) |
|
Day 90 (N = 351) |
6.8 (4.1 – 10.7) |
|
Day 180 (N = 355) |
6.5 (4.0 – 9.6) |
|
Day 365 (N = 346) |
6.5 (3.8 – 10.0) |
The protocol-specified target cyclosporine trough concentrations (Ctrough,CsA) for Group B were 50-100 ng/mL; however, the observed median Ctroughs,CsA approximated 100 ng/mL throughout the 12-month trial. The protocol-specified target Ctroughs,CsA for Group A were 150-300 ng/mL for the first 3 months and 100-200 ng/mL from month 4 to month 12; the observed median Ctroughs,CsA approximated 225 ng/mL for the first 3 months and 140 ng/mL from month 4 to month 12.
While patients in all groups started MMF at 1 gram twice daily, the MMF dose was reduced to less than 2 g per day in 63% of patients in the tacrolimus treatment arm by month 12 (Table 23); approximately 50% of these MMF dose reductions were due to adverse reactions. By comparison, the MMF dose was reduced to less than 2 g per day in 49% and 45% of patients in the two cyclosporine arms (Group A and Group B, respectively), by month 12 and approximately 40% of MMF dose reductions were due to adverse reactions.
| Time period (Days) | Time-averaged MMF dose (grams per day)* | ||
|---|---|---|---|
| Less than 2.0 | 2.0 | Greater than 2.0 | |
|
|||
|
0-30 (N = 364) |
37% |
60% |
2% |
|
0-90 (N = 373) |
47% |
51% |
2% |
|
0-180 (N = 377) |
56% |
42% |
2% |
|
0-365 (N = 380) |
63% |
36% |
1% |
|
Key: Time-averaged MMF dose = (total MMF dose)/(duration of treatment) |
|||
In a second randomized, open-label, multicenter trial (Study 2), 424 kidney transplant patients received PROGRAF (N = 212) or cyclosporine (N = 212) in combination with MMF 1 gram twice daily, basiliximab induction, and corticosteroids. In this trial, the rate for the combined endpoint of BPAR, graft failure, death, and/or lost to follow-up at 12 months in the PROGRAF/MMF group was similar to the rate in the cyclosporine/MMF group. There was, however, an imbalance in mortality at 12 months in those patients receiving PROGRAF/MMF (4%) compared to those receiving cyclosporine/MMF (2%), including cases attributed to over-immunosuppression (Table 24).
| PROGRAF/MMF | Cyclosporine/MMF | |
|---|---|---|
| (N = 212) | (N = 212) | |
|
||
|
Overall Failure |
32 (15.1%) |
36 (17.0%) |
|
Components of efficacy failure |
|
|
|
BPAR |
16 (7.5%) |
29 (13.7%) |
|
Graft loss excluding death |
6 (2.8%) |
4 (1.9%) |
|
Mortality |
9 (4.2%) |
5 (2.4%) |
|
Lost to follow-up |
4 (1.9%) |
1 (0.5%) |
|
Treatment Difference of efficacy failure compared to PROGRAF/MMF group (95% CI*) |
|
1.9% (-5.2%, 9.0%) |
The protocol-specified target tacrolimus whole blood trough concentrations (Ctrough,Tac) in Study 2 were 7-16 ng/mL for the first three months and 5-15 ng/mL thereafter. The observed median Ctroughs,Tac approximated 10 ng/mL during the first three months and 8 ng/mL from month 4 to month 12 (Table 25). Approximately 80% of patients maintained tacrolimus whole blood trough concentrations between 6 to 16 ng/mL during months 1 through 3 and, then, between 5 to 12 ng/mL from month 4 through 1 year.
| Time | Median (P10-P90*) tacrolimus whole blood trough concentration range
(ng/mL) |
|---|---|
|
|
|
Day 30 (N = 174) |
10.5 (6.3 – 16.8) |
|
Day 60 (N = 179) |
9.2 (5.9 – 15.3) |
|
Day 120 (N = 176) |
8.3 (4.6 – 13.3) |
|
Day 180 (N = 171) |
7.8 (5.5 – 13.2) |
|
Day 365 (N = 178) |
7.1 (4.2 – 12.4) |
The protocol-specified target cyclosporine whole blood concentrations (Ctrough,CsA) were 125 to 400 ng/mL for the first three months, and 100 to 300 ng/mL thereafter. The observed median Ctroughs,CsA approximated 280 ng/mL during the first three months and 190 ng/mL from month 4 to month 12.
