Fluorodopa F18: Package Insert / Prescribing Info
Package insert / product label
Dosage form: injection
Medically reviewed by Drugs.com. Last updated on Oct 7, 2024.
On This Page
- Indications and Usage
- Dosage and Administration
- Dosage Forms and Strengths
- Contraindications
- Warnings and Precautions
- Adverse Reactions/Side Effects
- Drug Interactions
- Use In Specific Populations
- Description
- Clinical Pharmacology
- Clinical Studies
- How Supplied/Storage and Handling
- Patient Counseling Information
Highlights of Prescribing Information
FLUORODOPA F 18 Injection, for intravenous use
Initial U.S. Approval: 2019
Indications and Usage for Fluorodopa F18
Fluorodopa F 18 Injection is a radioactive diagnostic agent indicated for use in positron emission tomography (PET) to visualize dopaminergic nerve terminals in the striatum for the evaluation of adult patients with suspected Parkinsonian syndromes (PS). Fluorodopa F 18 PET is an adjunct to other diagnostic evaluations. (1)
Fluorodopa F18 Dosage and Administration
• The recommended adult dose is 185 megabecquerels (MBq) [5 millicuries (mCi)] by intravenous injection infused over 1 minute. (2.2)
• Use aseptic techniques and radiation shielding to maintain sterility during all operations involved in the manipulation and administration of Fluorodopa F 18 Injection. (2.1, 2.2)
• Instruct patients to void immediately before imaging and start imaging at approximately 80 minutes post administration (with a 9 second CT scan for attenuation correction) followed by 3D PET scan from 80 to 100 minutes post administration. (2.5)
• See full prescribing information for additional preparation, administration, imaging and radiation dosimetry information. (2)
Dosage Forms and Strengths
Injection: clear, colorless solution in a multiple-dose glass vial containing 37 MBq/mL to 1,480 MBq/mL (1 mCi/mL to 40 mCi/mL) of Fluorodopa F 18 Injection. (3)
Contraindications
None (4)
Warnings and Precautions
Radiation risks: Use smallest dose necessary for imaging and ensure safe handling to protect the patient and healthcare worker from radiation exposure. (5.1)
Adverse Reactions/Side Effects
Injection site pain occurred with administration based on a review of the published literature. (6.2)
To report SUSPECTED ADVERSE REACTIONS, contact The Feinstein Institutes for Medical Research at 516-562-1052 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
Use In Specific Populations
• Lactation: To decrease radiation exposure to a nursing infant, advise a lactating woman to pump and discard breastmilk for at least 24 hours (12 half-lives) after administration of Fluorodopa F 18 Injection. (8.2)
See 17 for PATIENT COUNSELING INFORMATION.
Revised: 1/2021
Full Prescribing Information
1. Indications and Usage for Fluorodopa F18
Fluorodopa F 18 Injection is indicated for use in positron emission tomography (PET) to visualize dopaminergic nerve terminals in the striatum for the evaluation of adult patients with suspected Parkinsonian syndromes (PS). Fluorodopa F 18 PET is an adjunct to other diagnostic evaluations.
2. Fluorodopa F18 Dosage and Administration
2.1 Radiation Safety - Drug Handling
• Handle Fluorodopa F 18 Injection with appropriate safety measures to minimize radiation exposure [see Warnings and Precautions (5.1)]. Use waterproof gloves, effective shielding and appropriate safety measures to avoid unnecessary radiation exposure to the patient, occupational workers, clinical personnel, and other persons.
2.2 Recommended Dosage and Administration
Recommended Dose
• The recommended dose for adults is 185 megabecquerels (MBq) [5 millicuries (mCi)] administered as an intravenous injection infused over 1 minute.
• Minimize the dose of Fluorodopa F 18 Injection consistent with the objectives of the procedure and the nature of the imaging cameras employed.
Administration
• Use aseptic techniques and radiation shielding during all operations involved in the manipulation and administration of Fluorodopa F 18 Injection.
• Calculate the necessary volume to administer based on calibration time and dose.
• Inspect Fluorodopa F 18 Injection visually and do not use the drug if the solution contains particulate matter or is discolored.
• Measure the patient dose immediately prior to administration in a dose calibrator.
• Dispose of unused drug in compliance with applicable regulations.
2.3 Patient Preparation
Hydration
• Patients must have nothing to eat or drink, except water for 4 hours before administration
• To minimize the radiation absorbed dose to the bladder, instruct patient to:
o hydrate 4 hours prior to the administration of Fluorodopa F 18 Injection and continue hydration after the study.
o void 70 minutes after administration of Fluorodopa F 18 Injection and as frequently thereafter as possible for the next 12 hours.
