Gastrointestinal Bleeding
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What do I need to know about gastrointestinal (GI) bleeding?
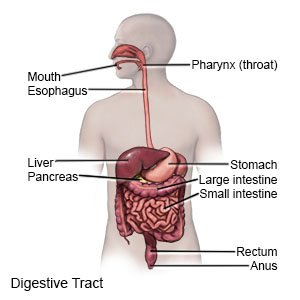
GI bleeding may occur in any part of your digestive tract. This includes your esophagus, stomach, intestines, rectum, or anus. Bleeding may be mild to severe. Your bleeding may begin suddenly, or start slowly and last for a longer period of time. Bleeding that lasts for a longer period of time is called chronic GI bleeding.
 |
What causes GI bleeding?
The cause of your GI bleeding may not be known. The following are common causes:
- Inflammation, ulcers, or infection in your digestive tract
- Swollen blood vessels in your digestive tract that break open and bleed
- Tears in the lining of your esophagus caused by forceful, repeated vomiting
- Crohn disease, colitis, cancer, or diverticulosis
- Hemorrhoids or a tear in the lining of your anus
What are the signs and symptoms of GI bleeding?
Symptoms depend on where the bleeding is, what is causing it, and how much blood you have lost. You may have any of the following:
- Blood in your vomit, or vomit that looks like coffee grounds
- Dark or bright red blood in your bowel movements
- Bleeding from your rectum
- Cramping or pain in your abdomen
- Fatigue, weakness, or dizziness
- Shortness of breath
- Pale skin or gums, and sweaty or clammy skin
- Faster heartbeat than usual
- Urinating less than usual or not at all
- Fainting or loss of consciousness
How is GI bleeding diagnosed?
You may need treatment and monitoring in the hospital. Tell the healthcare provider if you take blood thinner medicine. You may need medicine to reverse the effects of blood thinner medicine. You may need any of the following to find the cause of GI bleeding:
- Blood tests may be done to measure your blood cell levels. This information will tell healthcare providers how much blood you have lost. Blood tests will also check for infection and get information about your overall health.
- A sample of your bowel movement can be tested for blood or infection.
- X-ray or CT pictures may show bleeding or problems in your digestive tract. Contrast liquid may be given to help your digestive tract show up better in pictures. Tell a healthcare provider if you have ever had an allergic reaction to contrast liquid.
- An endoscopy is a procedure to find the cause of bleeding in your esophagus, stomach, or small intestine. A capsule endoscopy may be done as an outpatient procedure. Ask your healthcare provider for more information about a capsule endoscopy.
- A colonoscopy is a procedure to find the cause of bleeding in your intestines or rectum.
How is GI bleeding treated?
Your bleeding may get better without treatment. If bleeding is severe or causes symptoms, you may need any of the following:
- Treatment during endoscopy or colonoscopy may be done. Medicine may be injected into your esophagus, stomach, or intestines to stop bleeding. Heat or an electrical current may also be applied to stop bleeding. Other procedures, such as banding, may be used. Banding uses a plastic band to cut off the blood supply to a blood vessel. This stops the bleeding in your digestive tract.
- Surgery may be needed to find and stop GI bleeding.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
What can I do to prevent GI bleeding?
- Manage GI conditions as directed. Examples of GI conditions include gastroesophageal reflux, peptic ulcer disease, and ulcerative colitis. Take all medicines for these conditions as directed.
- Limit or do not take NSAIDs. Ask your healthcare provider if it is safe for you to take NSAIDs. NSAIDs can increase your risk for ulcers and GI bleeding.
- Do not drink alcohol. Alcohol can cause ulcers and esophageal varices. Esophageal varices are swollen blood vessels in your esophagus. Over time the blood vessels become weak and may bleed.
- Do not smoke. Nicotine and other chemicals in cigarettes and cigars can increase your risk for ulcers. Ask your healthcare provider for information if you currently smoke and need help to quit. E-cigarettes or smokeless tobacco still contain nicotine. Talk to your healthcare provider before you use these products.
Related medications
Call 911 for any of the following:
- You have shortness of breath or trouble breathing.
- You faint or lose consciousness.
- You have chest pain.
When should I seek immediate care?
- You feel dizzy or are too weak to stand.
- Your heart is beating faster than usual.
- You vomit blood, or your vomit looks like coffee grounds.
- You have blood in your bowel movement.
- You have abdominal pain or swelling.
When should I contact my healthcare provider?
- You have bowel movements that are tarry or black.
- You have nausea or are vomiting.
- You have heartburn.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Gastrointestinal Bleeding
Treatment options
Care guides
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