Patients in both groups started MMF at 1 gram twice daily. The MMF dose was reduced to less than 2 grams per day by month 12 in 62% of patients in the PROGRAF/MMF group (Table 26) and in 47% of patients in the cyclosporine/MMF group. Approximately 63% and 55% of these MMF dose reductions were because of adverse reactions in the PROGRAF/MMF group and the cyclosporine/MMF group, respectively [see Adverse Reactions (6.1)].
| Time period (Days) | Time-averaged MMF dose (g/day)* | ||
|---|---|---|---|
| Less than 2.0 | 2.0 | Greater than 2.0 | |
|
|||
|
0-30 (N = 212) |
25% |
69% |
6% |
|
0-90 (N = 212) |
41% |
53% |
6% |
|
0-180 (N = 212) |
52% |
41% |
7% |
|
0-365 (N = 212) |
62% |
34% |
4% |
|
Key: Time-averaged MMF dose = (total MMF dose)/(duration of treatment) |
|||
14.2 Liver Transplantation
The safety and efficacy of PROGRAF-based immunosuppression following orthotopic liver transplantation were assessed in two prospective, randomized, non-blinded multicenter trials. The active control groups were treated with a cyclosporine-based immunosuppressive regimen (CsA/AZA). Both trials used concomitant adrenal corticosteroids as part of the immunosuppressive regimens. These trials compared patient and graft survival rates at 12 months following transplantation.
In one trial, 529 patients were enrolled at 12 clinical sites in the United States; prior to surgery, 263 were randomized to the PROGRAF-based immunosuppressive regimen and 266 to the CsA/AZA. In 10 of the 12 sites, the same CsA/AZA protocol was used, while 2 sites used different control protocols. This trial excluded patients with renal dysfunction, fulminant hepatic failure with Stage IV encephalopathy, and cancers; pediatric patients (≤ 12 years old) were allowed.
In the second trial, 545 patients were enrolled at 8 clinical sites in Europe; prior to surgery, 270 were randomized to the PROGRAF-based immunosuppressive regimen and 275 to CsA/AZA. In this trial, each center used its local standard CsA/AZA protocol in the active-control arm. This trial excluded pediatric patients, but did allow enrollment of subjects with renal dysfunction, fulminant hepatic failure in Stage IV encephalopathy, and cancers other than primary hepatic with metastases.
One-year patient survival and graft survival in the PROGRAF-based treatment groups were similar to those in the CsA/AZA treatment groups in both trials. The overall 1-year patient survival (CsA/AZA and PROGRAF-based treatment groups combined) was 88% in the U.S. trial and 78% in the European trial. The overall 1-year graft survival (CsA/AZA and PROGRAF-based treatment groups combined) was 81% in the U.S. trial and 73% in the European trial. In both trials, the median time to convert from IV to oral PROGRAF dosing was 2 days.
Although there is a lack of direct correlation between tacrolimus concentrations and drug efficacy, data from clinical trials of liver transplant patients have shown an increasing incidence of adverse reactions with increasing trough blood concentrations. Most patients are stable when trough whole blood concentrations are maintained between 5 to 20 ng/mL. Long-term post-transplant patients are often maintained at the low end of this target range.
Data from the U.S. clinical trial show that the median trough blood concentrations, measured at intervals from the second week to one year post-transplantation, ranged from 9.8 ng/mL to 19.4 ng/mL.