Pre-medication and Medication Withdrawal
• Carbidopa blocks systemic/peripheral decarboxylation of Fluorodopa F 18 Injection to increase uptake in the brain. Administer 150 mg of Carbidopa orally at least 60 minutes (and no longer than 120 minutes) prior to the administration of Fluorodopa F 18 Injection.
• Instruct the patient to discontinue medications for the treatment of Parkinson’s disease 12 hours prior to administration of Fluorodopa F 18 Injection [see Drug Interactions (7)].
2.4 Radiation Dosimetry
The estimated human absorbed radiation dose for 10 human subjects (8 men and 2 women; mean age 50 ±8.8 yr) from intravenous administration of Fluorodopa F 18 Injection is shown in Table 1. In subjects who voided at 40 min post-injection, the radiation absorbed dose to the bladder wall was 50% lower than the radiation absorbed dose in subjects who voided at 2 hours post-injection. The identified critical organ is the urinary bladder.
| Organ | Absorbed Dose per unit activity (mGy/MBq) |
| Urinary bladder wall | 0.30 |
| Heart wall | 0.01 |
| Pancreas | 0.01 |
| Spleen | 0.01 |
| Lungs | 0.01 |
| Kidneys | 0.03 |
| Ovaries | 0.02 |
| Uterus | 0.03 |
| Lower Large Intestine wall | 0.02 |
| Liver | 0.01 |
| Gallbladder wall | 0.01 |
| Small Intestine | 0.01 |
| Upper Large Intestine wall | 0.01 |
| Stomach wall | 0.01 |
| Adrenals | 0.01 |
| Testes | 0.01 |
| Red marrow | 0.01 |
| Thymus | 0.01 |
| Thyroid | 0.01 |
| Muscle | 0.01 |
| Bone surfaces | 0.01 |
| Breast | 0.01 |
| Skin | 0.01 |
| Brain | 0.01 |
| Remaining organs | 0.01 |
| Effective dose (mSv/MBq) | 0.03 |
aICRP Publication 128, Radiation Dose to Patients from Radiopharmaceuticals, Annals of the ICRP, Vol. 44, No. 2S, 2015.
2.5 Imaging Guidelines
• Instruct the patient to void immediately before imaging, 70 minutes post administration.
• Start imaging at about 80 minutes post administration (with a 9 second CT scan for attenuation correction) followed by 3D PET scan from 80 to 100 minutes post administration.
2.6 Image Interpretation
Fluorodopa F 18 PET scans are interpreted visually, based upon the appearance and shape of the putamen and caudate of the striatum. Optimum presentation of the reconstructed images for visual interpretation is transaxial slices parallel to the anterior commissure-posterior commissure (AC-PC) line. Determination of whether an image is negative or positive is made by assessing the shape and intensity of the striatal signal (see Figure 1 and 2). Image interpretation does not involve integration of the image with clinical signs and/or symptoms.
Negative Scans: A full crescent shaped putamen and caudate image (see Figure 1). FDOPA uptake is clearly delineated from the background activity in the brain. It is bilaterally symmetrical and of uniform thickness in both caudate and putamen (comma- or crescent-shaped).
Figure 1: Negative Scan
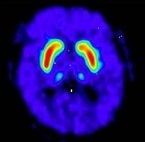
Positive Scans: A reduction in the size and shape of putamen (unilaterally or bilaterally) or both putamen and caudate (unilaterally or bilaterally). All of the following are considered positive:
• FDOPA uptake is asymmetric in the putamen; normal on one side but reduced on the contralateral side with respect to the background, especially in the posterior part. Caudate uptake is symmetrical on both sides and clearly delineated from the background (see Figure 2, A).
• FDOPA uptake is bilaterally reduced in the putamen (see Figure 2, B).
• FDOPA uptake is bilaterally reduced in the putamen and in the caudate nuclei (see Figure 2, C).
Figure 2: Positive Scans
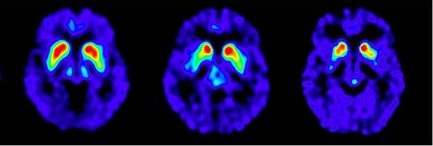
A B C
3. Dosage Forms and Strengths
Injection: clear, colorless solution containing 37 MBq/mL to 1,480 MBq/mL (1 mCi/mL to 40 mCi/mL) of Fluorodopa F 18 Injection, at calibration time in a multiple-dose glass vial.
