Chronic Kidney Disease
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
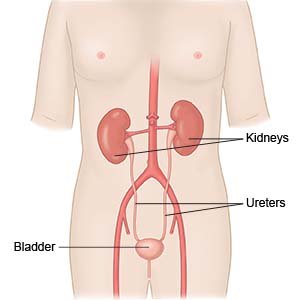
Chronic kidney disease (CKD) is the gradual and permanent loss of kidney function. It is also called chronic kidney failure, or chronic renal insufficiency. Normally, the kidneys remove fluid, chemicals, and waste from your blood. These wastes are turned into urine by your kidneys. CKD may worsen over time and lead to kidney failure. Your CKD team will help you and your family plan for your care at home. The team will help you create goals and find ways to meet your goals. Your care plan may change over time as your needs change.
 |
DISCHARGE INSTRUCTIONS:
Call your local emergency number (911 in the US) if:
- You have a seizure.
- You have shortness of breath.
Seek care immediately if:
- You are confused and very drowsy.
Call your doctor or nephrologist if:
- You suddenly gain or lose more weight than your healthcare provider has told you is okay.
- You have itchy skin or a rash.
- You urinate more or less than you normally do.
- You have blood in your urine.
- You have nausea and are vomiting.
- You have fatigue or muscle weakness.
- You have hiccups that will not stop.
- You have questions or concerns about your condition or care.
Medicines:
- Medicines may be given to decrease blood pressure and get rid of extra fluid. You may also receive medicine to manage health conditions that may occur with CKD, such as anemia, diabetes, and heart disease.
- Take your medicine as directed. Contact your healthcare provider if you think your medicine is not helping or if you have side effects. Tell your provider if you are allergic to any medicine. Keep a list of the medicines, vitamins, and herbs you take. Include the amounts, and when and why you take them. Bring the list or the pill bottles to follow-up visits. Carry your medicine list with you in case of an emergency.
What you can do to manage CKD:
Management may include making some lifestyle changes. Tell your healthcare provider if you have any concerns about being able to make changes. He or she can help you find solutions, including working with specialists. Ask for help creating a plan to break large goals into smaller steps. Your plan may include any of the following:
- Manage other health conditions. Your healthcare provider will work with you to make a care plan that meets your needs. You will be checked regularly for heart disease or other conditions that can make CKD worse, such as diabetes. Your blood pressure will be closely monitored. You will also get a target blood pressure and help making a plan to reach your target. This may include taking your blood pressure at home.

- Maintain a healthy weight. Your weight and body mass index (BMI) will be checked regularly. BMI helps find if your weight is healthy for your height. Your healthcare provider will use other tests to check your muscle and protein levels. Extra weight can strain your kidneys. A low weight or low muscle mass can make you feel more tired. You may have trouble doing your daily activities. Ask your provider what a healthy weight is for you. He or she can help you create a plan to lose or gain weight safely, if needed. The plan may include keeping a food diary. This is a list of foods and liquids you have each day. Your provider will use the diary to help you make changes, if needed. Changes are based on your health and any other conditions you have, such as diabetes.
- Create an exercise plan. Regular exercise can help you manage CKD, high blood pressure, and diabetes. Exercise also helps control weight. Your provider can help you create exercise goals and a plan to reach those goals. For example, your goal may be to exercise for 30 minutes in a day. Your plan can include breaking exercise into 10 minute sessions, 3 times during the day.

- Create a healthy eating plan. Your provider may tell you to eat food low in potassium, phosphorus, or protein. Your provider may also recommend vitamin or mineral supplements. Do not take any supplements without talking to your provider. A dietitian can help you plan meals if needed. Ask how much liquid to drink each day and which liquids are best for you.
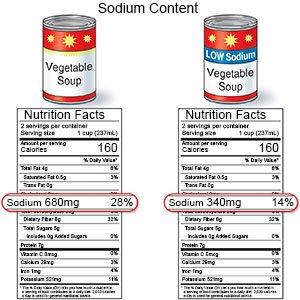
- Limit sodium (salt) as directed. You may need to limit sodium to less than 2,300 milligrams (mg) each day. Ask your dietitian or healthcare provider how much sodium you can have each day. The amount depends on your stage of kidney disease. Table salt, canned foods, soups, salted snacks, and processed meats, like deli meats and sausage, are high in sodium. Your provider or a dietitian can show you how to read food labels for sodium.
- Limit alcohol as directed. Alcohol can cause fluid retention and can affect your kidneys. Ask how much alcohol is safe for you. A drink of alcohol is 12 ounces of beer, 5 ounces of wine, or 1½ ounces of liquor.
- Do not smoke. Nicotine and other chemicals in cigarettes and cigars can cause kidney damage. Ask your provider for information if you currently smoke and need help to quit. E-cigarettes or smokeless tobacco still contain nicotine. Talk to your provider before you use these products.
- Ask about over-the-counter medicines. Medicines such as NSAIDs and laxatives may harm your kidneys. Some cough and cold medicines can raise your blood pressure. Always ask if a medicine is safe before you take it.
- Ask about vaccines you may need. CKD can increase your risk for infections such as pneumonia, influenza, and hepatitis. Vaccines lower your risk for infection. Your healthcare provider will tell you which vaccines you need and when to get them.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
Follow up with your doctor or nephrologist as directed:
You will need to return for tests to monitor your kidney and nerve function, and your parathyroid hormone level. Your medicines may be changed, based on certain test results. Write down your questions so you remember to ask them during your visits.
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Learn more about Chronic Kidney Disease
- FDA-Approved Weight Loss Drugs: Can They Help You?
- Side Effects of Weight Loss Drugs
- Top 10 Diabetes Treatments You May Have Missed
Treatment options
Care guides
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
