Hypercalcemia
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is hypercalcemia?
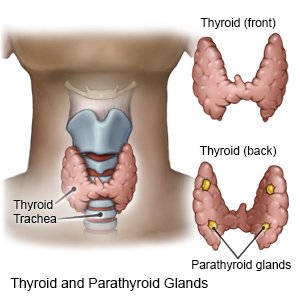
Hypercalcemia is a high level of calcium in your blood. Calcium levels are kept in balance by your parathyroid glands. Your parathyroid glands are located in your neck near your thyroid gland.
 |
What causes hypercalcemia?
- Overactive thyroid or parathyroid gland
- Medical conditions such as cancer, kidney failure, or sarcoidosis
- Medicines such as thiazide diuretics
- High doses of vitamin A or D supplements or antacids that contain calcium
- Lack of movement for long periods of time
What are the signs and symptoms of hypercalcemia?
You may have no signs or symptoms, or you may have any of the following:
- Muscle weakness and fatigue
- Confusion or trouble concentrating
- Headache
- Abdominal pain, constipation, nausea, vomiting, or loss of appetite
- Frequent urination or increased thirst
- Bone or joint pain
How is hypercalcemia diagnosed?
Your healthcare provider will ask about any medicines or supplements you take. Your provider may also ask if you have a family history of hypercalcemia. Blood and urine tests will be done to measure your calcium and parathyroid hormone levels. Other tests may also be done to find the cause of your hypercalcemia.
Related medications
How is hypercalcemia treated?
Treatment depends on the cause of your hypercalcemia. You may need any of the following:
- IV fluids may be given to treat dehydration and to help your body get rid of extra calcium.
- Medicines may be given to help lower your calcium level or to treat the cause of your hypercalcemia.
- Surgery may be needed to remove one or more parathyroid gland.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
How do I manage my hypercalcemia?
- Drink liquids as directed. Liquids will help prevent dehydration and kidney stones. Ask your healthcare provider how much liquid to drink each day and which liquids are best for you.
- Follow your healthcare provider's advice on ways to stay active. Activity can help prevent your hypercalcemia from getting worse.
When should I contact my healthcare provider?
- You feel confused, or you have trouble concentrating.
- You have new or worsening symptoms.
- You have symptoms of dehydration, such as increased thirst, dark yellow urine, and little or no urine.
- You have questions or concerns about your condition or care.
When should I seek immediate care or call 911?
- You feel fluttering or jumping in your chest.
- You feel like you are going to pass out.
- You have nausea and you are vomiting.
- You have pain in the middle of your back that moves across to your side, or that spreads to your groin.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
