Barrett Esophagus
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is Barrett esophagus?
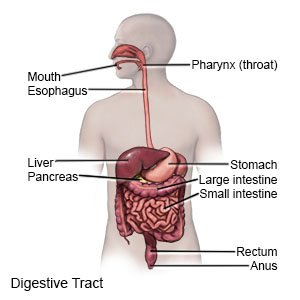
Barrett esophagus is a condition that causes cells in your esophagus to change into cells similar to intestine cells. The changed cells may become pre-esophageal cancer cells. This means they are not currently cancer but may become cancer. Dysplasia is a term used to describe the condition of having pre-cancer cells.
 |
What increases my risk for Barrett esophagus?
The exact cause of Barrett esophagus is not known. The following may increase your risk:
- Long-term gastroesophageal reflux disease (GERD)
- Age older than 50
- A family history of GERD, Barrett esophagus, or esophageal cancer
- A large amount of fat in your abdomen
- Past or current cigarette use
What are the signs and symptoms of Barrett esophagus?
Signs and symptoms are usually related to the signs and symptoms of GERD. You may have any of the following:
- Heartburn (burning pain in your chest)
- Pain after meals that spreads to your neck, jaw, or shoulder
- Pain that gets better when you change positions
- Bitter or acid taste in your mouth
- A dry cough
- Trouble swallowing or pain with swallowing
- Hoarseness or a sore throat
- Burping or hiccups
- Feeling full soon after you start eating
How is Barrett esophagus diagnosed?
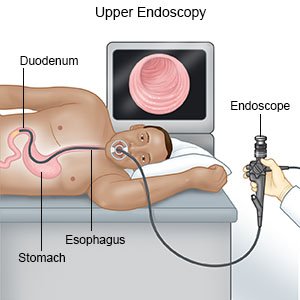
An endoscopy is a procedure used to see the inside of your esophagus and stomach. A scope is a long, bendable tube with a light on the end of it. A camera may be hooked to the scope. Your healthcare provider may also take tissue samples to be tested for dysplasia. Grades are used to describe the tissue samples. The grade can range from negative (no dysplasia) to high-grade (a large amount). You have a higher risk for cancer with high-grade dysplasia.
 |
How is Barrett esophagus treated?
The goal of treatment is to control your symptoms and prevent esophageal cancer. Your healthcare provider may also suggest that you make changes in the foods you eat and in your lifestyle. You may need any of the following:
- Anti-reflux medicines help decrease the stomach acid that can irritate your esophagus and stomach. These medicines may include proton pump inhibitors (PPI) and histamine type-2 receptor (H2) blockers. You may also be given medicines to stop vomiting.
- Endoscopic ablation is used to destroy dysplasia cells with heat, cold, or light. Your body may be able to create healthy esophageal cells after this treatment.
- Surgery may be used to wrap the upper part of your stomach around the esophageal sphincter to strengthen it. Surgery may be needed to remove dysplasia cells. For high-grade dysplasia, any affected part of your esophagus may need to be removed. New esophagus tissue is created from part of your stomach or intestine.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
What can I do to manage Barrett esophagus?
- Follow up with your healthcare provider or gastroenterologist as directed. Endoscopy and biopsy are done regularly to help look for early signs of esophageal cancer. If you have no dysplasia, your providers may do these tests in 1 year. You may then need the tests every 3 to 5 years, depending on your risk for cancer. If you do have dysplasia, you may need the tests several times each year. Timing depends on the dysplasia grade and treatment used.
- Do not eat foods that make your symptoms worse. Examples are chocolate, garlic, onions, spicy or fatty foods, citrus fruits (oranges), and tomato-based foods (spaghetti sauce). Do not have alcohol, caffeine, or carbonated drinks, such as soft drinks. Ask your provider if you should not have other foods or drinks.
- Maintain a healthy weight. Ask your provider what a healthy weight is for you. Your provider can help you create a weight loss plan, if needed.
- Do not smoke. Nicotine and other chemicals in cigarettes and cigars may worsen acid reflux. Ask your provider for information if you currently smoke and need help to quit. E-cigarettes and smokeless tobacco still contain nicotine. Talk to your provider before you use these products.
 |
Where can I get support and more information?
- American Cancer Society
250 Williams Street
Atlanta , GA 30303
Phone: 1- 800 - 227-2345
Web Address: http://www.cancer.org
Call your local emergency number (911 in the US) if:
- You have severe chest pain and shortness of breath.
When should I seek immediate care?
- Your bowel movements are black, bloody, or tarry.
- Your vomit looks like coffee grounds or has blood in it.
When should I call my doctor?
- Your symptoms do not improve with treatment.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Barrett Esophagus
Treatment options
Symptoms and treatments
Medicine.com guides (external)
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