Pediatric Liver Transplantation Using PROGRAF Granules
The efficacy and safety of PROGRAF Granules plus corticosteroids were compared with a triple regimen of cyclosporine/corticosteroids/azathioprine in a randomized, open-label study, in de novo pediatric liver transplant patients. The study was conducted outside the United States and enrolled patients aged 16 years or younger. The distribution of pediatric patients by age was similar in both treatment groups, with a majority < 5 years. Patients were randomized to either tacrolimus for oral suspension 0.3 mg/kg/day (N = 91) or cyclosporine 10 mg/kg/day orally (N = 90) initiated 6 hours after completion of transplant surgery. Doses throughout the 1-year study period were adjusted to maintain whole blood trough levels within 5-20 ng/mL [see Dosage and Administration (2.3)]. Based on trough levels, doses of tacrolimus were adjusted to 0.17 mg/kg/day and 0.14 mg/kg/day by days 2 and 3, respectively. At 12 months, the incidence rate of BPAR, graft loss, death, or loss to follow-up was 52.7% in the tacrolimus group and 61.1% in the cyclosporine group (Table 27).
| PROGRAF Granules
(N = 91) | Cyclosporine
(N = 90) |
|
|---|---|---|
|
||
|
Overall Failure |
48 (52.7%) |
55 (61.1%) |
|
Components of efficacy failure |
||
|
BPAR |
40 (44.0%) |
49 (54.4%) |
|
Graft loss |
7 (7.7%) |
13 (14.4%) |
|
Graft loss excluding death |
1 (1.1%) |
6 (6.7%) |
|
Mortality |
6 (6.6%) |
7 (7.8%) |
|
Lost to follow-up |
2 (2.2%) |
0 |
|
Treatment Difference of efficacy failure compared to cyclosporine (95% CI*) |
-8.4% (-22.7%, 6.0%) | |
14.3 Heart Transplantation
Two open-label, randomized, comparative trials evaluated the safety and efficacy of PROGRAF-based and cyclosporine-based immunosuppression in primary orthotopic heart transplantation. In a trial conducted in Europe, 314 patients received a regimen of antibody induction, corticosteroids, and azathioprine in combination with PROGRAF or cyclosporine modified for 18 months. In a 3-arm trial conducted in the U.S., 331 patients received corticosteroids and PROGRAF plus sirolimus, PROGRAF plus mycophenolate mofetil (MMF) or cyclosporine modified plus MMF for 1 year.
In the European trial, patient/graft survival at 18 months post-transplant was similar between treatment arms, 92% in the tacrolimus group and 90% in the cyclosporine group. In the U.S. trial, patient and graft survival at 12 months was similar with 93% survival in the PROGRAF plus MMF group and 86% survival in the cyclosporine modified plus MMF group. In the European trial, the cyclosporine trough concentrations were above the pre-defined target range (i.e., 100 to 200 ng/mL) at Day 122 and beyond in 32% to 68% of the patients in the cyclosporine treatment arm, whereas the tacrolimus trough concentrations were within the pre-defined target range (i.e., 5 to 15 ng/mL) in 74% to 86% of the patients in the tacrolimus treatment arm. Data from this European trial indicate that from 1 week to 3 months post-transplant, approximately 80% of patients maintained trough concentrations between 8 to 20 ng/mL and, from 3 months through 18 months post-transplant, approximately 80% of patients maintained trough concentrations between 6 to 18 ng/mL.
The U.S. trial contained a third arm of a combination regimen of sirolimus, 2 mg per day, and full-dose PROGRAF; however, this regimen was associated with increased risk of wound-healing complications, renal function impairment, and insulin-dependent post-transplant diabetes mellitus, and is not recommended [see Warnings and Precautions (5.10)].
