Pulmonary Arterial Hypertension
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is pulmonary arterial hypertension (PAH)?
PAH is a condition that increases pressure in your pulmonary artery. The pulmonary artery is the large blood vessel that brings blood from your heart to your lungs.
 |
What causes PAH?
PAH may be passed from a parent to a child. This is called heritable or familial PAH. PAH with no known cause is called idiopathic PAH. Associated PAH means another condition caused you to develop PAH. The following are common causes of associated PAH:
- Certain conditions, such as tumors pressing on the pulmonary artery or sickle cell disease
- Problems in your heart, lungs, or blood vessels
- An infection, such as schistosomiasis or HIV
- Portal hypertension or cirrhosis
- Connective tissue diseases, such as scleroderma, lupus, or rheumatoid arthritis
- Certain weight loss medicines or illegal drugs
What are the signs and symptoms of PAH?
- Feeling weak and tired
- Weight gain or lack of appetite
- Shortness of breath with exercise
- Swelling in your ankles, legs, or abdomen
- Chest pain or heart palpitations (strong, fast heartbeats)
- Dizziness or feeling faint
- Cough, hoarseness, or wheezing
How is PAH diagnosed?
Your healthcare provider will ask about your medical history and examine you. You may need any of the following tests:
- Blood tests may be used to find the cause of your PAH. These tests may also show the amount of oxygen and carbon dioxide in your blood.
- A blood vessel test may be used to see if the small arteries in your lungs will widen (dilate) when you are given a medicine. The pressure in your pulmonary artery will be measured before and after the medicine is given.
- An EKG may be used to check for damage or problems in your heart. A short period of electrical activity in your heart is recorded.
- An x-ray, echocardiogram, CT, or MRI may be used to show the structure, movement, and blood vessels of your heart. You may be given contrast liquid to help healthcare providers see the pictures better. Tell the healthcare provider if you have ever had an allergic reaction to contrast liquid. Do not enter the MRI room with anything metal. The MRI machine uses a powerful magnet. Metal can cause serious injury from the magnet. Tell healthcare providers if you have any metal in or on your body.
- Cardiac catheterization is a procedure used to look for or treat a heart condition. A catheter is inserted in your arm, neck, or groin and moved into your heart. Contrast liquid is injected into an artery and x-rays of your blood flow are taken. Tell a healthcare provider if you have ever had an allergic reaction to contrast liquid.
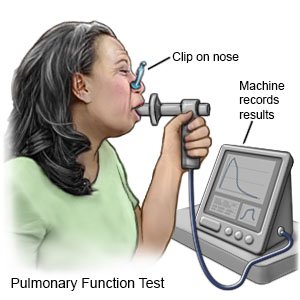
- Pulmonary function tests (PFTs) help healthcare providers learn how well your body uses oxygen. You breathe into a mouthpiece connected to a machine. The machine measures how much air you breathe in and out over a certain amount of time. PFTs help your healthcare providers decide the best treatment for you.
- A ventilation and perfusion (VQ) scan takes pictures of your lungs. During the perfusion part of the test, contrast liquid will be given through an IV. This liquid helps the blood flow in your lungs show up clearly on the monitor. During the ventilation part, you will breathe in a medical gas. Pictures will be taken to see how well your lungs take in oxygen. Tell a healthcare provider if you have ever had an allergic reaction to contrast liquid.
- A cardiopulmonary exercise test shows how much physical activity your heart and lungs can safely tolerate. You may be asked to ride a stationary bike or walk on a treadmill. Healthcare providers will monitor your oxygen level, heart rate, and blood pressure. Your provider will tell you how to prepare for these tests.
How is PAH treated?
PAH cannot be cured. The goals of treatment are to improve your symptoms and stop PAH from getting worse. You may need any of the following:
- Medicines may be given to improve blood flow, get rid of extra fluid, or prevent blood clots. Blood clot medicine may make you bruise or bleed more easily. Use a soft toothbrush and an electric shaver to prevent bleeding.