5. Warnings and Precautions
5.1 Radiation Risks
Fluorodopa F 18 Injection use contributes to a patient’s overall long-term radiation exposure, which is associated with an increased risk of cancer. Use the smallest dose necessary for imaging and ensure safe handling to protect the patient and health care worker [see Dosage and Administration (2.1, 2.2)].
6. Adverse Reactions/Side Effects
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice. No adverse reactions have been reported for Fluorodopa F 18 Injection based on an open-label clinical trial in 68 patients [see Clinical Studies (14)] and additional clinical experience in 53 patients.
6.2 Postmarketing Experience
The following adverse reactions have been identified during post approval of use of Fluorodopa F 18 Injection outside of the United States. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
General Disorders and Administration Site Conditions: Pain
Related/similar drugs
7. Drug Interactions
Aromatic L-amino acid decarboxylase (AADC) inhibitors
Prior to Fluorodopa F 18 Injection administration, use of AADC inhibitors (e.g. carbidopa, benserazide etc.) may increase Fluorodopa F 18 bioavailability to the brain by inhibiting peripheral decarboxylase activity and restricting peripheral Fluorodopa F 18 metabolism [see Dosage and Administration (2.3)].
Dopamine agonists, dopamine reuptake inhibitors, dopamine releasing agents (DRAs), peripheral catechol-O-methyltransferase (COMT) inhibitors, and monoamine oxidase (MAO) inhibitors
Therapy for Parkinson’s syndromes includes dopamine agonists, dopamine reuptake inhibitors, dopamine releasing agents (DRAs) such as psychostimulants of the amphetamine class, peripheral catechol-O-methyltransferase (COMT) inhibitors, and monoamine oxidase (MAO) inhibitors. Whether discontinuation of these drugs prior to Fluorodopa F 18 administration may minimize the interference with a Fluorodopa F 18 image is not fully known; however, if use of these drugs can be safely suspended, discontinue use 12 hours before administration of Fluorodopa F18 Injection [see Dosage and Administration (2.3)].
8. Use In Specific Populations
8.1 Pregnancy
Risk Summary
There are no available data on Fluorodopa F 18 Injection use in pregnant women. Additionally, animal reproductive and developmental toxicity studies have not been conducted with Fluorodopa F 18 Injection. However, all radiopharmaceuticals, including Fluorodopa F 18 Injection, have a potential to cause fetal harm depending on the stage of fetal development, and the magnitude of the radiation dose. If considering Fluorodopa F 18 Injection administration to a pregnant woman, inform the patient about the potential for adverse pregnancy outcomes based on the radiation dose from the drug and the gestational timing of exposure.
The estimated background risk of major birth defects and miscarriage for the indicated population is unknown. All pregnancies have a background risk of birth defect, loss, or other adverse outcomes. In the U.S. general population, the estimated background risks of major birth defects and miscarriage in clinically recognized pregnancies are 2 to 4% and 15 to 20%, respectively, regardless of drug exposure.
8.2 Lactation
Risk Summary
No data are available regarding the presence of Fluorodopa F 18 Injection in human milk, the effects of the drug on the breastfed child, or the effects of the drug on milk production. Exposure of Fluorodopa F 18 Injection to a breast fed infant can be minimized by temporary discontinuation of breastfeeding [see Clinical Considerations]. The developmental and health benefits of breastfeeding should be considered along with the mother’s clinical need for Fluorodopa F 18 Injection and any potential adverse effects on the breastfed child from Fluorodopa F 18 Injection or from the underlying maternal condition.
The body of scientific information related to radioactivity decay, drug tissue distribution and drug elimination shows that less than 0.01% of the radioactivity administered remains in the body after 24 hours.
Clinical Considerations
To decrease radiation exposure to a nursing infant, advise a lactating woman to pump and discard breastmilk for at least 24 hours (12 half-lives) after administration of Fluorodopa F 18 Injection.
11. Fluorodopa F18 Description
11.1 Chemical Characteristics
Fluorodopa F 18 Injection is a radioactive diagnostic agent used in PET imaging. The active ingredient 6-[18F] Fluoro-L-3, 4-dihydroxyphenylalanine has the molecular formula of C9H10FNO4 with a molecular weight of 214.18, and has the following chemical structure:
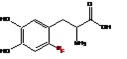
Fluorodopa F 18 Injection is a sterile, pyrogen-free, clear, colorless solution. Each mL contains between 37 MBq/mL to 1,480 MBq/mL (1 mCi/mL to 40 mCi/mL) of no-carrier added Fluorodopa F 18 (6-[18F] Fluoro-L-3, 4-dihydroxyphenylalanine) at the end of synthesis (EOS). There is 40.88 mg Na-EDTA, 140 mg ascorbic acid, and 663 mg ethanol in 28 mL ±1 mL sodium phosphate buffer. The pH of the solution is between 3 and 5.
