Molluscum contagiosum
Medically reviewed by Drugs.com. Last updated on Oct 7, 2024.
What is molluscum contagiosum?

Molluscum contagiosum is a skin disease caused by a virus that causes clusters of tiny, firm, flesh-colored or pearly bumps. The infection is mainly spread by direct skin-to-skin contact. The bumps or lesions appear at the site of contact anywhere on the body except the palms of the hands and soles of the feet.
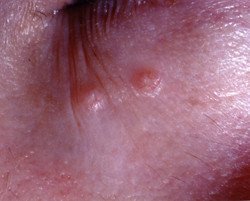
Symptoms of molluscum contagiosum
Usually, the only symptom of molluscum contagiosum is the tiny bumps on the skin. These flesh-colored or pearly growths look somewhat like tiny pimples with a central crater. A waxy substance may come out of the bumps when they are squeezed. Itching may also occur.
In children, the bumps tend to appear on the face, arms, legs and middle of the body. In adults, molluscum contagiosum tends to appear on the genitals, thighs, and lower abdomen because the infection usually is spread through sexual contact.
The bumps usually are grouped in one or two areas, but also can appear in many places on the body. Most people have fewer than 20 bumps. But people with weakened immune systems can develop several hundred bumps.
The bumps start out small, but can grow up to 3 to 6 millimeters (about 1/4 inch or less). In rare cases, the bumps can become as large as about an inch. This might happen in a person with a weakened immune system, such as someone with advanced HIV infection.
Many people itch at the site of the lesions, but for some people the bumps cause no symptoms.
Diagnosing molluscum contagiosum
Your doctor usually can diagnose molluscum contagiosum by looking at the skin bumps. If there is some question about the diagnosis, the doctor may do a biopsy, removing a small piece of a bump for examination under a microscope.
Expected duration of molluscum contagiosum
Individual bumps can last two to four months. But the disease can spread to other areas if the bumps come in contact with an uninfected area of skin, or if you touch a bump then touch an uninfected area. In most people, all lesions go away within six to nine months. However, in some people with weakened immune systems, the disease can last for years.
Preventing molluscum contagiosum
The only way to prevent molluscum contagiosum is to avoid close contact with people who have the disease.
Drugs used to treat this and similar conditions
Treatment options
The following list of medications are related to or used in the treatment of this condition.
Treating molluscum contagiosum
The infection may heal on its own after several months.
However, you or your child may want treatment to decrease the risk of infecting others and spreading to other parts of the body. Your doctor can remove the bumps in the office. He or she can freeze them with liquid nitrogen or scrape them off the skin.
In people with HIV and other conditions that weaken the immune system, it's harder to get rid of the bumps. However, if the immune system is improved by treating the HIV with HAART (highly active antiretroviral therapy), the lesions often go away on their own.
For people that continue to have molluscum, other possible treatments include cantharidin applied by a clinician in the office and laser surgery.
When o call a professional
See your doctor if you develop unexplained skin bumps. There are many different causes of skin eruptions, and a health professional can determine if you need treatment.
Prognosis
See your doctor if you develop unexplained skin bumps. There are many different causes of skin eruptions, and a health professional can determine if you need treatment.
Additional info
American Academy of Dermatology
https://www.aad.org/
Learn more about Molluscum contagiosum
Treatment options
Care guides
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