14.4 Lung Transplantation
The efficacy and safety of PROGRAF-based immunosuppression in primary lung transplantation were assessed in a non-interventional (observational) study using data from the U.S. Scientific Registry of Transplant Recipients (SRTR). The study analyzed outcomes based on discharge immunosuppression treatment regimen in recipients of a primary lung transplant between 1999 and 2017 who were alive at the time of discharge. In adult patients receiving tacrolimus immediate-release products in combination with MMF (n=15,478) or tacrolimus immediate-release products in combination with AZA (n=4,263), the one-year graft survival estimates from time of discharge were 90.9% and 90.8%, respectively. In pediatric patients receiving tacrolimus immediate-release products in combination with MMF (n= 450) or tacrolimus immediate-release products in combination with AZA (n=72), the one-year graft survival estimates from time of discharge were 91.7% and 84.7%, respectively.
16. How is Prograf supplied
16.1 PROGRAF (tacrolimus) Capsules, USP
|
Strength |
0.5 mg (containing the equivalent of 0.5 mg anhydrous tacrolimus USP) |
1 mg (containing the equivalent of 1 mg anhydrous tacrolimus USP) |
5 mg (containing the equivalent of 5 mg anhydrous tacrolimus USP) |
|
Shape/color |
oblong/light yellow |
oblong/white |
oblong/grayish red |
|
Branding on capsule cap/body | |||
|
100 count bottle |
NDC 0469-0607-73 |
NDC 0469-0617-73 |
NDC 0469-0657-73 |
Note: PROGRAF capsules USP are not filled to maximum capsule capacity. Capsule contains labeled amount.
Store and Dispense
Store at 20°C to 25°C (68°F to 77°F); excursions permitted 15°C to 30°C (59°F to 86°F) [See USP Controlled Room Temperature].
16.2 PROGRAF (tacrolimus) Injection
(for Intravenous infusion only)
NDC 0469-3016-01 Product Code 301601
5 mg/mL (equivalent of 5 mg of anhydrous tacrolimus USP per mL) supplied as a sterile solution in a 1 mL ampule, in boxes of 10 ampules
Store and Dispense
Store between 5°C and 25°C (41°F and 77°F).
16.3 PROGRAF Granules (tacrolimus for oral suspension)
|
Strength |
0.2 mg (containing the equivalent of 0.2 mg anhydrous tacrolimus USP) |
1 mg (containing the equivalent of 1 mg anhydrous tacrolimus USP) |
|
Shape/color |
White granules |
White granules |
|
1 carton containing 50 packets |
NDC 0469-1230-50 |
NDC 0469-1330-50 |
Store and Dispense
Store at 20°C to 25°C (68°F to 77°F); excursions permitted 15°C to 30°C (59°F to 86°F) [See USP Controlled Room Temperature].
16.4 Handling and Disposal
Tacrolimus can cause fetal harm. PROGRAF capsules should not be opened or crushed. Wearing disposable gloves is recommended during dilution of the injection or when preparing the oral suspension in the hospital and when wiping any spills. Avoid inhalation or direct contact with skin or mucous membranes of the powder or granules contained in PROGRAF capsules and PROGRAF Granules, respectively. If such contact occurs, wash the skin thoroughly with soap and water; if ocular contact occurs, rinse eyes with water. In case a spill occurs, wipe the surface with a wet paper towel. Follow applicable special handling and disposal procedures1.
17. Patient Counseling Information
Advise the patient to read the FDA-approved patient labeling (Patient Information and Instructions for Use).
17.1 Administration
Advise the patient or caregiver to:
- •
- Inspect their PROGRAF medicine when they receive a new prescription and before taking it. If the appearance of the capsule is not the same as usual, or if dosage instructions have changed, advise patients to contact their healthcare provider as soon as possible to make sure that they have the right medicine. Other tacrolimus products cannot be substituted for PROGRAF.
- •
- Take PROGRAF at the same 12-hour intervals every day to achieve consistent blood concentrations.
- •
- Take PROGRAF consistently either with or without food because the presence and composition of food decreases the bioavailability of PROGRAF.