- You may need extra oxygen if your blood oxygen level is lower than it should be. You may get oxygen through a mask placed over your nose and mouth or through small tubes placed in your nostrils. Ask your healthcare provider before you take off the mask or oxygen tubing.
- Surgery may be used to help blood flow from one part of the heart to another. You may need lung or heart transplant surgery if other treatments do not work and your condition is severe.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
What can I do to manage PAH?
- Check your blood pressure (BP) at home. Sit and rest for 5 minutes before you take your BP. Extend your arm and support it on a flat surface. Your arm should be at the same level as your heart. Follow the directions that came with your BP monitor. If possible, take at least 2 BP readings each time. Take your BP at least twice a day at the same times each day, such as morning and evening. Keep a record of your BP readings and bring it to your follow-up visits. Ask your healthcare provider what your BP should be.

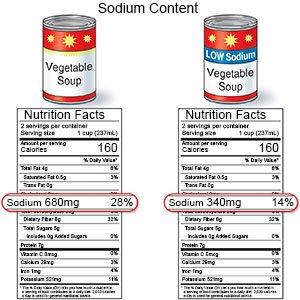
- Limit sodium (salt) as directed. Too much sodium can affect your fluid balance. Check labels to find low-sodium or no-salt-added foods. Some low-sodium foods use potassium salts for flavor. Too much potassium can also cause health problems. Your provider will tell you how much sodium and potassium are okay for you to have in a day. Your provider may recommend that you limit sodium to 2,300 mg a day.
- Follow the meal plan recommended by your provider. A dietitian or your provider can give you more information on low-sodium plans or the DASH (Dietary Approaches to Stop Hypertension) eating plan. The DASH plan is low in sodium, unhealthy fats, and total fat. It is high in potassium, calcium, and fiber.

- Limit liquids as directed. You may need to drink less liquid to help balance your fluid level. Ask how much liquid you should drink each day. Your provider will give you an exact amount of liquid to drink each day. You may be limited to less than 2 liters a day.
- Do not smoke. Nicotine and other chemicals in cigarettes and cigars can increase your BP and also cause lung damage. Ask your provider for information if you currently smoke and need help to quit. E-cigarettes or smokeless tobacco still contain nicotine. Talk to your provider before you use these products.
- Limit or avoid alcohol. Alcohol can make it hard for you to control your BP. Limit alcohol to 1 drink within 24 hours if you are female. Limit alcohol to 2 drinks within 24 hours if you are male. A drink of alcohol is 12 ounces of beer, 5 ounces of wine, or 1½ ounces of liquor.
- Be physically active, as directed. Physical activity, such as exercise, may help decrease your symptoms and improve your heart function. Physical activity also helps with weight control. Do not start a physical activity program before you talk with your provider.
- Avoid activities that raise your body temperature. Do not sit in a sauna, hot tub, or hot bath. This can lower your blood pressure and cause you to faint.
- Talk to your provider about pregnancy if you are female. Pregnancy may not be safe for you. You may need to change your birth control method if you currently use birth control pills. Birth control pills may increase your risk for blood clots. Your provider can help you choose other methods that work for you.
- Manage health conditions affecting PAH. You may need treatment for sleep apnea, hypertension, or other medical conditions. Ask your provider for more information.
- Do not travel to high altitudes unless your provider says it is okay. You may need to bring extra oxygen if you are traveling to a high altitude or are flying.
Call your local emergency number (911 in the US) if:
- You have chest pain or heart palpitations.
- You have shortness of breath at rest, especially when you lie down.
- Your lips or fingers turn blue.
When should I seek immediate care?
- You are confused or feel like you are going to faint.
- Your legs or ankles are swollen.
- You cough up blood.
When should I call my doctor?
- You have a fever.
- Your symptoms keep you from doing your daily activities.
- Your fingers or toes are clubbed (the ends are round and thick).
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Pulmonary Arterial Hypertension
Treatment options
Medicine.com guides (external)
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