11.2 Physical Characteristics
Fluorine F 18 is a cyclotron produced radionuclide that decays by positron emission to Oxygen O 18 (stable) and has a physical half-life of 109.7 minutes. The principal photons useful for imaging are the dual 511 keV gamma photons, which are produced and emitted simultaneously in opposite direction following positron-electron annihilation (Table 2).
| Radiation/Emission | % Per Disintegration | Mean Energy |
| Positron(+) | 96.73 | 249.8 keV |
| Gamma(±)* | 193.46 | 511.0 keV |
*Produced by positron annihilation
11.3 External Radiation
The point source air-kerma coefficient for F 18 is 3.75 × 10-17 Gy m2 / (Bq s). The half-value layer (HVL) for the 511 keV photons is 5 mm lead (Pb). The range of attenuation coefficients for this radionuclide as a function of lead shield thickness is shown in Table 3. For example, the interposition of a 9 mm thickness of Pb, with a coefficient of attenuation of 0.25, will decrease the external radiation by 75%.
| Shield thickness (Pb) mm | Coefficient of Attenuation |
| 0 | 0.00 |
| 5 | 0.50 |
| 9 | 0.25 |
| 15 | 0.10 |
| 29 | 0.01 |
| 39 | 0.001 |
| 52 | 0.0001 |
For use in correcting for physical decay of this radionuclide, the fractions remaining at selected intervals after calibration are shown in Table 4.
| Time Since Calibration | Fraction Remaining |
| 0* | 1.000 |
| 15 min | 0.909 |
| 30 min | 0.826 |
| 60 min | 0.683 |
| 110 min | 0.500 |
| 220 min | 0.250 |
| 440 min | 0.060 |
| 12 hours | 0.011 |
| 24 hours | 0.0001 |
*Calibration time
12. Fluorodopa F18 - Clinical Pharmacology
12.1 Mechanism of Action
In dopaminergic nerve terminals in the brain, Fluorodopa (FDOPA) F 18 is decarboxylated by amino acid decarboxylase to Fluorodopamine (FDA) F 18 and stored in presynaptic vesicles in the brain. The accumulation of F 18 FDA in the striatum is visually detected in the PET scan.
12.2 Pharmacodynamics
Optimal PET imaging is achieved between 75 to 90 minutes after administration of Fluorodopa F 18 Injection based on its pharmacokinetics. The relationship between Fluorodopa F 18 dose and plasma concentration is not fully characterized.
12.3 Pharmacokinetics
Distribution
Following the intravenous administration, Fluorodopa F 18 is cleared from the blood with a biologic half-life of about 1 to 3 hours. The time course of “background” brain radioactivity after Fluorodopa F 18 was evaluated. F 18 activity in the cerebellum was greater than the parietal or occipital cortex during the first 30 minutes after Fluorodopa F 18 suggesting regional differences in amino acid transport.
Elimination
Fluorodopa F 18 is cleared from the blood and tissue within 24 hours.
Metabolism: Fluorodopa F 18 is decarboxylated by aromatic amino acid decarboxylase in the striatum to Fluorodopamine F 18. Fluorodopamine F 18 is also metabolized via monoamine oxidase to yield [18F] 6-fluoro-3,4-dihydroxyphenylacetic acid (18FDOPAC) and subsequently by COMT to yield [18F]6-fluorohomovanillic acid (18FHVA).
Elimination: 80% of the radioactivity is eliminated through the urine. Urine radioactivity peaks at about 30 minutes post-injection. The radiation absorbed dose to the bladder wall is reduced by emptying the bladder just before scanning.
14. Clinical Studies
The safety and efficacy of F-18 FDOPA were evaluated in a prospective single-arm study conducted at a single center that enrolled 68 adult patients with possible Parkinsonian syndrome (PS). In the study, F-18 FDOPA image reads were compared to a reference clinical diagnostic standard of Parkinsonian syndrome or non-Parkinsonian syndrome (non-PS) established at 6 to 9 months after the F-18 FDOPA PET scan by a movement disorder specialist blinded to F-18 FDOPA PET results. The reference clinical diagnostic standard for PS included Parkinson's disease (PD), progressive supranuclear palsy (PSP), corticobasal degeneration (CBD), and multiple system atrophy (MSA). These conditions have been associated with dopaminergic neurodegeneration and F-18 FDOPA PET imaging was not designed to distinguish among the conditions. The reference clinical diagnostic standard for non-PS included essential tremor (ET) diagnosis, vascular parkinsonism, drug-induced parkinsonism, and other non-PS diagnoses.