- •
- Not to eat grapefruit or drink grapefruit juice in combination with PROGRAF [see Drug Interactions (7.2)].
- •
- If the patient is receiving PROGRAF Granules, advise that the dose should be given immediately after preparation and not to save the dose for later. Advise the caregiver to carefully read the Instructions for Use.
17.2 Development of Lymphoma and Other Malignancies
Inform patients they are at increased risk of developing lymphomas and other malignancies, particularly of the skin, due to immunosuppression. Advise patients to limit exposure to sunlight and ultraviolet (UV) light by wearing protective clothing and using a broad spectrum sunscreen with a high protection factor [see Warnings and Precautions (5.1)].
17.3 Increased Risk of Infection
Inform patients they are at increased risk of developing a variety of infections, including opportunistic infections, due to immunosuppression and to contact their physician if they develop any symptoms of infection such as fever, sweats or chills, cough or flu-like symptoms, muscle aches, or warm, red, painful areas on the skin [see Warnings and Precautions (5.2)].
17.4 New Onset Diabetes After Transplant
Inform patients that PROGRAF can cause diabetes mellitus and should be advised to contact their physician if they develop frequent urination, increased thirst, or hunger [see Warnings and Precautions (5.4)].
17.5 Nephrotoxicity
Inform patients that PROGRAF can have toxic effects on the kidney that should be monitored. Advise patients to attend all visits and complete all blood tests ordered by their medical team [see Warnings and Precautions (5.5)].
17.6 Neurotoxicity
Inform patients that they are at risk of developing adverse neurologic reactions including seizure, altered mental status, and tremor. Advise patients to contact their physician should they develop vision changes, delirium, or tremors [see Warnings and Precautions (5.6)].
17.7 Hyperkalemia
Inform patients that PROGRAF can cause hyperkalemia. Monitoring of potassium levels may be necessary, especially with concomitant use of other drugs known to cause hyperkalemia [see Warnings and Precautions (5.7)].
17.8 Hypertension
Inform patients that PROGRAF can cause high blood pressure which may require treatment with antihypertensive therapy. Advise patients to monitor their blood pressure [see Warnings and Precautions (5.8)].
17.9 Thrombotic Microangiopathy
Inform patients that PROGRAF can cause blood clotting problems. The risk of this occurring increases when patients take PROGRAF and sirolimus or everolimus concomitantly, or when patients develop certain infections. Advise them to seek medical attention promptly if they develop fever, petequiae or bruises, fatigue, confusion, jaundice, oliguria. [see Warnings and Precautions (5.16)]
17.10 Drug Interactions
Instruct patients to tell their healthcare providers when they start or stop taking any medicines, including prescription medicines and nonprescription medicines, natural or herbal remedies, nutritional supplements, and vitamins. Advise patients to avoid grapefruit and grapefruit juice [see Drug Interactions (7)].
17.11 Pregnancy, Lactation and Infertility
Inform women of childbearing potential that PROGRAF can harm the fetus. Instruct male and female patients to discuss with their healthcare provider family planning options including appropriate contraception. Also, discuss with pregnant patients the risks and benefits of breastfeeding their infant [see Use in Specific Populations (8.1, 8.2, 8.3)].
Encourage female transplant patients who become pregnant and male patients who have fathered a pregnancy, exposed to immunosuppressants including tacrolimus, to enroll in the voluntary Transplantation Pregnancy Registry International. To enroll or register, patients can call the toll free number 1-877-955-6877 or https://www.transplantpregnancyregistry.org/ [see Use in Specific Populations (8.1)].
Based on animal studies, PROGRAF may affect fertility in males and females [see Nonclinical Toxicology (13.1)].
17.12 Myocardial Hypertrophy
Inform patients to report symptoms of tiredness, swelling, and/or shortness of breath (heart failure).
17.13 Immunizations
Inform patients that PROGRAF can interfere with the usual response to immunizations and that they should avoid live vaccines. [see Warnings and Precautions (5.14)].
