Laparoscopic Adrenalectomy
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
WHAT YOU NEED TO KNOW:
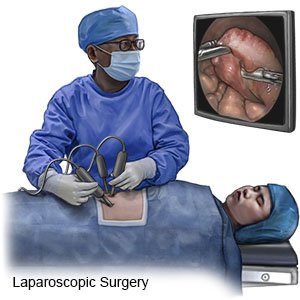
Laparoscopic adrenalectomy is surgery to remove all or part of your adrenal gland. It is usually done when a small tumor is found on the gland. Small incisions are made in your abdomen. A laparoscope is inserted through the incisions. A laparoscope is a long metal tube with a tiny video camera and a light on the end. The camera displays pictures of your adrenal glands on a monitor. The monitor is used to guide the surgery tools to the right place.
HOW TO PREPARE:
The week before your surgery:
- Arrange to have someone drive you home after your surgery.
- Tell your surgeon about all medicines you currently take. He or she will tell you if you need to stop any medicine for surgery, and when to stop. He or she will tell you which medicines to take or not take on the day of surgery.
- If you have diabetes, ask your healthcare provider for instructions about what you may eat and drink before your surgery. If you use medicine to treat diabetes, your provider may have instructions about using it before surgery. You may need to check your blood sugar level more often before and after surgery.
- Contrast liquid may be used during your surgery to help your adrenal glands show up better in the pictures. Tell your surgeon if you have ever had an allergic reaction to contrast liquid.
- If you are a woman, tell your healthcare provider if you know or think you might be pregnant.
- You may need to have blood tests, an electrocardiogram (ECG), chest x-ray, and other tests.
The night before your surgery:
You may be told not to eat or drink anything after midnight.
The day of your surgery:
- Take only the medicines your surgeon told you to take.
- An IV will be put in a vein. You may be given liquids or medicine through the IV.
- An anesthesiologist may talk to you about medicine to make you sleepy before your surgery. Tell him or her if you or any member of your family had a problem with anesthesia.
- You or a close family member will be asked to sign a legal piece of paper (informed consent). It gives your healthcare provider permission to do the surgery. It also explains the problems that may happen with the surgery, and your treatment choices. Be sure all of your questions have been answered before you sign this form.
WHAT WILL HAPPEN:
What will happen:
- You may be given general anesthesia to keep you asleep and free from pain during surgery.
- Small incisions will be made in your abdomen. Healthcare providers will insert the laparoscope and other tools into the incisions. Your abdomen will be filled with carbon dioxide gas to make it swell. The adrenal gland will be separated from its attachments and removed.
- The incisions will be closed by stitches or tape, and covered with bandages.
After your surgery:
You will be taken to a recovery room until you are fully awake. Healthcare providers will watch you closely for any problems. Do not get out of bed until your healthcare provider says it is OK. When healthcare providers see that you are OK, you will be taken back to your hospital room. The bandages covering your stitches will keep the area clean and dry to prevent infection.
CONTACT YOUR HEALTHCARE PROVIDER IF:
- You have a fever.
- Your skin is itchy, swollen, or has a rash.
- You have questions or concerns about your surgery.
Seek Care Immediately if
- You have trouble breathing or your heart is beating faster than usual.
- Your abdomen is tender and hard.
- Your vomit contains blood.
Risks
Problems may happen during your surgery and may lead to open surgery. An example is bleeding that cannot be controlled. Your stomach, intestines, blood vessels, or kidneys may get injured during the surgery. You could also have trouble breathing, get an infection, or have too much bleeding after surgery. You may develop a life-threatening blood clot. The gas used to expand your abdomen may cause shoulder or chest pain for 1 to 2 days after your surgery.
Related medications
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