Carbidopa (150 mg) was administered orally to patients approximately 60 minutes prior to the administration of Fluorodopa F 18 Injection. Each patient was injected 5 mCi F-18 FDOPA (range 4.5-5.5 mCi), and PET images were acquired 80-100 minutes post injection.
F-18 FDOPA PET images were evaluated independently by 3 readers blinded to clinical information who had no other role in patient assessment. Patients with at least one cardinal feature of PS were referred to the study by physicians who were uncertain of a diagnosis. Thirty-three of these patients had symptoms for 2 years or less. Fifty-six of these patients completed F-18 FDOPA PET imaging and at least 6 month clinical follow-up. Among these 56 patients, 32% were female and 68% were male. Mean patient age was 66 years. Thirty-three patients were categorized as PS, and twenty-three patients were categorized as non-PS based on minimum 6 month clinical follow-up by a movement disorder specialist.
Table 5 shows the positive percent agreement and negative percent agreement of F-18 FDOPA Injection PET image results with the reference clinical diagnostic standard. Positive percent agreement represents the percent of patients with positive F-18 FDOPA PET images among all the patients with a clinical diagnostic reference standard of PS. Negative percent agreement represents the percent of patients with negative F-18 FDOPA PET images among the patients with a non-PS clinical diagnostic reference standard.
| n=56 Patients |
Positive percent agreement Positive test/Clinical PS (95 % CI) |
Negative percent agreement Negative test/Clinical non-PS (95 % CI) |
| Reader 1 |
24/33 73% (55, 87) |
21/23 91% (72, 99) |
| Reader 2 |
16/33 49% (31, 67) |
21/23 91% (72, 99) |
| Reader 3 |
19/33 58% (39, 75) |
19/23 83% (61, 94) |
The effectiveness of F-18 FDOPA PET as a screening or confirmatory test and for monitoring disease progression or response to therapy has not been established.
16. How is Fluorodopa F18 supplied
Fluorodopa F 18 Injection (NDC 13267-346-57) is supplied as a clear, colorless injection in a septum capped glass vial containing between 37 MBq/mL to 1,480 MBq/mL (1 mCi/mL to 40 mCi/mL), of Fluorodopa F 18 at calibration time, in 28 mL ±1 mL.
Storage
Store the Fluorodopa F 18 Injection vial upright in a lead shielded container at 25°C (77°F); excursions permitted between 15ºC to 30°C (59ºF to 86°F). Avoid direct light.
The expiration date and time are provided on the container label. Use Fluorodopa F 18 Injection within 8 hours from the time of the end of synthesis (EOS).
Handling
This radiopharmaceutical is for distribution and use by persons licensed authorized by the U.S. Nuclear Regulatory Commission or the relevant regulatory authority of an Agreement State. Store and dispose of Fluorodopa F 18 in compliance with the appropriate regulations of the government agency authorized to license the use of this radionuclide.
17. Patient Counseling Information
Patient Preparation
Instruct patients to:
• Drink water in the 4 hours before their PET study and continue hydration with water or other fluids (as tolerated) after the study.
• Void 70 minutes after the administration of Fluorodopa F 18, before the start of the imaging study, and as frequently as possible after the study is complete for a total of 12 hours [see Dosage and Administration (2.3)].
Lactation
To decrease radiation exposure to a nursing infant, advise a lactating woman to pump and discard breastmilk for at least 24 hours (12 half-lives) after administration of Fluorodopa F 18 Injection. (8.2)
| FLUORODOPA
F18
fluorodopa f18 injection |
|||||||||||||||
|
|||||||||||||||
|
|||||||||||||||
|
|||||||||||||||
|
|||||||||||||||
|
|||||||||||||||
| Labeler - THE FEINSTEIN INSTITUTES FOR MEDICAL RESEARCH (110565913) |
| Registrant - THE FEINSTEIN INSTITUTES FOR MEDICAL RESEARCH (110565913) |
| Establishment | |||
| Name | Address | ID/FEI | Business Operations |
|---|---|---|---|
| THE FEINSTEIN INSTITUTES FOR MEDICAL RESEARCH | 110565913 | positron emission tomography drug production(13267-346) | |


