Total Thyroidectomy
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
AMBULATORY CARE:
What you need to know about a total thyroidectomy:
A total thyroidectomy is surgery to remove all of your thyroid gland.
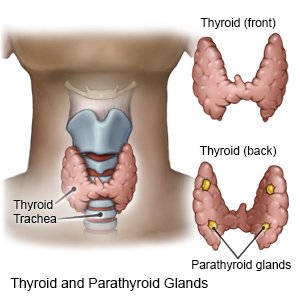 |
How to prepare for a total thyroidectomy:
- Your surgeon will tell you how to prepare. You may be told not to eat or drink anything after midnight on the day of surgery. Arrange to have someone drive you home when you are discharged.
- Tell your surgeon about all medicines you currently take. Your surgeon will tell you if you need to stop any medicine for the surgery, and when to stop. Your surgeon will tell you which medicines to take or not take on the day of surgery.
- Tell your surgeon about any allergies you have, including to anesthesia or medicines. You may be given antithyroid medicine to lower the amount of thyroid hormone made by your thyroid gland.
- You may need blood tests before your surgery to check the amounts of calcium and thyroid hormone in your blood. You may also need ultrasound, CT, or MRI pictures of your thyroid. This will help your surgeon plan your surgery.
What will happen during a total thyroidectomy:
- You will be given general anesthesia to keep you asleep and free from pain during surgery. Your surgeon will make 1 or more incisions on your lower neck. Your surgeon will remove your thyroid gland. If you have cancer, your surgeon may also remove the tissue and lymph nodes around your thyroid gland.
- A drain may be placed into your incision to remove extra fluids from the surgery area. Your incision will be closed with stitches or surgical glue and covered with a bandage.
What to expect after a total thyroidectomy:
You will be taken to a recovery room until you are fully awake. Healthcare providers will watch you closely for problems. Do not get out of bed until your provider says it is okay. Tell providers if you have difficulty breathing or swallowing. Tell them if your bandage feels like it is getting tight. You will have blood tests to check your calcium and thyroid hormone blood levels. You may need to stay in the hospital overnight or longer, depending on your condition.
Risks of a total thyroidectomy:
- You may bleed more than expected or develop a hematoma (pooling of blood). This may make it hard for you to breathe or swallow and needs to be treated immediately. Your vocal cords may be damaged and cause your voice to be hoarse or weak. This may become a long-term problem. You may develop a blood clot in your arm or leg. The clot may travel to your heart or brain and cause life-threatening problems, such as a heart attack or stroke.
- Your parathyroid glands may not work as well as they should after surgery. This can cause your calcium levels to drop too low. Low calcium levels can cause many problems, including an irregular heartbeat, muscle spasms, and seizures. This may be a short-term problem after surgery, or it may be a long-term problem.
Call your local emergency number (911 in the US), or have someone call if:
- You have sudden swelling in your neck or trouble swallowing.
- You have trouble breathing.
- You have a seizure.
Related medications
Seek care immediately if:
- Your arm or leg feels warm, tender, and painful. It may look swollen and red.
- Your incision comes apart, or blood soaks through your bandage.
- You suddenly feel lightheaded and short of breath.
- You have chest pain when you take a deep breath or cough, or you cough up blood.
- Your incision is swollen, red, or has pus coming from it.
- You have sudden tingling or muscle cramps in your face, arm, or leg.
- You have muscle spasms in your legs and feet that do not go away.
Call your endocrinologist or surgeon if:
- You have a fever.
- You have pain in your surgery area that does not go away after you take pain medicine.
- You lose weight, feel very nervous and hungry, and sweat for no reason.
- You feel very tired and cold, gain weight for no reason, and your skin is very dry.
- You vomit several times in a row.
- You have new voice weakness or hoarseness, or it is getting worse.
- You have questions or concerns about your condition or care.
Medicines:
- Thyroid medicine will replace the hormone your thyroid would have produced. You will need to take this medicine every day.
- Prescription pain medicine may be given. Ask your healthcare provider how to take this medicine safely. Some prescription pain medicines contain acetaminophen. Do not take other medicines that contain acetaminophen without talking to your healthcare provider. Too much acetaminophen may cause liver damage. Prescription pain medicine may cause constipation. Ask your healthcare provider how to prevent or treat constipation.
Incision site care:
Check the incision site every day for signs of infection, such as redness, swelling, or pus. Carefully wash your skin near the incision site with soap and water. Dry the area and put on new, clean bandages as directed. Change your bandages when they get wet or dirty.
Self-care:
- Follow activity instructions. Do not lift anything heavier than 10 pounds or do vigorous activities. Do not drive until your surgeon says it is okay. These actions will put too much stress on your incision. Ask your surgeon which activities are safe for you. Also ask when you can return to your usual activities such as work or school.
- Ask your healthcare provider about supplements. Your provider will tell you if you need to take calcium or vitamin D, and how much to take.
Follow up with your endocrinologist or surgeon as directed:
You will need to return to have your incision site checked and stitches removed. You may also need blood tests to monitor your calcium, parathyroid, and thyroid hormone levels. Write down your questions so you remember to ask them during your visits.
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