Distributed by:
Astellas Pharma US, Inc.
Northbrook, IL 60062
PROGRAF® is a registered trademark of Astellas Pharma Inc. All other trademarks and registered trademarks are the property of their respective owners.
398977-PRG
|
Patient Information PROGRAF® (PRO-graf) (tacrolimus) capsules, for oral use PROGRAF® (PRO-graf) Granules (tacrolimus for oral suspension) |
||
|
Read this Patient Information before you start taking PROGRAF and each time you get a refill. There may be new information. This information does not take the place of talking with your healthcare provider about your medical condition or your treatment. |
||
|
What is the most important information I should know about PROGRAF? PROGRAF can cause serious side effects, including:
|
||
|
|
|
|
What is PROGRAF?
|
||
|
Who should not take PROGRAF? Do not take PROGRAF if you:
|
||
|
What should I tell my healthcare provider before taking PROGRAF? Before taking PROGRAF, tell your healthcare provider about all of your medical conditions, including if you:
Tell your healthcare provider about all the medicines you take, and when you start a new medicine or stop taking a medicine, including prescription and over-the-counter medicines, vitamins, natural, herbal, or nutritional supplements. Especially tell your healthcare provider if you take:
Ask your healthcare provider or pharmacist if you are not sure if you take any of the medicines listed above. PROGRAF may affect the way other medicines work, and other medicines may affect how PROGRAF works. Know the medicines you take. Keep a list of your medicines and show it to your healthcare provider and pharmacist when you get a new medicine. |
||
|
How should I take PROGRAF?
PROGRAF capsules:
PROGRAF Granules:
|
||
|
What should I avoid while taking PROGRAF?
|
||
|
What are the possible side effects of PROGRAF? PROGRAF may cause serious side effects, including:
|
||
|
|
|
|
||
|
|
|
|
||
|
|
|
|
||
|
The most common side effects of PROGRAF in people who have received a kidney, liver, heart, or lung transplant are: |
||
|
|
|
|
Tell your healthcare provider if you have any side effect that bothers you or that does not go away. These are not all the possible side effects of PROGRAF. For more information, ask your healthcare provider or pharmacist. Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088. |
||
|
How should I store PROGRAF? PROGRAF capsules
PROGRAF Granules
Keep PROGRAF and all medicines out of the reach of children. |
||
|
General information about the safe and effective use of PROGRAF.
|
||
|
What are the ingredients in PROGRAF? Active ingredient: tacrolimus Inactive ingredients: PROGRAF capsules: croscarmellose sodium, hypromellose, lactose monohydrate, and magnesium stearate. The 0.5 mg capsule shell contains ferric oxide, gelatin, and titanium dioxide. The 1 mg capsule shell contains gelatin and titanium dioxide. The 5 mg capsule shell contains ferric oxide, gelatin, and titanium dioxide. PROGRAF Granules: croscarmellose sodium, hypromellose, and lactose monohydrate. Distributed by: Astellas Pharma US, Inc. Northbrook, IL 60062 PROGRAF® is a registered trademark of Astellas Pharma Inc. All other trademarks and registered trademarks are the property of their respective owners. 398977-PRG For more information, go to www.astellas.com/us or call 1-800-727-7003. |
||
This Patient Information has been approved by the U.S. Food and Drug Administration. Revised: 08/2023
Instructions for Use
PROGRAF® Granules
(PRO-graf)
(tacrolimus for oral suspension)
Your healthcare provider has prescribed PROGRAF® Granules, which comes in individual packets that will need to be mixed with water before giving the medicine to your child.
Read this Instructions for Use and the Patient Information for the first time and each time you get a refill of PROGRAF Granules (tacrolimus for oral suspension). There may be new information.
This Instructions for Use does not take the place of talking to your child’s healthcare provider about their medical condition or treatment. Ask the healthcare provider if you have any questions about how to mix or give a dose of PROGRAF Granules the right way.
