Fine Needle Breast Biopsy
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
AMBULATORY CARE:
What you need to know about a fine needle breast biopsy (FNBB):
A FNBB is a procedure to remove a sample of fluid or tissue from your breast. The samples are sent to a lab and tested for cancer or infection.
How to prepare for a FNBB:
- Your healthcare provider will talk to you about how to prepare for your procedure. You may need to stop taking blood thinner medicine or aspirin 3 days before your procedure. The provider may tell you not to eat or drink anything 8 hours before your procedure. The provider will tell you what medicines to take or not take on the day of your procedure.
- You may be given contrast liquid during your procedure to help the tissue show up better in the pictures. Tell the healthcare provider if you have ever had an allergic reaction to contrast liquid. An MRI may also be used during your procedure. Do not enter the procedure room with anything metal. Metal can cause serious injury. Tell the healthcare provider if you have any metal in or on your body. Also tell him or her if you are pregnant or think you are pregnant. Special shields can be used during the procedure to keep your baby safe.
- Do not put on lotions or powders on the day of your procedure. Do not put on deodorant if your biopsy will be taken near your armpit. These products may cause particles to appear on your x-ray. Wear loose-fitting clothing to your procedure. Arrange for someone to drive you home and stay with you after your procedure.
What will happen during a FNBB:
- You may be given IV sedation to help you relax during your procedure. You may also be given local anesthesia to numb the surgery area. With local anesthesia, you may still feel pressure or pushing during your procedure, but you should not feel any pain. You may be given contrast liquid through your IV to help your breast tissue show up better in pictures.
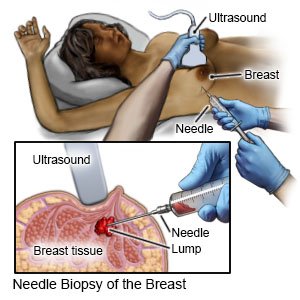
- Your healthcare provider may make a small incision in your breast. He or she will insert a needle through your skin and into the tissue. The provider may use x-ray, ultrasound, or MRI pictures to help guide the needle to the correct place. When the needle reaches the fluid or tissue, samples will be taken. Your healthcare provider may use a syringe or small vacuum to help remove the fluid or tissue.
- After your healthcare provider takes samples, he or she may mark the area with a small wire or metal clip. The provider may also inject the area with liquid dye. This will help other healthcare providers find the abnormal tissue at a later time. The provider will remove the needle and apply pressure to the area. You will not need stitches. A small bandage will be placed over your biopsy site. Your healthcare provider may also wrap a tight-fitting bandage across both breasts. This may prevent bleeding, swelling, and pain at the biopsy site.
What will happen after a FNBB:
Healthcare providers will monitor you until you are awake. You may need a mammogram if a marker was inserted during your procedure. This will make sure that it is in the correct place. You may be sore or have bruising or swelling in your breast for a few days. Do not breastfeed for 24 to 48 hours if you received contrast liquid. The contrast liquid may harm your baby. You may go home after your procedure or you may need to spend a night in the hospital.
Risks of a FNBB:
You may bleed more than expected or get an infection. A pocket of blood or fluid may form under your skin. You may need surgery to drain or remove it. The biopsy needle may make a hole in your lung and cause trouble breathing. You may need other treatments to fix the hole.
Call 911 for any of the following:
- You feel lightheaded, short of breath, and have chest pain.
- You cough up blood.
- You have trouble breathing.
Related medications
Seek care immediately if:
- Blood soaks through your bandage.
- Your bruise suddenly gets larger and feels hard.
- You have severe pain in your breast.
Contact your healthcare provider if:
- You have a fever or chills.
- Your biopsy site is red, swollen, or draining pus.
- You have nausea or are vomiting.
- Your skin is itchy, swollen, or you have a rash.
- Your pain does not get better after you take pain medicine.
- You have questions or concerns about your condition or care.
Medicines:
You may need any of the following:
- NSAIDs , such as ibuprofen, help decrease swelling, pain, and fever. This medicine is available with or without a doctor's order. NSAIDs can cause stomach bleeding or kidney problems in certain people. If you take blood thinner medicine, always ask your healthcare provider if NSAIDs are safe for you. Always read the medicine label and follow directions.
- Acetaminophen decreases pain and fever. It is available without a doctor's order. Ask how much to take and how often to take it. Follow directions. Read the labels of all other medicines you are using to see if they also contain acetaminophen, or ask your doctor or pharmacist. Acetaminophen can cause liver damage if not taken correctly.
- Prescription pain medicine may be given. Ask your healthcare provider how to take this medicine safely. Some prescription pain medicines contain acetaminophen. Do not take other medicines that contain acetaminophen without talking to your healthcare provider. Too much acetaminophen may cause liver damage. Prescription pain medicine may cause constipation. Ask your healthcare provider how to prevent or treat constipation.
- Take your medicine as directed. Contact your healthcare provider if you think your medicine is not helping or if you have side effects. Tell your provider if you are allergic to any medicine. Keep a list of the medicines, vitamins, and herbs you take. Include the amounts, and when and why you take them. Bring the list or the pill bottles to follow-up visits. Carry your medicine list with you in case of an emergency.
Care for your biopsy site as directed:
If you have a tight-fitting bandage, you can remove it in 24 to 48 hours, or as directed. Ask your healthcare provider when your biopsy site can get wet. Carefully wash around the site with soap and water. It is okay to let soap and water gently run over your biopsy site. Do not scrub the site. Dry the area and put on new, clean bandages as directed. Change your bandages when they get wet or dirty. Check your biopsy site every day for signs of infection such as redness, swelling, or pus. Do not put powders or lotions on your biopsy site.
Self-care:
- Apply ice on your biopsy site for 15 to 20 minutes every hour or as directed. Use an ice pack, or put crushed ice in a plastic bag. Cover it with a towel before you apply it to your skin. Ice helps prevent tissue damage and decreases swelling and pain.
- Rest as directed. Do not lift anything heavier than 5 pounds, play sports, or exercise for 24 hours or as directed. These activities may cause bleeding. Short walks around the house are okay.
- Drink plenty of liquids as directed. Liquids help flush contrast liquid from your body. Ask how much liquid to drink each day and which liquids are best for you.
- Wear a supportive bra as directed. You may have to wait until you remove the tight-fitting bandage to wear a bra. You can wear a sports bra or a wireless bra that fits snugly. A supportive bra may help decrease swelling and pain.
Follow up with your doctor as directed:
Write down your questions so you remember to ask them during your visits.
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Learn more about Fine Needle Breast Biopsy
Care guides
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