Important information:
These instructions are for preparing PROGRAF Granules only.
These instructions should not be used for PROGRAF capsules.
- •
- Mix PROGRAF Granules in water to make an oral suspension.
- •
- Give all of the prepared oral suspension to your child right away after preparing. Do not save the prepared oral suspension for later use.
- •
-
Use glass or metal materials to prepare your child’s dose of PROGRAF Granules.
- o
- Do not use any plastic (PVC) materials to prepare PROGRAF Granules. The granules will stick to a plastic container and your child may not receive their full dose.
- •
-
Do not breathe in (inhale) or let the granules in PROGRAF or the prepared oral suspension come in contact with your skin or eyes.
- o
- If you get the granules or the prepared oral suspension on your skin, wash the area well with soap and water.
- o
- If you get the granules or the prepared oral suspension in your eyes, rinse with plain water.
If you spill the granules, wipe the surface with a wet paper towel. If you spill the prepared oral suspension, dry the area with a dry paper towel and then wipe the area with a wet paper towel. Throw away the paper towels in the trash and wash your hands well with soap and water.
For each dose of PROGRAF Granules mixed with water that will be given using a glass cup, you will need the following supplies (See Figure A):
- •
- Carton containing PROGRAF Granules packets. Follow the instructions on the carton for the number of packets your child’s healthcare provider has prescribed for each dose.
- •
- paper towels
- •
- pair of scissors
- •
- metal stirring spoon
- •
- measuring device
- •
- 1 small clean glass cup (plastic containers should not be used)
- •
- container with drinking water
Figure A
For each dose of PROGRAF Granules (tacrolimus for oral suspension) mixed with water that will be drawn up and given using an oral syringe, you will need the following supplies (See Figure B):
- •
- Carton containing PROGRAF Granules packets. Follow the instructions on the carton for the number of packets your child’s healthcare provider has prescribed for each dose.
- •
- paper towels
- •
- pair of scissors
- •
- metal stirring spoon
- •
- measuring device
- •
- 1 small clean glass cup (plastic containers should not be used)
- •
- container with drinking water
- •
- 1 non-PVC oral syringe (ask your pharmacist for the oral syringe you should use)
Figure B
How should I store PROGRAF Granules packets?
Store PROGRAF Granules packets at room temperature between 68°F to 77°F (20°C to 25°C).
Do not throw away any medicines via wastewater or household waste. Ask your pharmacist how to throw away medicines you no longer use.
Keep PROGRAF Granules and all medicine out of the reach of children.
This Instructions for Use has been approved by the U.S. Food and Drug Administration.
Distributed by:
Astellas Pharma US, Inc.
Northbrook, IL 60062
PROGRAF® is a registered trademark of Astellas Pharma Inc.
341124-PRG
Revised: 11/2022
| PROGRAF
tacrolimus capsule, gelatin coated |
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
| PROGRAF
tacrolimus capsule, gelatin coated |
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
| PROGRAF
tacrolimus capsule, gelatin coated |
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
| PROGRAF
tacrolimus injection, solution |
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
| PROGRAF
tacrolimus granule, for suspension |
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
| PROGRAF
tacrolimus granule, for suspension |
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
| Labeler - Astellas Pharma US, Inc. (605764828) |
Frequently asked questions
More about Prograf (tacrolimus)
- Check interactions
- Compare alternatives
- Pricing & coupons
- Reviews (28)
- Drug images
- Latest FDA alerts (2)
- Side effects
- Dosage information
- During pregnancy
- Generic availability
- FDA approval history
- Drug class: calcineurin inhibitors
- Breastfeeding
- En español
Patient resources
- Prograf drug information
- Prograf (Tacrolimus Intravenous) (Advanced Reading)
- Prograf (Tacrolimus Oral) (Advanced Reading)

 607” on capsule body
607” on capsule body 617” on capsule body
617” on capsule body 657” on capsule body
657” on capsule body
 607
607 617
617 657
657